Lumbar puncture
Spinal tap
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 10 Feb 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
A lumbar puncture is used to diagnose meningitis and some other brain and spinal cord disorders.
At a glance
A lumbar puncture is a procedure to collect a sample of fluid from around your brain and spinal cord.
It is most commonly used to help diagnose conditions such as meningitis.
During the procedure, a thin needle is inserted into your lower back after numbing the skin.
The procedure usually takes 30-45 minutes in total.
Some people develop a headache afterwards, and there are small risks of infection or bleeding.
After the test, you may need to lie flat and avoid strenuous activities for a period.
In this article:
Video picks for Other tests and investigations
Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor, specialist, or local hospital.
Continue reading below
What is a lumbar puncture?
A lumbar puncture (sometimes called a spinal tap) is a procedure where a sample of cerebrospinal fluid (CSF) is taken for testing. CSF is the fluid that surrounds the brain (cerebrum) and spinal cord. This test is most commonly used to diagnose meningitis (an infection of the meninges - the structure that surrounds the brain and spinal cord). It is also used to help diagnose some other conditions of the brain, spinal cord and central nervous system, including a subarachnoid haemorrhage which is a type of bleed inside the brain.
When is a lumbar puncture needed?
Back to contentsIf you, or your child, is admitted to hospital with symptoms that could be caused by meningitis then a lumbar puncture may be done urgently, either in the emergency department or very soon after your admission to a ward. Alternatively, you might be admitted for a planned lumbar puncture, as part of the diagnostic process for a long-term (chronic) neurological condition.
Continue reading below
How is a lumbar puncture done?
Back to contentsUsually you lie on a couch on your side with your knees pulled up against your chest. Sometimes it is done with you sitting up and leaning forwards on some pillows. The doctor or nurse will clean an area of your lower back with antiseptic.
They will then inject some local anaesthetic into a small area of skin which lies over a space between two lower spinal bones (vertebrae). This stings a little at first but then makes the skin numb.
The doctor then pushes a thin hollow needle through the skin and tissues between two vertebrae into the space around the spinal cord which is filled with CSF. Because the skin is numbed with local anaesthetic, most people do not feel pain. You may feel pressure as the needle is inserted. However, some people do have a sharp feeling in the back or leg when the needle is pushed through.
Procedure method
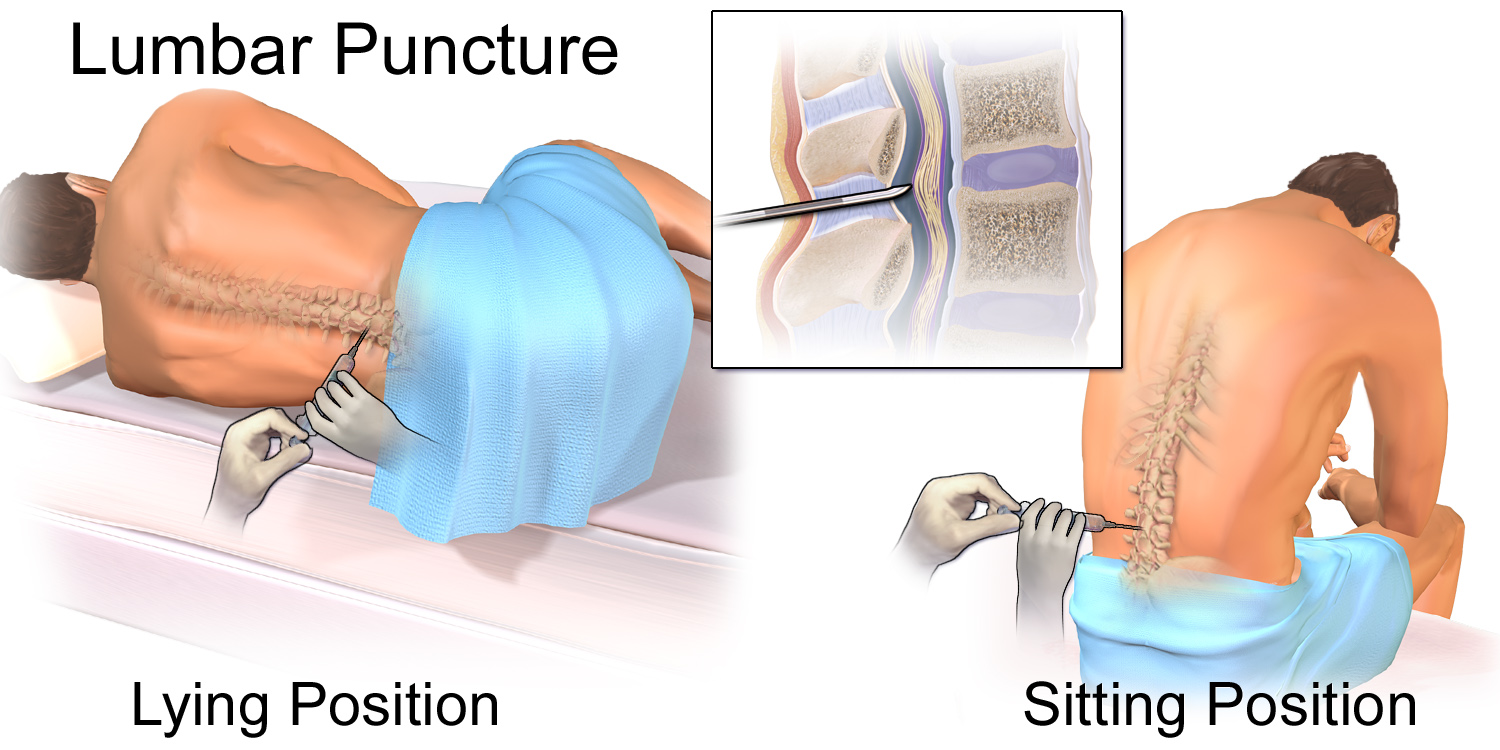
© Blausen.com staff, "Blausen gallery 2014", Wikiversity Journal of Medicine, via Wikimedia Commons
Some fluid leaks back through the needle and is collected in a sterile pot. If you have possible meningitis, this fluid sample is sent to the laboratory to be examined under the microscope to look for germs (bacteria), red blood cells and white blood cells, which are a sign of infection. It is also 'cultured' to see if any bacteria grow and what type they are.
