Asthma inhalers
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 20 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:AsthmaPeak flow meter for asthma
An inhaler is a device containing a medicine that is taken by breathing it in (inhaling). Inhalers are the main treatment for asthma and help to control asthma symptoms. There are many different types of inhaler.
This leaflet gives information on the medicines inside inhalers, the types of inhaler device and some general information about inhalers. This leaflet is only about inhalers for asthma. It is important to recognise that the same inhalers can be used in other medical conditions (for example, chronic obstructive pulmonary disease) but that the way they are used may be different.
In this article:
Video picks for Asthma
Continue reading below
How do asthma inhalers work?
The medicine inside an inhaler goes straight into the airways when breathed in. This means that a much smaller dose is needed than if it were to be taken as a tablet or liquid by mouth. The airways and lungs are treated but little of the medicine gets into the rest of the body.
The official drug/medicine name is called the generic name. Different drug companies can use the same generic medicine and produce different brands - these are the proprietary medicine names. There are many different brands of inhalers. Inhalers can have generic names and be produced by different drug companies too.
Types of asthma inhalers
Back to contentsThere are different asthma inhaler devices that deliver the same medicine. In the treatment of asthma, the medicine inside inhalers can be divided into:
Relievers (short-acting bronchodilators).
Preventers (steroid inhalers).
Long-acting bronchodilators.
Combination inhalers, which contain both long-acting bronchodilators and steroids.
Reliever inhalers - contain short-acting bronchodilator medicines (also known as SABAs)
These medicines are called bronchodilators as they widen (dilate) the airways (bronchi).
A reliever inhaler is used when needed to ease symptoms of breathlessness, wheeziness or feeling tight-chested. The medicine in a reliever inhaler relaxes the muscle in the airways which opens the airways wider,. Symptoms usually ease quickly.
The two main reliever medicines are called salbutamol and terbutaline. These come in various brands made by different companies. There are different asthma inhaler devices that deliver the same reliever medicine. Salbutamol brands include Airomir®, Salamol®, Salbulin® and Ventolin®. Terbutaline often goes by the brand name Bricanyl®.
These inhalers are usually (but not always) blue in colour. Other inhalers containing different medicines can be blue too so it is important to check the label.
Sometimes, a reliever inhaler is prescribed as the only treatment for asthma, without any other inhalers. However, the UK guidelines changed in 2024, and now recommend that reliever inhalers should not be used as the only treatment for someone with asthma; instead, people with asthma should always use an inhaled steroid as well - either as a separate inhaler, or in a combination inhaler.
This is because a reliever inhaler only provides short-term symptom relief for asthma. It doesn't actually treat the main problem in asthma - inflammation (swelling) of the airways and lungs - but inhaled steroids do.
If you are only using a reliever inhaler, speak to a GP or asthma nurse to discuss a change in treatment.
Preventer inhalers - usually contain a steroid medicine (inhaled corticosteroids - ICSs)
These are taken every day to help prevent asthma attacks and to reduce symptoms of asthma. The type of medicine commonly used in preventer inhalers is a steroid. Steroids work by reducing the inflammation in the airways. When the inflammation is reduced, the airways are much less likely to become narrow and cause symptoms such as wheezing.
Steroid inhalers are usually taken twice per day and sometimes more frequently during an exacerbation (flare-up) of asthma symptoms.
It takes 7-14 days for the steroid in a preventer inhaler to build up its effect. This means it does not give immediate relief of symptoms (like a reliever does). After a week or so of treatment with a preventer, the symptoms have often gone or are much reduced. It can sometimes take up to six weeks for maximum benefit.
If asthma symptoms are well controlled with a regular preventer, then a reliever inhaler should only be needed occasionally and sometimes not at all.
The aim of treatment with asthma inhalers is to manage asthma symptoms so that the reliever inhaler should almost never be needed.
Inhalers that contain a medicine called nedocromil (brand name Tilade®) are sometimes used as preventers, particularly in adults and in children aged over 5 years. However, they do not usually work as well as inhaled steroids and have not been shown to work at all in children under 5. They are no longer recommended.
The main inhaled steroid preventer medications are:
Beclometasone. Brands include Clenil Modulite®, and Qvar®. These inhalers are usually brown and sometimes red in colour.
Budesonide. Brands include Easyhaler Budesonide®, Novolizer Budesonide® and Pulmicort®.
