Erythema multiforme
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 14 Mar 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is erythema multiforme?
Erythema multiforme (EM) is a skin condition due to an immune-mediated hypersensitivity reaction to infections or drugs.12 It presents as a dermatological eruption featuring iris or target lesions, although other forms of skin lesion can occur - hence the name. It is usually an acute, self-limiting disease that affects the skin. Mucosal lesions are present in 25% to 60% of patients with erythema multiforme.
EM must be distinguished from the rare but more serious and life-threatening conditions, Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN).3
How common is erythema multiforme? (Epidemiology)2
Back to contentsErythema multiforme can occur at any age but most commonly presents between the ages of 20 and 40. 20% of cases occur in children. Males are affected slightly more often than females with a ratio of 5:1. Erythema multiforme occurs equally in all ethnic groups. The prevalence is thought to be considerably lower than 1%.
Continue reading below
Causes of erythema multiforme (aetiology)1 2
Back to contents90% of cases of erythema multiforme are caused by infections.
Infections
Herpes simplex virus (HSV) 1 and 2 infections (account for >50% of cases).
Mycoplasma pneumonia infections.
Fungal infections.
Other viruses (varicella-zoster virus, cytomegalovirus, hepatitis C virus, and HIV).
Drug reactions
Barbiturates.
Penicillins.
Phenothiazines.
Sulfonamides.
Anticonvulsants.
Non-steroidal anti-inflammatory drugs.
Vaccinations (diphtheria-tetanus, hepatitis B, smallpox, covid-19).
Other causes
Heavy metals.
Topical therapies.
Herbal remedies.
Poison ivy.
Symptoms of erythema multiforme (presentation)1 2
Back to contentsHistory
There may be either no prodrome or a mild upper respiratory tract infection. The rash starts abruptly, usually within three days. It starts on the extremities, being symmetrical and spreading centrally.
There may be some mild burning or itching sensation but the skin is not tender.
Recurrent EM is thought to be usually due to reactivation of HSV.
Half of children with the rash have recent herpes labialis. It usually precedes the EM by 3 to 14 days but it can sometimes be present at the onset.
Examination
The iris or target lesion is the classical feature of the disease.
Initially, there is a dull red macule or urticarial plaque that enlarges slightly up to 2 cm over 24-48 hours. In the middle, a small papule, vesicle or bulla develops, flattens, and then may clear. The intermediate ring forms and becomes raised, pale and oedematous. The periphery slowly becomes violaceous and forms a typical concentric target lesion.
The lesions can expand to form plaques which are several centimetres in diameter.
Some lesions are atypical targets with only two concentric rings. Polycyclic or arcuate lesions may occur.
Erythema multiforme
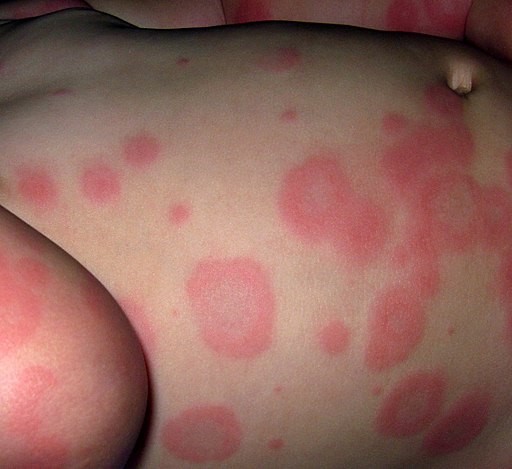
© Grook Da Oger, CC BY-SA 3.0, via Wikimedia Commons
Erythema multiforme
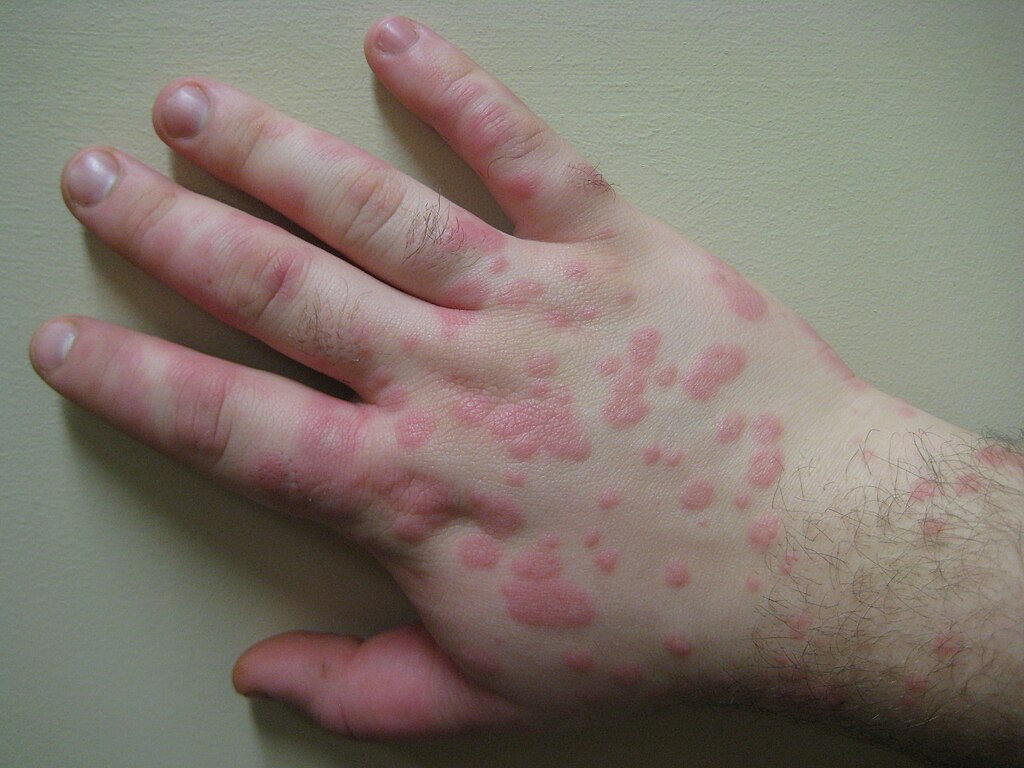
© James Heilman, MD, CC BY-SA 3.0, via Wikimedia Commons
Köbner's phenomenon may occur. This lesion occurs along the line of previous skin trauma.
