Congenital pigmented naevus
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 22 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: congenital melanocytic naevus, naevocellular naevus, giant hairy naevus
A congenital melanocytic naevus is a proliferation of benign melanocytes that are present at birth or develop shortly after birth.1
Congenital pigmented naevi initially appear as flat, pigmented lesions of various sizes. They are usually solitary lesions but can be multiple. They may be very large (giant congenital naevi). Less often they may appear after birth in the first two years of life (congenital naevus tardive). As the lesion ages, it tends to become raised and may become hairy. The main clinical concern is the development of malignant melanoma.
Continue reading below
How common is a congenital pigmented naevus? (Epidemiology)1
Small congenital naevi (less than 1.5 cm adult size) occur in 1 in 100 births.
Medium congenital naevi (1.5–20 cm adult size) occur in 1 in 1000 births.
Giant congenital melanocytic naevi (more than 20 cm adult size) are much rarer (1 in 20,000 live births).
Congenital pigmented naevus symptoms (presentation)
Back to contentsThe naevus may be noted at birth or shortly afterwards. Patients may otherwise present because of cosmetic concerns or concerns about the risk of melanoma.
Medium-sized congenital naevus on the forearm.
Congenital naevus
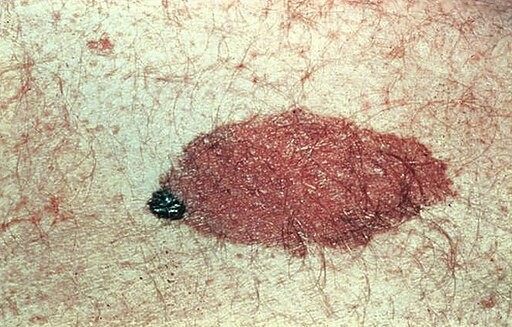
© CDC/ Carl Washington, M.D., Emory Univ. School of Medicine; Mona Saraiya, MD, MPH, Public domain, via Wikimedia Commons
Congenital melanocytic naveus
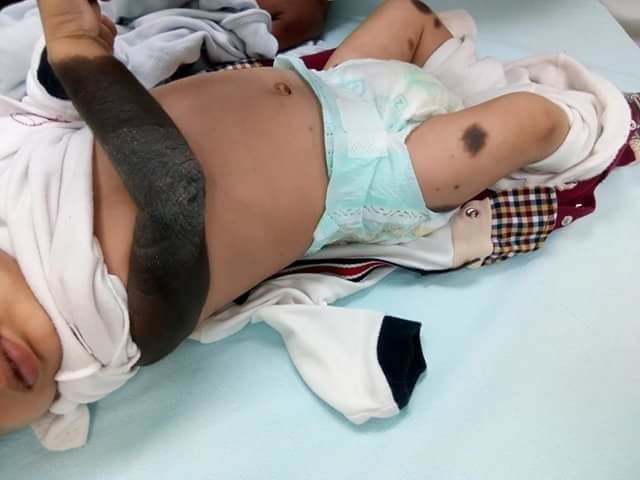
© Mohammad2018, CC BY-SA 4.0, via Wikimedia Commons
Congenital melanocytic naevi usually grow proportionally with the child. As a rough guide, the likely adult size of a congenital naevus can be calculated as:1
Lower limbs: adult size is x 3.3 size at birth.
Upper limbs/torso: adult size is x 2.8 size at birth.
Head: adult size is x 1.7 size at birth.
Continue reading below
Differential diagnosis
Back to contentsSee separate article Pigmented Skin Lesions, which lists "red flag" warning symptoms and signs.
Investigations
Back to contentsTypical small/medium lesions with no suspicious features usually require no investigation.
Dermoscopy may be useful in assessing lesions and determining the degree of suspicion of malignant melanoma.2
Biopsy of the lesion may be used for suspicious lesions; smaller lesions can be subjected to excision biopsy, larger lesions requiring partial biopsy, possibly with dermatological/plastic surgical advice.