Ciclesonide. Brand name Alvesco®.
Fluticasone. Brand name Flixotide®. This is a yellow-coloured or orange-coloured inhaler.
Mometasone. Brand name Asmanex Twisthaler®.
Bone strength (density) may be reduced following long-term use of high doses of inhaled corticosteroids. Therefore people who use steroid inhalers for asthma need to make sure they have a good supply of calcium in their diet. Good sources of calcium include:
Milk and other dairy products.
Bread.
Some vegetables (curly kale, okra, spinach and watercress).
Some fruits (eg, dried apricots).
See the separate leaflet called Preventing steroid-induced osteoporosis.
Long-acting bronchodilator inhalers (LABAs)
The medicines in these inhalers work in a similar way to relievers, but work for up to 12 hours after each dose has been taken. They include salmeterol (brand name Serevent® and Neovent®) and formoterol (brand names Atimos®, Foradil®, and Oxis®).
A long-acting bronchodilator can be added alongside a steroid inhaler if symptoms are not fully controlled by the steroid inhaler alone. This may be in two separate asthma inhalers or in a combined inhaler (see below).
Combination inhalers
Combination inhalers contain two or more different medications. Most combination inhalers for asthma contain an inhaled steroid and a long-acting bronchodilator.
Examples of combination inhalers are:
Seretide® (salmeterol and fluticasone). This is a purple-coloured inhaler.
Because there are lots of different-coloured inhalers available, it is helpful to remember their names, as well as the colour of the device. This might be important when people are being treated by a doctor without the medical records. Keeping a list of the names of medicine inhalers in a wallet or purse can help with this and reduce mistakes and confusion.
Continue reading below
Asthma inhaler regimes
Back to contentsThere are several different ways of using inhalers. They might be recommended by healthcare professionals in different situations. These include:
As-needed reliever only
This involves using a reliever inhaler only when needed to control asthma symptoms.
This used to be a common treatment regime, especially for people with mild or occasional asthma symptoms.
However, it is no longer recommended as a treatment plan for asthma, because it does not prevent asthma attacks, and does not provide as good control of asthma symptoms as other options.
Anti-inflammatory reliever (AIR)
This involves using a combination inhaler that contains a reliever (formoterol) and an anti-inflammatory steroid. This inhaler is only used when you get asthma symptoms. The reliever medication opens up the airways quickly, and the steroid reduces the inflammation and swelling in the lungs.
AIR treatment has replaced as-needed reliever only treatment regimes. It is suitable for people with mild asthma who only get occasional symptoms.
Regular preventer and as-needed reliever
This involves using a preventer inhaler regularly (every day, even if you are feeling well) to treat and control the asthma, and using a reliever only when needed when asthma symptoms flare up.
The preventer inhaler contains a steroid, and may also be given as a combination inhaler.
The aim of treatment is to get things to the stage where you only need to use the reliever inhaler occasionally, or not at all. You should not need to use your reliever inhaler on more than three days a week.
If you do, it means your asthma is not well controlled - speak to your doctor or asthma nurse, and they may suggest a change in treatment to get things better.
MART therapy
MART stands for maintenance and reliever therapy. MART involves using one single combination inhaler, instead of separate preventer and reliever inhalers.
A MART combination inhaler contains formoterol, a long-acting bronchodilator that gets to work quickly, and an inhaled steroid, which treats inflammation and swelling in the airways.
A MART inhaler should be used regularly (twice a day), and should also be taken when asthma symptoms get worse, or if you have an asthma attack.
MART appears to work better than the regular preventer and as-needed reliever regime, and is increasingly being used as the regime of choice for people with moderate or severe asthma.
Inhaler devices
Back to contentsDifferent inhaler devices suit different people. Asthma inhaler devices can be divided into five main groups:
Pressurised metered dose inhalers (MDIs).
Breath-activated inhalers - MDIs and dry powder inhalers.
Soft mist inhalers.
Inhalers with spacer devices.
Nebulisers.
The standard MDI inhaler
MDI inhaler
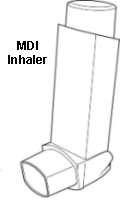
A standard MDI is shown above. The MDI has been used for over 40 years and is used to deliver various types and brands of asthma medicines. It contains a pressurised inactive gas that propels a dose of medicine in each 'puff'. Each dose is released by pressing the top of the inhaler.
