Chickenpox in children
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 16 Mar 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Viral rashesMeaslesChickenpox in adults and teenagersScarlet feverHand, foot and mouth diseaseSchool exclusion for infections
Chickenpox causes spots (a rash) and can make a child feel generally unwell. Treatment aims to ease symptoms until the illness goes. Full recovery is usual in children aged under 12 years. Serious complications are rare but are more likely to occur in children with a poor immune system, such as those on chemotherapy.
In this article:
Video picks for Infections
Continue reading below
What is chickenpox?
What is chickenpox?
Chickenpox is an infection caused by the varicella-zoster virus. Most children have chickenpox at some stage. Most commonly, children get chickenpox before the age of 10 years. The immune system makes proteins called antibodies during the infection. These fight the virus and then provide lifelong protection against it (immunity). Therefore, it is uncommon to have more than one bout of chickenpox in your lifetime.
Severe chickenpox in a child
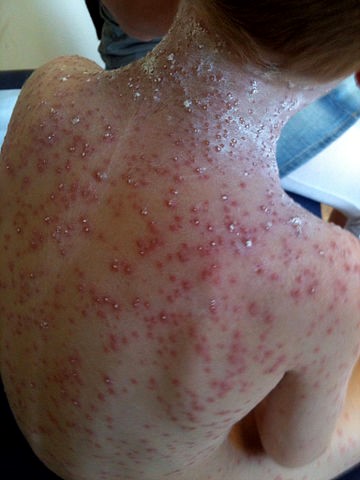
© Gzzz, CC BY-SA 4.0, via Wikimedia Commons
Chickenpox symptoms
Back to contentsThe main symptom of chickenpox is a rash. Flu-like symptoms are also common and typically start a day or so before a rash. Children with chickenpox may have:
A high temperature (fever), aches and a headache that often starts a day or so before a rash appears.
Spots (rash). Spots appear in crops. They develop into small blisters and are itchy. They can be anywhere on the body. Several crops may develop over several days. Some children may be covered in spots; others have only a few or even none. The rash starts off looking like red spots, which then blister, and then scab over.
Loss of appetite or feeding problems.
Chickenpox in a child
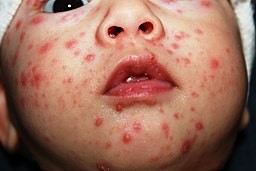
© Øyvind Holmstad, CC BY-SA 4.0, via Wikimedia Commons
Some children feel quite unwell for a few days. Others appear only mildly ill. Most are much better within a week. The blisters dry up and scab. They gradually fade but may take up to two weeks to go completely.
Continue reading below
Chickenpox treatment
Back to contentsTreatment of chickenpox is mainly aimed at easing symptoms and trying to make your child as comfortable as possible whilst the immune system deals with the virus. Treatments include:
A soothing cream (emollient)
This may help the itch. Calamine lotion is the one most used, although it is not known how effective it is.
A sedating antihistamine
A tablet or liquid medicine may help with sleep if itch is a problem. This can be used in children over 1 year old. Give a dose at bedtime. You can buy these at pharmacies or get them on prescription. Chlorphenamine (Piriton®) is the one most used. It can also be helpful for itch during the daytime but may cause some sleepiness as a side-effect.
Keep fingernails cut short
Keeping your child's fingernails short will help to stop deep scratching.
Dress children comfortably
Use cool smooth fabrics such as cotton so they are not cold or overheated.
How to treat a fever
Back to contentsA fever commonly occurs with chickenpox, and may make your child feel uncomfortable and irritable. The following are things that you can do that may bring the temperature down and make your child feel more comfortable:
You can give paracetamol
This will help to lower a temperature. You can buy paracetamol in liquid form, or as melt-in-the-mouth tablets, for children. It comes in various brand names. The dose for each age is given with the medicine packet.
Paracetamol does not treat the cause of the fever. It merely helps to ease discomfort. It also eases headaches, and aches and pains. You do not need to use paracetamol if your child is comfortable and not distressed by the fever, aches or pains.
Ibuprofen has been used with paracetamol in the past. The National Institute for Health and Care Excellence (NICE) has recommended that ibuprofen no longer be used for chickenpox. This is because some studies suggested that there may be an association with more severe skin reactions if ibuprofen is used for chickenpox. While more evidence is awaited, the advice is to avoid ibuprofen in this situation.
Take extra layers of clothes off your child
If the room is normal room temperature. It is wrong to wrap up a feverish child. The aim is to prevent overheating or shivering.
Give lots to drink
This helps to prevent a lack of fluid in the body (dehydration). You might find that a child is more willing to have a good drink if they are not so irritable. So, if they are not keen to drink, it may help to give some paracetamol first. Then, try the child with drinks half an hour or so later when his/her temperature is likely to have come down.
