Scarlet fever
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 27 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Viral rashesMeaslesChickenpox in childrenChickenpox in adults and teenagersHand, foot and mouth diseaseSchool exclusion for infections
Scarlet fever is an infectious disease that mainly affects children under the age of 10 years.
In this article:
Video picks for Infections
Continue reading below
What is scarlet fever?
Scarlet fever is due to a throat infection caused by a germ (bacterium) called streptococcus, usually group A streptococcus. It causes a rough-feeling red rash, sore throat, fever and sometimes other complications
What causes scarlet fever?
Back to contentsScarlet fever is caused by a tiny germ (bacterium) called Streptococcus pyogenes. The germ is sometimes called 'group A Strep' or GAS. This germ causes quite a few illnesses, including skin infections, chest infections and infections of the heart.
Sometimes the germs (bacteria) only cause a sore throat, without causing the rash of scarlet fever. This is often called a 'Strep throat' or simple tonsillitis.
But in scarlet fever, the streptococcus bacterium releases toxins that spread through the body. The toxins cause the rash and, if untreated, can cause problems in the kidneys and heart even years later, which you can read more about in the treatment and complications section.
Continue reading below
What are the symptoms of scarlet fever?
Back to contentsSore throat.
Redness of the tongue with tiny white spots (this occurs around the same time).
Sometimes swelling of the tongue a few days later.
A red, rough-feeling rash on their chest, tummy and cheeks. It feels a bit like sandpaper and usually appears 12-48 hours after infection.
Scarlet fever starts with a very sore throat and a high temperature (fever). It is often initially put down to tonsillitis.
Sometimes at roughly the same time as the sore throat comes on, the tongue goes red, with tiny white spots. This makes it look like a strawberry, hence the name: strawberry tongue. This is pretty typical of scarlet fever.
After the sore throat and whitish tongue comes a red rash on the cheeks, chest and tummy. If you run your hands over the rash on the tummy and chest it feels slightly rough, like fine sandpaper. This is the typical rash of scarlet fever.
Child with scarlet fever
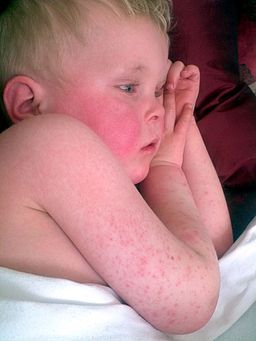
© By www.badobadop.co.uk (Own work) via Wikimedia Commons
After a couple of days the tongue, previously only slightly red with white spots, goes very red and a bit bigger than usual. Some people call this a 'beef tongue'.
Strawberry tongue
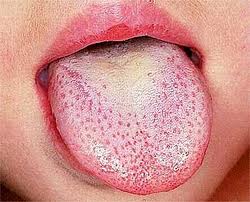
© By Afag Azizova (Own work) via Wikimedia Commons
By this stage, the combination of a sore throat, rough-feeling rash and red tongue makes the diagnosis of scarlet fever fairly obvious to doctors.
If left untreated, the rash and sore throat will fade over about 10 days, but the skin sometimes peels (like with sunburn).
Not all people with streptococcal skin infections develop the rash, as some people are not sensitive to the poison (toxin). A mild form of scarlet fever may occur; this is often called scarlatina.
How common is scarlet fever?
Back to contentsScarlet fever is most common in children aged less than 10 years, with 4-year-olds most likely of all to catch it. 89% of cases in the UK are in children under 10 years.
Although adults can get scarlet fever, this is very unusual. However, the symptoms and treatment are the same as for children.
Scarlet fever used to be very common in the 1800s and early 1900s because of overcrowding and poor living conditions. In those days it was the leading cause of death in children.
But it got much rarer as general health measures improved. There have been some recent outbreaks in the UK, usually in schools, but antibiotics can now treat scarlet fever very effectively.
Continue reading below
When to see a doctor about scarlet fever
Back to contentsYou should get advice from a healthcare professional if you or your child:
May have scarlet fever based on the symptoms outlined above.
Have scarlet fever and chickenpox at the same time.
Have already been seen by a healthcare professional but not feeling any better after a few days.
Feel ill again weeks after scarlet fever has got better (this may be a sign of a complication, such as rheumatic fever).
Are feeling unwell and have been in contact with someone who has scarlet fever.
Scarlet fever is very easily spread so check with your GP surgery as they may suggest a phone consultation rather than risk passing the infection to anyone else at the GP surgery.
What is the treatment for scarlet fever?
Back to contentsBecause scarlet fever is caused by a germ and can cause serious complications without treatment, the best treatment is antibiotics. These take a little time to get to work, so it's also important to give general treatment to relieve symptoms in the meantime.
Antibiotics
The best antibiotic is penicillin. It almost always kills the scarlet fever germ.
You need to take a long course of penicillin: ten days. This is longer than for a simple throat or ear infection and it requires quite a lot of perseverance and organisation to complete the course.
