Intradermal and compound naevi
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 25 Mar 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
See also the separate Pigmented skin lesions article.
Continue reading below
What are intradermal naevi?1 2
Intradermal naevi are a form of melanocytic naevus. A melanocytic naevus (or 'mole') is a common benign skin lesion due to a local proliferation of pigment cells (melanocytes). A brown or black melanocytic naevus contains the pigment melanin, so may also be called a pigmented naevus.
An intradermal naevus has naevus cell nests in the dermis, and presents as a papule, plaque or nodule with a pedunculated, papillomatous or smooth surface.
Some intradermal naevi may have the same degree of pigmentation as the surrounding skin. They are the classical skin or flesh-coloured 'mole', elevated from the skin's surface, that most people would recognise as such. Some are pigmented.3
Intradermal naevi may appear spontaneously or grow from a pre-existing pigmented mole. They usually develop from the end of childhood onwards and may appear at any stage throughout adulthood, although they are probably quite rare as a new phenomenon after the age of 60. Intradermal naevi have the following characteristics:
Small (5 mm-1 cm).
Raised from the surface of the skin (rounded, dome-shaped, pedunculated or warty appearance).
May be associated with hair growth (particularly in older patients).
How common are intradermal naevi? (Epidemiology)4
Intradermal naevi are extremely common, as are all the melanocytic naevi. Indeed they affect so many people that some consider that they cannot be classed as a pathological entity - rather, a normal variant.
Symptoms of intradermal naevi
Intradermal naevi do not present that often, as most people recognise them as a benign dermatological phenomenon.
They may be detected coincidentally during a consultation, or brought up as a 'whilst I'm here' phenomenon.
They are most likely to present if they are newly noticed.
Visual appearance of intradermal naevi
Intradermal naevi
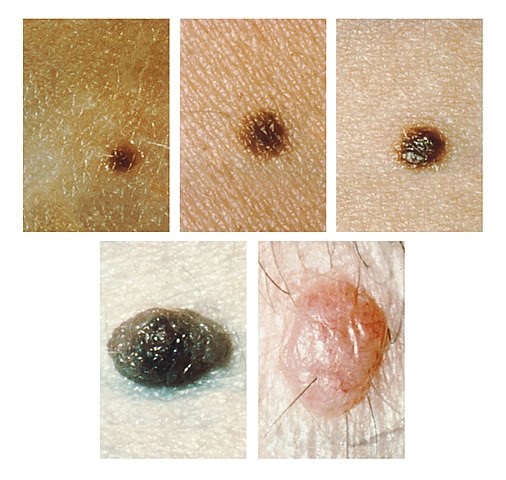
© Unknown photographer, Public domain, via Wikimedia Commons
Differential diagnosis5
History and appearance of intradermal naevi are fairly characteristic and so they are not usually confused with other lesions.
They may resemble early basal cell carcinoma or a neurofibroma.
Basal cell carcinoma will usually have a shorter history, be noted to be growing quite quickly and have associated telangiectasia.
Where there is doubt as to the diagnosis then excision biopsy will resolve the question.
Investigations
None is usually required.
If there has been significant recent growth of intradermal naevi then consider excision biopsy to exclude basal cell carcinoma.
Where a previously non-pigmented lesion develops pigmentation then excision biopsy should be carried out.
Intradermal naevi treatment
No treatment is required unless the patient is concerned about the lesion's cosmetic appearance or there are suspicions of an alternative diagnosis.
Excision biopsy may be used for diagnostic purposes.
Shave and cautery (dermal electrosurgical shave excision) are a good method for removing them, with apparently better cosmetic results than excision biopsy.6
Injection of local anaesthetic directly into the lesion before shaving may improve the cosmetic result.7
Facial lesions may be best removed for cosmetic purposes by a dermatological surgeon or plastic surgeon, particularly in young patients, due to the high risk of medicolegal claims in this area of practice if there is a poor cosmetic outcome.
Complications and prognosis
Intradermal naevi have no complications as such and are benign, slow-growing lesions.
If they occur in the external auditory meatus they can obstruct the auditory canal and impair hearing.8
There are potential complications associated with their removal.
Prognosis is excellent, as it is a benign lesion with no risk of transformation to melanoma.
What are compound naevi?2
Back to contentsCompound naevi have nests of naevus cells at the epidermal-dermal junction as well as within the dermis, and present as a central raised area surrounded by a flat patch.1
Compound naevi are dark brown in colour. Compound naevi are considered to be benign neoplasms of melanocytes if they arise in later life.9
Compound naevi arise from a flat (junctional) naevus that exists earlier in life and may have a raised central portion of deeper pigmentation with surrounding tan-brown macular pigmentation. Pigmentation may be uneven within the naevus but is usually symmetrically distributed. Compound naevi are usually of a round/oval shape and roughly 2 mm-7 mm in diameter. They may exist with a variable degree of pigmentation and even be the same colour as the surrounding skin. Their name is derived from the fact that they contain junctional melanocytes (responsible for their pigmentation) and intradermal melanocytes (responsible for the elevation of the lesion).
How common are compound naevi? (Epidemiology)
Melanocytic naevi in the general population are exceedingly common in congenital and acquired form. Their prevalence is so high that some believe they cannot even be considered an abnormality or pathological entity, as most people with light-coloured skin will have at least a few.10
Compound naevi are much more common in ethnic groups with light skin but they still have an appreciable prevalence in those with more pigmented skin. Congenital melanocytic naevi occur in approximately 1% of newborns at birth. Acquired melanocytic naevi are usually seen from the age of one year, peak in number during the second and third decades of life and disappear between the seventh to ninth decades.11
Signs and symptoms of compound naevi (presentation)
Compound naevi symptoms
Establish if the lesion is congenital or acquired (compound naevi are acquired).