This type of inhaler is quick to use, small and convenient to carry. It needs good co-ordination to press the canister and breathe in fully at the same time. Sometimes these are known as evohalers (depending upon the manufacturer).
The standard MDI is the most widely used inhaler. However, MDIs are difficult to use properly. Common errors include:
Not shaking the inhaler before using it.
Inhaling too sharply or at the wrong time.
Not holding your breath long enough after breathing in the contents.
MDIs are best used with a spacer (see below), which helps the medicine to get to the right place in the lungs.
MDIs contain a gas (propellant) which is a greenhouse gas, and can contribute to global warming.
Some brands of newer MDIs have much lower carbon footprints than others, despite having the same ingredients and the same effect on asthma treatment. Many healthcare professionals are recommending a switch to more environmentally-friendly inhalers.
Dry powder inhalers and soft mist inhalers (see below) have a lower carbon footprint, and don't contain greenhouse gases.
Breath actuated MDI
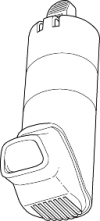
Breath-activated inhalers
These are alternatives to the standard MDI. Some are still pressurised MDIs, but don't need the canister on top to be pressed. The autohaler shown above is an example. Another example of a breath-activated MDI is the easi-breathe inhaler.
Other breath-activated inhalers are also called dry powder inhalers. These inhalers do not contain the pressurised inactive gas to propel the medicine. A dose is triggered by breathing in at the mouthpiece.
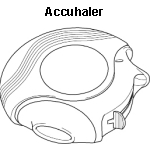
Accuhalers, clickhalers, easyhalers, novolizers, turbohalers and twisthalers are all breath-activated dry powder inhalers. Some types are shown below.
Accuhaler
Turbohaler
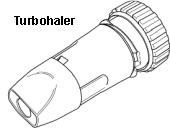
The individual devices all have some differences in how they are operated but, generally, they require less co-ordination than the standard MDI so can be useful for people with arthritis of their hands or who struggle with co-ordination. However, they do require the ability to take a significant breath in. They tend to be slightly bigger than the standard MDI.
Soft mist inhalers
Soft mist inhalers use liquid medicine to create a mist that is inhaled. They are easy to use for most people, and are less likely to cause coughing or irritation of the throat than MDIs or dry powder inhalers.
Spacer devices
Asthma spacer adult

© Tradimus, CC BY-SA 3.0, via Wikimedia Commons
Spacer devices are used with pressurised MDIs. They increase the amount of inhaled medication reaching the lungs by up to 70%, making them much more effective. They also reduce the amount of medication which gets into the rest of the body, therefore reducing side effects.
There are various types but they all work in the same way - an example is shown above. The spacer between the inhaler and the mouth holds the medicine like a reservoir when the inhaler is pressed.
A valve at the mouth end ensures that the medicine is kept within the spacer until it is breathed in. On breathing out, the valve closes. Good co-ordination is not needed. Spacers are not easy to use when out and about as they are quite bulky - however all MDI asthma inhalers should be used through a spacer when at home.
A face mask can be fitted on to some types of spacers instead of a mouthpiece. This is sometimes done for young children and babies who can then use the inhaler simply by breathing in and out normally through the mask.
There are several different types of spacer. Examples are Able Spacer®, Aerochamber Plus®, Optichamber®, Pocket Chamber®, Volumatic® and Vortex®. Some spacer devices fit all MDIs; others are only compatible with specific brands of inhalers.
Tips on using a spacer device
These have a valve at the mouth end - the spacer in the picture above is an example:
Do one puff at a time, even if the prescribed dose is more than one puff.
Shake the inhaler before firing each puff.
Start breathing in from the mouthpiece as soon as possible after firing the puff.
Try to hold your breath for a few moments when you have breathed in.
Breathe in and out a few times with your mouth around the mouthpiece before firing the next puff. Normal breaths are fine - this is sometimes known as tidal breathing.
Check that the valve opens and closes with each breath.
A face mask can be put on to the valve end for babies and young children. They just breathe normally with their face against the mask. The valve opens and closes with each breath in and out. Hold the spacer slightly tilted with the inhaler end uppermost to help the valve open and close easily.
Static charge can build up on the inside of the plastic chamber. This can attract particles of medicine, and reduce the output when the spacer is used. To prevent this, wash the plastic spacer as directed by the maker's instructions. This is usually before first use, and then about once a month with washing up liquid and water. Let it dry in air without rinsing or wiping.
