Macular disorders
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 19 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Macular degeneration article more useful, or one of our other health articles.
In this article:
Continue reading below
What is the macula?
The macula is the central region of the retina situated at the posterior pole of the eye, between the superior and inferior temporal arteries, 3 mm lateral (temporal) to the optic disc. It is the part of the retina which produces central vision, for seeing those things which we try to focus on closely, for detecting detail, for reading and close work - for most people the key normal, functional vision.
The macula is 5.5 mm in diameter and contains within it the 1.5 mm diameter fovea and, within that, the foveola, a 0.35 mm area that houses the highest concentration of cone photoreceptors in the retina (to the exclusion of rods) and is concerned with enabling maximal, central visual acuity. There are no vessels overlying the foveola, which is entirely supplied by the underlying capillaries of the choroid.
Diagram detailing the macula
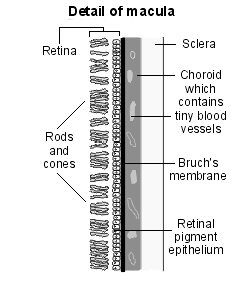
Evaluation of the macula
Back to contentsSymptoms associated with macular dysfunction
Impairment of central vision. This may be characterised as something appearing to obstruct the central vision or as a blurred patch.
Metamorphopsia. This describes a distortion of images - notably of straight lines ('If you look at the window, do all the sides of the frame look straight?').
Distortion of image size occurs uncommonly. Objects may appear bigger (macropsia) or smaller (micropsia). This may in turn give rise to diplopia, as there is a discrepancy between the image perceived in the healthy eye and in the diseased eye.
Continue reading below
Assessment of macular function
Back to contentsVisual acuity
The most important test is the assessment of visual acuity. Note distant acuity using a Snellen chart, making sure that you have identified any past history of previous visual acuity problem (eg, amblyopia). If you have access to a near vision booklet, assess the near vision too. Ask the patient to hold the booklet at about 30 cm (about an arm's length) and, using their usual reading glasses, read the short passages, one eye at a time.
Amsler grid
There are several forms of Amsler grids but the most common one is a 10 cm by 10 cm grid printed on a plain white paper.1 It is evenly divided into 0.5 cm by 0.5 cm squares and has a small black dot at its centre. Ask the patient to cover one eye and hold the grid about 30 cm away from them, preferably resting on a surface so that they can draw on the paper. The steps to using it are:
Ask: 'What is at the centre of the paper?' (failure to see the dot suggests a central scotoma).
(If there is no central scotoma): 'I want you to focus on the central dot and tell me whether you can see all four corners of the big box out of the corner of your eye.'
'Still focusing on the central dot: Are any of the small boxes missing? Where? Can you shade out the area where they are missing?'
'Finally, whilst still focusing on the central dot: Do any of the lines appear distorted? Where? Can you draw over those lines that are not straight?'
Rest and then test the fellow eye.
Abnormalities of any of the answers suggest macular pathology. Patients can use the grid at home and test themselves (remind them to do one eye at a time).1
Examination of the macula
Ophthalmoscopy - the macula is visible as a dark circular patch between the vascular arches, the fovea being about 1 disc diameter lateral to the disc itself. The foveola is usually seen as a bright pinpoint yellow reflex at the centre of the macula. If you ask the patient to look directly at the light, the macula is then right in front of your line of vision. This may be uncomfortable for the patient, and it is best left until the end of the fundoscopic examination.
Slit-lamp biomicroscopy - this provides a good view of the macula and the underlying retinal pigment epithelium.
Fluorescein angiography - this involves observation of the passage of fluorescein dye through the retinal and choroidal circulation. Fluorescein is injected peripherally and, some seconds later, a series of photographs is taken of the fundus through dilated pupils. Both eyes are photographed for comparison. This enables the identification of abnormal blood vessels, loss of blood vessels, blockages and leaks. Most patients experience a temporary discolouration of the skin (yellow tinge) and urine (orange tinge) and some may experience nausea and vomiting. More serious (but uncommon) adverse effects include allergy and anaphylaxis. For this reason patients are asked to wait in clinic for some time after the angiography.
Indocyanine green angiography - this follows the principle of fluorescein angiography but enables better visualisation of the choroidal circulation. It may be performed at the same time as fluorescein angiography, the two tests being run simultaneously. Adverse effects are less common and include sneezing, pruritus, nausea and vomiting. Syncope, backache and local skin necrosis may occasionally occur. Indocyanine green is contra-indicated in patients with iodine allergy or in those who are pregnant.
