Rectal bleeding in children
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 18 Aug 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Rectal bleeding in children article more useful, or one of our other health articles.
In this article:
Rectal bleeding in children is less common than in adults. It can cause a great deal of anxiety amongst parents and thus requires appropriate assessment, explanation and reassurance. The vast majority of rectal bleeding in children is benign but it may indicate serious underlying pathology.
Continue reading below
How common is rectal bleeding in children?
The incidence and prevalence of rectal bleeding in children are poorly documented. Certain causes such as anal fissure are common in general practice. Overall it is not a common presentation in children attending hospital.
History
Back to contentsQuestions to ask about the bleeding
Is the bleeding acute or chronic?
What is the colour of the blood? Is it bright or dark?
Melaena rather than bright red blood indicates bleeding is higher in the bowel (usually duodenal or above).
Anorectal disorders, anal fissures and distal polyps cause bright red bleeding. Dark blood or blood mixed with stool suggests more proximal source of bleeding.
Be aware that massive upper gastrointestinal bleeding can cause bright red rectal bleeding in children when transit time is short.
What is the quantity of bleeding?
Questions to ask about other symptoms
Either accompanying or antecedent to the bleeding:
Is there any vomiting? An infectious cause is suggested by diarrhoea and vomiting, fever, illness in others, recent travel, etc.
Has there been any straining?
What is the character of stools passed? Constipation and large hard stools predispose to fissures. Accompanying diarrhoea and signs of obstruction suggest intussusception, volvulus and, in some groups, even necrotising enterocolitis. Acute bloody diarrhoea in children is a medical emergency.
Has there been any abdominal pain?
Has there been any trauma?
Questions to ask about general health
Is the child eating and thriving?
Is there any past history of illness, including jaundice, blood disorders, or intrauterine or neonatal conditions?
Questions to ask about family history
Is there any history of gastrointestinal disease (acute or chronic)?
Is there any history of haematological disease?
Is there a family history of polyps?1
Questions to ask about medication
Particularly use of:
Non-steroidal anti-inflammatory drugs.
Steroids.
Iron supplements.
Any substances likely to colour the stool (liquorice, bismuth, etc).
Continue reading below
Examination
Back to contentsLook for signs of shock.
Look for signs of bleeding from other areas (oropharyngeal, nasal, etc).
Examination of the skin may reveal evidence of systemic disorders (for example, Henoch-Schönlein purpura and Peutz-Jeghers syndrome).
Examine the abdomen. Look for signs of constipation. Hyperactive bowel sounds may occur with upper gastrointestinal haemorrhage.
Examine the perianal area. Look for evidence of fissures or fistulas and assess perianal skin.
Consider rectal examination. This may reveal polyps, masses or occult blood.
Differential diagnosis
Back to contentsThe likely causes of rectal bleeding in children vary with age.
Swallowed maternal blood:
Occurs in neonates.
Also found in regurgitated milk of breast-fed infants. Maternal nipples may be cracked and sore.
Anal fissure:
Occurs in neonates and infants but also in older children.
Bright red blood and pain are features of this condition.
Fissure is visible on examination and no further investigation is required.
Stool softeners may be needed if the child is constipated.
Close-up view of anal fissure
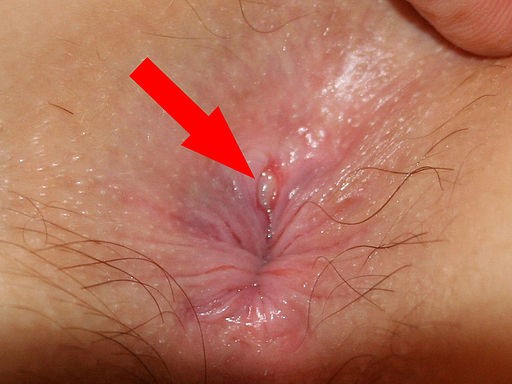
© Bernardo Gui, Public domain, via Wikimedia Commons
Can occur in neonates and infants.
In neonates, it is heralded by sudden onset of melaena and bilious vomiting.
In infants, volvulus can also occur and presenting features include vomiting and abdominal distension.
Rectal bleeding occurs relatively late with development of gangrenous bowel.
Classic plain X-ray finding in midgut volvulus is the double bubble sign. Ultrasound can also be used.
Occurs most often between 4 and 10 months.2
Pain (paroxysms about every 10-20 minutes of colicky abdominal pain), distension, vomiting and a sausage-shaped mass are characteristic, as is the passage of blood and mucus in the form of redcurrant jelly stool.
Abdominal X-ray - may show dilated gas-filled proximal bowel, paucity of gas distally, and multiple fluid levels (but may be normal in the early stages).
Ultrasound - may show doughnut or target sign, pseudokidney/sandwich appearance. It is a very effective modality and many consider it the investigation of choice.
Generally, these cause painless recurrent bleeding.1
In infants and up to teenage years they are most often juvenile polyps which autoamputate and usually require no treatment.
Other polyposis syndromes are diagnosed at colonoscopy.3 Syndromes include juvenile polyps and polyposis, Peutz-Jeghers polyposis and familial adenomatous polyposis.
This is more common in children aged younger than 2 years, and in males.4 5
The patient usually reports bright red blood in the stools. The amount may vary from minimal recurrent episodes to a large shock-producing haemorrhage. Meckel's diverticulum should always be excluded in a child presenting with massive painless rectal bleeding.
