Keloid scars
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 16 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Keloid article more useful, or one of our other health articles.
In this article:
Continue reading below
What is a keloid scar?
A keloid scar is one in which there is overgrowth of dense fibrous tissue. This usually develops after the injury has healed. It extends beyond the borders of the original wound. It does not normally regress spontaneously and it will usually recur after excision. This contrasts with hypertrophic scars, which stay within the borders of the original wound.
The term 'chéloïde' was coined by Alibert in 1806, from the Greek 'chele', meaning crab's claw - to describe the lateral growth of tissue into unaffected skin.1
How common are keloid scars?(Epidemiology)2 3
Back to contentsKeloid scars have long been thought to be more common in people with darker skin tones, especially people of African heritage. However, the evidence of a link between keloid scarring risk and ethnicity has recently been disputed, given weak epidemiological evidence.4
There is equal sex distribution.
The peak age is 20-30 years and keloids are less common at the extremes of age.
Half of patients with keloid have a family history of keloid scar formation, suggesting an inheritable genetic component.
Continue reading below
Keloid causes (aetiology)
Back to contentsThe cause is unknown, although there are various theories, including:5
Dysfunction of the extracellular matrix which controls growth factor activity.
Abnormalities in collagen turnover.
An inherited abnormal response to dermal injury.
An immune reaction to sebum.
Genetic susceptibility - for example, a genome-wide association study (GWAS) found a common genetic risk factor predisposing to the development of keloid, in a sample of Chinese Han and Japanese people.6
Hormonal factors - keloid is associated with pregnancy and puberty.3
Keloid symptoms7 8
Back to contentsHistory
Symptoms: usually cosmetic, although the scar may be tender, painful, itch or produce a burning sensation.
There is usually a history of trauma that may be accidental, surgical or cosmetic.
Sites for keloid formation: the most common areas are the sternum, shoulder, earlobe and cheek.
Keloid on back of ear
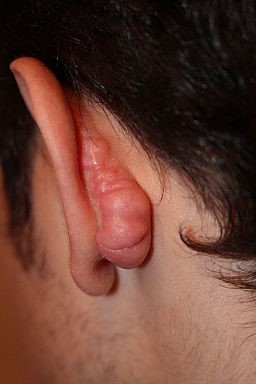
© Htirgan, CC BY-SA 3.0, via Wikimedia Commons
Burn scars or infected lesions, including acne, are more likely to form keloids.
Clinical features
The scar has grown beyond the original line of trauma and may be raised and irregular.
Keloid post-surgery
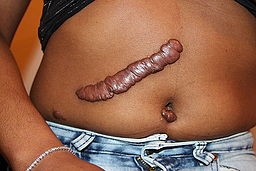
© Htirgan, CC BY-SA 3.0, via Wikimedia Commons
The texture is rubbery.
It is red in the early stages but becomes brown or pale with age.
There are no hair follicles or sweat glands within the scar.
Keloids over a joint can contract and restrict movement.
Clinical course - the natural history is variable:
Most lesions grow for weeks-months but growth can continue for years.
Growth is usually slow but some keloids can enlarge rapidly over months.
When they stop growing, they remain stable or regress slightly.
Assessment
The diagnosis is made clinically in most cases.If there is significant diagnostic uncertainty and alternative diagnoses are suspected, a skin biopsy may be helpful.
Assess the patient's concerns and the impact of the scar(s) on their life.
Check if the scar reduces mobility - eg, near a joint.
Continue reading below
Differential diagnosis3
Back to contentsHypertrophic scars are also red and prominent but do not extend beyond the wound border. Hypertrophic scars usually appear within a month of the injury, grow for several months and then regress, whereas keloid scars may appear later and continue growing for longer.
Keloid scar treatment2
Back to contentsKeloid scars are difficult to treat. There are various options. Reviews suggest that combinations of treatments are probably the most effective.7
Local steroids7 8
Intralesional steroid injections, with triamcinolone, are a mainstay of treatment and prevention - reviews suggest that it improves the majority of scars.
Injections are given every 2-6 weeks until improvement.
Side-effects: pigment changes, telangiectasias and subcutaneous atrophy (which may resolve).
Steroid-impregnated tape applied for 12 hours/day may flatten keloids.
