Coronary angiography
Peer reviewed by Dr Adrian Bonsall, MBBSLast updated by Dr Colin Tidy, MRCGPLast updated 9 Aug 2017
Meets Patient’s editorial guidelines
This page has been archived.
It has not been reviewed recently and is not up to date. External links and references may no longer work.
Coronary angiography is a specialised X-ray test to find out detailed information about your heart (coronary) arteries. It is mainly used if you have angina, to assess which if any of the arteries are blocked, and how severely the arteries are blocked. It involves a procedure called catheterisation.
In this article:
Coronary arteries do not show up on a plain X-ray. With coronary angiography, dye is injected down the coronary arteries. The arteries and their smaller branches then show up clearly on an X-ray 'like a road map'. Dye is injected into the coronary arteries by using a catheter. (A catheter is a thin, flexible, hollow tube.)
Coronary angiography can show the exact site and severity of any narrowing of the coronary arteries. This helps the doctor to decide on what treatment you may need. For example, if the narrowing is mild and does not need surgery; or, if the narrowing is severe and you should have a coronary artery bypass graft or coronary angioplasty.
Computerised tomography (CT) coronary angiogram
A CT coronary angiogram shows the blood flow through the coronary arteries. This test is similar to a traditional coronary angiogram that uses X-rays but the dye is injected into a small vein in your arm rather than an artery in your groin. A CT coronary angiogram is not as good as a traditional coronary angiogram at detecting narrowing of small coronary arteries. The CT coronary angiogram is useful to rule out the diagnosis of coronary heart disease (eg angina) and useful if you might have heart failure or an abnormality in the structure of your heart. See separate leaflet called CT Scan for more general information.
i3_l.jpg
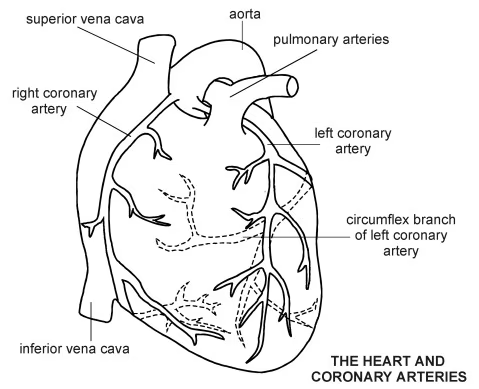
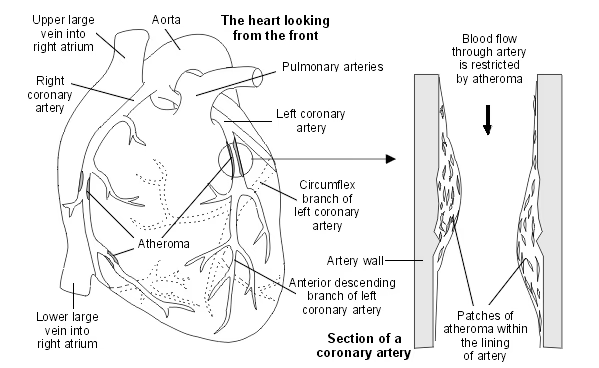
Heart with atheroma
Continue reading below
How is coronary angiography done?
You lie on a couch in a catheterisation room. An X-ray machine is mounted above the couch. A thin, flexible tube (a catheter) is inserted through a wide needle or small cut in the skin into a blood vessel in the groin or arm. Local anaesthetic is injected into the skin above the blood vessel. Therefore, it should not hurt when the catheter is passed into the blood vessel.
Coronary angiography
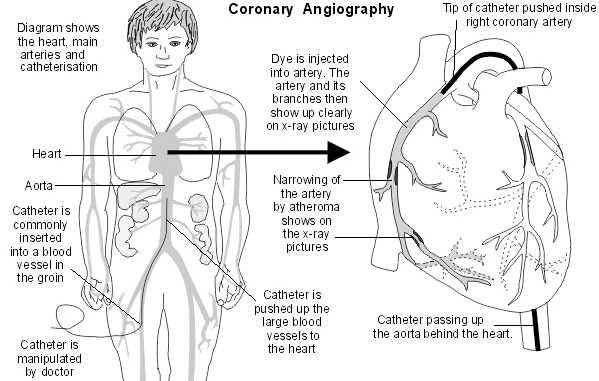
The doctor gently pushes the catheter up the blood vessel towards the heart. Low-dose X-rays are used to monitor the progress of the catheter tip which is gently manipulated into the correct position. You may be able to see the progress of the catheter on the X-ray monitor.
