Blue naevus
Peer reviewed by Dr Laurence KnottLast updated by Dr Colin Tidy, MRCGPLast updated 31 Mar 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: Tièche-Jadassohn naevus, Jadassohn-Tièche naevus, common blue naevus, cellular blue naevus, chromatophoroma, melanofibroma
Continue reading below
What is a blue naevus?
A melanocytic naevus (or 'mole') is a common benign skin lesion due to a local proliferation of pigment cells (melanocytes). A brown or black melanocytic naevus contains the pigment melanin, so may also be called a pigmented naevus. The blue naevus is a uniform structureless lesion, steel blue in colour.1
A blue naevus is a small blue- or grey-coloured lesion of the skin, with an appearance similar to a mole. They derive their blue colour from their pigmentation with melanin and relatively deep position within the epidermis. One theory of blue naevus's origin is that they represent embryonic neural crest cells that have failed to migrate into the epidermis in the usual fashion:2 . There are two forms
Common blue naevus
The most common form, 2-7 mm in diameter.
Slightly raised and smooth lesion with macular, papular or plaque-like appearance.
Grey-blue to bluish-black in colour.
Does not have any malignant potential.
Usually a solitary lesion with a predilection for the head (especially the scalp), neck, sacral area and dorsum of the hands/feet.
Cellular blue naevus
Much rarer than the common form.
Larger lesion, often 1-3 cm in diameter.
Raised lesions with a smooth surface.
The same colour as the common form.
Often solitary and found on the buttocks, sacral region and the back of the hands/feet.
Large blue naevi on the trunk have been reported with cellular changes similar to a melanoma, although metastases have never been reported.3
How common is blue naevus? (Epidemiology)4
Back to contentsBlue naevi are present from a young age but relatively unusual at birth.5
They are common in Asian populations, with a prevalence of 3% of Japanese. The prevalence in white adults has been reported as 0.5-4%.
They are around twice as common in women as they are in men.
Continue reading below
The visual appearance of blue naevus
Back to contentsBlue naevus
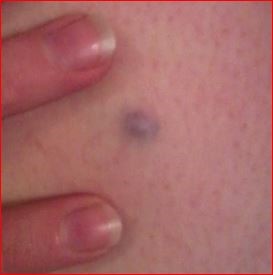
© Dannii Brighton, CC BY-SA 3.0, via Wikimedia Commons
By Dannii Brighton, CC BY-SA 3.0, via Wikimedia Commons
Blue naevus symptoms (presentation)
Blue naevus usually arises during the second decade and do not change in shape or size thereafter.
Rarely, they can be present from birth.
If the cellular form of the lesion undergoes malignant transformation this usually manifests as a precipitate increase in size or, more rarely, as ulceration.6
Blue naevus can be found as pigmented lesions at unusual sites - eg, the female genitourinary tract,7 8 beneath nails, spermatic cord, bronchus, lymph nodes and prostate. Blue naevi found in the oral mucosa are rare but can have tendency to malignancy.9
Differential diagnosis for blue naevus10 11 12
Back to contentsMelanocytic naevus.
Combined naevus.
Compound naevus.
Neurofibroma.
Histiocytoma.
Tattooing effect (deliberate, or material accidentally pushed into the skin during trauma - eg, coalminer's tattoo, ink pens).
Thrombosed plantar wart.
Apocrine hydrocystoma.
Congenital naevus.
Granuloma telangiectaticum.
Naevi of Ota and Ito.
Continue reading below
Associated diseases
Back to contentsCarney's syndrome/complex is a rare association of blue naevi with further abnormalities of the skin and other organs, inherited in an autosomal dominant fashion.
Blue naevus causes cardiac, endocrine, cutaneous and neural myxomatous tumours, plus a variety of pigmented lesions of the skin and mucosae.13
Investigations
Back to contentsNone is usually required.
If the nature of a lesion is uncertain then dermoscopy may be performed by a dermatologist to distinguish it from melanomatous lesions.
Occasionally even dermoscopy is insufficient and biopsy may be required.14
Fluorescence in situ hybridisation (FISH) assay is sometimes needed to diagnose cellular blue naevi from blue naevus-like melanoma.15
Blue naevus treatment and management 16 17
Back to contentsTypical lesions with no other features that would suggest an alternative diagnosis, particularly melanoma, can be left alone, and the patient reassured.
However, as for any pigmented lesion, where there is doubt as to the diagnosis, it is safest to refer for dermatological advice.
