Shingles
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Surangi Mendis, MRCGPLast updated 23 Jan 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Shingles article more useful, or one of our other health articles.
In this article:
Synonyms: herpes zoster and varicella zoster
Continue reading below
What is shingles?
Shingles is caused by the human herpesvirus-3 (HHV-3). Primary shingles infection usually occurs in childhood, producing chickenpox (varicella) although it can be subclinical.
After this, the virus lies dormant in the sensory nervous system in the geniculate, trigeminal or dorsal root ganglia. It may lie dormant for many years, kept in check by the immune system before reactivating, usually within a single dermatomal segment.
When this happens, the virus travels along the affected nerve over 3 to 4 days, causing perineural and intraneural inflammation along the way.
There isn't always a clear reason for a flare-up but associations include ageing (most patients are over 50 years old), immunosuppressive illness, or psychological or physical trauma. Reactivation of the virus is thought to be associated with immunosuppression as a result of a decline in cell-mediated immunity.
In immunocompetent patients, the most frequent site of reactivation is the thoracic nerves followed by the ophthalmic division of the trigeminal nerve (ophthalmic shingles), which can progress to involve all structures of the eye.
If the mucocutaneous division of the VII cranial nerve is involved, vesicular lesions in the ear, facial paralysis, associated hearing loss, sometimes occurring with tinnitus and vertigo, are known as Ramsay Hunt syndrome.1 Shingles may also affect the cervical, lumbar and sacral nerve roots.
How common is shingles? (Epidemiology)2
Back to contentsChickenpox is a very common childhood illness. At least 90% of adults raised in the UK are immune, having been exposed in childhood.3 All these people are at risk of developing shingles.
Shingles is thought to primarily affect older people but it can arise at any age, including in children. The incidence and severity of shingles increases with age. The annual incidence of shingles for those aged 70 to 79 years is estimated to be around 790 to 880 cases per 100,000 people in England and Wales. The lifetime risk is estimated at one in four.
Rarely, chickenpox can be acquired from a patient with active shingles; the lesions shed virus (transmission is by direct contact or droplet spread). However, shingles cannot be caught from contact with a person with chickenpox.
Shingles risk factors
Increasing age significantly increases the incidence, morbidity and mortality of shingles.
Incidence and risk are increased in the immunocompromised patient. Consider underlying immunodeficiency in those presenting with shingles affecting more than one dermatome.
HIV, Hodgkin's lymphoma and bone marrow transplantation all present a high risk.
Continue reading below
Shingles symptoms
Back to contentsShingles can be divided into the pre-eruptive phase, acute eruptive phase and chronic phase - postherpetic neuralgia (PHN).
Pre-eruptive phase
In the pre-eruptive phase there is no skin lesion to see but 80% of patients complain of burning, itching or paraesthesia in one dermatome.
This usually lasts for a day or two but it can be over a week before the characteristic eruption appears.
The patient may feel unwell with malaise, myalgia, headache and fever but these symptoms may abate as the eruption appears.
In the pre-eruptive phase the skin may be tender but there are no lesions to see. There may be lymphadenopathy.
It can be difficult to confidently make a diagnosis of shingles before the characteristic rash appears.
Eruptive phase
The eruptive phase occurs when the skin lesions appear. Most, but not all, adults have acute, neuritic pain in this phase. A few have severe pain without any eruption, called zoster sine herpete. Young adults and children are most likely to be free of pain.
Crust formation and drying occurs over 7 to 10 days and is followed by resolution at 14 to 21 days.
Patients are infectious (resulting infection is chickenpox) until the lesions have crusted over and dried.
In the eruptive phase the rash first appears as a patch of erythematous, swollen plaques with clusters of small vesicles. This eruption is virtually diagnostic of shingles. It may not affect the whole dermatome but it will not extend outside it. Hence, any rash that crosses the midline is not shingles.
More vesicles may erupt over the next 5 to 7 days. They form crusts that fall off by three weeks.
In elderly and immunocompromised patients, the eruptive phase is longer and more extensive. It occasionally results in haemorrhagic blisters, skin necrosis and secondary bacterial infections.
