Sinusitis
Peer reviewed by Dr Surangi Mendis, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 9 Jan 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Acute sinusitis article more useful, or one of our other health articles.
In this article:
Synonym: rhinosinusitis
Continue reading below
Introduction
The paranasal sinuses refer to the frontal, maxillary, sphenoidal and ethmoidal sinuses. These develop as diverticula from the nasal mucosa and are rudimentary or absent at birth, only expanding rapidly during the eruption of permanent teeth and again at puberty.
Diagnostic difficulties may arise due to referred pain: the maxillary sinus is innervated by the infraorbital nerve and anterior, middle and posterior superior alveolar nerves. Hence, pathology here may be felt as upper jaw pain, toothache or pain in the skin of the cheek.
This article will give you an overview of rhinosinusitis. We also have articles dealing with Allergic Rhinitis and Nasal Polyps.
What is sinusitis?
Back to contentsSinusitis is an inflammation of the membranous lining of one or more of the sinuses. Sinusitis is also referred to as rhinosinusitis because inflammation of the nasal mucosa generally accompanies sinusitis.
It can occur as a result of a variety of causes of inflammation, the pathophysiology being that this leads to sinus cavity obstruction and subsequent infection (acute sinusitis) and chronic inflammation (chronic disease). Sinusitis may be classified as:
Acute: an infection lasting 7-30 days.
Subacute: the inflammation lasts 4-12 weeks.
Recurring: there are >3 significant acute episodes in a year lasting ≥10 days with no intervening symptoms.
Chronic: symptoms persist for >90 days (these may be caused by irreversible changes in the mucosal lining of the sinuses), with or without acute exacerbations.
Viral disease is said to last less than 10 days, whereas worsening symptoms after 5 days, or symptoms extending beyond 10 days, suggest bacterial infection.
Continue reading below
Factors predisposing to sinus membrane inflammation
Back to contentsUpper respiratory tract infection.
Allergy.
Smoking.
Hormonal status (eg, pregnancy).
Nasal dryness.
Presence of a foreign body.
Inhalation of irritants (eg, cocaine).
Iatrogenic (eg, nasogastric tubes, mechanical ventilation).
Dental problems (eg, trauma, infection).
Some sporting activities (eg, swimming, diving, high-altitude climbing).
Mechanical obstruction (eg, normal anatomical variations, nasal polyps).
Previous history of trauma (nose, cheeks).
Immunocompromise.
Rare causes include cystic fibrosis, neoplasia, as a part of Samter's triad (aspirin sensitivity, rhinitis, asthma), sarcoidosis, granulomatosis with polyangiitis (GPA) and immotile cilia syndrome. Sinus surgery can also predispose individuals.
Clinical assessment of the sinuses
Back to contentsIn general practice, the most helpful examination technique is simple palpation, as this is quick and easy to perform.
Examination of the sinuses should be complemented by assessment of the nose (external and speculum examination) to assess for evidence of related pathology. Thereafter, investigations are guided by clinical suspicion.
Palpation
All but the sphenoidal sinuses can be palpated for tenderness:
Frontal sinus - press upward beneath the medial side of the supraorbital ridge.
Maxillary sinus - press against the anterior wall, below the inferior orbital margin.
Ethmoidal sinus - press medially against the medial wall of the orbit.
Sinuses
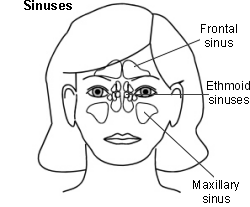
Percussion
Theoretically, sinuses can be percussed for evidence of dullness but the area to percuss is small and their sizes vary from one individual to another. This examination may elicit tenderness where there is infection.
Transillumination
This requires a darkened room and a torch equipped with a sheath which can be drawn up around the light source. It is used to visualise the frontal and maxillary sinuses:
Frontal sinus - draw the sheath up around the light source so that light is only emitted from the tip. This is placed under the medial orbital roof, just posterior to the rim. Direct superomedially and press gently so that no light leaks into the room. Look for a reddish glow just above the eyebrow.
