MRCP scan
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Surangi MendisLast updated 17 Aug 2023
Meets Patient’s editorial guidelines
An MRCP scan is a scan that uses magnetic resonance imaging to produce pictures of your liver, bile ducts, gallbladder and pancreas.
Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
In this article:
Continue reading below
What is an MRCP scan?
MRCP stands for magnetic resonance cholangiopancreatography.
What is MRCP scan used for?
MRCP is a type of magnetic resonance imaging (MRI). See the separate leaflet called MRI Scan for more details.
MRCP produces detailed images of your liver, gallbladder, bile ducts, pancreas and pancreatic duct. It is a less invasive alternative to endoscopic retrograde cholangiopancreatography (ERCP). See the separate leaflet called ERCP (Endoscopic Retrograde Cholangiopancreatography) for more details. It can provide similar diagnostic information to the ERCP and so it can replace the ERCP in high-risk patients to avoid significant complications.
Continue reading below
Why do I need an MRCP scan?
The uses of MRCP include:
Checking your liver, bile ducts, gallbladder and pancreas for gallstones, tumours, infection or inflammation.
Investigating the cause of inflammation of your pancreas (pancreatitis).
Investigating unexplained abdominal pain (tummy pain).
Other abnormalities an MRCP can identify:
Structural abnormalities of the cystic and hepatic ducts.
Complications from biliary surgery.
Gallstones (choledocholithiasis).
Biliary strictures.
Pancreatic cysts.
Trauma to the biliary system.
The bile ducts and nearby structures
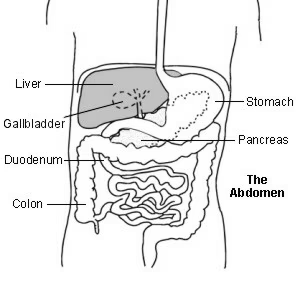
Bile is made in your liver. The liver is in the upper right part of your abdomen (tummy). Bile passes from liver cells into tiny tubes called bile ducts. These join together like branches of a tree to form the common bile duct. Bile constantly drips down the common bile duct, and through an opening called the papilla into the first part of your gut after your stomach, the duodenum.
Diagram showing detail around the pancreas
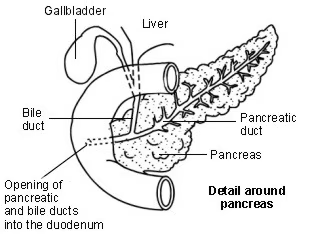
Liver function
The gallbladder lies under the liver on the right side of the upper abdomen. It is like a pouch which comes off the common bile duct. It is a reservoir which stores bile between meals. Your gallbladder contracts (squeezes) when you eat. This empties the stored bile back into the common bile duct. The bile passes along the remainder of the common bile duct into your duodenum. Bile helps to digest food, particularly fatty foods.
Patient picks for Imaging
The pancreas is a large gland that makes chemicals (enzymes). These flow down the pancreatic ducts, into the main pancreatic duct and through the papilla into your duodenum. The pancreatic enzymes are vital to digest food. Your pancreas also makes some chemicals (hormones) such as insulin.
Continue reading below
How does MRCP work?
MRCP uses MRI technology. It is essentially an MRI scan, which uses a strong magnetic field and radio waves to create pictures of tissues, organs and other structures inside your body, on a computer. Sometimes you may receive an injection of 'contrast' when you have this test. Contrast is a substance that enhances the MRI picture. It makes it easier for doctors to see various parts of the body.
What are the advantages of an MRCP scan?
The MRCP is a non-invasive imaging technique (meaning nothing has to be placed inside your body to obtain the images) that does not involve exposure to radiation.
MRI-type imaging can provide detailed images of the soft-tissue structures of the body such as the heart, liver, pancreas and many other organs. This detail makes MRI an invaluable tool in early diagnosis and evaluation of cancer.
MRCP can produce images as good as those obtained by the more invasive exam called ERCP, without its associated risks including pancreatitis (or inflammation of the pancreas), perforation (piercing) of the pancreatic and bile ducts and bowel, and the risks associated with intravenous sedation required for ERCP.
What are the limitations of an MRCP scan?
You need to be able to remain perfectly still and follow breath-holding instructions in order to get high-quality images. If you are anxious, confused or in severe pain, you may find it difficult to lie still during imaging.
A person who is very large may not fit into certain types of MRI machines. There are weight limits on the scanners.
Implants and other metallic objects can also make it difficult to obtain clear images.
How does an MRI scan work?
Your body contains millions of hydrogen atoms. When you are in an MRI scanner:
A strong magnetic field aligns particles called protons which are within the hydrogen atoms. All the protons line up in parallel with the magnetic field, like tiny magnets. (Normally the millions of protons all lie in random directions.)
Then, short bursts of radio waves are sent from the scanner into your body. The radio waves knock the protons from their position.
When the burst of radio waves stops, the protons realign back into place. As they do so they emit radio signals. The protons in different tissues of the body realign at different speeds. Therefore, the signal emitted from different body tissues varies. So, for example, softer tissues can be distinguished from harder tissues on the basis of the signals sent.