Shingles: herpes zoster abdominal rash
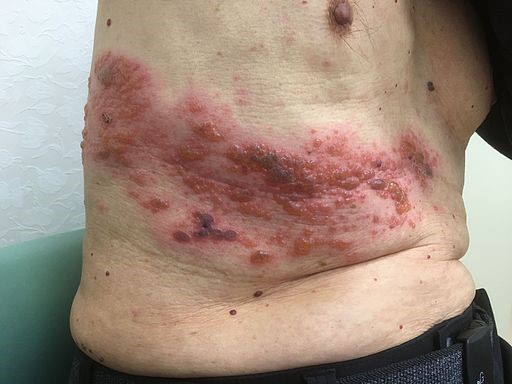
© melvil, CC BY-SA 4.0, via Wikimedia Commons
Chronic phase
Chronic phase, or PHN, is persistent or recurring pain lasting 30 days or more after the acute infection or after all lesions have crusted.
Variations
Back to contentsOphthalmic shingles4
Synonyms: herpes zoster ophthalmicus, ophthalmic herpes zoster
Shingles: herpes zoster affecting the forehead and eye
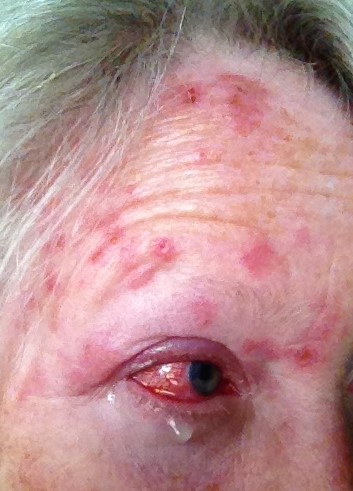
© Burntfingers, CC BY-SA 4.0, via Wikimedia Commons
Example of ophthalmic shingles
Ophthalmic shingles, involving the ophthalmic branch of the trigeminal nerve, accounts for 10-20% of cases of zoster. Ophthalmic herpes presents a danger to sight and the patient should see an ophthalmologist the same day. Antiviral therapy is mandatory for this condition at any age.
If the tip of the nose has a rash, the nasociliary branch of the trigeminal nerve is involved. This branch supplies the globe and so it is very likely that the eye will be affected (at least 75% of cases). This is called Hutchinson's sign; he described it in 1868. The eye can be seriously affected with little evidence of a shingles rash.
Acute lesions of the orbit or globe develop within three weeks of the onset of the rash. They may resolve swiftly or linger and recur over years.
Patients may have a red eye, decreased visual acuity, epiphora, photophobia and forehead tenderness.
Other problems affect various parts of the eye:5
Lids - bilateral eyelid oedema can develop, as well as blepharitis and ptosis.
Conjunctiva - giving rise to a follicular conjunctivitis.
Episclera and sclera - resulting in inflammation (episcleritis and scleritis).
Cornea - keratitis; multiple features may occur - eg, multiple small epithelial dendrites (seen after instilling fluorescein), stromal and neurotrophic keratitis, raised mucous plaques and so on. This is one of the sites where significant visual loss can occur.
Anterior eye - uveitis, paralysis ± atrophy of the iris and secondary glaucoma (about 10% of cases).
Posterior eye - retinitis, choroiditis and optic neuritis.
Nerve damage can include oculomotor palsies and neuralgia.
Tissue scarring can include lid deformities, neuralgia and lipid keratopathy.
Ramsay Hunt syndrome
See the separate Herpes Zoster Oticus (Ramsay Hunt Syndrome) article.
Continue reading below
Shingles differential diagnosis
Back to contentsBefore the rash appears, the pain may be thought to originate from under the affected dermatome and so it must be considered as a possible cause of chest or abdominal pain.
Cluster headaches or migraine - consider in the prodromal phase.
Ramsay Hunt syndrome may present as Bell's palsy before the rash appears.
The rash, especially if present without pain, may be mistaken for atopic eczema, eczema herpeticum, contact dermatitis, herpes simplex or impetigo. Diagnosis of eczema/dermatitis may lead to this viral infection being treated with steroid cream.
Consider the differentials of the acute red eye where there is no rash (eg, conjunctivitis, corneal abrasion, keratitis).
If you strongly suspect ophthalmic shingles, look for a rash or evidence of a previous rash, such as pigmentary changes along the hairline, or consider zoster sine herpete.
Investigation
Back to contentsShingles diagnosis is usually clinical, based on typical lesions in the distribution of a single dermatome. Various techniques to detect the virus or antibodies may be possible after consultation with a microbiologist.
Scraping for smears and cultures are usually negative, as the viruses are difficult to recover.