There are occasional reports of recurrence of the lesion in a satellite form after excision; such lesions must be examined by further excision biopsy, preferably with dermatological opinion, to exclude malignant transformation.
Complications of blue naevus
Back to contentsCommon blue naevi do not have any complications, are benign and persist unchanged throughout life.
Cellular blue naevi are also usually benign but may, rarely, undergo malignant transformation.
Cellular naevi are larger and so more likely to present and undergo excision biopsy.
Prognosis
Back to contentsThe prognosis for both types of lesion is excellent.
In the rare cases where cellular naevi become malignant then prognosis is improved by earlier diagnosis, as for melanoma.18
Further reading and references
- Improving outcomes for people with skin tumours including melanoma; NICE Guidance (May 2010 update)
- Tièche-Jadassohn naevus; Whonamedit.com
- Sakamoto S, Oiso N, Narita T, et al; Blue nevus with a dermoscopic appearance of peripheral streaks with branches. Case Rep Dermatol. 2014 Feb 25;6(1):66-8. doi: 10.1159/000360215. eCollection 2014 Jan.
- Melanocytic naevus; DermNet NZ
- Jonjic N, Dekanic A, Glavan N, et al; Cellular Blue Nevus Diagnosed following Excision of Melanoma: A Challenge in Diagnosis. Case Rep Pathol. 2016;2016:8107671. doi: 10.1155/2016/8107671. Epub 2016 May 26.
- North JP, Yeh I, McCalmont TH, et al; Melanoma ex blue nevus: two cases resembling large plaque-type blue nevus with subcutaneous cellular nodules. J Cutan Pathol. 2012 Dec;39(12):1094-9. doi: 10.1111/cup.12015. Epub 2012 Nov 12.
- Leung AKC, Barankin B; An adolescent with a smooth, blue-black nodule on the dorsal wrist. Consultant Pediatricians. 2014;13(11):501-503.
- Lawrence F; Neonatal and Infant Dermatology, 2014.
- Kasturi S et al; Cellular blue nevus - A challenging entity. International Archives of Integrated Medicine, Vol. 2, Issue 2, February, 2015.
- Craddock KJ, Bandarchi B, Khalifa MA; Blue nevi of the Mullerian tract: case series and review of the literature. J Low Genit Tract Dis. 2007 Oct;11(4):284-9.
- Fitzhugh VA, Houck K, Heller DS; Vaginal blue nevus: report of a case and review of the literature. J Low Genit Tract Dis. 2011 Oct;15(4):325-7. doi: 10.1097/LGT.0b013e318213f3b8.
- Santos Tde S, Frota R, Martins-Filho PR, et al; Extensive intraoral blue nevus--case report. An Bras Dermatol. 2011 Jul-Aug;86(4 Suppl 1):S61-5.
- Blue Nevus; DermIS (Dermatology Information System), 2013
- Blue Nevus; American Osteopathic College of Dermatology
- Plensdorf S, Livieratos M, Dada N; Pigmentation Disorders: Diagnosis and Management. Am Fam Physician. 2017 Dec 15;96(12):797-804.
- Carney Complex, Type 1: CNC1; Online Mendelian Inheritance in Man (OMIM)
- Di Cesare A, Sera F, Gulia A, et al; The spectrum of dermatoscopic patterns in blue nevi. J Am Acad Dermatol. 2012 Aug;67(2):199-205. doi: 10.1016/j.jaad.2011.08.018. Epub 2011 Oct 26.
- Gammon B, Beilfuss B, Guitart J, et al; Fluorescence in situ hybridization for distinguishing cellular blue nevi from blue nevus-like melanoma. J Cutan Pathol. 2011 Apr;38(4):335-41. doi: 10.1111/j.1600-0560.2010.01667.x. Epub 2011 Jan 19.
- Blue Naevus; Primary Care Dermatology Society, 2012
- Sardana K, Chakravarty P, Goel K; Optimal management of common acquired melanocytic nevi (moles): current perspectives. Clin Cosmet Investig Dermatol. 2014 Mar 19;7:89-103. doi: 10.2147/CCID.S57782. eCollection 2014.
- Damsky WE, Bosenberg M; Melanocytic nevi and melanoma: unraveling a complex relationship. Oncogene. 2017 Oct 19;36(42):5771-5792. doi: 10.1038/onc.2017.189. Epub 2017 Jun 12.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 30 Mar 2027
31 Mar 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free