Squamous cell carcinoma of skin
SCC
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 26 Nov 2021
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Skin cancer types article more useful, or one of our other health articles.
In this article:
Continue reading below
What is squamous cell carcinoma?
Primary cutaneous squamous cell carcinoma (SCC) is a malignant tumour that arises from the keratinising cells of the epidermis or its appendages. It is locally invasive and has the potential to metastasise to other organs of the body.1
How common is squamous cell carcinoma? (Epidemiology)
Back to contentsSkin cancers are the most common cancers diagnosed and incidence is rising across the world.
There has been almost a 3-fold increase in incidence in the United States between the 1970s and the 2000s, with an incidence of incidence of 140 per 100,000 American men and 50 per 100,000 American women in 2012.2
SCC is the second most common skin cancer (behind basal cell carcinoma (BCC)).1
Incidence varies by country, skin colour, and outdoor behaviour, and is highest in Australia with an incidence of between 271 and 593 per 100,000 population.3
Cutaneous squamous cell carcinomas are increasing worldwide.4
Risk factors for squamous cell carcinoma2
UV exposure is the most significant risk factor.
Increased susceptibility to UV light exposure occurs in people with type 1 or 2 skin.
Male sex.
Increasing age.
Environmental exposure to other carcinogens including arsenic, polycyclic aromatic hydrocarbons, nitrosamines, alkylating agents, and ionizing radiation.
Immunosuppression.
Pre-existing lesions for example chronic wounds, lichen sclerosus, lichen planus, human papillomavirus, cutaneous lupus erythematoss, actinic keratosis.
Genetic conditions - for example, xeroderma pigmentosum and albinism.
Drugs - a variety of drugs from immunosuppressive agents such as mycofenalate, azathioprine and cyclosporin to diuretics such as hydrochlorothiazide have been associated with an increased risk of cutaneous squamous cell carcinoma. Vismodegib, a hedgehog pathway inhibitor indicated for advanced or metastatic basal cell carcinoma (BCC), was previously shown to have an 8-fold increase of cSCC, but this conclusion has not been reproducible in recent studies.5
Continue reading below
Squamous cell carcinoma symptoms126
Back to contentsSquamous cell carcinomas usually arise within a pre-existing actinic keratosis.
They often grow over weeks or months; they vary from a few mm in size to several cm.
They are typically characterized by a scaly, erythematous, or hyperpigmented papule or plaque.
There may be ulceration or fungation; they are often tender or painful.
They often arise on sun-exposed areas such as the face, forearms, ear, hands and lower legs.
SCC may give rise to local metastases or spread to local lymph nodes.7
Squamous cell carcinoma - forearm
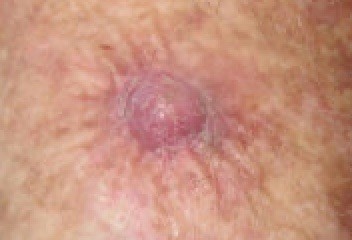
© Dermanonymous(Own work), via Wikimedia Commons
Squamous cell carcinoma - cheek
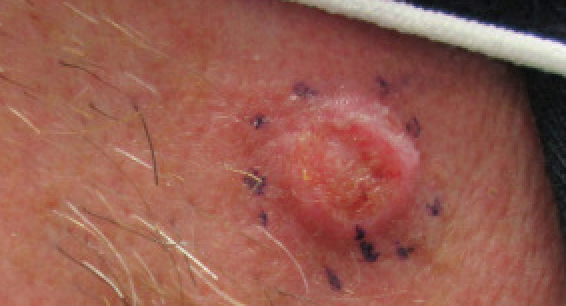
© Dermanonymous(Own work), via Wikimedia Commons
Squamous cell carcinoma - nose
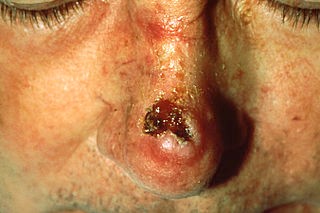
© Unknown photographer, Public domain, via Wikimedia Commons
Differential diagnosis
Back to contentsThere are a number of important conditions which can produce similar-looking skin lesions:
Keratoacanthoma (can be difficult to differentiate even histologically).