A direct immunofluorescence assay can be used; it is more sensitive than viral culture and can differentiate herpes simplex viral infections from varicella-zoster virus (VZV) infections.
Tests for varicella-zoster virus include the following:
Molecular biology tests based on in vitro nucleic acid amplification (PCR tests). These are currently considered the most reliable. Nested PCR test has high sensitivity but is susceptible to contamination leading to false-positive results. Real-time PCR tests are rapid, easy to perform, as sensitive as nested PCR, have a lower risk of contamination, and also have more sensitivity than viral cultures.
The Tzanck smear of vesicular fluid. This shows multinucleated giant cells. It has lower sensitivity and specificity than direct fluorescent antibody (DFA) or polymerase chain reaction (PCR).
Varicella-zoster virus-specific IgM antibody can be detected in blood during the active infection of chickenpox or shingles but not when the virus is dormant.
Direct fluorescent antibody testing of vesicular fluid or corneal fluid can be done when there is eye involvement.
PCR testing of vesicular fluid, a corneal lesion, or blood in a case with eye involvement or disseminated infection.
Where the presentation is atypical (eg, severe disease or a rash extending beyond one dermatome), possible immunodeficiency should be considered.
Shingles treatment6 7
Back to contentsGeneral
The shingles rash should be kept clean and dry to avoid secondary bacterial infection. Adhesive dressings should be avoided. If the rash can be covered, or if the lesions have all crusted, there is no need to avoid school or work.
If the rash is weeping and not in a covered part of skin, however, the person should not attend school or work.
Topical therapy
Topical antiviral treatment is not recommended. Topical antibiotic treatment may be indicated for secondary bacterial infection.
Oral antiviral therapy
Oral aciclovir has been shown to shorten the duration of shingles signs and symptoms and may reduce the incidence and severity of complications from ophthalmic shingles.
However, Cochrane reviews have found no evidence that aciclovir reduces the incidence of PHN.8
The antivirals that are used are (adult dose):9
Aciclovir 800 mg five times a day for seven days (continuing for two days after crusting of lesions in those who are immunocompromised).
Valaciclovir 1000 mg three times a day for seven days; or
Famciclovir 500 mg three times a day for seven days (ten days in immunocompromised individuals) or 750 mg once or twice a day for seven days.
One review found a significant reduction in risk of pain with valaciclovir and famciclovir for management of herpes zoster virus (HZV) including ophthalmicus. Valaciclovir or famciclovir were both shown to provide significant reduction in the risk of HZV-associated pain.10
An oral antiviral drug should be started within 72 hours of rash onset for:
People of any age with non-truncal involvement (eg, affecting the neck, limbs or perineum).
Cases where there is moderate or severe pain or rash.
Those with ophthalmic involvement.
People who are immunocompromised.
Ramsey Hunt syndrome.
Since the evidence, that oral aciclovir (and possibly other antivirals) do not significantly reduce the incidence of postherpetic neuralgia, clinical judgement should be used to consider whether an oral antiviral should be offered to patients over the age of 50.8
If it is not possible to initiate treatment within 72 hours, consider starting an antiviral drug up to one week after rash onset, especially if the person is at higher risk of severe shingles or complications (eg, continued vesicle formation, older age or severe pain).
For pregnant women, seek specialist advice regarding prescribing antiviral treatment in pregnancy.
Children who are not immunocompromised do not usually require antiviral treatment. Immunocompromised children at high risk of disseminated or severe infection should be treated with a parenteral antiviral drug.
Longer and more intense (intravenous) treatments may be required in the elderly and the immunocompromised.
Early and effective treatment reduces complications.11
Steroids12
The use of oral corticosteroids in the treatment of patients with zoster infection is controversial. As an adjuvant option in the treatment of patients with acute zoster infection, oral corticosteroids have been shown in some studies to ameliorate the inflammatory features and so reduce pain and cosmetically improve the rash. However, studies have shown conflicting results and many consider that any limited benefit is outweighed by the adverse effects of corticosteroids, especially in the elderly.
An exception is Ramsay Hunt syndrome; high-dose oral corticosteroids and antiviral therapy are usually given, ideally starting within 72 hours of onset of symptoms. The effectiveness of steroid use for Ramsay Hunt syndrome is unknown, although it is unlikely to do harm and may potentially facilitate recovery of the facial palsy. Where used, steroids must be co-prescribed with antiviral therapy due to their immunosuppressive properties. Steroids should be avoided in people with:
Hypertension.