Congenital pigmented naevi (particularly giant or multiple lesions) can be associated with neurocutaneous melanosis; if suspected then neuroimaging is advisable, seeking evidence of leptomeningeal melanotic lesions.3
Continue reading below
Associated diseases
Back to contentsNeurocutaneous melanosis (rare congenital syndrome characterised by the presence of large or multiple congenital melanocytic naevi and benign or malignant pigment cell tumours of the leptomeninges).3
Congenital pigmented naevus treatment and management4
Back to contentsIf there is a classical history, no features to suggest melanoma and no desire for cosmetic intervention by the patient, then reassurance about the nature of the lesion is all that is needed.
There is no evidence that surgical removal alters melanoma risk. Lesions which can technically be removed completely are at very low risk, but those at highest risk are not feasible to remove. Surgical removal for cosmetic reasons does have a place in management, particularly for facial lesions, and can involve either serial excision, split-thickness grafting, or balloon expansion.
Congenital melanocytic naevi lighten in line with the patient’s own background skin tone. Hence lighter skinned individuals get more lightening than darker. This happens over a period of years, and the colour of the congenital melanocytic naevus at birth must not be considered to be an appropriate guide to the final colour. Superficial removal techniques such as laser, dermabrasion and curettage do not alter the final colour and any colour change is temporary, and the congenital melanocytic naevus will gradually resume the colour related to the skin tone of the individual. These techniques can be painful with a risk of scarring, and are therefore not recommended.
Complications1
Back to contentsMalignant transformation to melanoma. The risk of melanoma is mainly related to the size of the congenital melanocytic naevus.5
Melanoma is more likely to develop in giant congenital naevi (lifetime estimates are 5–10%), particularly in lesions that lie across the spine or where there are multiple satellite lesions.
It appears that the actual risk of malignant transformation in lesions of small size is less than 1%.
Neurocutaneous melanosis (may cause a variety of neurological problems - particularly hydrocephalus).
Complications associated with excision of lesions (particularly a problem with very large ones).
Congenital neurological disease4
Congenital neurological disease has not been described with a solitary congenital melanocytic naevus at birth, of any size or site. However, the main complication of multiple congenital melanocytic naevi is congenital abnormalities in the central nervous system.
Infants with multiple congenital melanocytic naevi at birth, of any size or site, should have a single screening MRI of the brain and whole spine with contrast, ideally within 0-6 months of life. If the MRI scan is normal (80% of cases with two or more congenital melanocytic naevi at birth) no further routine scans are required, and the neurological outlook is excellent. If the MRI scan shows congenital neurological disease this will need specialist management as necessary.
Prognosis1
Back to contentsPrognosis depends on whether there is any transformation to melanoma and this does not happen in the vast majority of small and medium naevi.
When a melanoma arises within a giant congenital melanocytic naevus, the prognosis is unfavourable due to the deeper origin of the tumour rendering it more difficult to detect on clinical examination, resulting in a later stage at presentation. The deeper location also facilitates earlier spread. In 24% of cases, the melanoma has already spread to other sites (metastases) at the time of the first diagnosis.
Prevention
Back to contentsTo prevent melanoma in all people, but particularly those with large congenital pigmented naevi, advise:
Reducing ultraviolet (UV) light exposure.
Reducing peak sunlight exposure during most intense sun periods.
Use of sunscreens (controversial - some suspect they may increase UV exposure).
Use of hats and clothing to shield from intense sunlight.
Further reading and references
- Navarro-Fernandez IN, Mahabal GD; Congenital Nevus. StatPearls, Jan 2023.
- Congenital melanocytic naevi, DermNet NZ
- Lodha R, McDonald WS, Elgart GW, et al; Dermoscopy for congenital melanocytic nevi. J Craniofac Surg. 2003 Sep;14(5):661-5.
- Di Rocco F, Sabatino G, Koutzoglou M, et al; Neurocutaneous melanosis. Childs Nerv Syst. 2004 Jan;20(1):23-8. Epub 2003 Oct 24.
- Congenital melanocytic naevus; Primary Care Dermatology Society.
- Arneja JS, Gosain AK; Giant congenital melanocytic nevi of the trunk and an algorithm for treatment. J Craniofac Surg. 2005 Sep;16(5):886-93.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Aug 2028
22 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free