Maxillary sinus - pull the sheath back so that light is transmitted circumferentially from the end of the torch. The torch is placed in the patient's mouth with the instruction to seal the lips around the torch but to leave the jaw open. Direct the light superiorly and look for a red glow in the malar areas.
Continue reading below
Acute sinusitis
Back to contentsThis is defined as a bacterial or viral infection of the sinuses lasting fewer than four weeks and resolving completely with the appropriate management.
It tends to arise as a result of a viral infection.
Causes of acute sinusitis
It is commonly caused by Streptococcus pneumoniae, Haemophilus influenzae and Moraxella catarrhalis.1 The latter is more common in children. In adult patients with suspected acute maxillary sinusitis following a viral upper respiratory infection, about one half have been found to have pus or mucopus in the sinus aspirate, and one third had bacterial pathogens growing in culture.1 Other causes of mucosal swelling (such as allergy) may also lead to impairment of clearance of sinus mucus and subsequent acute sinusitis.
How common is acute sinusitis?
Acute sinusitis is common in adults, with an estimated prevalence of 6-15%.2 Around 1-2 in 100 European visits to a GP are thought to be due to symptoms of acute sinusitis. Acute sinusitis can affect any age group, but is less common in children because their sinuses are not fully developed. It has been reported that around 6-7% of children presenting with respiratory symptoms have features consistent with a definition of acute sinusitis.
Acute sinusitis symptoms
Most commonly, patients present with a non-resolving cold (>1 week or worsening symptoms over 4-5 days) which may have a biphasic character: the initial viral infection (rhinitis) which appears to begin settling is followed by further malaise relating to the sinusitis.1
There may be pain over the affected sinus (this is neither sensitive nor specific and is often described as 'pressure' by the patient). There may be pyrexia, purulent nasal discharge ± decreased or absent smell. Local sinus pain with unilateral predominance in addition to purulent rhinorrhoea had an overall reliability of 85% for diagnosing sinusitis.1 A poor response to nasal decongestants can be suggestive and, in the intensive care setting, this diagnosis should be considered in pyrexia of unknown origin.
Signs
There may be little to elicit other than pain on palpation of the sinuses. Erythema and oedema of the nasal mucosa may also be found.
Diagnosis
Acute sinusitis is diagnosed if there is:
Facial discomfort (eg, a feeling of congestion or fullness, often unilateral and worse when bending forwards) or pain.
Nasal obstruction or (purulent) nasal discharge or postnasal drip.
Decreased or absent sense of smell.
This may be accompanied by:
In children, symptoms of rhinitis predominate ± the additional feature of ear discomfort due to the blockage of the Eustachian tube.
Investigations
Diagnosis is made on the above criteria. There is some controversy about carrying out further investigations, which are generally not required.
CT imaging may be used in secondary care settings where there is diagnostic uncertainty. Sinus puncture and nasendoscopy may have a role in a secondary care setting where there is a pressing need for organism identification.
Differential diagnosis
Adenoiditis, particularly in children.
There are also a number of causes of headaches.
Treatment
Most cases can be managed in the primary care setting.3
Most patients can be reassured that this is generally a viral infection similar to a cold but which takes a little longer to resolve (about 2.5 weeks).
Helpful measures to relieve symptoms include:
Paracetamol/ibuprofen for pain/fever.
Intranasal decongestant (oral is not recommended for sinusitis) for a maximum of a week.
Nasal irrigation with warm saline solution.
Warm face packs, which may provide localised pain relief.
Adequate fluids and rest.
People presenting with symptoms for around 10 days or fewer should not be offered an antibiotic prescription.3 They suggest the clinician give advice about the usual course of acute sinusitis (2 to 3 weeks); an antibiotic not being needed; managing symptoms, including fever, with self-care, and seeking medical help if symptoms worsen rapidly or significantly, do not improve after three weeks, or they become systemically very unwell. The exception to this would be if the patient is not suitable to admit but they are systemically unwell or at high risk of complications due to pre-existing comorbidity. Such cases include patients with:
Significant heart, lung, renal, liver or neuromuscular disease; immunosuppression or cystic fibrosis.
Acute cough who are older than 65 years of age with two of the following risk factors, or older than 80 years of age with one of the following risk factors:
Hospitalisation in the previous year.