The dose will be worked out according to the age and weight of the child, but is likely to be 125-250 mg four times a day, for ten days.
If the child is allergic to penicillin then erythromycin or clarithromycin can be used instead.
But penicillin is the best for scarlet fever so it's important to check if the child is genuinely allergic to penicillin. Sometimes previous side-effects (like vomiting or diarrhoea) can be wrongly labelled as an allergy.
General treatment of a fever
It is generally important for anyone who is unwell to keep their fluid levels up.
Water alone is fine but a little bit of sugar will help the water to be absorbed. Dilute squash is fine. In a young child, milk is good too.
If the child is distressed by the fever - for example, they are limp, drowsy or whimpering - it is worth trying paracetamol.
Paracetamol can bring a high temperature (fever) down a little but it does not treat the underlying infection.
Using paracetamol in children or babies does not reduce the risk of febrile convulsions.
You should dress them in clothes that are appropriate for the outside or inside temperature. There is no need to strip down feverish children, fan them, or mop them with wet towels. In studies, none of these treatments has been shown to help.
Ibuprofen is generally not recommended in infections that involve the skin.
Generally antibiotics and fluids are the best treatment for scarlet fever.
How is scarlet fever diagnosed?
Back to contentsIn general the diagnosis can be made on the clinical picture, no tests are usually necessary.
If there is any doubt as to the diagnosis, a doctor can take a throat culture, or 'throat swab' - using something that looks like a long cotton bud.
They will send it to the hospital to be tested for the germ that causes scarlet fever. But the results will take a few days to come back, so if scarlet fever is suspected it's usually best to start antibiotic treatment first.
There is a blood test which can detect the scarlet fever germ (the anti-streptolysin titre test, or ASO for short). But the blood test is only positive from between one week and one month after the infection. So it won't tell you if someone has scarlet fever right now, only if they had it in the past.
A family doctor, or GP, will be able to recognise scarlet fever and should not need blood tests or throat swabs to make the diagnosis.
What are the possible complications of scarlet fever?
Back to contentsTreatment with antibiotics reduces the chance of complications. Complications now occur very rarely. However, if they do occur, they can be serious.
They can be broadly divided into early complications, which occur within days, and later complications, which happen weeks or months after the infection seems to have gone.
Early complications
Complications due to the spread of the infection can occur early in the infection and may include the following:
Throat infection and collection of pus (abscess).
Sinus infection.
Meningitis and brain abscess.
Later complications
Later complications are rare, but when they do happen problems start weeks, months or even years after the infection has cleared.
These occur as a result of immune reactions in the tissues. The body's immune system, rather than the germ itself, are causing the problem. These may include:
Rheumatic fever (which can damage the heart).
Kidney damage (glomerulonephritis).
This is why it's important to take the full course of antibiotics, even if your child seems to be getting better by themself.
Is scarlet fever contagious?
Back to contentsYes. Coughs or sneezes and breathing out the germs (bacteria) can pass it on (be infectious) to others. Scarlet fever can even be passed on by close contact or by sharing towels, baths, clothes or bed linen with an infected person.
It takes 2-4 days to develop symptoms after being infected. You should keep children with scarlet fever off school and away from others, for 24 hours after starting antibiotics.
Once a person has had scarlet fever, they are very unlikely to get it again. This is because they become immune to the bacteria. However, it is possible to have repeated attacks, as there are different types of streptococcal bacteria which cause the infection.
The recent outbreak of scarlet fever has sometimes occurred in schools where there is also an outbreak of chickenpox. If you have a child who has recently had chickenpox and then gets scarlet fever you need to watch out for signs of serious infection.
These may include joint pains, high temperature (fever) and persistent skin infection. There is no evidence that catching scarlet fever when pregnant will put your baby at risk.
What is the outlook for people with scarlet fever?
Back to contentsIn the past, scarlet fever used to be a very serious condition. Fortunately, nowadays for most cases, scarlet fever is a mild, self-limiting illness. Most children will recover fully within a week or so, even without treatment. (However, it is best to have treatment - see above.)
Deaths from scarlet fever are now extremely rare in the western world.
Patient picks for Infections

Children's health
Mumps
Mumps is an infection caused by a virus. It mainly affects the salivary glands, which are around the face. Sometimes other parts of the body are affected. Mumps normally affects children, but can occur at any age. Mumps is now uncommon in the UK as children are routinely immunised against mumps.
by Dr Philippa Vincent, MRCGP

Children's health
Croup
Croup is an infection of the voice box (larynx) and windpipe (trachea). These are the upper and lower parts of the breathing tube that connects the mouth to the top of the lungs. The usual cause of croup is a viral infection.
by Dr Toni Hazell, MRCGP
Further reading and references
- Scarlet fever: guidance and data; Public Health England
- Fever in under 5s: assessment and initial management; NICE Guidance (last updated November 2021)
- Exclusion table; UK Health Security Agency 2022
- Scarlet fever; NICE CKS, July 2023 (UK access only)
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 25 Sept 2028
27 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.