Eosinophilic oesophagitis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Laurence KnottLast updated 14 May 2021
Meets Patient’s editorial guidelines
The oesophagus is the gullet, or food pipe, that connects the mouth to the stomach. Inflammation of the oesophagus is known as oesophagitis. Commonly, the inflammation is caused by acid leaking up from the stomach (a condition known as acid reflux). In some people, however, it can be caused by a condition known as eosinophilic oesophagitis. In eosinophilic oesophagitis, particular types of white blood cells (called eosinophils) gather in large numbers in the lining of the oesophagus, causing inflammation. It occurs in children and in adults. The condition can be controlled by making changes to your diet and/or taking steroids. Occasionally, an operation to stretch the oesophagus through a telescope (endoscope) may be needed.
In this article:
Continue reading below
What is eosinophilic oesophagitis?
Oesophagitis means inflammation of the gullet or oesophagus. In eosinophilic oesophagitis (EO) lots of white cells called eosinophils can be seen in the oesophageal lining. EO is thought to occur due to a combination of genetic makeup and the body's response to the environment. If you have EO you may be allergic to certain foods, although tests do not always identify the specific foods causing the problem. You are also more likely to have other allergies such as asthma or hay fever.
What are the symptoms of eosinophilic oesophagitis?
The symptoms of EO vary depending on whether you are an adult, a teenager or a child. If you are an adult you may notice difficulty in swallowing (dysphagia) and have the feeling that food is sticking in the gullet. If you are a teenager you may start being sick (vomiting) and have chest or stomach pain. These symptoms are similar to those of people who have acid reflux (also known as gastro-oesophageal reflux disease). If your child has EO, you may notice that they refuse food and fail to gain weight.
Continue reading below
What are the treatments for eosinophilic oesophagitis?
Dietary manipulation
You may be advised to alter your diet, either as the main treatment for your EO or in addition to other treatment. Dietary manipulation may involve cutting out certain foods to which you may be allergic.
Sometimes food allergy tests may be able to identify which foods to avoid but these tests do not always provide the answer. If your allergy tests are not helpful, you may be advised to avoid the types of food which are well known to cause allergic reactions. Common foods that can do this include nuts, seafood, milk, egg, wheat and soya products. A dietician and/or an allergy specialist may be involved in giving you advice about what changes to your diet you need to make,
Usually you need to avoid these foods for about six weeks and then gradually reintroduce them one by one. Another approach, most commonly used in children, is to try a specially made-up mixture of basic food chemicals called amino acids. This mixture needs to be taken instead of food for about six weeks. Your child may not like the taste of the mixture and it may be difficult to persevere with this treatment. However, it is particularly useful if your child has a severe form of EO which is difficult to control.
Steroids
Steroids such as fluticasone are often recommended, with or without dietary manipulation. They are usually prescribed in the form of an inhaler. It is the same type of inhaler as that used by patients with asthma. However, you will be asked to spray the inhaler into your mouth without breathing in and to swallow the powder without water. You should not eat food or drink liquids for half an hour after spraying the medicine. Another type of steroid called budesonide is also available in liquid form. The liquid form is not specially made for people with EO but comes in small plastic containers called budesonide respules which are used by asthma patients. This can be mixed with a sweetener called sucralose, or with honey or chocolate syrup. This is a particularly useful option for children who have problems with the inhaler method.
Editor’s note
Dr Sarah Jarvis, 5th July 2021
Orodispersible budesonide tablets
The National Institute for Health and Care Excellence (NICE) has published new guidance on the use of budesonide in orodispersible tablet form. These are tablets which dissolve in your mouth - they are sometimes called orally disintegrating tablets.
The committee recommends that these tablets should be offered as an option for treating eosinophilic oesophagitis in adults only. They should be used for people with eosinophilic oesophagitis in order to bring about remission (ie to relieve symptoms).
Gastroscopy (endoscopy)
You may need to have a gastroscopy using an endoscope if dietary manipulation or steroids do not work. You may also need endoscopy if you develop a complication of EO such as narrowing of the oesophagus.
Who does eosinophilic oesophagitis affect?
Most people with EO are white men between the ages of 30-50 years. However, the condition can occur in all ages and in both sexes. Men are three times more likely than women to be affected. For unknown reasons, it has become more common in recent years, currently affecting about 7 in 100,000 people every year.
Continue reading below
How is eosinophilic oesophagitis diagnosed?
If you are suspected of having EO, you will need to have a gastroscopy (endoscopy). This involves putting a thin flexible telescope called an endoscope through the mouth and down into the gullet (oesophagus). The endoscope has a tiny light and video camera at the end. These help the doctor to take a film and see inside your oesophagus. An instrument can also be passed down the endoscope to take a small sample of the lining of the oesophagus (a biopsy). Your symptoms, the appearance of the lining of your oesophagus and the biopsy report will all help the doctor to diagnose EO.
If your child is suspected of having EO, endoscopy can be performed using a smaller tube.
Sometimes, blood tests and/or skin prick tests are used to help identify specific foods that might be causing the condition. These are more commonly used in children than in adults.
Does eosinophilic oesophagitis get better?
EO can be controlled in most cases by dietary manipulation and/or steroid medicine. However, you or your child may find that the condition returns as soon as treatment is stopped. Treatment may therefore need to be continued long-term to keep the condition under control.
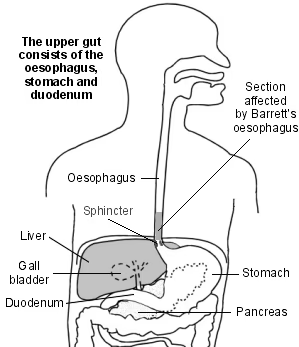
Understanding the oesophagus and stomach
When we eat, food passes down the gullet (oesophagus) into the stomach. Cells in the lining of the stomach make acid and other chemicals which help to digest food. Stomach cells also make mucus which protects them from damage from the acid. The cells lining the oesophagus are different and have little protection from acid.
There is a circular band of muscle (a sphincter) at the junction between the oesophagus and stomach. This relaxes to allow food down but then normally tightens up and stops food and acid leaking up (refluxing) into the oesophagus. In effect, the sphincter acts like a valve.
Barrett's oesophagus
Further reading and references
- Murali AR, Gupta A, Attar BM, et al; Topical steroids in eosinophilic esophagitis: Systematic review and meta-analysis of placebo-controlled randomized clinical trials. J Gastroenterol Hepatol. 2016 Jun;31(6):1111-9. doi: 10.1111/jgh.13281.
- Furuta GT, Katzka DA; Eosinophilic Esophagitis. N Engl J Med. 2015 Oct 22;373(17):1640-8. doi: 10.1056/NEJMra1502863.
- Velikova T; Challenges and updates in the management of eosinophilic esophagitis. Prz Gastroenterol. 2020;15(1):27-33. doi: 10.5114/pg.2019.84476. Epub 2019 Apr 12.
- Visaggi P, Savarino E, Sciume G, et al; Eosinophilic esophagitis: clinical, endoscopic, histologic and therapeutic differences and similarities between children and adults. Therap Adv Gastroenterol. 2021 Jan 31;14:1756284820980860. doi: 10.1177/1756284820980860. eCollection 2021.
- Budesonide orodispersible tablet for inducing remission of eosinophilic oesophagitis; NICE Technology appraisal guidance, June 2021
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 13 May 2026
14 May 2021 | Latest version

Feeling unwell?
Assess your symptoms online for free