Pneumonia
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Mohammad Sharif Razai, MRCGPLast updated 24 Jan 2023
Meets Patient’s editorial guidelines
In this series:Chest infectionAcute bronchitisAspiration pneumoniaPost-operative chest infectionBronchoscopy
Pneumonia is an inflammation of the lung tissue. It is usually due to infection. Pneumonia tends to be more serious than bronchitis. Bronchitis is an inflammation or infection of the large airways - the bronchi. Sometimes bronchitis and pneumonia occur together - this is called bronchopneumonia.
In this article:
Have you seen posters in your GP's waiting room warning about the unnecessary use of antibiotics for coughs and colds? You may also have seen adverts on the TV about the dangers of pneumonia and how important it is for some people to get vaccinated. Confusing, isn't it? Well, this leaflet is designed to help you tell the difference between pneumonia and a run of the mill chest infection, when to see a doctor, and the treatment you may need.
Continue reading below
What is pneumonia?
Pneumonia is inflammation of the lung tissue usually caused by a bacterial infection (such as Mycoplasma pneumoniae and Streptococcus pneumoniae), but it can also be caused by viral infections such as COVID-19.
This infection leads to the air sacs in your lungs (alveoli) being filled with fluid, which makes it hard for oxygen to reach your blood stream. This means patients have trouble breathing.
Pneumonia can affect either one or both lungs and you can even have it without knowing. This is sometimes called walking pneumonia.
Anybody can catch pneumonia but is mostly affects people younger than 2 or over the age of 65 due to their weakened immune systems. Smoking and alcohol consumption may also raise your risk of catching pneumonia.
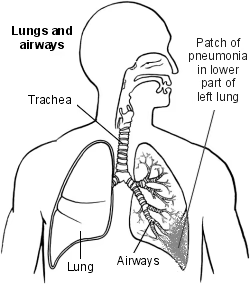
It's often more serious than bronchitis, which is inflammation or infection of the large airways - the bronchi (see diagram). You can get both conditions at the same time. This is called bronchopneumonia.
Pneumonia patch diagram
What causes pneumonia?
Pneumonia is an infection commonly caused by a germ. The germ is usually a bacterium or a virus (viral pneumonia). There are three or four different bacteria that are the most common causes of different types of pneumonia. There is also a well-known group of bacteria that causes pneumonia in about 3 out of 10 cases. They are called atypicals. Other germs such as fungi, yeasts, or protozoa can sometimes also cause pneumonia (fungal pneumonia).
Rarely, non-infective pneumonia is caused by inhaling poisons or chemicals. Many different substances can cause this. They can be in the form of liquids, gases, small particles, dust or fumes.
You may breathe in some bacteria, viruses, or other germs. If you are normally healthy, a small number of germs usually doesn't matter. They will be trapped in your phlegm (sputum) and killed by your immune system. Sometimes the germs multiply and cause lung infections. This is more likely to happen if you are already in poor health or have certain health conditions- for example:
If you are frail or elderly.
If you have a chest disease.
If you have a low immunity to infection (weakened immune system). Low immunity can be caused by such things as immunosuppressant medication, untreated HIV, or another serious illness.
However, even healthy people sometimes develop pneumonia.
Pneumonia can sometimes develop after a large operation like organ transplant, though particularly after operations in the region of your head or neck. Having an anaesthetic can increase the risk. This can be referred to as hospital acquired pneumonia.
Aspiration pneumonia
A particular type of pneumonia is known as aspiration pneumonia. Small amounts of stomach contents or liquid produced in the mouth or throat can be inhaled into the lungs. The inhaled substance can be very irritating to the lungs, cause infection or block the smaller airways. Aspiration pneumonia usually happens in frail, elderly people, people who are drowsy or unconscious, or people who have conditions which cause swallowing difficulties.
Is pneumonia contagious?
