newborn experience with jejunum atresia
Posted , 3 users are following.
My daughter was born with jejunum atresia. I am sharing my experience starting from diagnostic until her hospital discharge with hope that this read would be helpful for other parents in similar situation.
Initial Diagnostic:
During the last pregnancy scans of my wife, Gynaecologist noticed abnormal enlargement of a part of baby intestine, she warn us of the possible problem and recommend us to undertake the delivery at hospital with specialised Paediatric and child surgery facility.
Baby Delivery:
As per the recommendation, we undertook the delivery at Frankfurt Hochst Krankenhaus. Baby was born normally however soon after the birth baby vomited out the excreta (black greenish). We informed the nursing staff about the possible problem however they didnt took us seriously until baby vomit again the second time 20-25 minutes later. They called the doctor on duty who took baby away for further examination.
Confirmation:
Around an hour later Doctors confirmed us the problem of complete intestine blockage in baby and need for immediate operation to remove blockage. They were not sure of the number of blockages, which can only be known during the operation and so would the procedure of correction.
Operation took around 4 hours after which they confirmed that there was only one blockage in Jejunum and they successfully removed it. As the part of intestine after blockage never actually developed, they couldnt join both ends and had to create two opening on the stomach (with intestine ends stitched) from which they want to manually feed output of first one into other to let the other one grow until they can be rejoined.
Problem:
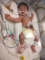
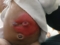
Post operation baby was kept in ICU and a bag is attached on upper intestine end to collect the excreta (picture below)
Here food intake was reduced to 1ml and was increased depending on how well she was passing it out. She was always given glucose along with anaesthesia and antibiotics to prevent infection.
Problem:
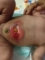
One week post operation, baby broke some of her stitches due to her movement, this created uneven surface which posed challenges in sticking the collecting bottle. it was realised that her excreta from intestine was getting spilled out of collecting bottle onto her stomach which was resulting into skin burning (due to acidic nature of excreta). Burnt skin made it impossible to stick the bottle altogether resulting into even greater skin burn and started a recursive process of skin burn and excreta spill.
Meanwhile the spilled excreta also started getting inside stomach from place of raptured/broken stitches. Possibility of new stitches were denied by surgeon, moreover attempts to block hole with cotton and other things didn't yielded any positive results.
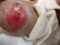
Yellow patch is the hole plugged with cotton (cotton after getting smeared with excreta was proving further harmful)
HoD of surgery department suggested to put sugar inside the hole to reduce the impact of acidic excreta.
Further as excreta was not getting collected during this time, there was no feed into other undeveloped intestine and hence no improvement in its size.
2 weeks passed and there was no improvement, besides the problem was aggravating.
Different methods were tried to make pouch hold its place atop burnt skin and stop excreta from spilling like methods employed to treat second/third degree burn and use of special 3M bottles, power, creams and bandages however none showed any improvement.
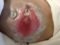
Nurses were instructed to remove excreta from skin immediately however still no improvement as excreta was not getting removed immediately (delay in removal during night, shift change, other emergency etc.). photos below with increased burn size:
I and my wife, decided to stay alongside baby full time to remove excreta and moist immediately. We monitored baby 24 hours a day, sleeping in turns to ensure that she is not left unattended any minute. Our efforts paid off and after 3-4 days itself, we saw the healing signs on skin. After a week and half, burnt was going off and special 3M adhesive bottles were able to stick. Precise incision was required on bottle opening, this prevented further leak, bottles were required to be replaced as soon as they were coming off or making space for leak, i.e. every 4-5 hours.
Continuation:
After championing the above problem, we were able to collect excreta in bottle and this was pumped into other side at regular intervals of 3 hours. Size of undeveloped intestine started to increase however yet not in proportion that it can be switched together and the process continued.
After around 1.5 months since she was born with the problem, doctors declared that size of both ends to be in proportion for stitching together. Blood test before operation came with surprise that her hemoglobin was low and blood transfusion was required before operation. 2 week of further delay was added in the process.
After 2 months our daughter came home, she is 7 months now and is doing good, we take her for checkup every three months.
1 like, 3 replies


jenny1910 gargdeepesh
Posted
Am so sorry you have to go through all these and at last conquer every challenges.
Gute besserung to Ur daughter and alles gute to you and Ur wife.
God is faithful.
Stay healthy..
mandmmom gargdeepesh
Posted
gargdeepesh mandmmom
Posted
I wish you all the very best with your kid, God bless.
Please feel free to let us know if you have more questions and we will answer as per best of our knowledge.