Current use of oral corticosteroids.
When the person has been unwell for around 10 days or more, with no improvement, the clinician can consider prescribing a high-dose nasal corticosteroid for 14 days for adults and for children aged 12 years and over.
Alternatively they may offer a deferred antibiotic prescription, taking account of evidence that antibiotics make little difference to how long symptoms last, or the proportion of people with improved symptoms; withholding antibiotics is unlikely to lead to complications; antibiotics may cause possible adverse effects, particularly diarrhoea and nausea.
Also inform people of factors that might make a bacterial cause more likely.
Referral criteria
Arrange hospital admission if there is severe systemic infection.
Arrange hospital admission if there are complications of sinusitis. Look for:
Suspicion of intracranial spread - severe frontal headache, frontal swelling, symptoms or signs of meningitis or focal neurological signs.
Suspicion of spread to the orbit - see the separate Orbital and Preseptal Cellulitis article.
Consider referral for high-risk patients - eg, those who are immunocompromised.
Refer for urgent ENT opinion if there are unilateral symptoms (eg, mass, bloodstained discharge, crusting, non-tender facial pain, facial swelling or unilateral nasal polyps).
Consider routine referral for persistent infections (three or more attacks per year) or persistent symptoms despite an adequate course of second-line antibiotics.
Steam inhalation, antihistamines and mucolytics are no longer recommended. There is no clear evidence supporting the use of complementary or alternative medicine.
Antibiotic choice
If a decision is made to use antibiotics, there are several guidelines available to follow. NICE CKS suggests:2
First-line: phenoxymethylpenicillin (500 mg qds for five days) or co-amoxiclav if more systemically unwell. Alternatives for those who are allergic to penicillin are doxycycline (200 mg stat then 100 mg od for seven days - not in children aged <12 or pregnant women) or clarithromycin (250 mg-500 mg bd for seven days), or erythromycin.
High dose produces quicker improvement but there is an increased risk of diarrhoea.4
American guidelines suggest amoxicillin as first line antibiotic where needed and a cephalosporin with clindamycin for those who are allergic to penicillin.5
Offer review in seven days if needed for patients not treated with antibiotics and whose symptoms worsen within 72 hours, or do not resolve after 72 hours for those treated with antibiotics.
If response to antibiotics is poor, consider compliance issues, look for complications and consider a second-line antibiotic.
Refer if there is still no response or if the patient is deteriorating.
Management principles for children are the same but doxycycline is contra-indicated. Pregnant or breast-feeding mothers in whom antibiotics are considered vital should be treated with erythromycin.
Complications
These are rare (around 2.5 to 4.3 per million people per year).3 They occur more commonly in children. They include orbital cellulitis, meningitis, brain abscess, osteomyelitis (known as Pott's puffy tumour when the frontal bone is affected) and cavernous sinus thrombosis. Very occasionally, there is formation of a cutaneous fistula. Acute sinusitis can become chronic.
Prognosis
Symptoms are likely to be relatively slow to resolve (2-3 weeks, regardless of whether antibiotics are taken or not) but over two thirds of patients experience improvement or resolution of symptoms without antibiotic treatment.
Chronic sinusitis
Back to contentsChronic sinusitis is multifactorial in nature and can include infectious, inflammatory, or structural factors.
Thus, other aetiologies such as allergic rhinitis (dust mites, moulds), exposures (airborne irritants, cigarette smoke or other toxins), structural causes (nasal polyps, deviated nasal septum), ciliary dysfunction, immunodeficiencies, and fungal infections should be considered.6
When infection does occur, it is most frequently caused by anaerobes, Gram-negative bacteria, S. aureus, and coagulase-negative staphylococci. Patients with chronic sinusitis are more likely to have a chronic underlying problem (see risk factors in 'Management' section, above) and patients with this diagnosis should be actively investigated to rule out any treatable conditions.
How common is chronic sinusitis?
Chronic sinusitis is a common condition, affecting 1 in 10 UK adults.2 Data suggest a prevalence of 4.5-12% in North American and European populations. Its prevalence increases with age, and it is more likely to occur in women, and in people with asthma, chronic obstructive pulmonary disease, or a history of allergy.