Nebulisers
Nebulisers are machines that turn the liquid form of a short-acting bronchodilator medicines into a fine mist like an aerosol. This is breathed in with a face mask or a mouthpiece.
Nebulisers are no more effective than normal inhalers and should never be bought without advice from an expert in asthma (a respiratory nurse or consultant, or a GP or practice nurse). They are occasionally useful in people who are very tired (fatigued) with their breathing or in people who are very breathless all the time.
Nebulisers are used mainly in hospital for severe attacks of asthma when large doses of inhaled medicines are needed. They are used less commonly than they were in the past as modern spacer devices are as good as nebulisers for giving large doses of inhaled medicines.
Continue reading below
Are there any side-effects from asthma inhalers?
Back to contentsAt standard doses, the amount of medicine in asthma inhalers is small compared with tablets or liquid medicines. Therefore side-effects tend to be much less of a problem than with tablets or liquid medicines which is one of their main advantages. However some side-effects do occur in some people. The leaflet which comes with the inhaler will detail all possible side effects but these are the more common or important ones:
Sore throat
Sometimes when using a steroid inhaler (particularly at high doses) the back of the throat can feel sore. Sometimes the voice can become more hoarse as well. Thrush infection in the mouth can also develop which can usually be treated easily with medication if needed.
Rinsing the mouth with water and brushing teeth after using a steroid inhaler reduces the likelihood of developing a sore throat or thrush. Also, some inhaler devices or using an asthma inhaler via a spacer are less likely to cause throat problems. A change to a different device may help if mouth problems or thrush occur.
Note: A persistent hoarse voice that does not settle after three weeks needs further investigation as it can be due to other causes. If you have this symptom you should seek medical advice.
Osteoporosis
A high dose of inhaled steroid over a long time may be a risk factor for developing osteoporosis. You can help to prevent osteoporosis by taking regular exercise, not smoking, maintaining a healthy weight and eating a diet with enough calcium.
Delayed growth in children
Children who use an inhaled steroid over a long time should have their growth monitored. There is a small risk that enough steroid may get from the lungs and into the body (via the bloodstream), to delay growth. This risk has to be balanced against the risk of a child with asthma not having a steroid preventer - which can include more frequent asthma attacks (requiring oral steroids), hospitalisation, poor growth and death.
The latest studies suggest that adult height could be reduced by 1.2cm by the use of several years of inhaled steroids but that the use of oral steroids for asthma attacks and the effects of long-term ill-health such as severe asthma also affect growth.
Mental health problems
Steroid medicines may aggravate depression and other mental health problems and may very rarely cause mental health problems. This is more common with steroid tablets but can very occasionally be caused by steroid inhalers. Medical advice should be sought if worrying mood or behavioural changes occur.
Which asthma inhaler device should I use?
Back to contentsThis depends on various factors such as:
Convenience. Some inhalers are small, can go easily in a pocket, and are quick to use - for example, the standard MDI inhaler.
Age. Children under the age of 6 years generally cannot use dry powder inhalers because they are unable to generate the strength of breath needed to inhale the medicine . Children aged under 12 years generally cannot use standard MDI inhalers properly without a spacer. Some elderly people find the MDI inhalers difficult to use.
Co-ordination. Some devices need more co-ordination than others.
Side-effects. As discussed earlier, if thrush or sore throat develops, a different device might be recommended.
Often the choice of inhaler is just personal preference. Most GPs and practice nurses have a range of devices to demonstrate.
Patient picks for Asthma

Chest and lungs
Peak flow meter for asthma
This leaflet provides information about the peak flow meter which is used by some people with asthma.
by Dr Doug McKechnie, MRCGP
Chest and lungs
Asthma
Asthma is a common condition that affects the airways. The typical symptoms are wheeze, cough, chest tightness, and shortness of breath. Symptoms can range from mild to severe. Treatment usually works well to ease and prevent symptoms. Treatment is usually with inhalers. This leaflet gives a general overview of asthma. There are other separate leaflets in this series.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Asthma: diagnosis, monitoring and chronic asthma management (BTS, NICE, SIGN); NICE guideline (November 2024)
- Global Strategy for Asthma Management and Prevention; Global Initiative for Asthma – GINA. 2024.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Jan 2028
20 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.