Acute kidney injury
Peer reviewed by Dr Adrian Bonsall, MBBSLast updated by Dr Colin Tidy, MRCGPLast updated 31 Aug 2016
Meets Patient’s editorial guidelines
This page has been archived.
It has not been reviewed recently and is not up to date. External links and references may no longer work.
Acute kidney injury is a condition where your kidneys suddenly stop working properly. Usually this happens when you are unwell from another illness. If you have acute kidney injury you are often already ill in hospital. If not, you will usually be sent to hospital to be looked after. The earlier acute kidney injury is picked up, and the more carefully you are monitored, the better the chance of your kidneys recovering.
Acute kidney injury used to be called acute renal failure.
In this article:
Continue reading below
Understanding kidneys: where they are and what they do
Cross-section diagram of the urinary tract
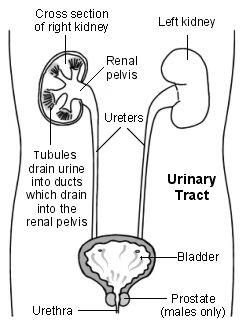
The two kidneys lie to the sides of the upper part of the tummy (abdomen), behind the intestines, and either side of the spine. Each kidney is about the size of a large orange but bean-shaped.
Patient picks for Other kidney problems
A large artery - the renal artery - takes blood to each kidney. The artery divides into many tiny blood vessels (capillaries) throughout the kidney. In the outer part of the kidneys tiny blood vessels cluster together to form structures called glomeruli.
Each glomerulus is like a filter. The structure of the glomerulus allows waste products and some water and salt to pass from the blood into a tiny channel called a tubule. The liquid that remains at the end of each tubule is called urine. The urine then passes down a tube called a ureter which goes from each kidney to the bladder. Urine is stored in the bladder until it is passed out when we go to the toilet.
The main functions of the kidneys are to:
Filter out waste products from the bloodstream, to be passed out in the urine.
Help control blood pressure - partly by the amount of water passed out of the body as urine and partly by making hormones which are involved in blood pressure control.
Make a hormone called erythropoietin, which stimulates the bone marrow to make red blood cells. This is needed to prevent anaemia.
Control the amount of fluid in the body.
Help keep various salts and chemicals in the blood at the right level.
What is acute kidney injury (AKI)?
If you have AKI your kidneys suddenly stop working as well as they should. This means the fluid, salts and chemicals in your body can rise or fall to abnormal levels and make you very ill. If there is too much acid, or there are too many salts, in your body your other organs can be affected. For example, your heart, lungs, brain, muscles, eyes, etc, can stop working properly. If the kidneys aren't getting rid of enough fluid, your body can become overloaded with it. This can cause swelling in your legs, or make it difficult to breathe.
It is different from chronic kidney disease (CKD) which is a much more gradual process which can happen over many years.
Continue reading below
How common is acute kidney injury (AKI)?
In people who are unwell in hospital, AKI is common. Nearly as many as 1 in 5 people in hospital develop AKI. It is even more common in patients who are extremely unwell in intensive care units.
Who develops acute kidney injury (AKI)?
AKI is more common over the age of 65. People who have another serious illness and are in hospital are more likely to develop it. It may happen to people who are having operations, especially if they are older. It may happen to some people who are having a special X-ray with a dye (contrast) which contains iodine.
Some things make you more likely to develop AKI in these situations - for example:
Being older.
Having another illness like diabetes, heart failure or liver disease.
Being dependent on a carer for fluids.
Having a bad infection (for example, from a urinary infection, chest infection or skin infection).
Some medicines - for example:
Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, diclofenac or naproxen.
Some blood pressure pills that work on the kidney.
Some antibiotics called aminoglycosides (such as gentamicin).
'Water tablets' (diuretics).
Lacking in fluid in the body (being dehydrated).
Another problem with your kidneys, such as CKD.
Having had AKI before.
Children can develop AKI too. This is more likely if they have:
Severe diarrhoea.
A cancer of the blood cells.
To rely on a parent or carer for fluids (more likely to become dehydrated).
Low blood pressure.
Another kidney illness such as nephritis.
A severe infection.
Continue reading below
What causes acute kidney injury (AKI)?
There are many things that can cause the kidneys to stop working properly. Sometimes it happens due to more than one cause.
Causes include:
Severe infections.
Blockage in the urinary system.