The fluid can also be tested for protein, sugar and other chemicals if necessary. Sometimes the doctor will also measure the fluid pressure. This is done by attaching a special tube to the needle, which can measure the pressure of the fluid coming out.
The needle is usually in for about 1-2 minutes. As soon as the required amount of fluid is collected, the needle is taken out and a sticking plaster put over the site of needle entry.
How long does a lumbar puncture take?
Back to contentsIn total the procedure will take about 30-45 minutes; this includes the time to get you ready in the correct position and set up all the equipment.
Continue reading below
Are there any side-effects or risks from a lumbar puncture?
Back to contentsSome people develop a post lumbar puncture headache. This usually goes after a few hours. It is best to lie down for a few hours after the test, as this makes a headache less likely to develop. There is also risk of infection or bleeding at the needle puncture site and although rare, some damage to the spinal cord or brain may occur as a result on a lumbar puncture. It is very important that you tell the doctor if you are taking anticoagulants (blood-thinning drugs) so that they can take any necessary precautions to reduce the risk of bleeding.
Recovering from a lumbar puncture
Back to contentsIt is sensible to stay lying flat for a period of time after a lumbar puncture - the doctor who does it will tell you how long. They will usually advise you not to operate heavy machinery or drive for at lest 24 hours and not to play sport or do any strenuous activities for at least a week.
Patient picks for Other tests and investigations

Tests and investigations
Audiology
If you or a family member suspect that you have a hearing problem, then an audiologist will usually provide an assessment and also may be involved in providing any treatment needed. Certain conditions causing balance difficulties or dizziness can arise due to problems in the ear and audiologists can undertake specialist tests to investigate these problems as well.
by Dr Surangi Mendis, MRCGP

Tests and investigations
Nerve conduction studies
Nerve conduction studies help to test how well and how fast nerves conduct electrical signals. Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Caroline Wiggins, MRCGP
Frequently asked questions
What is cerebrospinal fluid (CSF)?
Cerebrospinal fluid (CSF) is the fluid that surrounds both the brain (cerebrum) and the spinal cord. A lumbar puncture involves taking a sample of this fluid for testing.
What conditions can a lumbar puncture help diagnose?
A lumbar puncture is most commonly used to diagnose meningitis, which is an infection of the membranes surrounding the brain and spinal cord. It can also help diagnose other conditions affecting the brain, spinal cord, and central nervous system, including a subarachnoid haemorrhage, which is a type of bleed inside the brain. It can also be used as part of the diagnostic process for some long-term (chronic) neurological conditions.
What happens to the fluid sample after it's collected?
Once collected, the fluid sample is sent to a laboratory. There, it is examined under a microscope to look for germs (bacteria), red blood cells, and white blood cells, which can indicate an infection. It is also 'cultured' to see if any bacteria grow and to identify their type. Additionally, the fluid can be tested for protein, sugar, and other chemicals if required. Sometimes, the pressure of the fluid itself is also measured.
Does a lumbar puncture hurt?
Before the procedure, local anaesthetic is injected into the lower back to numb the skin. This injection may sting a little at first. While the needle is inserted, most people do not feel pain, though you might feel some pressure. However, some individuals may experience a sharp sensation in their back or leg when the needle is pushed through.
Can I prevent a headache after the procedure?
Some people develop a headache after a lumbar puncture. To make a headache less likely to develop, it is best to lie down for a few hours after the test. If a headache does occur, it usually goes away after a few hours.
What precautions should I take after a lumbar puncture?
After the procedure, it is advisable to stay lying flat for a period of time, as instructed by your doctor. You will usually be advised not to operate heavy machinery or drive for at least 24 hours, and to avoid playing sports or engaging in strenuous activities for at least a week.
Further reading and references
- Bacterial meningitis and meningococcal septicaemia: Management of bacterial meningitis and meningococcal septicaemia in children and young people younger than 16 years in primary and secondary care; NICE Clinical Guideline (last updated February 2015)
- Meningococcal disease: guidance, data and analysis; UK Health Security Agency (last updated April 2022)
- Sepsis - recognition, diagnosis and early management; NICE Guideline (July 2016 - updated January 2024)
- Viallon A, Botelho-Nevers E, Zeni F; Clinical decision rules for acute bacterial meningitis: current insights. Open Access Emerg Med. 2016 Apr 19;8:7-16. doi: 10.2147/OAEM.S69975. eCollection 2016.
- Cognat E, Koehl B, Lilamand M, et al; Preventing Post-Lumbar Puncture Headache. Ann Emerg Med. 2021 Sep;78(3):443-450. doi: 10.1016/j.annemergmed.2021.02.019. Epub 2021 May 7.
Continue reading below
About the authorView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Feb 2028
10 Feb 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.