Carpal fractures and dislocations
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 28 Jul 2021
Meets Patient’s editorial guidelines
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Scaphoid wrist fracture article more useful, or one of our other health articles.
In this article:
The wrist is the most commonly injured joint in the body1 . Carpal bone fractures make up a significant proportion of injuries to the wrist. The complex bone shape and articulations make diagnosis more difficult and missed injuries more common. It is important to suspect and recognise carpal injuries, as they are difficult to diagnose and can cause permanent disability if untreated.
The usual mechanism of injury causing a carpal fracture is either a fall on to the outstretched hand, or direct trauma to the wrist area. Higher-impact injuries from falls or severe road traffic accidents can lead to dislocations of the carpal bones. A hard blow to the wrist during high-speed contact sports or from a projectile (eg, a ball, bat or club) may also cause fracture.
It is important to have patients describe the injury; acting out the traumatic event if possible. The physician must consider the age of the patient when evaluating the mechanism of injury. For example, the injury resulting from a fall on to the outstretched hand with the wrist extended will vary depending on the patient's age, typically causing a greenstick fracture in a toddler, a growth plate fracture in an adolescent, a scaphoid fracture in a young adult, and a Colles' (distal radius) fracture in an older adult with osteoporosis.
Athletes form an important subgroup of patients experiencing this injury. 25% of all athletic injuries occur to the hand or wrist2 . Hand and wrist injuries are more common in adolescent athletes than in adults.
The incidence of wrist fractures among women increases gradually with age from the age of 50 years. They are most likely to occur in women over 65 years old. In men, fracture rates remain low until later in life. Only 15% of wrist fractures occur in men and this rate does not increase much with age3 .
Continue reading below
Anatomy
Diagram showing scaphoid position
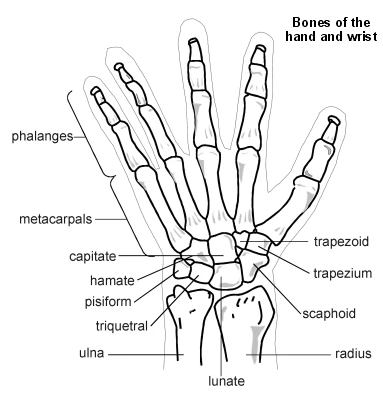
There are eight carpal bones in the region of the wrist, arranged in two rows and tightly interwoven with each other by intrinsic and extrinsic wrist ligaments:
The proximal row consists of the scaphoid, lunate, triquetrum and pisiform. These bones are closely approximated to the distal radius, with the scaphoid located most radially.
The distal row consists of the hamate, capitate, trapezoid and trapezium. This row is closely approximated to the metacarpal bones. The trapezium is located most radially.
The scaphoid links the two rows of carpals.
The lunate acts as a central anchor for the carpal bones.
The carpal bones are bound to each other by short intercarpal ligaments - for example, the scapholunate and the triquetrolunate.
Articulations
The distal radius articulates with the bones of the proximal carpal row (except the pisiform and triquetrum) at the radiocarpal joint. The radiocarpal and intercarpal ligaments support this joint.
The proximal carpal row articulates with the distal row at the carpocarpal joints. The intercarpal ligaments support these joints.
The distal carpal row articulates with the proximal end of the metacarpal bones at the carpometacarpal joints.
Carpal bone fractures
Carpal bone fractures can be difficult to detect on conventional X-ray and may require CT for diagnosis.
Fractures involving the carpal bones account for 18% of hand fractures.
Over 80% of carpal fractures involve the scaphoid; the second most common carpal bone to fracture is the triquetrum4 . Other carpal bones are much less commonly fractured. Capitate fractures are especially rare because the capitate bone sits in a protected position5 .
Where carpal fracture is suspected, X-rays in the anteroposterior (AP), lateral and oblique views are needed. Bone scans and CT scans are sometimes helpful if the fracture is not obvious on plain X-ray and should be considered where fracture is still suspected.
The management of carpal fractures depends on prompt diagnosis, stable and anatomical alignment of the involved carpal bone, protective immobilisation of the injury, and careful rehabilitation.
Scaphoid fracture
This is discussed in the separate Wrist Fractures article.
Triquetrum fracture
The triquetrum lies just distal to the ulnar styloid in the proximal carpal row6 . It lies under the pisiform bone so is difficult to palpate. To allow palpation, the hand must be radially deviated, exposing the triquetrum from beneath the ulnar styloid. Fractures can either be of a peripheral chip or through the body.