Other treatments
Do not cold-sponge a child who has a fever. This used to be popular, but it is now not advised. This is because the blood vessels under the skin become narrower (constrict) if the water is too cold. This reduces heat loss and can trap heat in deeper parts of the body. The child may then get worse. Many children also find cold-sponging uncomfortable.
Some people use a fan to cool a child. Again, this may not be a good idea if the fanned air is too cold. However, a gentle flow of air in a room which is room temperature may be helpful. Perhaps just open the window or use a fan on the other side of the room to keep the air circulating.
Continue reading below
Treatment for special at-risk groups
Back to contentsSome children have a higher risk of developing complications from chickenpox. In addition to the above treatments, they may need extra treatment such as aciclovir (an antiviral medicine) or vaccination. If your child has not already had chickenpox and is in one in the following groups, you should see a doctor urgently if they have contact with chickenpox, or have symptoms of it:
Children (babies) less than 1 month old.
Children with a poor immune system. For example, children with leukaemia, immune diseases or HIV/AIDS.
Children taking certain medication such as steroids, immune-suppressing medication or chemotherapy.
Children with severe heart or lung disease.
Children with severe skin conditions.
Antiviral medication is also used for adults and teenagers who develop chickenpox, as they too have a higher risk of complications. However, antiviral medication is not normally advised for healthy children aged over 1 month and under 12 years who develop chickenpox.
Complications of chickenpox
Back to contentsMost of the time, children with chickenpox recover fully and have no complications. Uncommonly, one or more of the following complications can occur.
The spots do not usually scar unless they are badly scratched.
Some spots become infected with germs (bacteria) in some cases. This is the most common complication in children. If this occurs, the surrounding skin becomes red and sore. Antibiotics in the form of creams or medicine may then be needed.
Inflammation of the lung (pneumonia) and inflammation of the brain (encephalitis) are rare complications.
Vary rarely, other serious complications develop. For example:
Reye's syndrome. (a very rare condition with brain and liver problems).
Ataxia (problems co-ordinating movements).
Henoch-Schönlein purpura (a condition that can affect the kidneys).
Inflammation of various parts of the eye.
Therefore, although serious complications are rare, it is best to be watchful. See a doctor if your child develops any worrying symptoms that you are unsure about such as:
Breathing problems.
Weakness such as a child becoming wobbly on his/her feet.
Drowsiness.
Fits (convulsions).
Pains or headaches which become worse despite paracetamol.
Being unable to take fluids, due to a severe rash in the mouth.
A severe rash, or a rash which bruises or bleeds into the skin (haemorrhagic rash).
Becoming generally more and more unwell.
Shingles
Shingles is caused by the same virus that causes chickenpox and is a very delayed complication of chickenpox. Anyone who has had chickenpox in the past may develop shingles.
Shingles is an infection of a nerve and the area of skin supplied by the nerve. It causes a rash and pain in a local band-like area along the affected nerve. About 1 in 5 people have shingles at some time in their lives. It can occur at any age, but it is most common in people over the age of 50.
The reason why shingles may occur is because the virus does not completely go after you have chickenpox. Some virus particles remain inactive in the nerve roots next to your spinal cord. They do no harm there and cause no symptoms.
For reasons that are not clear, the virus may begin to multiply again (reactivate). This is often years later. The reactivated virus travels along the nerve to the skin to cause shingles. See the separate leaflet called Shingles (Herpes Zoster) for details.
Note: you can catch chickenpox from being exposed to a person with shingles if you have not had chickenpox yourself. However, you cannot catch shingles from a person with chickenpox, or catch shingles from a person with shingles.
Is chickenpox infectious?
Back to contentsA person with chickenpox is very infectious. The virus spreads in the air from person to person. For example, if you have not already had chickenpox, you stand a good chance of catching it if:
You are in the same room as someone with chickenpox for more than 15 minutes; or
You have any face-to-face contact with someone with chickenpox, such as a conversation.
Nine in ten people who have not had chickenpox would catch it after being exposed in this way.
It takes between 7 and 21 days (most commonly 10-14 days) to develop symptoms after catching the virus (the incubation period).
Protecting others
Back to contentsA person with chickenpox is infectious from two days before the spots first appear until they have all crusted over (commonly about five days after onset of the rash). A child with chickenpox should stay off school or nursery for five days from the onset of the rash and until all the lesions have crusted. Also, whilst infectious, they should keep away from at-risk people who may develop a severe illness if they get chickenpox. These include:
Pregnant women who have not had chickenpox in the past. Chickenpox can be severe and cause complications during pregnancy. See the separate leaflet called Chickenpox Contact in Pregnancy for more information.
