Otitis media with effusion
Glue Ear
Peer reviewed by Dr Rachel Hudson, MRCGPLast updated by Dr Surangi Mendis, MRCGPLast updated 20 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Glue ear article more useful, or one of our other health articles.
In this article:
Continue reading below
What is otitis media with effusion?
Otitis media with effusion (OME), also called glue ear, is characterised by a collection of fluid in the middle-ear cleft. There is chronic inflammation without signs of acute inflammation.
OME is the most common cause of hearing impairment (and the most common reason for elective surgery) in childhood, where it usually follows an episode of acute otitis media (AOM). It is uncommon in adults, in whom Eustachian tube dysfunction is the predominant cause and suspicious aetiologies should be considered.1
Ear diagram and glue ear
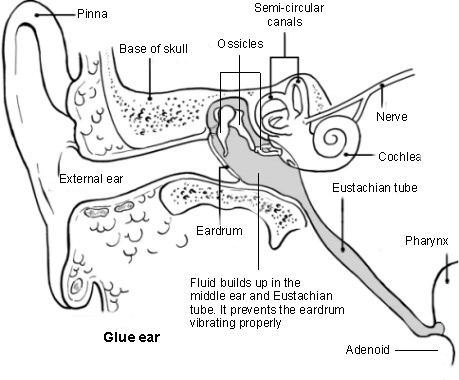
Most cases of otitis media with effusion resolve spontaneously. However, persistent hearing loss can occur. in affected ears the average hearing loss is mild but it can be moderately severe, causing significant functional listening difficulty in a small number of cases. Surgery (grommet insertion, usually performed with adenoidectomy) may be offered in persistent and symptomatic cases occurring in childhood.2 Temporary hearing aids can also be used for those wishing to avoid surgical intervention.
How common is otitis media with effusion? (Epidemiology)1
Back to contentsOtitis media with effusion is the most common cause of acquired hearing loss in childhood.
It is more common between the ages of 6 months to 4 years.
More than 50% of children will experience otitis media with effusion in the first year of life.
1 in 8 primary school children (5-6 years) have fluid in one, or both ears at any one time.
In children with Down's syndrome, cleft palate or other craniofacial anomalies, the prevalence is 60-85%.
It is most common in the winter months.
It is much less common in adults.3
Risk factors (children)1
The winter season.
A history of recurrent AOM or frequent upper respiratory tract infections.
Impaired Eustachian tube function associated with cleft palate.
Down's syndrome (increased susceptibility to infection due to impaired immunity and craniofacial malformation).
Primary ciliary dyskinesia.
Adenoidal infection or hypertrophy.
Allergies and atopic tendencies; asthma, eczema, urticaria.
Frequent upper respiratory tract infection.
Daycare attendance.
Having older siblings.
Lower parental socio-economic group.
Parents who smoke.
One study found a link between gastro-oesophageal reflux in children and OME: it is postulated that reflux increases the level of inflammatory cytokines present in the nasopharynx and middle ear.4
Risk factors (adults)3
Middle ear fluid in adults needs to be viewed with suspicion, particularly if unilateral. In one series of adult cases with serous otitis media with effusion over a 10-year period, 59 patients had unilateral effusion and 26 cases were bilateral. A nasopharyngeal mass was documented in 69%. Examination under anaesthesia and nasopharyngeal biopsy was undertaken in all of those noted to have a mass and malignancy was found in 4.7%.
Acute otitis media is uncommon in adults and is thus not a common precursor to otitis media with effusion.
Eustachian tube dysfunction (ETD) is the main aetiological factor in adults. Causes of ETD include:
Infection/inflammation:
Severe nasopharyngeal infection (eg, sinusitis) inflames the Eustachian tube openings, resulting in ETD.
Severe or chronic allergy may produce the same effect.
Anatomical blockage:
Severe nasal septal deviation with an obstructed airway.
The presence of tonsils and adenoids with obstruction to Eustachian tubes.
A nasopharyngeal tumour near Eustachian tube openings.
Radiation to the head and neck following cancer treatments.
Radical head and neck surgery, on maxillary sinuses and/or palate, that transects the Eustachian tube.
Secondary inflammation from allergic rhinitis.
Frequent upper respiratory infection. Some viruses may directly damage the Eustachian tube lining, decreasing ciliary clearance.
Trauma (usually barotrauma - eg, after a dive or flight).