It is possible to catch pneumonia from an infected person. The bacteria that cause pneumonia can be breathed in via sneezes or coughs. These bacteria can also be transferred to you by touching a surface an infected person has come into contact with.
However, not everybody exposed to pneumonia-causing bacteria will develop pneumonia.
Similarly, it can depend on the type of pneumonia. If the source of pneumonia is from viral infection, contact with an infected person may transfer the virus, but you may not develop pneumonia as a result.
Usually, your immune system will destroy the bacteria or virus and you'll be fine, but pneumonia infection does sometimes occur in healthy people.
Continue reading below
What are the symptoms of pneumonia?
The common symptoms of pneumonia include:
Cough.
Feeling generally unwell.
A high temperature (fever).
Loss of appetite.
Sweating.
Shivering.
Headaches.
Aches and pains.
All these symptoms are also seen in flu (influenza) so it is sometimes difficult to diagnose pneumonia in the early stages. See the separate leaflet called Influenza and Flu-like Illness for further details.
Coughing
Coughing up a lot of phlegm (sputum) is more likely to happen in pneumonia than in flu. The phlegm may become yellow-coloured or green-coloured. It may be streaked with blood, or you may cough up more significant amounts of blood.
Shortness of breath
You may become short of breath, start breathing faster than normal and develop a tight chest. A sharp pain in the side of the chest may develop if the infection involves the pleura. The pleura is the membrane between the lung and the chest wall. A doctor may hear crackles when listening to your chest with a stethoscope.
When should you see a doctor for pneumonia?
If you have asthma or chronic obstructive pulmonary disease (COPD) you should ask your doctor for advice. They may have given you recommendations about increasing your inhaler medication or taking a 'rescue pack' of antibiotics and steroid tablets at the first sign of an infection. For those with asthma, this information may be in your personalised asthma action plan. If not, speak with them for advice if you develop symptoms of a chest infection.
There are a number of pneumonia symptoms that mean you should see a GP even if you do not have any other lung problems. They include:
If a fever, wheezing or headache becomes worse or severe.
If you develop fast breathing, shortness of breath, or chest pains.
If you cough up blood or if your phlegm becomes dark or rusty-coloured.
If you become drowsy or confused.
If a cough lasts for longer than 3-4 weeks.
If you have repeated bouts of acute bronchitis.
If any other symptom develops that you are concerned about.
Continue reading below
How is pneumonia diagnosed?
Symptoms
A doctor will suspect pneumonia from asking about your symptoms and how you are feeling. They may also ask about your medical history and that of your family. They will be interested in whether you smoke, how much and for how long. The examination may include checking your temperature. Sometimes your doctor will check how much oxygen is circulating around your body. This is done with a small device that sits on the end of your finger and measures the amount of oxygen in your blood. The doctor will listen to your chest, so they may want you to lift or take off your top. If you want a chaperone during the examination, the doctor will arrange one. If you have asthma, they may ask you to check your peak flow measurement. They will listen to your chest with a stethoscope. Tapping your chest over the infected lung is also sometimes performed. This is called percussion. An area of infected lung may sound dull.
X-ray
A chest X-ray may be required to confirm the diagnosis and to see how serious the infection is.
Other tests
These tests are usually carried out if you need to be admitted to hospital. They include sending a sample of phlegm (sputum) for analysis and blood tests to check if the infection has spread to your blood.
Pneumonia treatment
Home treatment
Treating pneumonia at home may be fine, if you are normally well and the pneumonia is not severe.
An antibiotic such as amoxicillin is prescribed when pneumonia is suspected. Once pneumonia is diagnosed, it's best to start treatment within four hours. Infection with a germ (bacterial infection) is a common cause and antibiotics kill bacteria. Amoxicillin is usually effective against the most common causes. If it doesn't seem to be effective and your doctor suspects a less common bacterium, they may change it. If you are allergic to penicillin (amoxicillin is a type of penicillin) your doctor will prescribe an alternative that works just as well. Providing you can take them, antibiotics in capsule, tablet or liquid form are preferred to injections through a vein (intravenous). Antibiotic treatment is usually effective, and you can expect to recover fully. Symptoms should start to improve after three days if the treatment is working. In most cases, antibiotics can be stopped in five days, unless you are still very unwell. You may feel tired for a while after the infection has cleared. If the symptoms persist for longer than three weeks, you should ask your doctor to check you again.
