Meningitis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 10 Feb 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Meningitis is inflammation of the tissues around the brain. It is a serious condition, caused by various types of bacteria, viruses and fungi. The infection that causes meningitis often causes a blood infection as well (this is known as septicaemia) which can be life-threatening. If you suspect meningitis - obtain medical help immediately.
In this article:
Video picks for Meningitis and sepsis
What is meningitis?
Meningitis is an inflammation of the lining covering the brain and spinal cord (the meninges). It is usually caused by the germs from a bacterial or viral infection. As a result there are two main types of meningitis - bacterial, and viral. Much more rarely, meningitis can be due to other causes such as severe types of fungal infection or tuberculosis.
Continue reading below
How common is meningitis?
Bacterial meningitis and associated sepsis (septicaemia) have become less common over the past few decades. It is a serious illness and well known due to the media coverage when outbreaks occur. There are around 500-700 cases of bacterial meningitis in the UK every year.
Overall in the UK, Neisseria meningitidis (meningococcus), Streptococcus pneumoniae (pneumococcus), and Haemophilus influenzae type b (Hib) are the most common causes of acute bacterial meningitis in children aged 3 months or older and adults.
In babies younger than 1 month of age (neonates), Streptococcus agalactiae, Escherichia coli, S. pneumoniae, and Listeria monocytogenes (listeriosis) are the most common causes.
In children aged 3 months or older, N. meningitidis, S. pneumoniae, and Hib are the most common causative organisms.
In adults, S. pneumoniae is the most common cause of bacterial meningitis.
Viral meningitis is more common than bacterial meningitis but exact figures are not known. It is a complication of various viral illnesses. Viral meningitis is usually less serious than a bacterial cause. Most people who develop viral meningitis make a full recovery.
Other types of germs (infections) such as fungi and tuberculosis (TB) are rare causes of meningitis.
What causes meningitis?
Back to contentsBacterial meningitis
Neisseria meningitidis (meningococcus) is a common germ (bacterium), living harmlessly in the nose and throat of about 1 in 4 people. These people are called carriers. This bacterium does not survive outside the body. Close contact is needed to pass it on to others, such as intimate kissing, coughing or sneezing near to others.
Rarely, this bacterium overcomes the body's immune system and gets into the blood to cause meningitis and/or septicaemia. It is not clear why a few people are prone to serious illness and many other people are carriers of the same bacterium but have no ill effect.
Most cases of meningococcal infection are isolated cases. The risk of others catching it is low, as many people are carriers and/or have natural immunity. Sometimes small outbreaks occur when two or more people in the same household or community are affected.
Streptococcus pneumoniae (pneumococcus) is a less common cause of bacterial meningitis. This too is carried in the nose or throat by many people, with no ill effect. Again, meningitis probably occurs due to a breakdown in the immune system. It most commonly occurs in people aged over 45 years and in babies. Meningitis due to this bacterium is not thought to be passed on through touching (it is not contagious).
Other bacteria which less commonly cause meningitis include Haemophilus influenzae type b (Hib), Escherichia coli (E. coli), Listeria monocytogenes and TB. The infection with meningitis from these germs may occur for various reasons, such as a complication of an infection in another part of the body.
Viral meningitis
A variety of germs (viruses) can travel to the lining that covers the brain and spinal cord (the meninges) and cause inflammation. For example, mumps, herpes, chickenpox, influenza and many other viral infections are sometimes the cause of viral meningitis.
Continue reading below
Meningitis symptoms
Back to contentsPeople with meningitis may suffer from one or more of the following symptoms. Note that not all symptoms may occur. For example, the classic symptoms of neck stiffness and rash may not occur. If you suspect meningitis, look at our meningitis symptoms checklist and get medical help immediately.
Common early warning symptoms
Many children who are developing meningitis have nonspecific symptoms such as just feeling or looking generally unwell. These symptoms may include having a high temperature (fever), being more tired than usual and feeling sick.