Continue reading below
Spectrum of otitis media5
Back to contentsOtitis media (OM) is an umbrella term for a group of complex infective and inflammatory conditions affecting the middle ear. All OM involves pathology of the middle ear and middle ear mucosa. OM is a leading cause of healthcare visits worldwide and its complications are important causes of preventable hearing loss, particularly in the developing world.6
There are various subtypes of OM. These include AOM, OME, chronic suppurative otitis media (CSOM), mastoiditis and cholesteatoma. They are generally described as discrete diseases but in reality there is a great degree of overlap between the different types. OM can be seen as a continuum/spectrum of diseases:
Acute otitis media is acute inflammation of the middle ear, typically characterised by severe otalgia and possibly fever. A subtype of AOM is acute suppurative OM, characterised by the presence of pus in the middle ear. In around 5% the eardrum perforates.
Otitis media with effusion is a chronic inflammatory condition without acute inflammation, which often follows a slowly resolving AOM. There is an effusion of glue-like fluid behind an intact tympanic membrane and signs and symptoms of acute inflammation are absent.
CSOM is long-standing suppurative middle ear inflammation, usually with a persistently perforated tympanic membrane.
Mastoiditis is acute inflammation of the mastoid periosteum and air cells, occurring when AOM infection spreads out from the middle ear.
Cholesteatoma occurs when keratinising squamous epithelium (skin) is present in the middle ear as a result of tympanic membrane retraction.
Otitis media with effusion symptoms in children1
Back to contentsHistory
OME may be detected by the newborn hearing screening test.
Hearing loss is the usual presenting symptom, although this is easily missed in very young children. Hearing loss in children may present with:
Mishearing, difficulty with communication in a group, listening to the TV at excessively high volumes or needing instructions to be repeated.
Lack of concentration, withdrawal. This may present as behavioural difficulties.
Impaired speech and language development.
Impaired school progress.
Mild intermittent ear pain with fullness or popping.
There may be a history of recurrent ear infection, upper respiratory tract infections or nasal obstruction.
Occasionally balance problems may be a feature.
Assess the severity of the hearing loss and impact on the child's life by asking about:
Fluctuations in hearing.
Lack of concentration or attention, or being socially withdrawn.
Changes in behaviour.
Listening skills and progress at school or nursery.
Speech or language development.
Balance problems and clumsiness.
Examination findings
Examine the ears with an otoscope:
Opacification of the drum (other than due to scarring).
There are usually no signs of inflammation or discharge on examination.
Loss of the light reflex, or a more diffused light reflex.
Indrawn, retracted, or concave drum.
Decreased or absent mobility of the drum.
Presence of bubbles or fluid level.
Yellow or amber colour change to the drum.
Fullness or bulging of the drum, although this is not typical.
Examine the nose and throat to exclude predisposing factors.
Tympanometry provides quantitative information about fluid in the ear but is generally considered a specialist investigation.
Continue reading below
Otitis media with effusion symptoms in adults
Back to contentsAdult otitis media with effusion is more often unilateral than in children, which may reflect the underlying causes.
Typical symptoms include:
Otitis media with effusion in adults usually presents with hearing loss.
A feeling of aural fullness.
Crackling or popping tinnitus.
A foreign body sensation in the external auditory canal.
Mild, diffuse aural pain.
Complaints of acute ear pain (rare).
A vague sense of unsteadiness without true vertigo may be seen.
Investigations in children1
Back to contentsChildren with persistent symptoms or signs should be referred for a hearing assessment. Referral should be to a centre which holds specific expertise in paediatric audiology.
Not all cases require referral. Spontaneous resolution often occurs, so it's worth observing for up to three months to see whether the symptoms and signs resolve ('active observation').7 50% of children with 20 dB hearing loss will recover in three months without treatment.
Hearing assessment
Hearing tests of children with persistent otitis media with effusion typically show a mild conductive hearing loss involving one or both ears. In some cases, no hearing loss is seen by the time of the assessment, or moderate loss may be detected which is more likely to require intervention, particularly if the loss is bilateral.
School entry hearing screening in the UK
Routine screening for hearing loss when children start primary school began in the 1950s, before the introduction of the current newborn hearing screening programme. The school age hearing screen continues in many, but not all, parts of the country.
A UK National Screening Committee review in 2019 concluded that uncertainties remained relating to:
How many children starting school with temporary hearing loss would be identified by a national programme.
The accuracy of screening tests used to detect permanent hearing loss in children starting school.
The advantage of screening children at school entry age.
It was not clear whether the best course of action was to discontinue or extend school age screening. They recommend that screening should continue only where it is already implemented while further research is undertaken to evaluate its effectiveness.8
Where school entry screening remains in place, it is worth noting that the assessment does not provide a quantitative level of hearing loss - children identified by the screening process are referred by the screening service to a paediatric audiology centre for formal hearing assessment.