Pressure or occlusive dressings
These are used both for treatment and prevention, with minimal adverse effects, provided they are practical and acceptable to the patient.9
Silicone gel - this is applied as topical gel or a gel-impregnated sheet.7 There is weak evidence that these provide benefit for prevention in people at high risk of keloid scarring; trials showing benefit in the treatment of keloid scars are poor quality and at high risk of bias.10
Compression earrings - are used after excision of earlobe keloids and give good rates of recurrence-free healing; they should be worn 24 hours/day.7
Other pressure dressings may be used.
Surgery8
Surgical excision on its own has a very high recurrence rate and the recurring scar may even be larger than the original. Results can be improved by:
Meticulous surgical technique.
Additional treatments such as intralesional steroids, occlusive or pressure dressings or radiotherapy.
Radiotherapy11
Radiotherapy is an option, particularly post-surgery for the treatment of keloid scars. There have been concerns about its safety, due to its carcinogenic properties but, providing surrounding tissues are protected, the risk is very low. Implantation of radioactive seeds (brachytherapy) post-surgery has limited, but positive, results.12
Cryotherapy2
Cryotherapy has been used alone and combined with other treatments. Reported results vary:
Cryotherapy may stop early-stage keloids from growing.
It may be effective in combination with intralesional steroid.
Hypopigmentation is a side-effect.
Two randomised controlled trials compared intralesional cryotherapy with excision and either corticosteroid injection or brachytherapy; intralesional cryotherapy was inferior to excision and brachytherapy for resistant keloids.13
Other possible treatments
Laser treatment8
The evidence base supporting the use of lasers in keloid scars is not as large as that supporting their use in hypertrophic scars. Further research is required to determine the mechanism of action for different laser systems and to examine such outcomes as scar erythema, scar texture, degrees of symptom relief, recurrence rates and adverse effects.14
One study reported the successful use of carbon dioxide laser ablation followed by intralesional steroids.15
Pulsed dye lasers and Nd:YAG lasers are reported to give encouraging results, with few adverse effects. However, pulsed dye lasers are less effective on dark skin.7 Combination treatment of CO2 fractional laser, pulsed dye laser and triamcinolone acetonide injection has been successfully used for refractory keloid scars on the upper back.16
Laser treatment may reduce the redness of keloids without shrinking them.
A combination of intralesional steroids and intense pulsed light has been found to produce clinical improvement in the size of the scar.17
Interferon therapy
Intralesional interferon alfa-2b has been shown to reduce keloid scars to a greater extent than steroids and may be particularly useful in cases which are resistant to intralesional steroids.18
5-fluorouracil3
May be beneficial when used alone or in combination with other treatments.
Possible side-effects are pain, hypopigmentation and tissue sloughing.
Bleomycin3
This cytotoxic agent can be given locally as intralesional injections and improved scars in one small study. Side-effects were hyperpigmentation and dermal atrophy.
Retinoids
Topical or intralesional retinoids have been used in clinical trials and produced moderate improvements but should not be considered first-line.19
Other treatments being explored include mitomycin C, tamoxifen, methotrexate and imiquimod.19
Keloid scar prevention2 7 8
Back to contentsFor people at high risk of or with a history of keloids:
Avoid body piercing, tattoos and unnecessary incisions such as cosmetic surgery - particularly to skin sites more prone to keloid formation (see under 'Presentation', above).
Treat acne thoroughly to reduce lesions and potential for scarring.
If surgery is required, it may be combined with dressings, intralesional steroids or other treatments (see under 'Management', above) to reduce the likelihood or size of keloid scarring. Care with surgical technique is important.
Further reading and references
- Dong X, Mao S, Wen H; Upregulation of proinflammatory genes in skin lesions may be the cause of keloid formation (Review). Biomed Rep. 2013 Nov;1(6):833-836. Epub 2013 Sep 25.
- Park TH, Park JH, Chang CH; Clinical features and outcomes of foot keloids treated using complete surgical excision and full thickness skin grafting followed by corticosteroid injections. J Foot Ankle Res. 2013 Jul 15;6(1):26.
- Addison T; On the Keloid of Alibert, and on True Keloid. Med Chir Trans. 1854;37:27-47. doi: 10.1177/095952875403700106.