Paediatric chronic rhinosinusitis is commonly found by ear, nose and throat specialists and may occur as a result of a viral upper respiratory tract infection.
Chronic sinusitis symptoms
These are similar to those of acute sinusitis but not as florid.
Signs
A dull ache on palpation and nasal mucosal inflammation may be noted. Nasal purulence is strongly suggestive and an ear examination should be performed to rule out middle ear fluid. In older patients, it is prudent to complement this with a full neurological examination, as some neurological disorders can be associated with chronic sinusitis.
Diagnosis
The diagnostic criteria are as for acute sinusitis but the symptoms last for more than 12 weeks. It is worth noting that, compared with acute sinusitis, loss of smell is more commonly described and facial pain is less common. Chronic sinusitis may be complicated by acute exacerbations.
Investigations
These are not usually needed in primary care but, should they be organised, the same limitations apply as those outlined for acute disease.
This said, it is important concurrently to assess for evidence of nasal polyps (an important differential - assessment can be found in the separate article Nasal Polyps) as well as for evidence of predisposing factors for chronic sinusitis including:
Chronic dental infection.
Presence of a foreign body (especially in children).
Aspirin sensitivity.
GPA.
Differential diagnosis
Rhinitis (allergic or non-allergic).
Nasal polyps (with which it may be associated).
Foreign bodies in the airways.
Fungal sinusitis.
Tumours (eg, nasopharyngeal, tumours of the sinus or of the nasal cavity, skull base).
Turbinate dysfunction.
Juvenile nasopharyngeal angiofibroma.
Recurring and chronic sinusitis treatment
Management in the first instance is medical, irrespective of whether polyps are present or absent.
There is no consensus on an approach to the management of chronic sinusitis. The treatment should focus on modulating triggers, reducing inflammation, and eradicating the infection.6 Use of oral steroids, topical steroids, antibiotics and nasal saline irrigation are all options for management, dependent on the severity of symptoms. 7
Where there are acute exacerbations complicating the chronic problem, use management strategies outlined under 'Acute sinusitis', above. If these episodes are frequent, consider referring.
Management principles are the same in children but have a lower threshold for referring. Bear in mind that this condition is relatively rare in children and consider alternative diagnoses (eg, rhinitis or adenoidal disease).
Attention to good dental hygiene and stopping smoking (including avoiding passive smoking where possible) are helpful.
When nasal steroids are used, treatment should last at least eight to 12 weeks with proper usage.6
Antihistamines should only be used if an allergic component is suspected.
Antibiotics can be given for an extended period of three weeks. However, there is no consensus on their routine use in chronic sinusitis, nor is there consensus on antibiotic selection.
Empiric antifungal treatment should not be given.
Chronic sinusitis with polyps should be treated with topical nasal steroids.2 If severe or unresponsive to therapy after 12 weeks, a short course of oral steroids can be considered.
Functional endoscopic sinus surgery can be considered for patients who fail medical management. In more complicated cases, it can serve as an adjunct to medical management. The goal of this surgery is to relieve obstructions, to restore drainage and mucociliary clearance, and to ventilate the sinuses.2
Referral for chronic sinusitis
Actively ask about predisposing conditions and manage these accordingly (see 'Investigations', above). If there is no improvement or if there have been more than three exacerbations requiring antibiotics in one year, referral is appropriate. Worrying features outlined in the box above (see 'Acute sinusitis') should also prompt referral.
Specialist treatment
Specialist management may involve further medical care (such as initiation of antibiotics) or endoscopic sinus surgery when there are complications, anatomical variations causing local obstruction, allergic fungal disease or patients who remain very symptomatic despite medical treatment.
It is aimed at restoring sinus ventilation to correcting mucosal opposition in order to restore the mucociliary clearance system. This is limited by long-term scarring and adhesions around the ostium of the sinus. To address this, balloon catheter dilation of the sinus ostia (balloon cineplasty) has been developed.8 This new technique appears promising both in terms of technical success rate and symptomatic relief. To date, it has been associated with a low complication rate.8
Complications
Acute exacerbations are the most common complication and are associated with the same rare complications as those outlined above for acute sinusitis. Additionally, these patients may experience:
Adenoiditis, dacryocystitis and laryngitis in children.