Investigations in adults2
Back to contentsOtitis media with effusion has a lower prevalence in adults and is frequently associated with other underlying diagnoses. Unilateral OME in an adult is a suspicious finding.
Paranasal sinus disease is the main underlying cause of OME in adults, accounting for two thirds of cases in one series. However, other causes include head and neck tumours.
Adults with otitis media with effusion should therefore be fully evaluated, including use of flexible nasal endoscopy, for underlying conditions.
Nasopharyngeal tumours are relatively more common in patients of Southern Chinese ethnicity. One study in Taiwan suggested that all adults with OME in whom a cause is not clearly understood should have full nasopharyngeal evaluation, including biopsy.9 For this reason, NICE guidance suggests that adults of Chinese or South-East Asian family origin with hearing loss and a middle ear effusion not associated with an upper respiratory tract infection should be referred to ENT via a 2 week wait suspected cancer pathway.10
Otitis media with effusion treatment and management1 7
Back to contentsOME management in children
Advice
Give written information about OME to parents of affected children and reassure parents that:
OME is a self-limiting illness and 90% of children will have complete resolution within one year, although recurrence is common.
There is no proven benefit from treatment with any medication or alternative therapy.
Parental smoking increases the risk of OME.
Advise parents of children with hearing loss that hearing tactics can be used to facilitate communication. Parents and caregivers can assist by:
Facing their child when speaking to them.
Slowing their speech.
Keeping speech clear.
Increasing speech volume slightly.
Turning off competing stimuli such as radio or TV.
Encouraging daily reading, which helps language development.
Hearing aid use
NICE recommends hearing aids for children with bilateral OME and hearing loss where surgery is not acceptable or is contra-indicated or if aiding is in line with parental or child preference.
Medical management (eg, antibiotics, topical or systemic antihistamines or decongestants) is not recommended.
High-quality evidence of multiple short- and long-term outcomes repeatedly and unequivocally demonstrated no benefit for use of antihistamines and decongestants over placebo for treating OME. Routine use of antibiotics is also not recommended. Additionally, side-effects and harms may occur with use of these medications.
The treatment of adults with uncomplicated OME is generally extrapolated from that of children. If there is an underlying cause then this should be treated appropriately. There is a lack of clear evidence on the treatment of uncomplicated OME in adults.
Referral
Most children who present with OME can be safely managed with active observation.
Earlier referral may be considered for children with significant hearing difficulties, particularly if there are developmental, social or educational difficulties, or if there is pre-existing hearing impairment.
Active observation is not appropriate for children who have significant disability or who have associated high-risk conditions - eg, Down's syndrome, cleft palate. These children should be referred to paediatric audiology services and would typically remain under long-term surveillance to ensure hearing loss is detected early, should it develop.
Active observation7
The use of surgical treatment for OME has fallen dramatically in recent years with the recognition that many cases resolve with active observation.
Autoinflation13
This is a technique used to induce a Valsalva manoeuvre. NICE considers that evidence on the safety and efficacy of balloon dilation for Eustachian tube dysfunction is adequate to support the use of this procedure, provided that standard arrangements are in place for clinical governance, consent and audit.
There is a number of devices available for purchase. The Otovent® device is available over the counter and on NHS prescription. A balloon is inflated by blowing into it from one nostril, while sealing the other nostril with a finger. This action results in an increase in intranasal pressure and opening of the Eustachian tube (ie a Valsalva manoeuvre).
Surgery 1 7
NICE recommends that children who most benefit from surgery are those:
With persistent bilateral OME and persistent hearing loss lasting three or more months.
Children with better hearing, or only persistent unilateral hearing loss, but who have social, educational or developmental difficulties. They may exceptionally also benefit from surgical treatment.
Insertion of grommets - ventilation tubes 1 7
NICE concludes that insertion of grommets results in an improvement in hearing over a twelve-month period, which starts to tail off after six months. There is little evidence that language or speech development improves in the long term but significant short term in improvements in speech progression and overall development may be seen.
Tympanosclerosis frequently occurs after grommet insertion, although the long-term consequences of this are uncertain.
Infection after grommet insertion may occur. This can be managed with non-ototoxic topical antibiotic ear drops (eg, ciprofloxacin) for 5 to 7 days if otorrhoea occurs following grommet insertion. There is also a slightly increased incidence of chronic perforation.
Grommet insertion has traditionally been performed under general anaesthetic, although it is possible to perform the procedure under local anaesthetic. Topical anaesthetic is applied to the ear canal approximately 30 minutes prior to the procedure.