Have lots to drink, to avoid becoming lacking in fluid in the body (dehydrated).
Take regular paracetamol to ease high temperature (fever) and headaches.
Let a doctor know if symptoms do not improve over the following three days.
How long does pneumonia last?
How long pneumonia lasts depends on the severity of the illness. The NHS advises that it may take up to 6 months to feel completely back to normal. However, after 4-6 weeks, symptoms should have substantially reduced in mild cases.
Pneumonia hospital treatment
Hospital admission may be advised if you have severe pneumonia, or if symptoms do not quickly improve after you have started antibiotic treatment. Also, you are more likely to be treated in hospital if you are already in poor health, or if an infection with a more serious infecting germ is suspected. For example, if infection with Legionella pneumophila (the bacterium that causes Legionnaires' disease) is suspected. Even if you are in hospital, you are likely to be offered antibiotics in capsule, tablet or liquid form unless you have difficulties taking them, in which case they may be given through a vein, or if the condition is thought to be so serious that you need the antibiotics through a vein. Your antibiotic treatment will be stopped after five days, unless you are very unwell.
Sometimes oxygen and other supportive treatments are needed if you have severe pneumonia. Those who become severely unwell may need treatment in an intensive care unit or high dependency unit.
When you return home, even though the infection is treated, you may feel tired and unwell for some time.
Is pneumonia deadly?
If you are well enough to be looked after at home, the outlook (prognosis) for pneumonia is very good. Less than 1 person in 100 will die as a result of pneumonia. Those who die tend to be people who are older, those with weakened immune systems, or those who also have other health problems.
If you need to be looked after in hospital, the outlook is not quite so good. 5-14 people in 100 admitted with pneumonia to an ordinary ward rather than an intensive care unit may die. Again, these will usually be people who were unwell before they had pneumonia, or the elderly.
If the pneumonia is very severe or caused by an aggressive type of germ (bacterium), such as legionella, you may need to be moved to an intensive care unit in the hospital. In these cases of pneumonia, the outlook is much worse. Unfortunately, over 30% of these people may die.
If you are normally well but then developing repeated bouts of pneumonia, it may be the first sign of a problem of your lung (lung abscess) or immune system. Some tests of your immune system may be advised if pneumonia happens again for no apparent reason.
How to prevent pneumonia
One of the most effective methods of preventing pneumonia is through immunisation against the pneumococcus (the most common cause of bacterial pneumonia), and by having the annual flu (influenza) virus immunisation. These are both advised if you are at greater risk of developing these infections.
See the separate leaflets called Pneumococcal Immunisation and Immunisation for Flu (Flu Jab) for further details.
Cigarette smoke damages the lining of the airways and makes the lungs more prone to infection. So, stopping smoking will lessen your risk of developing lung infections.
Further reading and references
- Pneumonia: Diagnosis and management of community- and hospital-acquired pneumonia in adults; NICE Clinical Guideline (December 2014 - last updated October 2023)
- Cough (acute): antimicrobial prescribing; NICE Guidance (February 2019)
- Pneumonia (community-acquired): antimicrobial prescribing; NICE Guidance (September 2019)
- Pneumonia (hospital-acquired): antimicrobial prescribing; NICE Guidance (September 2019)
- Annotated BTS Guideline for the management of CAP in adults; British Thoracic Society (2009 - Summary of recommendations updated 2015)
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 23 Jan 2028
24 Jan 2023 | Latest version

Feeling unwell?
Assess your symptoms online for free