Orbital complications - cellulitis, orbital abscess and cavernous sinus thrombosis.
Intracranial complications - meningitis or abscess formation.
Mucocele formation.
Psychological problems associated with chronic pain and ill health.
Pain may be particularly bad when travelling by plane, especially on landing. Furthermore, scuba divers should consult with specialists, as their sinuses are more prone to barotrauma.
Prognosis
By its nature, this is a long-term problem which does not lend itself to rapid cure. Patients are often frustrated with their management, and poor communication can result in delays in receiving appropriate treatment and timely referral.9 Better coordinated care between general practice and specialist settings and consistency of advice have the potential to increase patient satisfaction and improve outcomes.
Fungal sinusitis
Back to contentsThis is an uncommon infection that was traditionally associated with immunocompromise but which is increasingly seen among the immunocompetent patient population. It is also associated with diabetes.
The most common culprits are the Aspergillus and Mucor species. These give rise to two distinct clinical pictures:
Non-invasive fungal sinusitis: this usually manifests itself with a chronic sinusitis picture before the correct diagnosis is made. It may be further classified into allergic fungal sinusitis and sinus mycetoma - a unilateral lesion usually involving the maxillary sinus.
Invasive fungal sinusitis: this may take on an acute, fulminant character when it is associated with a high mortality rate, unless recognised and treated early, or a more slowly invading nature which tends to occur in those with diabetes. A chronic granulomatous type is also described (almost exclusively) in immunocompetent North African patients.
Symptoms and signs of fungal sinusitis
Allergic fungal sinusitis (AFS) - symptoms of chronic sinusitis, which may be associated with asthma ± nasal polyposis, a cough and headache. AFS is almost exclusively a disease found in areas of high humidity, where mould counts are higher than other regions.10 In these territories, AFS can account for up to 32% of chronic cases undergoing functional endoscopic sinus surgery. Diagnosis is difficult and may only be made after repeated investigation (± surgery) for chronic sinusitis.
Sinus mycetoma - similar to the presentation of acute sinusitis. These (immunocompetent) patients may complain of blowing gravel-like material from the nose.
Acute invasive fungal sinusitis - patients are severely ill with fever, cough, nasal discharge, headache and mental status changes (there is a rapid spread to the orbit and the CNS).11 Orbital cellulitis may be evident. Dark ulcers may be seen on examination of the septum, the turbinates or the palate. Late on, there may be evidence of a cavernous sinus thrombosis.
Chronic invasive fungal sinusitis - similar to chronic sinusitis - patients are not acutely unwell but may show evidence of the orbital apex syndrome (optic neuropathy and restricted globe movements).
Granulomatous invasive fungal sinusitis - similar to chronic invasive sinusitis but with more apparent orbital features such as proptosis.
Diagnosis
This is usually made following referral to the ENT department. Serum total fungus-specific IgE concentrations may be elevated in patients with allergic fungal sinusitis and CT imaging will further help diagnosis.11 MRI scanning helps outline any CNS spread. Microbiology and histology provide the final diagnosis.
Treatment
This should be under the care of the ENT team. The mainstay of treatment is surgical, the aim being to debride the infected tissue (this ranges from conservative to radical, depending on the type of fungal sinusitis).
Antifungal treatment is used where there is invasive infection. Systemic steroids may be indicated postoperatively in patients with allergic fungal sinusitis.
Complications
Varying degrees of invasion and tissue erosion eventually occur in all types if left untreated. The orbit and CNS are then prone to infection and its consequences there.
Treatments of the more aggressive forms may leave the patient with significant head and neck deformities requiring long-term follow-up by plastic surgeons, as well as by immunologists and the infectious diseases team.
Prognosis
All but the acute invasive form carry a good prognosis once the diagnosis is made and treatment completed. Fulminant fungal sinusitis has a very high mortality rate, even with aggressive surgical and medical treatment.
Relapses are common during subsequent episodes of neutropenia so treatment with systemic antifungals as prophylaxis is indicated where this occurs.