Optical coherence tomography (OCT) - this provides a cross-sectional view of the retina, including the macula. It generates a 3-D image of the macula and optic disc and is invaluable in assisting the diagnosis of macular (and glaucomatous) pathology. It is quick and painless, and is increasingly available in most eye departments.
Macular disorders
Back to contentsA range of problems can affect the macula. The most common of these in the UK is age-related macular degeneration. Other common macular conditions are macular oedema, macular holes and Förster-Fuchs retinal spot (myopic maculopathy).
Other diseases that can affect the retina include (see links for further details):
There are other less common problems that can affect the macula:
Central serous chorioretinopathy (CSCR)2
Description - also known as central serous retinopathy (CSR), this condition is characterised by fluid leakage at the level of the retinal pigment epithelium (which lies just beneath the photoreceptors) in the macular area. It is usually idiopathic but may be associated with systemic hypertension, systemic and inhaled steroids, and pregnancy. There is a 5% prevalence in Cushing's syndrome. There are also interesting psychological associations typically described: patients are more likely to:
Have type A personalities.
Have conversional neuroses.
Be using psychopharmacological medications.
Stress or a disturbing psychological event precedes the onset of CSCR in the majority of patients. However, more recently, there has been some debate over these apparent psychological links.Presentation - the patient (typically aged between 20 and 45 years, and eight times more likely to be male) complains of acute blurring of the vision which may range from a mild central disturbance to a severe drop (eg, 6/60). Colours may appear washed out and there can be a central scotoma. Symptoms are usually unilateral. Metamorphopsia and image size distortion are common. Examination reveals reduced visual acuity and, very occasionally, a relative afferent pupillary defect (RAPD) - although presence of this prompts the thought of optic neuritis. Examination of the fundus reveals a well-demarcated, localised serous detachment of the neurosensory retina from the retinal pigment epithelium in the macular region.
Management - mainstays of treatment are observation, photodynamic therapy (PDT) and laser procedures. Observation is feasible due to possible spontaneous recovery in most acute CSCR cases. In general, PDT and laser procedures, such as conventional laser photocoagulation, are used to provide more rapid visual recovery, when disease does not improve spontaneously during observation.
Outcome - this tends to be excellent with spontaneous and full recovery usually occurring between 1 and 6 months. Occasionally, the course is prolonged (6-12 months), and may become chronic (>12 months). Only the latter is associated with permanent impairment of visual ability and, in these patients, the history has often been atypical and there may be bilateral pathology. The prognosis tends to be highly dependent on presenting visual acuity, with initial visual acuities of <6/9 usually recovering, on average, two to three Snellen lines over the next few years.2
Macular epiretinal membrane3
Description - this is a phenomenon in which neural support cells grow over the macula to form a membrane (epiretinal gliosis). This may be idiopathic or secondary to retinal surgical procedures, retinal vascular disease, intraocular inflammation or trauma. The membrane may be thin (cellophane maculopathy) or thickened and contracted (macular pucker).
Presentation - patients, who are usually middle-aged to elderly, may be asymptomatic or present with a decrease in visual acuity (mild in cellophane maculopathy (eg, 6/9), more in macular pucker (eg, 6/12 or worse)). Examination reveals a glistening membrane over the macula: there may also be retinal wrinkles radiating out from the macula.
Management - conservative management is supported by the fact that most epiretinal membranes are asymptomatic and do not progress, and some even regress. Aggressive management has been proposed for select cases, based on the fact that patients with better pre-operative visual acuity tend to have better postoperative results.
Outcome - visual acuity may not necessarily be improved but any image distortion may be helped by surgery. Poor prognostic features include long duration of symptoms prior to surgery, underlying macular co-pathology and low pre-operative visual acuity.
Choroidal folds4
Description - these arise as a consequence of choroidal congestion, scleral folding or contraction of one of the neuroretinal membranes. The condition is usually idiopathic but can also arise due to orbital disease (eg, thyroid eye disease), choroidal tumours (eg, melanomas), ocular hypotony (eg, following certain kinds of surgery) and a number of other reasons.
Presentation - patients will predominantly complain of metamorphopsia but, depending on the underlying cause and the extent of the folds, may also complain of a decreased visual acuity. Parallel grooves (like wrinkled cling film) can be seen stretching across the retina.
Management - this depends on the underlying cause. For example, traumatic folds are sometimes treated with injected triamcinolone.
Outcome - this depends on the underlying cause.
Best's disease (vitelliform macular dystrophy)5
Description - this rare autosomal dominant condition belongs to a group of hereditary fundus dystrophies known as 'inherited pattern dystrophies'.