Inflammatory bowel disease (IBD):6
This starts to become more common over the age of 2 years.
Bleeding occurs less often with Crohn's disease than with ulcerative colitis but both can cause bloody diarrhoea.
Rectal bleeding usually occurs in children known to have IBD rather than as a presenting feature of the IBD.
Includes that caused by Clostridium difficile and causes bleeding associated with profuse diarrhoea.
Gastroenteritis in many varieties (more commonly Campylobacter spp.).
Rarer causes of rectal bleeding in children
Rare causes need to be considered. Again, how rare a particular cause is can vary with age. It is sometimes necessary to consider upper gastrointestinal bleeding (including all causes such as drugs, gastro-oesophageal reflux, stress ulcers, etc) as a cause for rectal bleeding, as for adults. The shorter transit time in children makes this particularly worthy of consideration where a lower gastrointestinal cause is not obvious and in ill children with massive bleeding.
Occurs in neonates, usually at 3-10 days of age.
Recurrent bleeding in an infant recovering from this condition may indicate recurrence or stricture.
Sexual abuse may present with rectal bleeding. A high index of suspicion in the clinician will be alerted by unusual features in the history or examination.
Cow's milk protein allergy (CMPA) can cause rectal bleeding by way of an allergic proctocolitis. However, isolated rectal bleeding from CMPA is relatively uncommon.7
Solitary rectal ulcer syndrome:
Usually presents in older children (≥8 years old).9
Mucorrhoea, constipation, tenesmus and rectal prolapse are often seen.
Vascular lesions:
Older children/adolescents
In adolescents, the pattern of disease and the possible causes begin more to resemble the pattern in adults. Lower gastrointestinal bleeding is most often caused by:
Anal fissures and haemorrhoids.
Colonic polyps.
Gastroenteritis.
IBD.
Continue reading below
Investigations
Back to contentsMost cases of rectal bleeding in children are benign and self-limiting. The majority of cases will not require any investigation. When bleeding is substantial or recurrent consider:
FBC - anaemia or thrombocytopenia.
Clotting studies - clotting disorder is suspected.
LFTs - liver disease.
Imaging - this is not usually necessary or helpful but may be necessary where more unusual causes of bleeding need to be excluded (in ill children or children with substantial or recurrent bleeding).
Endoscopic examination in children is usually done under general anaesthesia and by specialist paediatric gastroenterologists.13
Management
Back to contentsThe management will depend on the cause and extent of bleeding. As most cases will be simple, self-limiting and benign, management will focus on explanation, reassurance and 'safety-netting'. When bleeding is profuse or recurrent then management will focus on resuscitation, investigation and then treatment of the cause.
Further reading and references
- Durno CA; Colonic polyps in children and adolescents. Can J Gastroenterol. 2007 Apr;21(4):233-9.
- Jiang J, Jiang B, Parashar U, et al; Childhood intussusception: a literature review. PLoS One. 2013 Jul 22;8(7):e68482. doi: 10.1371/journal.pone.0068482. Print 2013.
- Larsen Haidle J, Howe JR; Juvenile Polyposis Syndrome. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2015.
- Sagar J, Kumar V, Shah DK; Meckel's diverticulum: a systematic review. J R Soc Med. 2006 Oct;99(10):501-5.
- Sharma RK, Jain VK; Emergency surgery for Meckel's diverticulum. World J Emerg Surg. 2008 Aug 13;3:27. doi: 10.1186/1749-7922-3-27.
- Rufo PA, Bousvaros A; Current therapy of inflammatory bowel disease in children. Paediatr Drugs. 2006;8(5):279-302.
- Elizur A, Cohen M, Goldberg MR, et al; Cow's milk associated rectal bleeding: a population based prospective study. Pediatr Allergy Immunol. 2012 Dec;23(8):766-70. doi: 10.1111/pai.12009. Epub 2012 Oct 11.
- Kessmann J; Hirschsprung's disease: diagnosis and management. Am Fam Physician. 2006 Oct 15;74(8):1319-22.
- Suresh N, Ganesh R, Sathiyasekaran M; Solitary rectal ulcer syndrome: a case series. Indian Pediatr. 2010 Dec;47(12):1059-61. Epub 2010 Mar 15.
- Abdoon H; Angiodysplasia in a Child as a Cause of Lower GI Bleeding: Case Report and Literature Review. Oman Med J. 2010 Jan;25(1):49-50.
- Tiwary SK, Hakim MZ, Kumar P, et al; Jejunal angiodysplasia causing recurrent gastrointestinal bleeding presenting as severe anaemia and melena. BMJ Case Rep. 2015 Nov 13;2015. pii: bcr-2015-212798. doi: 10.1136/bcr-2015-212798.
- Oliva S, Cohen SA, Di Nardo G, et al; Capsule endoscopy in pediatrics: a 10-years journey. World J Gastroenterol. 2014 Nov 28;20(44):16603-8. doi: 10.3748/wjg.v20.i44.16603.
- Friedt M, Welsch S; An update on pediatric endoscopy. Eur J Med Res. 2013 Jul 25;18:24. doi: 10.1186/2047-783X-18-24.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Aug 2027
18 Aug 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free