When a lesion presents medically it is important to ascertain whether there have been any associated symptoms such as:
Enlargement.
Change in shape or size.
Change in pigmentation.
Itchiness/pain/irritation.
Bleeding.
Compound naevi signs
Examine the lesion in bright light, preferably daylight if available.
Use drawings or photography to note the site(s), size or shape and pigmentation of the lesion.
Establish that the lesion has the typical pattern of pigmentation and is raised from the level of the skin.
Distinguish from other similar raised benign tumours of the skin:
Dermatofibromas tend to feel firm or hard on palpation, whereas compound naevi are softer.
Seborrhoeic warts tend to have a 'stuck-on' appearance, rather than blending into the surrounding skin.
Melanoma tends to be darker, have an irregular border, be asymmetrical and have recently grown.
Visual appearance of compound naevi
Compound naevus with size gauge
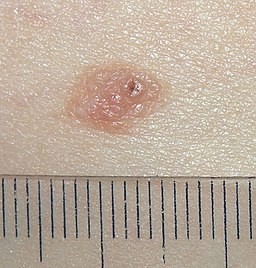
© Jmarchn, CC BY-SA 3.0, via Wikimedia Commons
Compound naevus on left buttock
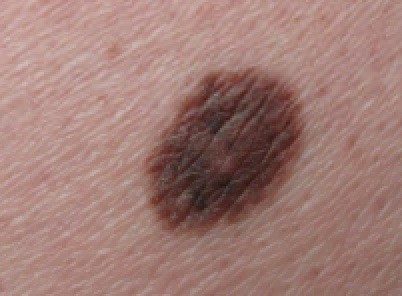
© Dermanonymous, CC BY-SA 4.0, via Wikimedia Commons
Differential diagnosis5
Lentigines.
Atypical mole (dysplastic naevus).
Other melanocytic naevi.
Pyogenic granuloma (usually reddish but may be brown).
Seborrhoeic keratosis.
Acanthoma.
Histiocytoma.
Skin tag (acrochordon).
Neuroma.
Naevi of Ota and Ito.
Diagnosing compound naevi (investigations)
No investigations are indicated in the case of a common, acquired compound naevus that has not undergone any recent change.
Some dermatologists may use dermoscopy to try to distinguish the nature of pigmented lesions.12
If there is any suspicion of malignant melanoma then the investigation of choice is excision biopsy.
Compound naevi treatment
If the diagnosis of compound naevus is clear and there has been no change in a long-standing lesion then reassurance and monitoring of the lesion are all that is usually required.
Where there is any doubt as to the diagnosis of compound naevi, perform excision biopsy or refer for dermatological advice.
Perform excision biopsy whenever the lesion has:
Grown.
Become symptomatic.
Developed asymmetry.
Developed an irregular border.
Altered its degree or pattern of pigmentation.
Developed satellite lesions.
Complications and prognosis
Compound naevi are benign lesions. They do not cause complications and they have an excellent prognosis.
Further reading and references
- Improving outcomes for people with skin tumours including melanoma; NICE Guidance (May 2010 update)
- Almazan-Fernandez FM, Fernandez-Pugnaire MA, Hernandez-Gil J, et al; Homogeneous blue pattern: A rare presentation in an acral congenital melanocytic nevus. Dermatol Online J. 2010 Aug 15;16(8):10.
- Ferreira L, Jham B, Assi R, et al; Oral melanocytic nevi: a clinicopathologic study of 100 cases. Oral Surg Oral Med Oral Pathol Oral Radiol. 2015 Sep;120(3):358-67. doi: 10.1016/j.oooo.2015.05.008. Epub 2015 May 28.
- Melanocytic naevus; DermNet NZ
- Damsky WE, Bosenberg M; Melanocytic nevi and melanoma: unraveling a complex relationship. Oncogene. 2017 Oct 19;36(42):5771-5792. doi: 10.1038/onc.2017.189. Epub 2017 Jun 12.
- Suwattee P, Schram SE, Warshaw EM; Digital polarized light dermoscopy of clinically nonpigmented dermal nevi. Dermatol Surg. 2007 Sep;33(9):1120-5. doi: 10.1111/j.1524-4725.2007.33229.x.
- Intradermal nevus; Libre Pathology, 2014
- Plensdorf S, Livieratos M, Dada N; Pigmentation Disorders: Diagnosis and Management. Am Fam Physician. 2017 Dec 15;96(12):797-804.
- Sardana K, Chakravarty P, Goel K; Optimal management of common acquired melanocytic nevi (moles): current perspectives. Clin Cosmet Investig Dermatol. 2014 Mar 19;7:89-103. doi: 10.2147/CCID.S57782. eCollection 2014.
- Zaiac M, Shah VV, Mlacker S, et al; Local anesthesia injection technique for aesthetic removal of dermal nevi. J Cosmet Dermatol. 2016 Jun 22. doi: 10.1111/jocd.12240.
- Kazikdas KC, Onal K, Kuehnel TS, et al; An intradermal nevus of the external auditory meatus. Eur Arch Otorhinolaryngol. 2006 Mar;263(3):253-5. Epub 2005 Jul 13.
- Trozak D et al; Dermatology Skills for Primary Care: An Illustrated Guide, 2007.
- Compound Nevus; Libre Pathology, 2014
- Russak J et al; Pigmented Lesions in Children, Semin Plast Surg 20(3): 169–179, 2006.
- Kim JK, Nelson KC; Dermoscopic features of common nevi: a review. G Ital Dermatol Venereol. 2012 Apr;147(2):141-8.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 24 Mar 2027
25 Mar 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free