Presentation - asymptomatic or decreased vision; this may be in childhood, or in early adulthood, or it may not be detected until later on in life when there is another reason to carry out a fundal examination. It is characterised by well-defined, round yellow lesions which are often compared to an egg yolk (later followed by a scrambled egg appearance, and then atrophy). It is a bilateral condition.
Management - there is no effective treatment but laser treatment is sometimes used to address complications such as neovascular membrane formation.
Outcome - this depends on the type but ranges from excellent (adult vitelliform macular dystrophy) to poor (juvenile Best's disease: there is progressive macular scarring from the fifth decade of life which can eventually lead to legal severe sight impairment).
Other macular dystrophies
There are a number of other recognised macular dystrophies in addition to Best's disease. Generally, they tend to cause loss of photoreceptors with accumulation of debris around the retinal pigment epithelium. There is currently no effective treatment for these diseases and the emphasis is on diagnosis and appropriate counselling with supportive care as required. Conditions that fall into this category include:
Stargardt's disease, or fundus flavimaculatus (two clinical presentations of the same disease)5 .
Adult vitelliform degeneration.
Familial drusen.
Dominant cystoid macular oedema.
Cone degenerations.
Continue reading below
Other rare conditions affecting the macula
Back to contentsIdiopathic polypoidal choroidal vasculopathy6
Description - abnormality believed to originate in the inner choroid. The exact pathogenesis remains unclear; however, the pathologies involve dilated thin-walled aneurysmal vessels in the choroid bleeding (giving rise to the term posterior uveal bleeding syndrome), particularly around the macular region.
Presentation - the patient (more often non-white) presents with sudden, painless, unilateral visual impairment. Retinal pigment epithelial or full-thickness retinal detachments may be observed on examination ± vitreous haemorrhage.
Management - some patients benefit from laser treatment.
Outcome - this is usually good with spontaneous resolution of the haemorrhage.
Maculopathy in optic disc pit7
Description - an optic disc pit is a rare congenital abnormality associated with a visual field defect. Occasionally, the macula becomes involved in this condition: it accumulates subretinal fluid (possibly from the subarachnoid space, possibly from the vitreous) and this may eventually be associated with a retinal pigment epithelial detachment.
Presentation - these patients present at puberty with a progressive, painless visual impairment. The optic disc pit itself may be asymptomatic and so this may be the first time this diagnosis is made.
Management - there are no clear guidelines on the management, and numerous techniques have been described, including laser photocoagulation, intravitreal gas injection, macular buckling and pars plana vitrectomy with many different modifications.
Outcome - this depends on the degree of macular involvement and the need for treatment.
Solar maculopathy8
Description - the harmful effects of sunlight caused by looking directly into the sun include thermal and photochemical damage in the retinal pigment epithelium and photoreceptors. The histological damage occurs at the level of the retinal pigment epithelium melanosomes and photoreceptor external segment.
Presentation - 3-7 days after exposure the patient complains of impairment of central vision, with or without metamorphopsia and with or without a central scotoma. Examination reveals a variously impaired visual acuity and there may be small unilateral or bilateral yellow spots around the macula. About two weeks later, these are surrounded by mottling.
Diagnosis - can be confirmed by optical coherence tomography
Management - observation.
Outcome - the outcome is usually good. Visual acuity starts to improve 1 to 2 weeks after sun exposure, with improvement continuing to reach a maximum recovery at 6 months, and then reaches a plateau level, with variable but usually relatively mild residual symptoms.
Macular conditions arising in association with systemic problems
Back to contentsAngioid streaks9
Description - these arise as a result of degenerative structural abnormalities in the layers of the neuroretina and manifest themselves as crack-like dehiscences associated with calcium deposition. These structural changes arise as a result of systemic disease in 50% of cases. Such diseases include pseudoxanthoma elasticum, Ehlers-Danlos syndrome, rarely Paget's disease of bone and some haemoglobinopathies (eg, sickle cell disease).
Presentation - initially asymptomatic or slight decrease in vision but, over time, this becomes quite marked. There will be bilateral linear brown lesions on fundoscopy which intercommunicate in a ring-like fashion and, eventually, the optic nerve will be affected too. There are often associated fundal findings.
Management - initially observation alone, although some patients benefit from laser photocoagulation and surgery (removal of the neovascular membrane).
Outcome - ultimately, this is poor, as the streaks creep over the fovea, cause exudative leaks in the macula, and associated haemorrhage. This occurs in over 85% of patients.
Cancer-related maculopathy
Description - rarely maculopathy is a systemic manifestation of cancer elsewhere in the body: it tends to occur in association with small cell lung cancer and occasionally other epithelial tumours. It may be the first manifestation of these tumours. It is characterised by an autoimmune photoreceptor destruction but there are no ocular metastases.