Adenoidectomy
When planning grommet insertion for management of OME, adjuvant adenoidectomy should be considered. There is evidence that adenoidectomy with or without unilateral or bilateral grommet insertion reduces the presence or persistence of OME and in turn, this may have beneficial effects on hearing. However, adenoidectomy may cause velopharyngeal insufficiency or nasal regurgitation in children with palate abnormalities and so adenoidectomy should be avoided in this cohort.
Complications of otitis media with effusion
Back to contentsOtitis media with effusion may adversely affect speech, language development, behaviour and education. However:
Evidence shows only a weak association between OME and long term delays in speech and language development. Most studies suggest that any adverse effect is temporary in the majority of children.1
Otitis media with effusion prevention
Back to contentsParents and carers should be advised to avoid exposing children to tobacco smoke. Passive smoking increases the risk of OME.
If a child is bottle fed, feeding should take place in an upright position.
Parents should avoid using a dummy where possible. When one is used, ideally discontinue use before 12 months of age.
Ensure the child's vaccinations are up to date. One study found that A (H1N1) pandemic influenza vaccine afforded a two- to nine-fold protection against OME.4
Prognosis1
Back to contentsOtitis media with effusion (OME) usually resolves spontaneously within three months.
Older children are more likely to resolve within this time: 22% at 1 year; 50% at 3 years; 70% at 5 years; 95% at 10 years.
Persistence is more likely when a larger number of contributory factors is present, eg:
Bilateral OME, winter months, and a personal or sibling history of acute recurrent otitis media.
Persistence for six months in a child younger than 2 years of age has been measured as varying from 25-60%.
It is not clear whether adult OME not associated with malignancy is the same disease as that which occurs in childhood or whether it is a different condition. The chronic form tends to persist longer than that seen in childhood, likely due to ongoing co-founding factors such as smoking, allergies and sinonasal disease. However, evidence suggests that adults with OME tend to have had a history of OME in childhood.3
Dr Mary Lowth is an author or the original author of this leaflet.
Further reading and references
- Otitis media with effusion; NICE CKS, June 2021 (UK access only)
- Atkinson H, Wallis S, Coatesworth AP; Otitis media with effusion. Postgrad Med. 2015 May;127(4):381-5. doi: 10.1080/00325481.2015.1028317.
- Mills R, Hathorn I; Aetiology and pathology of otitis media with effusion in adult life. J Laryngol Otol. 2016 May;130(5):418-24. doi: 10.1017/S0022215116000943. Epub 2016 Mar 15.
- Cuhaci Cakir B, Beyazova U, Kemaloglu YK, et al; Effectiveness of pandemic influenza A/H1N1 vaccine for prevention of otitis media in children. Eur J Pediatr. 2012 Nov;171(11):1667-71. doi: 10.1007/s00431-012-1797-2. Epub 2012 Sep 30.
- Qureishi A, Lee Y, Belfield K, Birchall JP, Daniel M; Update on otitis media – prevention and treatment. Infection and Drug Resistance. 2014;7:15-24. doi:10.2147/IDR.S39637.
- Monasta L, Ronfani L, Marchetti F, et al; Burden of disease caused by otitis media: systematic review and global estimates. PLoS One. 2012;7(4):e36226. Epub 2012 Apr 30.
- Otitis media with effusion in under 12s; NICE guideline (August 2023)
- Child screening programme Hearing (child); UK National Screening Committee, 2019
- Ho KY, Lee KW, Chai CY, et al; Early recognition of nasopharyngeal cancer in adults with only otitis media with effusion. J Otolaryngol Head Neck Surg. 2008 Jun;37(3):362-5.
- Hearing loss in adults: assessment and management; NICE Guideline (June 2018 - last updated October 2023)
- Browning GG, Rovers MM, Williamson I, et al; Grommets (ventilation tubes) for hearing loss associated with otitis media with effusion in children. Cochrane Database Syst Rev. 2010 Oct 6;(10):CD001801. doi: 10.1002/14651858.CD001801.pub3.
- Venekamp RP, Burton MJ, van Dongen TM, et al; Antibiotics for otitis media with effusion in children. Cochrane Database Syst Rev. 2016 Jun 12;(6):CD009163. doi: 10.1002/14651858.CD009163.pub3.
- Otovent nasal balloon for otitis media with effusion; NICE Advice (MIB59), March 2016
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Nov 2028
20 Nov 2023 | Latest version
Last updated by
Dr Surangi Mendis, MRCGP
Peer reviewed by
Dr Rachel Hudson, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free