However, three symptoms that commonly develop early on - often before the more classic symptoms listed later - are:
Leg pains. The pains can become severe and prevent a child from standing or walking.
Cold hands or feet - even if the child has a high temperature.
Pale, dusky or blue colour of the skin around the lips.
Meningitis rash
A typical rash is common with meningococcal infection but does not always occur. The rash is red or purple. Small spots develop at first and may occur in groups anywhere on the body. They often grow to become blotchy and look like little bruises. One or two may develop at first but many may then appear in different parts of the body.
The spots/blotches do not fade when pressed (unlike many other rashes). To check for this do the glass test. Place a clear glass firmly on one of the spots or blotches. If the spot/blotch does not fade and you can still see it through the glass, get medical help immediately.
Glass test for meningitis rash
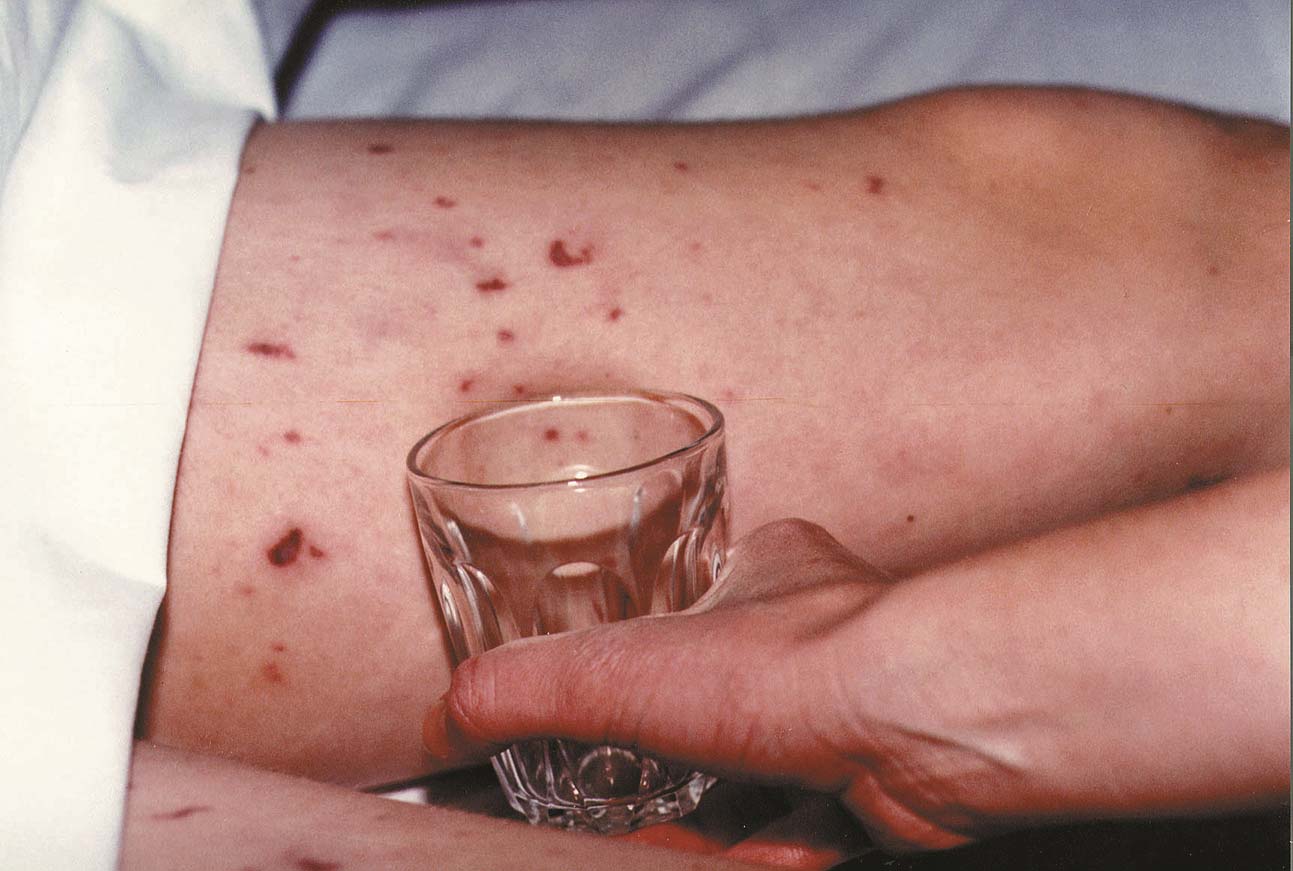
Reproduced with permission from Meningitis Now
The rash is a sign of sepsis. It may not occur with meningitis alone.