The tip of the catheter is pushed just inside a main coronary artery. Some dye is then injected down the catheter into the artery. Several X-ray films are rapidly taken as the dye is injected (the dye shows up clearly on X-ray films). The X-ray films are recorded as a moving picture and this is called an angiogram. The angiogram shows the vessels filling with blood and the sites of any narrowing can be seen.
The tip of the catheter is then put into the other main coronary artery and the test is repeated. So, an angiogram picture is built up of each of the coronary arteries and their branches.
You cannot feel the catheter inside the blood vessels. You may feel an occasional 'missed' or 'extra' heartbeat during the procedure. This is normal and of little concern. During the procedure your heartbeat is monitored by electrodes placed on your chest which provide a tracing on an electrocardiograph (ECG) machine. Sometimes a sedative is given before the test if you are anxious.
When the test is over, the catheter is gently pulled out. If it was inserted through a small cut in the skin in the arm then you will normally need a few stitches. If it was inserted through a wide needle in your groin then a nurse will press over the site of insertion for about 10 minutes to prevent any bleeding.
How do I prepare for a coronary angiography?
You should receive instructions from your local hospital about what you need to do in the days leading up to the test. The sort of instructions may include:
Before the day of the test you may need a blood test and an ECG to make sure you are OK to have the procedure.
If you take a 'blood-thinning' medicine (anticoagulant), such as warfarin, you are likely to need to stop this for 2-3 days before the test. (This prevents excessive bleeding from the site of the small, flexible tube (catheter) insertion.)
If you take insulin or medicines for diabetes, the timing of when to take these on the day of the test may need to be clarified.
If you may be pregnant, you need to tell the doctor who will do the test.
You may be asked to stop eating and drinking for a few hours before the test.
You may be asked to shave both groins before the test.
You will have to sign a consent form at some point before the test to confirm that you understand the procedure, understand the possible complications (see below) and agree to the procedure being done.
Continue reading below
How long does coronary angiography take?
It usually takes about 30 minutes. In most cases it is done as a day-case procedure.
After the test
The doctor will discuss what he or she found during the test. A letter is also sent to your GP giving details of the test results.
You will need to rest for a few hours after the test. You should ask a friend or relative to accompany you home. Most people are able to resume their normal activities the next day.
There may be some bruising at the site of the small, flexible tube (catheter) insertion which may be a little sore when the anaesthetic wears off. Painkillers such as paracetamol will help to ease this.
You may need to have some stitches removed after about seven days if a small cut was made to insert the catheter.
Continue reading below
Are there any risks or side-effects?
Most of the side-effects are minor and may include:
A bruise, which may form under the skin where the small, flexible tube (catheter) was inserted (usually the groin). This is not serious but it may be sore for a few days.
The small wound where the catheter is inserted sometimes becomes infected. Tell your GP if the wound becomes red and tender. A short course of antibiotics will usually deal with this if it occurs.
Some people have a short angina-type pain during angiography. This soon goes.
The dye may give you a hot, flushing feeling when it is injected. Many people also describe a warm feeling in the groin when the dye is injected - as if they have 'wet themselves'. These feelings last just a few seconds (and the operator will tell you when they are about to inject the dye). Rarely, some people have an allergic reaction to the dye.
Serious complications are rare. Some people have a stroke or a heart attack (myocardial infarction) during the procedure. Also, rarely, the catheter may damage a heart (coronary) artery. The risk of serious complications is small and is mainly in people who already have serious heart disease. As a consequence of serious complications, some people have died during this procedure. Your doctor will only recommend coronary angiography if they feel the benefits outweigh the small risk.
Further reading and references
- CT coronary angiography in patients with suspected angina due to coronary heart disease (SCOT-HEART): an open-label, parallel-group, multicentre trial; Lancet. 2015 Jun 13;385(9985):2383-91. doi: 10.1016/S0140-6736(15)60291-4. Epub 2015 Mar 15.
- Moss AJ, Newby DE; CT coronary angiographic evaluation of suspected anginal chest pain. Heart. 2015 Dec 8. pii: heartjnl-2015-307860. doi: 10.1136/heartjnl-2015-307860.
- Skelly AC, Hashimoto R, Buckley DI, et al; Noninvasive Testing for Coronary Artery Disease. Agency for Healthcare Research and Quality (US); 2016 Mar.
- Goyal N, Stillman A; Coronary CT angiography in acute chest pain. F1000Res. 2017 Jul 13;6:1125. doi: 10.12688/f1000research.11250.1. eCollection 2017.
Article History
The information on this page is written and peer reviewed by qualified clinicians.
9 Aug 2017 | Latest version

Feeling unwell?
Assess your symptoms online for free