Lack of fluid in the body (dehydration).
Heavy bleeding (haemorrhage).
Low blood pressure.
Some medicines (see previous section for medicines that can harm the kidneys).
Kidney diseases.
The dye (contrast) that is used for some kinds of scans and X-rays.
What are the symptoms of acute kidney injury (AKI)?
There may be no specific symptoms of AKI. Often you already have symptoms of the illness that has caused AKI.
Symptoms that may happen include:
Passing less urine than usual.
Feeling sick or being sick (vomiting).
Poor appetite.
Breathlessness.
Swelling in the legs or other parts of the body.
How is acute kidney injury (AKI) diagnosed?
Your doctor would test for AKI with urine tests and blood tests. Your urine will be measured to see how much you are passing. In most people with AKI, this is less than normal. It will also be tested with a 'dipstick' to check for protein, blood cells and sugar, amongst other things. This will help work out the cause. You will have a blood test for a substance called creatinine. This is an indicator for how well the kidneys are working. Higher levels mean that the kidneys aren't getting rid of waste products as effectively as they should.
You may need an ultrasound scan to look for blockages in the urinary system. Ultrasound scans use sound waves to create a picture of the kidneys and urinary system.
You may also need other tests to try to find the cause for AKI. These might include other blood tests, scans or X-rays.
How is acute kidney injury (AKI) treated?
There isn't a specific medicine to treat AKI. The treatment will depend on the cause of AKI and the severity of the AKI.
The treatment is to carefully look after all the things the kidneys usually do. You will normally be in hospital and have blood and urine tests regularly. You may need extra or special fluid through a drip. You may be on a restricted diet to help get the balance of proteins and salts right. Any medicines which might be harming your kidneys would be stopped. The cause of the problem would be treated if this is possible. (For example, you might need antibiotics for an infection or surgery for any blockage if these were the cause.)
Your doctor will keep a close eye on the balance of minerals and salts in your body. You will have regular tests for potassium, sodium, calcium, sugar (glucose), phosphate and creatinine. You may need treatment with medicines or through a drip if the levels are not right.
Sometimes you need to have dialysis if medicines and fluids aren't working and you are becoming more ill. Dialysis is a procedure where your blood is passed through a machine to remove the waste products (as your kidneys would do if they were working). There are different ways this is done. How often it is done and how long each session lasts will depend on the way it is done. You would be referred to a kidney specialist or an intensive care specialist for this. In most people this can be stopped once the kidneys are working properly again.
These decisions would be made after discussion with you and explaining the options to you (and/or your relatives or carers where appropriate).
What is the outlook (prognosis)?
The outlook varies hugely. It depends on how bad kidney function becomes, who is looking after you, the cause of the problem and how ill you were to begin with.
The National Institute for Health and Care Excellence (NICE) has produced guidelines to try to cut the numbers of people who develop acute kidney injury (AKI) and who die because of it. The outlook is better if it is picked up earlier.
Many people who recover from AKI have normal kidney function afterwards. However, some go on to develop chronic kidney disease (CKD). Some need to keep having dialysis. If you have had AKI once, you are more likely to have it again in the future.
How can acute kidney injury (AKI) be prevented?
Prevention is certainly better than cure for AKI. Patients in hospital should be tested for AKI regularly. This is done by frequent blood tests and measuring how much urine they produce (and weight for children). People having scans or X-rays with a dye (contrast) should be checked to see how likely they are to develop AKI. If they are at risk, and if the test is really necessary, the chances of AKI are lower if these patients have a drip with extra fluid first. They should be regularly checked after the test.
Medicines which cause kidney damage should be avoided where it is possible. If they can't be avoided, the lowest possible dose should be used and tests done regularly to keep a check on how the kidneys are coping.
Further reading and references
- Acute Kidney Injury; Renal Association (2011)
- Acute kidney injury - Prevention, detection and management of acute kidney injury up to the point of renal replacement therapy; NICE Guidelines (Aug 2013)
- Clinical practice guideline for acute kidney injury; KDIGO (Kidney Disease: Improving Global Outcome), 2012
- Northern Ireland Guidelines for Acute Kidney Injury; Guidelines And Audit Implementation Network (2014)
Article History
The information on this page is written and peer reviewed by qualified clinicians.
31 Aug 2016 | Latest version

Feeling unwell?
Assess your symptoms online for free