Diabetes mellitus.
Peptic ulcer.
Osteoporosis.
Caution is required where prescribing for elderly patients, who are at increased risk for serious adverse events.
Treatment of ocular problems11
Where there is intraocular involvement, various agents are used depending on which tissue is involved. An ophthalmologist should be involved to carry out a detailed assessment and tailor a management plan accordingly.
Patients may benefit from long-term application of ocular lubricants; cool compresses are advised for the conjunctivitis in the acute phase. Epithelial defects are sometimes treated with additional chloramphenicol ointment.
Patients may also require cycloplegics to help pain relief and intraocular pressure-lowering drugs.
Where there is retinitis, choroiditis or optic neuritis, admission for intravenous antivirals may be required.
Topical steroids may only be started under ophthalmic supervision (these are beneficial in certain specific cases and harmful in others).
Intravitreal antiviral therapy may be needed for immunocompromised patients with retinal necrosis.
Where neurotrophic ulcers develop, botulinum toxin administration to produce a protective ptosis may be considered (the effects wear off after about three months). Other options available to manage these ulcers include bandage contact lenses, tissue glue and tarsorrhaphy (the lids are sutured together; depending on the type of procedure, this may or may not be irreversible).
Shingles treatment may be required for many months, or even years.
Corneal scarring may require penetrating keratoplasty (corneal transplant).
Analgesia7
It may be necessary to provide quite strong analgesia if there is pain. First-line treatments include paracetamol (with or without codeine) and non-steroidal anti-inflammatory drugs (NSAIDs).
Tricyclic antidepressants, gabapentin, pregabalin, duloxetine (off-label), steroids and opioids are options used to reduce acute pain where the first-line treatments fail.
Topical analgesia with lidocaine patches has also been shown to be of benefit in the acute stage as well as for PHN. They must be applied to intact skin, not to the area of the rash.
If the pain is severe beyond the moment that the vesicles have crusted over then PHN has probably developed.
Seek specialist advice or refer to the pain team if:
Pain is inadequately controlled by oral analgesia.
A strong opioid (such as morphine) is being considered.
Referral7 11
Ophthalmic involvement: get immediate specialist advice or refer immediately (to be seen within 24 hours).
Immunocompromised patients: get immediate specialist advice regarding shingles treatment or refer immediately. Any patient with known immunodeficiency (including those with organ transplants and patients on systemic immunosuppression or chemotherapy) should be seen urgently by physicians in an infectious disease unit.
More severe disease, recurrence or multiple dermatomal involvement should raise suspicions of underlying immunosuppression; actively look for causes. Consider HIV in patients under 65 years of age.
Refer urgently where complications are present:
Signs of meningitis, encephalitis, or myelitis.
Cranial nerve palsies
Patients with extensive associated cellulitis may need to be admitted for intravenous antibiotics.
Seek specialist advice if a pregnant woman has shingles.
Patients with more severe or persistent neuralgia should be referred early to a pain clinic before the condition becomes chronic.
Shingles complications4
Back to contentsGeneral complications
Skin complications may occur: scarring, pigmentation, secondary bacterial infection.
Ramsay Hunt syndrome: describes a syndrome of lesions in the ear, facial paralysis, hearing loss, tinnitus and vertigo.
Bell's palsy.
Rarely, meningitis, encephalitis, myelitis or hemiparesis may occur.
Disseminated zoster occurs mainly in immunocompromised patients and may lead to visceral dissemination, resulting in pneumonia, encephalitis or hepatitis with a 5-10% mortality rate, even with antiviral drug treatment.
There is a negative impact on quality of life.
Morbidity associated with PHN increases with age.
Complications of ophthalmic shingles
Ocular complications include pain, anterior uveitis and varieties of keratitis. Possible long-term complications include chronic uveitis, keratitis and neuropathic ulceration.
Lid complications include ptosis, trichiasis, scarring of the skin and madarosis (loss of lashes).
