Granuloma annulare
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 15 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is granuloma annulare?
Granuloma annulare is a benign inflammatory condition of unknown aetiology with dermal papules and annular plaques. Histology reveals foci of degenerative collagen with palisaded granulomatous inflammation.1
A number of variants of the condition are recognised:2
Localised.
Generalised.
Subcutaneous.
Perforating.
Granuloma annulare causes (aetiology)
Back to contentsAetiology is essentially not known. Associations with systemic illnesses including diabetes, thyroid disease, malignancy and hyperlipidaemia have been suggested but not proven.3 It is thought to be due to a delayed hypersensitivity reaction to some part of the dermis with inflammation mediated by tumour necrosis factor alpha (TNF alpha).4
Continue reading below
How common is granuloma annulare? (Epidemiology)2 3
Back to contentsIt is a not uncommon condition but UK figures on incidence are not available. Granuloma annulare has an incidence of 0.04% in the USA, and has shown to be significantly associated with autoimmune disease, diabetes mellitus, and hyperlipidaemia.5
Localised is the most common type, accounting for around three quarters of all cases. This type is usually found in those under 30 years old. Lesions are typically localised to the dorsal surfaces of hands and/or feet. It is usually self-limiting within two years.
The generalised form includes generalised annular, disseminated papular and atypical generalised subtypes. It represents about 10-15% of cases. There are 10 or more lesions. It tends to last for longer and be more likely to require treatment. It usually occurs in adults, and may occur particularly around the skin folds of the trunk.
Subcutaneous granuloma annulare is most often seen in children, particularly between the ages of two and five. These may be mistaken for rheumatoid nodules.
Perforating granuloma annulare is the least common type. It occurs most often in children and young adults. There can be both localised and generalised forms. These are more likely to be symptomatic, causing pain or itch.
History
Back to contentsBoth localised and generalised varieties are usually asymptomatic. The subcutaneous variety may become a large subcutaneous mass. Lesions may be stable for months and then enlarge over weeks. Perforating types may present with pain or itch.
Continue reading below
Examination
Back to contentsLocalised lesions are usually groups of papules, about 1-2 mm in diameter with possible erythema. They tend to form an arc or a ring 1-5 cm in diameter. The centre of lesions may be slightly depressed and hyperpigmented. They are usually on the dorsal surfaces of hands, feet and fingers and the extensor surface of arms and legs.
Granuloma annulare
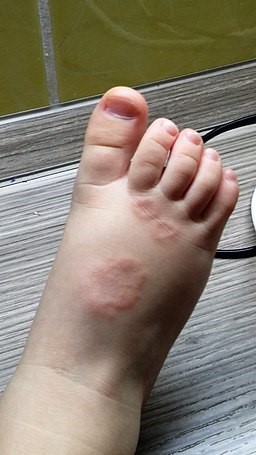
© Mravlja Matjaz, CC BY-SA 4.0, via Wikimedia Commons
The generalised variety has a similar appearance to the localised lesions but they are more numerous and more diffuse. They may coalesce into annular plaques 3-6 cm in diameter and these can expand over weeks or months. They tend to be on the limbs or the trunk. Subcutaneous lesions are firm, skin-coloured or pink, and not tender, and the overlying skin looks normal. They are usually solitary lesions but can occur in clusters. The lower limb, especially the pretibial surface is the most common area. Lesions are mobile, except on the scalp.
Generalised granuloma annulare of leg
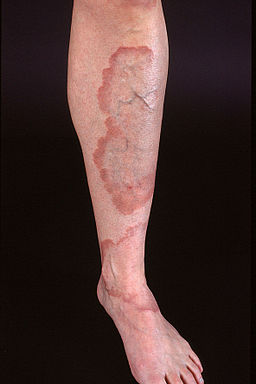
© Kreuter et al, My Core Competency is Competencyat en.wikipedia, CC BY-SA 2.0,via Wikimedia Commons
Perforating lesions are papules 1-4 mm in diameter with possibly some degree of erythema. They may be solitary or number in hundreds but often coalesce to form annular plaques. They tend to be larger and more ulcerated where they occur in middle-aged or elderly people and the lesions may leave hyperpigmented or hypopigmented scars. They tend to be on the extensor surface or lower arms or legs or the dorsal surface of hands. 'Perforating' refers to the histological appearance of the degenerating collagen fibres, rather than the clinical appearance.
