Spondylolisthesis and spondylolysis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Philippa Vincent, MRCGPLast updated 20 Nov 2021
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Cervical spondylosis article more useful, or one of our other health articles.
In this article:
Continue reading below
What is spondylolisthesis?
Spondylolisthesis is the movement of one vertebra relative to the others in either the anterior or posterior direction. It is commonest at L5-S1.
Anatomy of the vertebrae
The vertebrae can be divided into three portions:
Centrum - the body of the vertebra, which is involved in weight-bearing, and is formed of cancellous bone.
Dorsal arch - surrounds and protects the spinal cord. It carries the upper and lower facet joints of each vertebra which articulate with the facet joints of the vertebra above and below, respectively. The part of the vertebral arch between them is the thinnest part and is called the pars interarticularis, or the isthmus.
Posterior aspect - protrudes and can be palpated on the lower back.
Lumbar vertebra 1 inferior surface
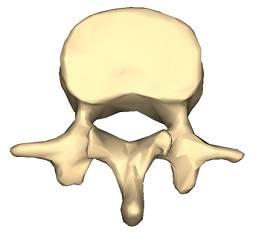
© Anatomography, via Wikimedia Commons
Lumbar vertebra 1 anterior surface
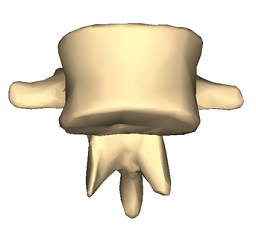
© Anatomography, via Wikimedia Commons
Click here to see a lumbar vertebra 1 close-up superior surface animation.
Types of spondylolisthesis1
Back to contentsStable or unstable.
Asymptomatic or symptomatic.
Graded according to degree of slippage; the Meyerding classification is based on the ratio of the overhanging part of the superior vertical body to the anterio-posterior length of the inferior vertebral body:
Grade I: 0-25%.
Grade II: 26-50%.
Grade III: 51-75%.
Grade IV: 76-100%.
Grade V (spondyloptosis): >100%.
Graded according to type; the Wiltse classification (1976):
Type I: dysplastic (congenital).
Type II: isthmic: secondary to a lesion involving the pars interarticularis:
Subtype A: secondary to stress fracture.
Subtype B: result of multiple healed stress fractures resulting in an elongated pars.
Subtype C: acute pars fracture (rare).
Type III: degenerative.
Type IV: post-traumatic: fracture in a region other than the pars.
Type V: pathological: diffuse or local disease.
Type VI: iatrogenic.
Continue reading below
Spondylolisthesis vs spondylolysis
Back to contentsSpondylolysis and spondylolisthesis are separate conditions, although spondylolysis often precedes spondylolisthesis.
Spondylolysis is a bony defect (commonly due to a stress fracture but it may be a congenital defect) in the pars interarticularis of the vertebral arch, separating the dorsum of the vertebra from the centrum. It may occur unilaterally or bilaterally. It most commonly affects the fifth lumbar vertebra and may cause back pain.
Spondylolisthesis refers to the anterior slippage of one vertebra over another (or the fifth vertebra over the sacrum).
Spondylosis is a general term for degenerative osteoarthritic changes in the spine. There may be changes in the facet joints with osteophyte formation and this may put pressure on the nerve roots, causing motor and sensory disturbance. Spondylosis is seen in around 80% of asymptomatic patients over 50; x-ray findings may not always be the cause of symptoms.2
How common is spondylolisthesis and spondylolysis? (Epidemiology)
Back to contentsSpondylolysis is a common diagnosis with a high prevalence in children and adolescents complaining of low back pain.
There is an increased risk of spondylolysis in young athletes like gymnasts, presumably due to impact-related stress fractures. However most cases are low-grade. At-risk activities include gymnastics, diving, tennis, cricket, weightlifting, football and rugby.
Isthmic spondylolisthesis affects around 3-7% of the population but is more common in young athletes. 60-80% of people with spondylolysis have associated spondylolisthesis.3
The majority of cases of spondylolysis and spondylolisthesis affect L5-S1 and most of the remainder affect L4-L5.