Other symptoms of meningitis that may occur in babies
These include:
Excessive crying - often high-pitched or moaning and different to their usual cry.
Fast breathing, or unusual patterns of breathing.
High temperature - but the baby may not look hot and the skin may look pale or blotchy, or turn blue. The hands and feet may feel cold. The baby may shiver.
Will not take feeds - sometimes, repeatedly being sick (vomiting).
Being irritable - especially when picked up and handled.
Drowsiness or sleepiness - does not wake easily.
A bulging fontanelle sometimes develops. The fontanelle is the soft spot on the baby's head.
Jerky movements may occur and the body may appear stiff. Sometimes the opposite occurs and the body appears quite floppy. Fits or seizures (convulsions) sometimes develop.
Other symptoms that may occur in older children and adults
These include:
High temperature and shivering - however, the hands and feet often feel cold.
Stiff neck - cannot bend the neck forward.
Headache - which can become severe.
Fast breathing.
Aches and pains in muscles or joints - the pains can become quite severe.
The skin may look pale or blotchy, or turn blue.
Dislike of bright lights - will shut the eyes and turn away from the light.
Drowsiness or confusion - may appear vacant.
Repeated vomiting. Sometimes, tummy (abdominal) pain and diarrhoea.
The course of symptoms
The symptoms often develop quickly, over a few hours or so. Symptoms can occur in any order and not all may occur. Sometimes symptoms develop more slowly, over a few days. The symptoms may suggest a less serious illness at first. For example, high temperature, headaches and vomiting are common with many viral illnesses such as flu. Therefore, even if you think it was flu to start with, if symptoms become worse then it may be meningitis.
How is meningitis diagnosed?
Back to contentsAny person with possible meningitis needs admission to hospital. Tests will include blood tests, a lumbar puncture, and scans (computerised tomography (CT) scan or magnetic resonance imaging (MRI) scan). Read more about lumbar puncture.
Continue reading below
What is the treatment for meningitis?
Back to contentsBacterial meningitis
Meningitis needs to be treated quickly with antibiotic injections. These may be started before admission to hospital - for example, your GP may give them while waiting for an ambulance. However it is essential to get to hospital for investigations and to start antibiotic treatment as soon as possible.
In hospital, further blood tests and a sample of the fluid that surrounds the spinal cord (a lumbar puncture) may be taken. These tests aim to confirm the diagnosis and to see which germ (bacterium) is causing the infection. The antibiotic may be changed depending on the results of the tests.
Intensive care is often needed, as the infection may cause shock and problems throughout the body. It is likely that fluids will need to be given directly into the veins (a drip). Oxygen is also often given through a mask on the face.
Steroid injections are also sometimes given. These work by reducing some of the inflammation that occurs with meningitis. Steroid medication has been shown in some studies to reduce the risk of developing hearing problems and other complications.
Viral meningitis
Antibiotics may be given at first when the cause of the meningitis is not known. The antibiotics are stopped if the cause of the meningitis is found to be viral. Antibiotics don't kill viruses. The body's immune system usually clears most viral infections.
What is the outlook for meningitis?
Back to contentsBacterial causes
The outlook (prognosis) often depends on how soon antibiotics are given after the illness starts. Most people make a good recovery if treated early enough. Without treatment, most people will die.