People with a poorly functioning immune system. For example, people with leukaemia, with HIV/AIDS, on steroid medication, or who are having chemotherapy.
The at-risk children listed earlier.
Healthy adults who have not had chickenpox may also want to avoid catching it, as the illness tends to be worse in adults.
Note: people with chickenpox should not travel by air until all the spots have crusted over.
Are you a healthcare worker?
Healthcare workers come into contact with people with poor immune systems, pregnant women and newborn babies. They should be aware that if they catch chickenpox, they can be infectious for two days before a rash or illness appears, and be a risk to patients. So, if you are a healthcare worker and come into contact with someone who has chickenpox (or who develops it within the following two days), then:
If you have been immunised against chickenpox, or have definitely had chickenpox in the past, you are likely to be immune. You should continue working but contact your occupational health department if you feel unwell or develop a rash.
If you are uncertain about whether you have had chickenpox or been immunised, you should have a test to see if you are immune. If you are not immune you should:
Avoid contact with high-risk patients for 8-21 days after the contact.
Report to occupational health before patient contact if you feel unwell or develop a high temperature (fever) or rash.
Get immunised against the chickenpox virus (the varicella-zoster virus).
Frequently asked questions
Back to contentsIs there a vaccine against chickenpox?
Yes, there is a vaccine that protects against the virus that causes chickenpox. It is part of the routine childhood immunisation programme in certain countries such as the USA, Canada and Australia. Currently, there are no plans to make immunisation against chickenpox routine for children in the UK.
In the UK, the vaccine is offered by the NHS to certain groups. For example, healthcare workers who are not immune to chickenpox. Also, to people who are not immune to chickenpox and who are in close contact with people with a poor immune system. For example, brothers and sisters of children on chemotherapy.
The chickenpox vaccine is available privately from many pharmacists for people aged 3-65 who are not pregnant, breastfeeding or trying for a baby. You will need a consultation with your pharmacist to check this vaccination is suitable for you or your child before it is given.
See also the separate article Should your child have the chickenpox vaccine?
Should I let my child catch chickenpox?
Some parents encourage their children to mix with others who have chickenpox in order to catch it.
Pros
Chickenpox is usually a milder illness in a child than in an adult.
The risk of serious complications is higher in adults. In particular, chickenpox during pregnancy can cause serious complications to both mother and baby.
Most people get chickenpox at some stage. As the risks are fewer if you have it as a child, it may be better to get it over with.
Cons
"I could not willingly let my child develop an illness."
Although rare, some children do have serious complications.
Different parents have different views on this issue. And remember, children who develop chickenpox spots (the rash) today will have been just as infectious over the previous two days when they were well, but were incubating the virus.
Also note: if someone in the family or home is temporarily at high risk of complications (listed earlier - pregnant women, etc) then it is best to put off deliberately catching it.
Can I go to work if my child has chickenpox?
If your child has chickenpox, you may need to stay at home to look after them until they can go back to school or nursery (when all the spots have formed a scab, which is usually five days after the spots first appear).
If you're healthy and have had chickenpox, you are otherwise fine to go to work and carry on normally, even if your child has chickenpox, but you should stick to good hygiene such as washing your hands frequently.
If you haven't had chickenpox or can't be certain that you have, you should assume that you will catch it from your child and so stay at home until all your spots have formed a scab. But remember it takes between 7 and 21 days (most commonly 10-14 days) to develop symptoms after catching the virus. It is particularly important to stay away from people who are at greater risk of complications if they catch the chickenpox virus (see special at-risk groups above).
See also the separate leaflet Chickenpox in Adults and Teenagers.
Patient picks for Infections

Children's health
Mumps
Mumps is an infection caused by a virus. It mainly affects the salivary glands, which are around the face. Sometimes other parts of the body are affected. Mumps normally affects children, but can occur at any age. Mumps is now uncommon in the UK as children are routinely immunised against mumps.
by Dr Philippa Vincent, MRCGP

Children's health
Head lice and nits
Head lice are small insects that live in human hair and feed on blood from the scalp. Their eggs are called nits.
by Dr Colin Tidy, MRCGP
Further reading and references
- Immunisation against infectious disease - the Green Book (latest edition); UK Health Security Agency.
- Guidance on infection control in schools and other childcare settings; UK Health Security Agency (September 2017 - last updated February 2023)
- Cohen J, Breuer J; Chickenpox: treatment. BMJ Clin Evid. 2015 Jun 15;2015. pii: 0912.
- Fever in under 5s: assessment and initial management; NICE Guidance (last updated November 2021)
- Chickenpox; NICE CKS, June 2022 (UK access only)
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Mar 2028
16 Mar 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.