Usual mechanism of injury: direct blow to the dorsum of the hand or a fall resulting in extreme dorsiflexion of the wrist.
Diagnosis: if there is a fracture, point tenderness is usually found. X-ray confirms diagnosis.
Management: uncomplicated fractures can usually be treated with immobilisation in a cast and physiotherapy after cast removal. Displaced fractures through the body require closed reduction and pinning or open reduction and internal fixation.
Lunate fracture
The lunate articulates proximally with the radius and distally with the capitate. It is palpable just distal to the radial tubercle7 . Fractures of the lunate are rare, accounting for 0.5-6.5% of all carpal fractures8 .
Usual mechanism of injury: either a direct blow to the wrist, or following chronic recurrent trauma. The recurrent trauma is thought to cause microfractures and lead to avascular necrosis of the lunate (Kienböck's disease). This may result in eventual collapse of the lunate and associated arthritis. See the separate Kienböck's Disease article.
Diagnosis: local tenderness to palpation is usual following an acute fracture. Suspect Kienböck's disease in someone who complains of central dorsal wrist pain, reduced grip strength and reduced wrist movement.
Management: immobilisation, stress reduction, revascularisation and lunate replacement are management options, depending on the severity and pattern of fracture.
Hamate fracture
The hook or the body of the hamate bone may be fractured but they are relatively rare carpal fractures (2% of all carpal fractures)9 .
Usual mechanism of injury: may be caused by a fall on to the outstretched hand. Often occurs when the patient falls while holding an object and the object lands between the ground and the ulnar side of the palm. Can follow direct trauma to the hypothenar eminence. The most frequent causes of fractures of the hamate hook are sports that require a strong grip such as golf and baseball, where an abnormal swing causes the handle to impact against the bone9 .
Diagnosis: pain is usually felt on the ulnar aspect of the palm or dorsoulnar aspect of the wrist, and is worsened by gripping. Grip strength may be reduced. Test the ulnar nerve as this is closely associated. Carpal tunnel X-ray view may be needed to detect hook fractures10 . CT scanning is also helpful. Scaphoid fracture is associated with higher-than-expected rates of concomitant hook of hamate fracture11 . These fractures are often minimally displaced, hence easily overlooked on CT. MRI may therefore be superior when investigating radiographically occult scaphoid fractures.
Management: non-displaced fractures are treated conservatively by cast immobilisation for six weeks. Displaced fractures usually require open reduction and internal fixation. Displaced fractures of the hook of the hamate are managed by early excision. There may otherwise be avascular changes after hook fractures which can lead to necrosis and non-union of the hamate hook12 .
Trapezium fracture
This is the third most common carpal fracture.
Usual mechanism of injury: direct blow to the dorsum of the hand or a fall on to a radially deviated closed fist.
Diagnosis: point tenderness over the trapezium. The patient complains of a weak and painful pinch grip. Carpal tunnel X-ray views may be needed.
Management: treated conservatively if non-displaced. A thumb spica cast is usually used. Displaced fractures are usually treated surgically. Trapezial ridge fractures may require surgical intervention.
Other carpal bone fractures
Other carpal bones are very rarely fractured. Fracture can occur with a powerful direct force, and multiple fractures are possible. Undisplaced fractures are usually treated conservatively. Surgery is often required for displaced fractures. Comminuted pisiform fractures require early excision to promote uncomplicated recovery.
Complications of carpal bone fractures
Most carpal bone fractures heal without complication. Early complications include:
Stiffness, pain or aching which is usually (but not always) short-lived.
Carpal osteoarthritis, which can be a late complication.
Continue reading below
Carpal dislocations
These are rare but devastating injuries. They can be associated with a carpal fracture. Fracture dislocations are twice as common as pure ligamentous dislocations. Isolated carpal dislocations are rare.
They include perilunate dislocations, trans-carpal fracture dislocations, radiocarpal dislocations, axial or longitudinal dislocations, and the rare isolated carpal bone dislocations.
The most common carpal dislocations are the lunate, the lunate with a scaphoid fracture, and perilunate dislocation.
Perilunate dislocations result from dislocation of the distal carpal row. Scaphoid fractures often accompany perilunate dislocation.
Carpal dislocations can lead to chronic pain and wrist instability. They are difficult to diagnose and are often missed.
Usual mechanism of injury
They most often result from high-energy trauma such as motor vehicle accidents, high-impact falls from a height on to an outstretched hand with rotation/wrist deviation, or industrial-related accidents.
Examination
The patient may just have diffuse wrist pain and diffuse tenderness to palpation. There may be associated swelling.
Vascular and neurological integrity of the hand should be checked and documented.