Presentation - gradual onset of dimming of the vision and associated shimmering photopsia (flashes of light). There may be bizarre visual images seen and night blindness. The symptoms are bilateral (but may be asymmetrical) and progressive with little to see on fundus examination.
Management - there may be a response to systemic steroids.
Outcome - the prognosis is poor, both visually and systemically.
Drug-induced maculopathies10
A number of maculopathies can manifest themselves as a result of systemic drug intake. The optimal management for these conditions is discontinuation of the medication where possible and observation in the ophthalmology outpatient clinic. Many resolve in time.
Drug-induced maculopathies include:
Hydroxychloroquine: changes in the photoreceptor layer and the retinal pigment epithelium, usually in the parafoveal and perifoveal regions; optical coherence tomography shows progressive thinning of the inner retina in patients without diagnosed retinal toxicity; changes usually noted after years of using the drug.
Pentosan polysulfate sodium: paracentral hyperpigmentation in the retinal pigment epithelium layer with surrounding vitelliform deposits; optical coherence tomography angiography shows choriocapillaris flow voids; changes usually noted after years of using the drug.
Intravitreal brolucizumab: intraocular inflammation and occlusive retinal vasculitis presenting around 25–30 days post-injection.
MEK inhibitors (cobimetinib): transient and self-limiting multifocal serous retinal detachments involving the central and peripheral retina.
Ulixertinib: cystoid macular oedema, subretinal fluid, and subretinal deposits between the retinal pigment epithelium and interdigitation zone.
Fibroblast growth factor receptor inhibitors (erdafitinib): central serous retinal detachment, usually asymptomatic or very mild symptoms.
Subconjunctival gentamicin: macular whitening and retinal haemorrhages within the immediate post-op period.
Intraocular moxifloxacin: toxic posterior segment syndrome; decreased visual acuity, loss of the subfoveal ellipsoid zone on optical coherence tomography, reduction of full-field retinal responses and negative electroretinogram.
Intracameral vancomycin: haemorrhagic occlusive retinal vasculitis (vascular sheathing, diffuse retinal haemorrhages, inner retinal ischaemia, and oedema).
Tamoxifen: crystalline deposits, pseudocystic foveal cavitations, thinner choroid, and total retinal thickness.
Ritonair: bilateral parafoveal retinal pigment epithelium mottling, loss of outer retinal and choriocapillaris layers, cone-rod dysfunction.
Efavirenz: bilateral central and paracentral visual field defects, retinal pigment epithelium mottling, loss of the outer retinal layers, reduced macular responses on multifocal electroretinogram.
Alkyl nitrites: a yellow spot at the fovea; optical coherence tomography shows disruption of the foveal photoreceptors.
Chloroquine and hydroxychloroquine both have the potential for retinotoxicity and may also result in corneal deposits. The retinopathy is related to the total cumulative dose and is more marked with chloroquine. Patients present with decreased vision (which may be severe in end-stage chloroquine maculopathy - less than 6/60 - and characterised by a 'bull's-eye' macular lesion: a well-defined red centre surrounded by a mottled yellow periphery), abnormal colour vision and difficulty in adjusting to darkness (nyctalopia). There may also be a scotoma.
The Royal College of Ophthalmologists recommends that:11
Visual acuity be recorded prior to starting these drugs.
All individuals who have taken hydroxychloroquine for greater than 5 years should receive annual monitoring for retinopathy.
All individuals who have taken chloroquine for greater than 1 year should receive annual monitoring for retinopathy.
All individuals taking hydroxychloroquine who have additional risk factors for retinal toxicity may be monitored annually after the initiation of therapy. This is to be decided by the prescribing physician should additional risk factors be present. Additional risk factors: concomitant tamoxifen use, impaired renal function (eGFR less than 60 ml/min/1.73 m2), dose of hydroxychloroquine greater than 5 mg/kg/day.
Other potential causes of drug-induced maculopathy include:
Vigabatrin - in around a third of cases, a visual field defect develops which is largely asymptomatic but optic atrophy may occur. The visual field defects are generally static once established - they do not progress but do not resolve on drug withdrawal. The Royal College of Ophthalmologists recommends organising a baseline visual field test which needs to be repeated every six months for the first three years of treatment and then annually thereafter.
Phenothiazines - drugs used in the treatment of schizophrenia can cause pigmentary changes affecting the macula, characterised by brown clumping of pigment ± loss of retinal pigment epithelium. Patients on these medications may be asymptomatic or present with blurred vision, browning of the vision or difficulty in seeing at night. Current prescribing practice should not lead to retinopathy.