Barosinusitis
Back to contentsBarotrauma of the paranasal sinuses is a risk factor for anyone exposed to ambient pressure changes, usually from travelling through mountainous regions, flying or diving. The problem arises as a result of the small size of the ostia of the sinuses limiting the exchange of gases and mucus.
This may lead to accumulation of secretions and an acute or chronic sinusitis. It is a relatively rare condition, most often affecting the frontal sinuses.
Symptoms and signs of barosinusitis
Mild inflammation may give rise to pain (particularly on returning to starting conditions - eg, back to sea level), congestion and occasional epistaxis.
More severe inflammation is characterised by severe, sharp pain and a pressure sensation which is typically in the forehead, in the mid-face or retro-orbital. Epistaxis is common. Clinical examination and findings are similar to those in acute sinusitis.
Diagnosis
This is generally made on history and examination. Think of this diagnosis in individuals who have recently been:
Scuba and sport diving.
Sky diving.
Flying in military/high-performance aircraft.
Exposed to pressure changes, with upper respiratory tract infection or sinusitis.
How common is barosinusitis?
The prevalence ranges from 34% in divers to 19.5% to 25% in pilots.12 Concomitant sinus inflammation increases the prevalence of barosinusitis in pilots, with rates of up to 34% in high-performance fighter pilots and 55% in commercial pilots. Hyperbaric oxygen treatment causes up to 3% of annual cases of barosinusitis. Those with poorly controlled allergies or anatomical abnormalities of the nose and paranasal sinuses are also more at risk.
Treatment
Treatment is best carried out as soon as the symptoms occur, although this is not always possible. Management involves oral analgesia, nasal decongestants to establish ventilation of the sinuses and a prophylactic course of antibiotics.
Prognosis
Patients should make a full recovery from an acute episode, although repeated barosinusitis can lead to chronic sinusitis.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Aring AM, Chan MM; Current Concepts in Adult Acute Rhinosinusitis. Am Fam Physician. 2016 Jul 15;94(2):97-105.
- Sinusitis; NICE CKS, May 2024 (UK access only)
- Sinusitis (acute): antimicrobial prescribing; NICE Guidelines (October 2017)
- Matho A, Mulqueen M, Tanino M, et al; High-dose versus standard-dose amoxicillin/clavulanate for clinically-diagnosed acute bacterial sinusitis: A randomized clinical trial. PLoS One. 2018 May 8;13(5):e0196734. doi: 10.1371/journal.pone.0196734. eCollection 2018.
- DeBoer DL, Kwon E; Acute Sinusitis.
- Kwon E, O'Rourke MC; Chronic Sinusitis
- Chronic Rhinosinusitis; ENT UK
- Balloon catheter dilation of paranasal sinus ostia for chronic sinusitis; NICE Interventional Procedure Guidance, September 2008
- Vennik J, Eyles C, Thomas M, et al; Chronic rhinosinusitis: a qualitative study of patient views and experiences of current management in primary and secondary care. BMJ Open. 2019 Apr 23;9(4):e022644. doi: 10.1136/bmjopen-2018-022644.
- Tyler MA, Luong AU; Current understanding of allergic fungal rhinosinusitis. World J Otorhinolaryngol Head Neck Surg. 2018 Nov 9;4(3):179-185. doi: 10.1016/j.wjorl.2018.08.003. eCollection 2018 Sep.
- Amin M, Shankar VS, Castro LC, et al; Invasive Fungal Sinusitis Minimally Evident by Physical Examination. Clin Pract Cases Emerg Med. 2018 May 18;2(3):258-259. doi: 10.5811/cpcem.2018.4.37872. eCollection 2018 Aug.
- Battisti AS, Lark JD; Barosinusitis. StatPearls Publishing; 2019-. 2019 Mar 13.
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Surangi Mendis, MRCGP
Consultant and Medical Author
MBBS, BSc (1st), MRCGP (2014), DFSRH, PGcert otology and audiology
Surangi Mendis is a consultant in Audiovestibular Medicine and Neuro-otology at The Royal National ENT and Eastman Dental Hospitals, UCLH.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 7 Jan 2029
9 Jan 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free