Keloid
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Caroline Wiggins, MRCGP Last updated 1 Jul 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
A keloid (also called a keloid scar) is an overgrowth of a scar, after the skin has been damaged. It is an abnormal type of wound healing. It is particularly common in people with dark skin or who have family members who have developed keloid scars.
In this article:
Video picks for Other skin problems
Continue reading below
What is a keloid scar?
A keloid scar is an overgrowth of the scar tissue that develops after a wound has healed. It expands beyond the original scar. Rather than stay in a straight line, for example, after a surgical incision, it can spread outwards and also upwards, giving a raised scar.
Who gets keloid scars?
Back to contentsKeloid scars are more common in people with black or brown skin, or white skin that tans after sunburn. Most people who develop a keloid are between 10-30 years old. Half of people with keloids will have members of their family who have also developed keloids.
Continue reading below
What causes keloid scars?
Back to contentsWe don't yet have a definite answer to explain why some people go on to develop keloid scars after an injury. But we have a pretty good idea of how it happens.
Keloid scars are an overgrowth of scar tissue after a skin injury. The keloid becomes larger than the original wound. When a keloid scar is formed, we know that the process of normal scar tissue being created and gradually fading away, to reveal new, healed skin, is changed. There are many ideas being researched about why this may happen, but at the moment we don't know exactly why.
How does a keloid scar form?
Back to contentsKeloid scars typically starts to develop about three months after the original skin injury though it can occur years later. The first thing you will probably notice is that rubbery scar tissue starts growing beyond the borders of the original injury. The growth is usually slow and once they stop growing they usually stay the same size or they can get a bit smaller.
Typical areas keloid scars develop
Keloid scars occur most often on areas of the body where the skin is stretched, rather than where skin feels looser. They are more common on the upper body, for example:
On the ears, after ear piercing.
On the chest or back after chickenpox, acne, or an injury.
On the upper arms or shoulder.
If a keloid scar is over a joint, such as your elbow, it can restrict your ability to move that joint.
Continue reading below
What do keloid scars feel like?
Back to contentsThey are usually smooth, slightly shiny, raised, firm skin growths which extend beyond the original skin injury.
They can feel itchy, prickly or sore.
Many people do not notice any itching or pain.
What do keloid scars look like?
Back to contentsThe image below shows a woman's ear affected by keloid scarring:
Keloid scarring on ear
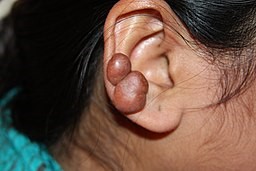
© Htirgan (Own work), CC BY-SA 3.0, via Wikimedia Commons
How does a doctor diagnose a keloid scar?
Back to contentsThere is no particular test for a keloid scar. It is diagnosed by a healthcare professional who will listen to what has happened, ask questions and examine the scar. They may want to look at scars you have elsewhere on your body to compare if this one is different to other ones you have.
Occasionally a keloid scar can mimic other skin tumours.
In that case, a biopsy will need to be taken by a specialist. A biopsy is a procedure where a sample of tissue is taken for further analysis.
The biopsy will be looked at under a microscope and a specialist (histopathologist) will be able to see the typical microscopic features of a keloid scar.
Note: a biopsy is hardly ever necessary because the history - that is, the patient's story - and the appearance of the skin growth allow the healthcare professional to diagnose a keloid without this test.
How to treat keloid scars
Back to contentsMany patients ask for their keloid scar to be 'cut out' (surgically excised). This is hardly ever successful and in fact can result in an even bigger keloid scar coming back. If surgical excision is tried it must be done by a specialist doctor such as a dermatologist or plastic surgeon and will usually be done in combination with another treatment.
Keloid scars can be difficult to treat and treatments can have side effects. It is important to be clear what you would like to achieve with treatment. Some people they want the itch or pain to improve, others want it to look more like the skin around the keloid. The medical team can then consider what treatment options are most likely to achieve what is important to you.
How to reduce keloid scars without surgery
One of the most common methods is injecting steroid (triamcinolone acetonide) and local anaesthetic into the keloid scar itself. The injections are done with a tiny needle, but can be a bit sore. This is called 'intralesional corticosteroid injection treatment':
The steroids and anaesthetic can help to stop the proliferation of the skin cells in the keloid scar.
The injections are usually given once a month for 4-6 months.
Side-effects of the steroids include the skin becoming thin, easily damaged, changing colour to become darker (hyperpigmentation) or lighter (hypopigmentation) than the surrounding skin, or being able to see many tiny blood vessels in the thinned skin.
New research suggests that combining the steroid injections with another form of treatment may reduce the possible side effects from the steroids and still improve the keloid. Many of these options are very new and the research is in small numbers of people and can give conflicting results. Further research is recommended before they are offered as standard treatments.
Other injection options may now include 5-FU, bleomycin, verapamil, hyaluronic acid and hyaluronidase, botulinum toxin, and collagenase.
Other treatment options include cryotherapy (using freezing temperatures), laser, radiofrequency ablation, radiation, and shock-wave therapy.
Sometimes steroids can be applied to the skin as an ointment under a dressing, or in a tape impregnated with steroids. can dampen down a keloid scar. Silicone dressings and compression dressings are also areas of research which have suggested they may help.
How to prevent keloid scars
Back to contentsIf you have a keloid scar then it is more likely future skin injuries will develop into a keloid scar. The best way to stop more keloids developing is to prevent unnecessary skin injuries.
People who are prone to keloid scars are advised to avoid body piercings, tattoos and ideally any surgery unless essential. Steer clear too of unnecessary procedures such as cosmetic surgery, especially in those areas of the body that are prone to keloids.
If you get acne, seek effective treatment at an early stage so the spots do not scar. If you are identified as being at risk of keloid and need an operation, your surgeon may offer you dressings, steroid injections or other treatments to reduce the risk of keloid developing.
Patient picks for Other skin problems