Toxic crystalline maculopathy - tamoxifen, canthaxanthin and methoxyflurane occasionally cause toxic retinopathy when taken in higher doses. This tends to present as a decrease in visual acuity. On examination, tiny, glistening deposits appear arranged in a ring around the macula. The condition may lead to a mild drop in visual acuity but current prescribing practices rarely lead to retinopathy.
Deferrioxamine - this may lead to a decrease in visual acuity associated with nyctalopia (night blindness). It can occur at any dosage level and has even been reported after a single dose.
Antimicrobials - didanosine (used in the treatment of HIV) can cause retinopathy in children, and clofazimine (anti-mycobacterial) can cause an extensive bull's-eye maculopathy with pigment deposit and atrophy.
Cocaine - ocular complications of topical (intranasal) cocaine abuse are rare but have been described. This is characterised by impaired colour vision on substance withdrawal.
Valsalva maculopathy12
Description - intraocular bleeding can occasionally occur as a result of a sudden, severe increase in intrathoracic or intra-abdominal pressure.
Presentation - the patient may complain of sudden distortion of central vision in one or both eyes and fundoscopy reveals a small, isolated macular haemorrhage in one or both eyes.
Management - mainly conservative.
Outcome - excellent.
Dr Mary Lowth is an author or the original author of this leaflet.
Further reading and references
- (2013)
- Macular degeneration - age-related; NICE CKS, August 2022 (UK access only)
- Amsler Grid: Test for Macular Degeneration or Other Vision Problems; All About Vision
- Wong KH, Lau KP, Chhablani J, et al; Central serous chorioretinopathy: what we have learnt so far. Acta Ophthalmol. 2016 Jun;94(4):321-5. doi: 10.1111/aos.12779. Epub 2015 Jul 1.
- Stevenson W, Prospero Ponce CM, Agarwal DR, et al; Epiretinal membrane: optical coherence tomography-based diagnosis and classification. Clin Ophthalmol. 2016 Mar 29;10:527-34. doi: 10.2147/OPTH.S97722. eCollection 2016.
- Jacobsen AG, Toft PB, Prause JU, et al; Long term follow-up of persistent choroidal folds and hyperopic shift after complete removal of a retrobulbar mass. BMC Res Notes. 2015 Nov 14;8:678. doi: 10.1186/s13104-015-1610-1.
- Altschwager P, Ambrosio L, Swanson EA, et al; Juvenile Macular Degenerations. Semin Pediatr Neurol. 2017 May;24(2):104-109. doi: 10.1016/j.spen.2017.05.005. Epub 2017 May 23.
- Bhoomibunchoo C, Yospaiboon Y, Thoongsuwan S, et al; Idiopathic polypoidal choroidal vasculopathy in Thai patients with clinical and angiographic choroidal neovascularization. Clin Ophthalmol. 2017 Feb 9;11:317-322. doi: 10.2147/OPTH.S126226. eCollection 2017.
- Moisseiev E, Moisseiev J, Loewenstein A; Optic disc pit maculopathy: when and how to treat? A review of the pathogenesis and treatment options. Int J Retina Vitreous. 2015 Aug 7;1:13. doi: 10.1186/s40942-015-0013-8. eCollection 2015.
- Abdellah MM, Mostafa EM, Anber MA, et al; Solar maculopathy: prognosis over one year follow up. BMC Ophthalmol. 2019 Sep 18;19(1):201. doi: 10.1186/s12886-019-1199-6.
- Mansour AM; Progressive symmetric vertical macular wide angioid streak-like lacquer crack. Int Med Case Rep J. 2016 Apr 19;9:95-9. doi: 10.2147/IMCRJ.S103068. eCollection 2016.
- Hsu ST, Ponugoti A, Deaner JD, et al; Update on Retinal Drug Toxicities. Curr Ophthalmol Rep. 2021;9(4):168-177. doi: 10.1007/s40135-021-00277-x. Epub 2021 Dec 21.
- Yusuf IH, Foot B, Lotery AJ; The Royal College of Ophthalmologists recommendations on monitoring for hydroxychloroquine and chloroquine users in the United Kingdom (2020 revision): executive summary. Eye (Lond). 2021 Jun;35(6):1532-1537. doi: 10.1038/s41433-020-01380-2. Epub 2021 Jan 9.
- Mukherjee C, Kumar A, Mitra A; Valsalva maculopathy: To treat or not to treat. Oman J Ophthalmol. 2018 Jan-Apr;11(1):78-81. doi: 10.4103/ojo.OJO_91_2016.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Sept 2028
19 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free