Investigations
AP X-ray view
When looking at the AP view to diagnose carpal dislocations, one approach is to imagine three arcs:
The first arc is formed by connecting the proximal articular margins of the proximal carpal row (the scaphoid, lunate and triquetrum).
The second arc is formed by connecting the distal articular margins of the same proximal carpal row.
The third arc is formed by joining the proximal articular margins of the capitate and hamate.
Any disruption of these parallel lines indicates subluxation or dislocation of the carpal bones.
Lateral X-ray view
There is normally a column seen with the radius below, then the lunate sitting in the radius cup and the capitate sitting in the lunate cup. If this column alignment is lost, it can mean a lunate or perilunate dislocation.
Management
The wrist should be rapidly immobilised with a cast, even if no injury is obvious on X-ray. Splinting should be to the fingertips.
Where carpal dislocation has occurred, or is suspected, urgent referral for orthopaedic opinion is necessary. Adequate analgesia should be given.
Minor dislocations may be treated by closed reduction; more complex injuries usually require open reduction and internal fixation.
Closed reduction is performed acutely, followed by open reduction and ligamentous and bony repair with internal fixation.
Complications
Complications include post-traumatic arthrosis, median nerve dysfunction, complex regional pain syndrome, tendon problems, and carpal instability.
Despite appropriate treatment, loss of wrist motion and reduced grip strength are common, as is persistent pain.
Dr Mary Lowth is an author or the original author of this leaflet.
Further reading and references
- Spiry C, Bacle G, Marteau E, et al; Radiocarpal dislocations and fracture-dislocations: Injury types and long-term outcomes. Orthop Traumatol Surg Res. 2018 Apr;104(2):261-266. doi: 10.1016/j.otsr.2017.12.016. Epub 2018 Feb 8.
- Ribeiro LM, Botton MA; Isolated Trapezoid Fracture in a Boxer. Am J Case Rep. 2019 Jun 5;20:790-793. doi: 10.12659/AJCR.915757.
- Gil JA, Weiss AC; The Weekend Warrior: Common Hand and Wrist Injuries in Athletes. R I Med J (2013). 2020 Sep 1;103(7):49-53.
- You JS, Chung SP, Chung HS, et al; The usefulness of CT for patients with carpal bone fractures in the emergency department. Emerg Med J. 2007 Apr;24(4):248-50.
- Stogner VA, Kaltenborn A, Laser H, et al; Hand injuries in sports - a retrospective analysis of 364 cases. BMC Musculoskelet Disord. 2020 Dec 8;21(1):826. doi: 10.1186/s12891-020-03807-z.
- Orces CH, Martinez FJ; Epidemiology of fall related forearm and wrist fractures among adults treated in US hospital emergency departments. Inj Prev. 2011 Feb;17(1):33-6. doi: 10.1136/ip.2010.026799. Epub 2010 Sep 28.
- Rhemrev SJ, Ootes D, Beeres FJ, et al; Current methods of diagnosis and treatment of scaphoid fractures. Int J Emerg Med. 2011 Feb 4;4:4. doi: 10.1186/1865-1380-4-4.
- Capitate; Wheeless' Textbook of Orthopaedics
- Triquetrium; Wheeless' Textbook of Orthopaedics
- Lunate; Wheeless' Textbook of Orthopaedics
- Guo W, Yuan B, Zhu Z, et al; Non-dislocation lunate fracture combined with distal radius fracture: A case report. Medicine (Baltimore). 2018 Dec;97(49):e13574. doi: 10.1097/MD.0000000000013574.
- Kim H, Kwon B, Kim J, et al; Isolated hook of hamate fracture in sports that require a strong grip comprehensive literature review. Medicine (Baltimore). 2018 Nov;97(46):e13275. doi: 10.1097/MD.0000000000013275.
- Hamate; Wheeless' Textbook of Orthopaedics
- Mandegaran R, Gidwani S, Zavareh A; Concomitant hook of hamate fractures in patients with scaphoid fracture: more common than you might think. Skeletal Radiol. 2018 Apr;47(4):505-510. doi: 10.1007/s00256-017-2814-3. Epub 2017 Nov 16.
- Xiao ZR, Zhang WG, Xiong G; Features of intra-hamate vascularity and its possible relationship with avascular risk of hamate fracture. Chin Med J (Engl). 2019 Nov 5;132(21):2572-2580. doi: 10.1097/CM9.0000000000000417.
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 27 Jul 2026
28 Jul 2021 | Latest version

Feeling unwell?
Assess your symptoms online for free