Skin, nail and hair health
Sun and sunburn
This leaflet discusses the risks and benefits of sunlight to your skin. It gives tips on how to enjoy sunshine safely so it you can do you good and reduce the risk of causing harm. It is very important to protect children from the sun. The delicate skin of a child is more sensitive to sun damage than the skin of an adult.
by Dr Caroline Wiggins, MRCGP

Skin, nail and hair health
Psoriasis
Psoriasis is a long-term skin condition that can also affect the nails and joints. It tends to flare up from time to time. Treatment with various creams or ointments can often clear or reduce patches (plaques) of psoriasis. Special light therapy and/or powerful medication are treatment options for severe cases where creams and ointments have not worked very well. People with psoriasis are more likely than usual to develop cardiovascular disease (heart disease and strokes).
by Dr Doug McKechnie, MRCGP
Further reading and references
- Davidson S, Aziz N, Rashid RM, et al; A primary care perspective on keloids. Medscape J Med. 2009;11(1):18. Epub 2009 Jan 20.
- Limmer EE, Glass DA 2nd; A Review of Current Keloid Management: Mainstay Monotherapies and Emerging Approaches. Dermatol Ther (Heidelb). 2020 Oct;10(5):931-948. doi: 10.1007/s13555-020-00427-2. Epub 2020 Jul 23.
- Thornton NJ, Garcia BA, Hoyer P, et al; Keloid Scars: An Updated Review of Combination Therapies. Cureus. 2021 Jan 30;13(1):e12999. doi: 10.7759/cureus.12999.
- Keloid and hypertrophic scar; DermNet.
- Ekstein SF, Wyles SP, Moran SL, et al; Keloids: a review of therapeutic management. Int J Dermatol. 2021 Jun;60(6):661-671. doi: 10.1111/ijd.15159. Epub 2020 Sep 9.
Continue reading below
About the author

Dr Laurence Knott
General Practitioner, Medical Author
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
About the reviewerView full bio

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 30 Jun 2028
1 Jul 2025 | Latest version
25 May 2011 | Originally published
Authored by:
Dr Laurence Knott

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.