A difficulty is that bacterial meningitis can develop quickly and can copy (mimic) other illnesses when symptoms first begin. Treatment may be delayed if the cause of early symptoms is not clear at first.
In some cases, a person can be well in the morning, develop flu-like symptoms by the afternoon and be critically ill or dead by the evening.
There are several complications that may occur after having meningitis. These include:
Hearing loss. This is the most common complication. It is common to have a hearing test after you have recovered from meningitis.
Learning problems. There is a small risk of your child developing problems with their learning and behaviour. Some children will require extra support and understanding in their schools.
Epilepsy. A small proportion of children have brain injury after meningitis, which can lead to epilepsy.
Kidney problems. A small number of children have kidney problems if their kidneys are affected as part of the septicaemia.
Joint or bone problems. The septicaemia can cause some damage to different tissues in the body. This can lead to scarring to the legs, arms and body. Some people experience joint or bone problems which may develop several years after having meningitis.
Limb amputation. Sometimes the blood supply to one or more arms or legs is so bad that the arm or leg dies and has to be amputated.
Viral meningitis
This can cause an unpleasant illness. However, most affected people make a full recovery. In a small number of cases, some brain injury occurs.
Editor’s note
Dr Krishna Vakharia, 9th January 2025
The National Institute for Health and Care Excellence (NICE) has set out some guidance to ensure patient safety. It has advised that all people who are clinically assessed and found not to have bacterial meningitis or meningococcal disease are given safety netting advice so they know which symptoms to watch out for and when to seek further help.
It has further advised that all patients need intravenous antibiotics (antibiotics given via a vein) within 1 hour of their arrival at hospital if they are suspected to have bacterial meningitis or suspected meningococcal disease.
All patients who have had meningitis or meningococcal disease should have follow up to test their hearing at 4 weeks and a follow up in secondary care after 6 weeks of discharge from the hospital.
Can meningitis be prevented?
Back to contentsMeningitis vaccine and immunisation
You can help prevent meningitis by being immunised with the meningitis vaccine. Children are routinely immunised against certain causes of meningitis. These include Haemophilus influenzae type b (Hib), group B and C meningococcus, pneumococcus and mumps. See the separate leaflet called Immunisation.
The vaccine for Group B meningococcus became part of the normal UK immunisation schedule from September 2015. A vaccine protecting against types A, C, W and Y is available for those aged 17-18 years and those in their first year at university.
Other vaccines may be used for travellers going to meningitis-prone countries.
Read more about meningococcal immunisation.
Contacts
Close contacts of a person with meningococcal infection have an increased risk of developing the illness. However, the risk is still low. Close contacts usually means household members, or intimate kissing contacts within the previous seven days. These people are offered a short course of antibiotics to prevent possible infection.
If group C meningococcus is the cause then immunisation is also offered to close contacts. Occasionally, an outbreak of two or more cases of meningococcal infection occurs in the same school, college, or similar community. Antibiotics and/or immunisation may then be offered to a wider group of people.
Patient picks for Meningitis and sepsis
Infections
Symptoms of sepsis in children
Sepsis is a life-threatening condition - the symptoms can be vague or severe. This leaflet covers what to look out for and when to seek help.
by Dr Krishna Vakharia, MRCGP

Infections
Symptoms of sepsis in adults
Sepsis is a severe condition that can be fatal if not caught early. Signs and symptoms can be vague or severe. This leaflet will let you know what symptoms to look out for.
by Dr Krishna Vakharia, MRCGP
Further reading and references
- Meningitis (bacterial) and meningococcal disease: recognition, diagnosis and management; NICE guidance (March 2024)
- Meningitis - bacterial meningitis and meningococcal disease; NICE CKS, December 2024 (UK access only)
- Sepsis - recognition, diagnosis and early management; NICE Guideline (July 2016 - updated January 2024)
- Immunisation against infectious disease - the Green Book (latest edition); UK Health Security Agency.
- Meningococcal disease: guidance, data and analysis; UK Health Security Agency (last updated April 2022)
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Feb 2027
10 Feb 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.