Rare ocular complications include optic neuritis, retinitis and ocular cranial nerve palsies. There is a complete or near resolution of ophthalmoplegia in about 65% of cases.13 Sight is threatened by neuropathic keratitis, perforation, secondary glaucoma, posterior scleritis, optic neuritis and acute retinal necrosis. Neurological complications are rare (one series reported this in 5.5% of patients) with meningoencephalitis being noted in a few patients.14
Long-term complications may be related to poor sensation of the cornea and poor motor function of the eyelid. This may put the eye at risk during episodes of impaired consciousness. There is risk of neuropathic ulceration and exposure keratopathy. There is also a risk of complications common to the disease elsewhere, such as PHN. The risk of long-term problems is such that it is recommended that a history of ophthalmic shingles should remain in the problems section of the medical record. There is a 6-14% chance of recurrence.15
Permanent sequelae of ophthalmic zoster infection may include chronic ocular inflammation, loss of vision, and debilitating pain.5 Gradual clouding of the cornea may occur.
Postherpetic neuralgia (PHN)
See the separate Postherpetic Neuralgia article.
Shingles prognosis
Back to contentsThe prognosis for younger and otherwise healthy patients is excellent.
Pregnant women and immunosuppressed patients have the highest risk of serious sequelae.
Elderly people have a significantly increased risk of complications, including PHN, bacterial infections and scarring.
Immune compromise carries poorer prognosis.
Mortality is rare. Disseminated disease in the severely immunocompromised has a case fatality rate reported to be 5-15%, with most deaths occurring due to pneumonia.2
Shingles prevention2 16
Back to contentsStudies have shown that giving older people (adults aged over 60 years) a shingles vaccine boosts their waning immunity and significantly reduces the morbidity due to HZV and PHN.17
Herpes zoster vaccine is effective in preventing herpes zoster disease. The shingles vaccine is well tolerated and produces few systemic adverse events; it is known to last at least three years. Re-vaccination is not considered necessary.18
There are two shingles vaccinations available, Shingrix® and the live attenuated Zostavax® vaccine.
Changes to the shingles vaccination programme in the England from 1 September 2023:19
Change of vaccine:
Shingrix® will replace Zostavax® for the whole shingles programme.
Shingrix® will require a 2-dose schedule for all cohorts. The dosing interval will differ for immunocompromised vs. immunocompetent patients.
Shingrix® should be offered to all people reaching eligible age on or after 1 September 2023. Those cohorts previously eligible for Zostavax® who are under 80 years of age, should continue to be offered Zostavax® until central stocks deplete, after which they should be offered Shingrix®.
individuals who have received Zostavax® previously should not be revaccinated with Shingrix®.
Shingrix® can be administered alongside other vaccines.
Patients can be immunised with the shingles vaccine at any point in the year as soon as they reach eligible age.
Changes to eligibility:
Immunocompromised cohort:
Since September 2021, Shingrix® has been available to immunocompromised individuals aged 70 to 79 years, who are contraindicated to receive Zostavax®, as part of the NHS shingles vaccination programme.
Since 1 September 2023, the eligibility has been expanded to all immunocompromised individuals aged 50 years and over (with no upper age limit).
Immunocompromised individuals who have already received 2 doses of Shingrix® do not need re-vaccination.
Immunocompromised individuals are the highest priority for vaccination given their risk of severe disease. The programme aims to catch up all immunocompromised individuals aged 50 years and over in the first year of implementation.
The second dose of Shingrix® should be given 8 weeks to 6 months after the first dose for this cohort.
Immunocompetent cohort:
The eligible age for immunocompetent individuals has changed from 70 to 60 years of age for the routine cohort, in a phased implementation over a 10 year period.
The routine offer will move from 70 to 60 years of age in 2 stages over a 10 year period as follows:
During stage 1 (1 September 2023 to 31 August 2028):
Shingrix® will be offered to those turning 70 and 65 years on or after 1 September 2023
Zostavax® will be offered to persons aged between 70 to 79 that were eligible for the vaccination programme before 1 September 2023. Once all stocks of Zostavax® are exhausted, these individuals can be offered Shingrix® if they have not previously been given a shingles vaccine.
During stage 2 (1 September 2028 to 31 August 2033):
Shingrix® will be offered to those turning 65 and 60 years of age.
From 1 September 2033 and thereafter, Shingrix® will be offered routinely at age 60 years.
Those who have been previously eligible (in stages 1 and 2) will remain eligible until their 80th birthday.
In the GMS Contract 2021-2022 update, several key changes for vaccination relevant to shingles vaccination were introduced. These include:
Vaccination and immunisation services become an essential service for all routine NHS-funded vaccinations including shingles (exceptions: childhood and adult seasonal influenza, and COVID-19 vaccination, which continue to be enhanced services).