BCC.
Malignant melanoma (particularly amelanotic malignant melanomas).
Seborrhoeic warts (especially if traumatised or infected).
Plantar warts or verrucas (beware periungual SCC).
Editor's note |
|---|
Dr Krishna Vakharia, 16th October 2023 Suspected cancer: recognition and referral8 The National Institute for Health and Care Excellence (NICE) has recommended that a person should receive a diagnosis or ruling out of cancer within 28 days of being referred urgently by their GP for suspected cancer. |
Continue reading below
Diagnosing squamous cell carcinoma (investigations)
Back to contentsInvestigation in general practice is primarily by visual inspection and dermoscopy.
Referral
Make a suspected cancer pathway referral (for an appointment within two weeks) for people with a skin lesion that raises the suspicion of squamous cell carcinoma.8
The Scottish Intercollegiate Guidelines Network (SIGN) guideline recommends prompt early referral if there have been high levels of cumulative psoralen plus ultraviolet A photochemotherapy, rapid tumour growth, poorly defined clinical margins or pain/dysaesthesia.9
Further investigations
In advanced stages of disease, further investigations to assess the extent of disease may be required (by the dermatologist):
Imaging including CT scanning (bone or soft tissue spread, particularly cervical lymph nodes) and MRI scanning (particularly for head and neck spread, perineural invasion).
Clinically enlarged nodes should be examined histologically - for example, by fine-needle aspiration or excisional biopsy.
Staging6
Back to contentsCutaneous squamous cell carcinoma is characterised as low- or high-risk depending on the chance of metastases or recurrence.
High-risk cSCC is defined as:
Diameter of 2cm or larger
Located on the ear, vermilion of the lip, central face, hands, feet or genitalia
Occurring in an elderly or immunosuppressed patient
Histological thickness greater than 2mm, poorly differentiated histology or where there is invasion of subcutaneous tissue, nerves or blood vessels.
In 2011, a new staging system was developed for cSCC:
Tumour staging for cutaneous SCC
TX: Th Primary tumour cannot be assessed
T0: No evidence of a primary tumour
Tis: Carcinoma in situ
T1: Tumour ≤ 2cm without high-risk features
T2: Tumour ≥ 2cm; or; Tumour ≤ 2 cm with high-risk features
T3: Tumour with the invasion of maxilla, mandible, orbit or temporal bone
T4: Tumour with the invasion of axial or appendicular skeleton or perineural invasion of skull base
Nodal staging for cutaneous SCC
NX: Regional lymph nodes cannot be assessed
N0: No regional lymph node metastasis
N1: Metastasis in one local lymph node ≤ 3cm
N2: Metastasis in one local lymph node ≥ 3cm; or; Metastasis in >1 local lymph node ≤ 6cm
N3: Metastasis in lymph node ≥ 6cm
Squamous cell carcinoma treatment and management 10
Back to contentsThere should be two levels of multidisciplinary teams: local hospital skin cancer multidisciplinary teams (LSMDTs) and specialist skin cancer multidisciplinary teams (SSMDTs).
All patients with a possible SCC should be referred urgently to a doctor trained in the specialist diagnosis of skin malignancy, normally a dermatologist, who is a member of either an LSMDT or an SSMDT.
In England, the target for patients with SCC referred through the two-week urgent GP referral route is that they must start their first definitive treatment within 62 days of GP referral. For all other patients with SCC in England, the target is that they must start their first definitive treatment within 31 days of the decision to treat. 11
Patients with a high risk of recurrence of skin cancer or of new primary cancers should be followed up in hospital but should still be instructed in self-examination and provided with written and photographic information.
Management options
Surgery:
The standard effective treatment is complete surgical excision and all excised specimens should be sent for histopathological examination. Mohs micrographic surgery shows significant benefit over standard excision with a recurrence rate at 5 years of 3.1% compared with 8.1%. Where the treatment is for a locally recurrent lesion (that had been treated previously), Mohs surgery has a further recurrence rate of 10% compared with 23.3%. 2
Where surgery is contra-indicated then other treatment options include superficial radiation therapy, 5-fluorouracil cream, imiquimod cream, cryotherapy, photodynamic therapy, and/or ablative laser therapy but these have higher recurrence rates than surgery.