Investigations
Back to contentsDiagnosis is essentially clinical and laboratory tests are not helpful unless another diagnosis is suspected. If in doubt, biopsy may be helpful.
Differential diagnosis2
Back to contentsMany annular skin lesions may be mistaken for granuloma annulare. Differential diagnosis includes:
In granuloma annulare, there are no surface changes to the skin. There is no scale, there are no vesicles or pustules, and the skin surface is smooth.
Granuloma annulare treatment2 3 5
Back to contentsThe local type does not usually require treatment, as it is asymptomatic and self-limiting. The generalised type may produce cosmetic embarrassment and require intervention. However, there is no evidence-based therapy available.
Options for localised lesions include:
Topical and intralesional corticosteroids are considered first-line therapies and can induce partial or complete regression in some patients.
Other therapies that may be tried include cryotherapy and laser ablation.
Generalised disease is not so amenable to the steroid treatment and is also less likely to resolve spontaneously. Systemic treatments have been disappointing. There are many options, none of which has a solid evidence base. They include:
Psoralen combined with ultraviolet A (PUVA) treatment.
Oral steroids.
Dapsone.
Ciclosporin and methotrexate.
Antibiotic combinations such as minocycline plus rifampicin plus ofloxacin.1
Antimalarials, such as hydroxychloroquine.
Isotretinoin.
The TNF inhibitor infliximab - may be useful in recalcitrant cases.6 7 Adalimumab has also been reported to be effective.8
With subcutaneous lesions in children, the best management is reassurance, although they can be excised surgically. Treatment of perforating lesions is disappointing.
Prognosis2
Back to contentsMost cases of localised granuloma annulare are self-limiting. Half of all cases will settle within two years. 40% of children have recurrent lesions.
The prognosis for generalised disease is worse, with some having a chronic course lasting up to 10 years, poor response to treatment, low chance of spontaneous remission and high risk of recurrence. Subcutaneous lesions often resolve spontaneously but may recur elsewhere.
Further reading and references
- Marcus DV, Mahmoud BH, Hamzavi IH; Granuloma annulare treated with rifampin, ofloxacin, and minocycline combination therapy. Arch Dermatol. 2009 Jul;145(7):787-9. doi: 10.1001/archdermatol.2009.55.
- Cyr PR; Diagnosis and management of granuloma annulare. Am Fam Physician. 2006 Nov 15;74(10):1729-34.
- Thornsberry LA, English JC 3rd; Etiology, diagnosis, and therapeutic management of granuloma annulare: an update. Am J Clin Dermatol. 2013 Aug;14(4):279-90. doi: 10.1007/s40257-013-0029-5.
- DermNet NZ: Granuloma annulare
- Joshi TP, Duvic M; Granuloma Annulare: An Updated Review of Epidemiology, Pathogenesis, and Treatment Options. Am J Clin Dermatol. 2022 Jan;23(1):37-50. doi: 10.1007/s40257-021-00636-1. Epub 2021 Sep 8.
- Hertl MS, Haendle I, Schuler G, et al; Rapid improvement of recalcitrant disseminated granuloma annulare upon treatment with the tumour necrosis factor-alpha inhibitor, infliximab; Br J Dermatol 2005 Mar;152(3):552-5.[abstract]
- Murdaca G, Colombo BM, Barabino G, et al; Anti-tumor necrosis factor-alpha treatment with infliximab for disseminated granuloma annulare. Am J Clin Dermatol. 2010 Dec 1;11(6):437-9. doi: 10.2165/11311040-000000000-00000.
- Werchau S, Enk A, Hartmann M; Generalized interstitial granuloma annulare--response to adalimumab. Int J Dermatol. 2010 Apr;49(4):457-60. doi: 10.1111/j.1365-4632.2010.04348.x.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Dec 2027
15 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free