Standardised Item-of-Service (IoS) fee for the delivery of each dose of all routine and annual vaccines at £10.06, fixed for three years.2
The introduction of a childhood varicella-zoster vaccine (as in the USA) would reduce the risk of HZV and, therefore, of PHN, when this cohort of children becomes elderly. However, there is concern that reducing the number of children with VZV by introducing a vaccine could lead to a short-term increase in HZV in those who are latently infected. Therefore, varicella-zoster vaccine is not included in the NHS routine vaccination programme for children.20
Further reading and references
- Shingles vaccination: eligibility poster Posters showing who is eligible for shingles vaccination for GP surgeries, hospitals, care homes and primary care settings.
- Wareham DW, Breuer J; Herpes zoster. BMJ. 2007 Jun 9;334(7605):1211-5.
- Shingles (herpes zoster): the Green Book, Chapter 28a; Public Health England
- Varicella: the Green Book, Chapter 34; Public Health England (June 2019)
- Johnson RW, Alvarez-Pasquin MJ, Bijl M, et al; Herpes zoster epidemiology, management, and disease and economic burden in Europe: a multidisciplinary perspective. Ther Adv Vaccines. 2015 Jul;3(4):109-20. doi: 10.1177/2051013615599151.
- Shaikh S, Ta CN; Herpes zoster ophthalmicus - comprehensive text and pictures, American Family Physician, November 2002
- Cohen JI; Clinical practice: Herpes zoster. N Engl J Med. 2013 Jul 18;369(3):255-63. doi: 10.1056/NEJMcp1302674.
- Shingles; NICE CKS, September 2024 (UK access only)
- Chen N, Li Q, Yang J, et al; Antiviral treatment for preventing postherpetic neuralgia. Cochrane Database Syst Rev. 2014 Feb 6;2:CD006866. doi: 10.1002/14651858.CD006866.pub3.
- British National Formulary (BNF); NICE Evidence Services (UK access only)
- McDonald EM, de Kock J, Ram FS; Antivirals for management of herpes zoster including ophthalmicus: a systematic review of high-quality randomized controlled trials. Antivir Ther. 2012;17(2):255-64. doi: 10.3851/IMP2011. Epub 2011 Dec 15.
- Lam FC, Law A, Wykes W; Herpes zoster ophthalmicus. BMJ. 2009 Aug 13;339:b2624. doi: 10.1136/bmj.b2624.
- Galluzzi KE; Managing herpes zoster and postherpetic neuralgia. J Am Osteopath Assoc. 2009 Jun;109(6 Suppl 2):S7-12.
- Sanjay S, Chan EW, Gopal L, et al; Complete unilateral ophthalmoplegia in herpes zoster ophthalmicus. J Neuroophthalmol. 2009 Dec;29(4):325-37.
- Srinivasan S, Ahn G, Anderson A; Meningoencephalitis-complicating herpes zoster ophthalmicus infection. J Hosp Med. 2009 Jul;4(6):E19-22.
- Opstelten W, Zaal MJW; Managing ophthalmic herpes zoster in primary care. BMJ 2005;331(7509):147.
- https://www.gov.uk/government/collections/shingles-vaccination-programme Shingles UK vaccination programme.
- Tseng HF, Smith N, Harpaz R, et al; Herpes zoster vaccine in older adults and the risk of subsequent herpes zoster JAMA. 2011 Jan 12;305(2):160-6.
- Gagliardi AM, Andriolo BN, Torloni MR, et al; Vaccines for preventing herpes zoster in older adults. Cochrane Database Syst Rev. 2019 Nov 7;2019(11). doi: 10.1002/14651858.CD008858.pub4.
- Shingles vaccination programme changes from september 2023; letter/introduction of shingrix vaccine for the whole programme and expansion of eligible cohorts letter.
- Chickenpox vaccine FAQs; NHS, 2019
Continue reading below
About the authorView full bio

Dr Surangi Mendis, MRCGP
Consultant and Medical Author
MBBS, BSc (1st), MRCGP (2014), DFSRH, PGcert otology and audiology
Surangi Mendis is a consultant in Audiovestibular Medicine and Neuro-otology at The Royal National ENT and Eastman Dental Hospitals, UCLH.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 3 Jan 2029
23 Jan 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free