Curettage and cautery/electrodesiccation:
Performed using a curette to remove soft material from the tumour. The base of the tumour is then destroyed, using either hyfrecation or cautery.
This is generally only used for low risk tumours on the limbs or trunk. 6
Cryotherapy/cryosurgery:
Can be used for very small low-risk tumours. 6
Radiotherapy:
Is only recommended for patients where surgery is contra-indicated (either because the patient is unsuitable for surgery or because the tumour is inoperable).
Is occasionally used as an adjuvant treatment.
Immunotherapy:
Cemiplimab is a human immunoglobulin G4 monoclonal antibody, which binds to the programmed death-1 (PD-1) receptor. This potentiates an immune response to tumour cells.
It has been recommended since July 2022 as an option in the UK for treating metastatic or locally advanced cutaneous squamous cell carcinoma in adults when curative surgery or curative radiotherapy is not suitable. 12
It can be used for up to 24 months but should be stopped earlier if the disease progresses.
A recent study suggests benefit from cemiplimab with disease control in 62% of patients. 13
Squamous cell carcinoma prognosis 2
Back to contentsThe overall mortality rate of cutaneous squamous cell carcinoma metastasis is low (1-2%).
However the mortality rate is higher in some regions, for example the southern United States.
Approximately 3% of squamous cell carcinomas will metastasise, most commonly to lymph nodes.
There is a 5-year survival rate of 90% in patients with a single lymph node involvement.
Prevention of squamous cell carcinoma
Back to contentsAvoiding sun exposure is the key to prevention, including:
Staying indoors or in the shade as much as possible between 11 am and 3 pm.
Covering up with clothes and a wide-brimmed hat when out in the sunshine.
Applying high sun protection factor sunscreen which also has high ultraviolet A (UVA) protection
Secondary prevention by early detection and effective management is also very important.
Further reading and references
- Squamous cell carcinoma of the skin; DermNet NZ
- Squamous Cell Carcinoma; British Association of Dermatologists, 2022
- Hadian Y, Howell JY, Ramsey ML, et al; Cutaneous Squamous Cell Carcinoma.
- The hidden Australian skin cancer epidemic, high-risk cutaneous squamous cell carcinoma: a narrative review; A Dettrick et al; Pathology
- Huang S, Jiang J, Wong HS, et al; Global burden and prediction study of cutaneous squamous cell carcinoma from 1990 to 2030: A systematic analysis and comparison with China. J Glob Health. 2024 May 3;14:04093. doi: 10.7189/jogh.14.04093.
- Cutaneous Squamous Cell Carcinoma: An Updated Review; R Jiang et al; Cancers
- Cutaneous squamous cell carcinoma; A Oakley, DermNet
- Corchado-Cobos R, Garcia-Sancha N, Gonzalez-Sarmiento R, et al; Cutaneous Squamous Cell Carcinoma: From Biology to Therapy. Int J Mol Sci. 2020 Apr 22;21(8). pii: ijms21082956. doi: 10.3390/ijms21082956.
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated April 2026)
- Management of Primary Cutaneous Squamous Cell Carcinoma; Scottish Intercollegiate Guidelines Network - SIGN (June 2014)
- Maubec E; Update of the Management of Cutaneous Squamous-cell Carcinoma. Acta Derm Venereol. 2020 Jun 3;100(11):adv00143. doi: 10.2340/00015555-3498.
- Skin Cancer; British Association of Dermatologists
- Cemiplimab for treating advanced cutaneous squamous cell carcinoma; NICE Technology appraisal guidance, June 2022
- Real-world evidence study on the early use of cemiplimab in the UK: REACT-CEMI (Real World evidence of advanced CSCC treatment with cemiplimab); A Challapalli et al; Frontiers in Immunology
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 25 Nov 2026
26 Nov 2021 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free