- Juckett G, Hartman-Adams H; Management of keloids and hypertrophic scars. Am Fam Physician. 2009 Aug 1;80(3):253-60.
- Gauglitz GG, Korting HC, Pavicic T, et al; Hypertrophic Scarring and Keloids: Pathomechanisms, Current and Emerging Treatment Strategies. Mol Med. 2010 Oct 5.
- Deyrup A, Graves JL Jr; Racial Biology and Medical Misconceptions. N Engl J Med. 2022 Feb 10;386(6):501-503. doi: 10.1056/NEJMp2116224. Epub 2022 Feb 5.
- Davidson S, Aziz N, Rashid RM, et al; A primary care perspective on keloids. Medscape J Med. 2009;11(1):18. Epub 2009 Jan 20.
- Zhu F, Wu B, Li P, et al; Association study confirmed susceptibility loci with keloid in the Chinese Han population. PLoS One. 2013 May 7;8(5):e62377. doi: 10.1371/journal.pone.0062377. Print 2013.
- Al-Attar A, Mess S, Thomassen JM, et al; Keloid pathogenesis and treatment. Plast Reconstr Surg. 2006 Jan;117(1):286-300.
- Leventhal D, Furr M, Reiter D; Treatment of keloids and hypertrophic scars: a meta-analysis and review of the literature. Arch Facial Plast Surg. 2006 Nov-Dec;8(6):362-8.
- Lebwohl M et al; Treatment of Skin Disease: Comprehensive Therapeutic Strategies, 2013
- O'Brien L, Jones DJ; Silicone gel sheeting for preventing and treating hypertrophic and keloid scars. Cochrane Database Syst Rev. 2013 Sep 12;2013(9):CD003826. doi: 10.1002/14651858.CD003826.pub3.
- Ogawa R, Yoshitatsu S, Yoshida K, et al; Is radiation therapy for keloids acceptable? The risk of radiation-induced Plast Reconstr Surg. 2009 Oct;124(4):1196-201.
- De Cicco L, Vischioni B, Vavassori A, et al; Postoperative management of keloids: Low-dose-rate and high-dose-rate brachytherapy. Brachytherapy. 2014 Feb 17. pii: S1538-4721(14)00025-7. doi: 10.1016/j.brachy.2014.01.005.
- Bijlard E, Timman R, Verduijn GM, et al; Intralesional cryotherapy versus excision with corticosteroid injections or brachytherapy for keloid treatment: Randomised controlled trials. J Plast Reconstr Aesthet Surg. 2018 Jun;71(6):847-856. doi: 10.1016/j.bjps.2018.01.033. Epub 2018 Feb 6.
- Jin R, Huang X, Li H, et al; Laser therapy for prevention and treatment of pathologic excessive scars. Plast Reconstr Surg. 2013 Dec;132(6):1747-58. doi: 10.1097/PRS.0b013e3182a97e43.
- Garg GA, Sao PP, Khopkar US; Effect of carbon dioxide laser ablation followed by intralesional steroids on keloids. J Cutan Aesthet Surg. 2011 Jan;4(1):2-6. doi: 10.4103/0974-2077.79176.
- Martin MS, Collawn SS; Combination treatment of CO2 fractional laser, pulsed dye laser, and triamcinolone acetonide injection for refractory keloid scars on the upper back. J Cosmet Laser Ther. 2013 Jun;15(3):166-70. doi: 10.3109/14764172.2013.780448. Epub 2013 Apr 29.
- Shamsi Meymandi S, Rezazadeh A, Ekhlasi A; Studying intense pulsed light method along with corticosteroid injection in treating keloid scars. Iran Red Crescent Med J. 2014 Feb;16(2):e12464. doi: 10.5812/ircmj.12464. Epub 2014 Feb 5.
- Lee JH, Kim SE, Lee AY; Effects of interferon-alpha2b on keloid treatment with triamcinolone acetonide intralesional injection. Int J Dermatol. 2008 Feb;47(2):183-6. doi: 10.1111/j.1365-4632.2008.03426.x.
- Viera MH, Amini S, Valins W, et al; Innovative therapies in the treatment of keloids and hypertrophic scars. J Clin Aesthet Dermatol. 2010 May;3(5):20-6.
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 15 Nov 2027
16 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free