These signals are detected by a receiving device in the scanner.
The receiving device transmits the signals to a computer. The computer creates a picture based on the radio signals emitted from the body.
How is a MRCP scan done?
An MRCP scan is carried out in an MRI scanner. The MRI scanner is like a tunnel about 1.5 metres long surrounded by a large circular magnet. You lie on a table that slides into the scanner. A receiving device, like an aerial, is placed behind, or around, the part of the body being examined. This detects the tiny radio signals emitted from your body. When each picture is being taken you need to keep still for a few minutes, otherwise the scan picture may be blurred.
The scan itself is painless. The whole procedure can take 15-40 minutes. It may be a little uncomfortable lying still on the couch for this time. In some cases an injection of a special contrast dye is given into the bloodstream via a vein on your arm.
The person who is qualified to carry out X-ray and scanning procedures is called a radiographer. The radiographer sits in the control room next to the scanner and observes through the window. However, you can talk to them, usually via an intercom and you will be observed at all times on a monitor.
The scanner is noisy so you will usually be given some headphones or earplugs to protect your ears from the noise. Quite often you can listen to the radio or some music of your choice through the headphones.
What should I do to prepare for an MRCP scan?
Usually very little. Your local hospital should give you information about what is required before you come for the scan, including when you should last eat or drink before the procedure. Because an MRCP involves the use of an MRI scanner there are certain safety procedures involved.
Before your procedure, the person carrying out your scan (the radiographer) will ask you a number of questions for your safety. The MRI scanner uses an extremely strong magnet, so people with certain types of medical implant cannot be scanned. This is because the magnet can potentially move medical devices with metal in them, or affect their function.
You will be asked to remove any jewellery, including your watch, before entering the MRI scanner. You will also need to remove any hair pins or hearing aids and also to leave your credit cards in a different room, as the strong magnets can affect these. You should tell the radiographer about any body piercings you may have.
Before you enter the scanning area you should be asked if you have any medical devices in your body. The following is not a definitive list but may help remind you of the type of things radiographers need to know about.
You should tell the radiographer if you have any of the following:
Internal (implanted) defibrillator.
Cochlear (ear) implant.
Surgical clips such as those used on brain aneurysms.
Artificial heart valves.
Implanted medicine infusion ports.
An implanted electronic device, including a cardiac pacemaker.
Artificial limbs or metallic joints.
Implanted nerve stimulators.
Pins, screws, plates, stents or surgical staples.
Generally, any metal objects that have been used during orthopaedic surgery are not a problem for this type of scan. It is also important to tell the test operator if you have ever had any metal fragments lodged in your eyes or your body. In some cases you may need an X-ray before the scan to make sure you are safe to enter the scanner.
What can I expect after an MRCP scan?
There are no after-effects from the scan. You can return to your normal activities as soon as the scan is over.
The pictures from the scan are studied by an X-ray doctor (a radiologist) who interprets and analyses the images. The radiologist then sends a signed report to the doctor who originally requested the scan, who will share the results with you.
Are there any side-effects or complications from an MRCP scan?
MRCP scans use MRI which is painless and safe. Unlike X-rays and some other imaging tests, an MRI scan does not use radiation. However:
Rarely, some people have reactions to the contrast dye which is sometimes used.
Pregnant women are usually advised not to have an MRI scan unless it is urgent. Although the scan is thought to be safe, the long-term effects of strong magnetic fields on a developing baby are not yet known.
Further reading and references
- Magnetic Resonance Cholangiopancreatography (MRCP); Radiological Society of North America, 2013
- Griffin N, Charles-Edwards G, Grant LA; Magnetic resonance cholangiopancreatography: the ABC of MRCP. Insights Imaging. 2012 Feb;3(1):11-21. doi: 10.1007/s13244-011-0129-9. Epub 2011 Sep 28.
- Goldfinger MH, Ridgway GR, Ferreira C, et al; Quantitative MRCP Imaging: Accuracy, Repeatability, Reproducibility, and Cohort-Derived Normative Ranges. J Magn Reson Imaging. 2020 Sep;52(3):807-820. doi: 10.1002/jmri.27113. Epub 2020 Mar 8.
- Kumar A, Mohanty NR, Mohanty M, et al; Comparison of MRCP and ERCP in the evaluation of common bile duct and pancreatic duct pathologies. Front Med Technol. 2023 Jul 12;5:946555. doi: 10.3389/fmedt.2023.946555. eCollection 2023.
- Swensson J, Zaheer A, Conwell D, et al; Secretin-Enhanced MRCP: How and Why-AJR Expert Panel Narrative Review. AJR Am J Roentgenol. 2021 May;216(5):1139-1149. doi: 10.2214/AJR.20.24857. Epub 2021 Mar 11.
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 15 Aug 2028
17 Aug 2023 | Latest version

Feeling unwell?
Assess your symptoms online for free