Lesions appear first on the extensor surfaces of the periphery and extend centrally. The palms, neck and face are often involved but the soles and flexures of the extremities less often.
There may be mucosal involvement. Whereas the skin lesions are painless, mucosal lesions are often painful. Oral lesions are most common with lips, palate and gingiva affected; urogenital and ocular membranes have also been known to have been affected.2
Occasionally the mucosal involvement is marked with few skin lesions.
Continue reading below
Diagnosing erythema multiforme (investigations)
Back to contentsUsually, no specific investigations are indicated.
Skin biopsy can be indicated in an atypical presentation or where there is recurrent EM without an obvious trigger.
Investigations may be required to discover the underlying cause - eg, CXR, drug history, atypical pneumonia titres.
An FBC will often show moderate leukocytosis, eosinophilia, neutropenia, mild anaemia, and thrombocytopenia.
ESR may be elevated in severe cases.
CXR may show interstitial disease if the underlying cause is Mycoplasma pneumoniae.
If the diagnosis is unclear, a skin biopsy may be suggested.
Differential diagnosis4
Back to contentsSJS.
TEN.
Pemphigoid.
Management of erythema multiforme6
Back to contentsIf a drug is thought to be responsible, it must be withdrawn. If an infection is suspected, it should be treated.
In recurrent disease due to HSV, antiviral therapy is beneficial.7
Symptomatic treatment may include analgesics, mouthwash and local skin care. Steroid creams may be used.
It may be helpful to emphasise to patients or parents that, although an underlying infection may be contagious, EM itself is not.
If the mouth is very sore, attention may have to be given to hydration and nutrition.
Dilute antiseptics, such as chlorhexidine, may help to prevent secondary infection. Lubricating drops for the eyes may be required.
Where erythema multiforme is severe and refractory, biologic agents such as thalidomide, anti-TNF, apremilast, rituximab, and JAK inhibitors have been shown to have some benefit.8
Complications of erythema multiforme
Back to contentsSecondary infection of lesions may occur. Serious complications are unusual in an immunocompetent patient. A very sore mouth may lead to dehydration and poor nutrition. Genitourinary lesions may result in urinary retention. If the eye is involved it is important to prevent infection or conjunctival scarring.
Significant mucosal involvement indicates erythema multiforme major which is likely to required hospitalisation for supportive care.9
Prognosis1
Back to contentsFurther reading and references
- Hafsi W, Badri T; Erythema Multiforme. StatPearls, 2021.
- Trayes KP, Love G, Studdiford JS; Erythema Multiforme: Recognition and Management. Am Fam Physician. 2019 Jul 15;100(2):82-88.
- Hafsi W, Badri T; Erythema Multiforme.
- Harr T, French LE; Toxic epidermal necrolysis and Stevens-Johnson syndrome. Orphanet J Rare Dis. 2010 Dec 16;5:39.
- Trayes KP, Savage K, Studdiford JS; Annular Lesions: Diagnosis and Treatment. Am Fam Physician. 2018 Sep 1;98(5):283-291.
- Drug allergy: diagnosis and management of drug allergy in adults children and young people; NICE Clinical guideline (September 2014; updated November 2018).
- Soares A, Sokumbi O; Recent Updates in the Treatment of Erythema Multiforme. Medicina (Kaunas). 2021 Sep 1;57(9):921. doi: 10.3390/medicina57090921.
- Sladden MJ, Johnston GA; More common skin infections in children. BMJ. 2005 May 21;330(7501):1194-8.
- Erythema multiforme; E Kechichian et al, Science Direct
- Erythema Multiforme; DermNet
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 13 Mar 2028
14 Mar 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free