Degenerative spondylolisthesis is more common in older people, particularly women.
Most cases of spondylolisthesis are asymptomatic.
Continue reading below
Spondylolisthesis causes (aetiology)
Back to contentsSpondylolisthesis commonly occurs due to a fracture or defect in the pars interarticularis, the narrowest part of the posterior vertebral arch between the upper and lower facet joints. When this is breached, the upper facet joint may no longer be able to hold the vertebra in place against the downward force of body weight and forward/downward slippage occurs.
Risk factors for spondylolisthesis
Risk factors that increase the risk of spondylolysis developing into spondylolisthesis include :
Female gender.
Young age.
Presence of spina bifida or spina bifida occulta.
Vertebral wedging.
Hyperlordosis.4
Positive family history.
Certain high-impact sports, as evidenced by increased rates in athletes and gymnasts.3
Symptoms of spondylolisthesis (presentation)
Back to contentsSpondylolisthesis symptoms
Presentation varies slightly by type although common spondylolisthesis symptoms include exercise-related back pain, radiating to the lower thighs, which tends to be eased by rest, particularly in positions of spinal flexion.
Isthmic spondylolisthesis
Most patients are asymptomatic, even with progressing slippage.
Symptoms often begin around the adolescent growth spurt.
Back pain - worse with activity (particularly back extension) - this may come on acutely or insidiously.
Pain may flare with sudden or trivial activities and is relieved by resting.
Pain is worse with higher grades of disease.
Pain may radiate to buttocks or thighs
There are usually no neurological features with lower grades of slippage but radicular pain becomes common with larger slips. Pain below the knee due to nerve root compression or disc herniation would suggest more severe slippage. High degrees of spondylolisthesis may present with neurogenic claudication or even cauda equina impingement.
Tightened hamstrings are very common
There may be enhanced lordosis and a waddling gait with shortened step length.
There may be gluteal muscular wasting.
Degenerative spondylolisthesis
Pain is aching in nature and insidious in onset.
Pain is in the low back and posterior thighs.
Neurogenic claudication may be present with lower-extremity symptoms worsening with exercise.
Symptoms are often chronic and progressive, sometimes with periods of remission.
If lumbar stenosis is also present, reflexes may be diminished.
Dysplastic spondylolisthesis
Presentation and physical findings are similar to isthmic spondylolisthesis but with a greater likelihood of neurological compromise.
Traumatic spondylolisthesis
Patients will have experienced acute trauma and are likely to have significant pain.
Severe slips may cause cauda equina compression with bladder and bowel dysfunction, radicular symptoms or neurogenic claudication.
Physical findings are as for the other types.
Pathological spondylolisthesis
Symptoms may be insidious in onset and associated with radicular pain.
Physical findings are as for the other types.
Spondylolysis symptoms
Most cases of spondylolysis are asymptomatic and identified incidentally.
It may present with low back pain provoked by lumbar extension, paraspinal spasm and tight hamstrings.
It frequently does not show on X-ray. It is important to consider it in the differential diagnosis of back pain, as its identification can prevent progression and avoid the potential need for aggressive intervention.
Differential diagnosis
Back to contentsOther causes of back pain need to be ruled out such as:
Spinal cord lesion.
Diagnosing spondylolisthesis (investigations)
Back to contentsBlood tests - looking for infection, myeloma, hypercalcaemia/hypocalcaemia.
Lateral spinal X-rays - will show spondylolisthesis. These are best performed in the position of maximal pain.
Oblique spinal X-rays - may (but will often not) detect spondylolysis.
Radionuclide scintigraphy and CT may help in cases of spondylolysis in distinguishing progressing lesions of the pars from stable lesions.
MRI is often performed perioperatively to look at relationships between the bony and neurological structures in the compromised area.
Spondylolisthesis treatment and management
Back to contentsThe goal of treatment is to relieve pain, stabilise the spinal segment, and stop or reverse the slippage. It is important to recognise that many of these treatment options, including bracing, early physiotherapy and steroid injections or nerve blocks, may not be available on the NHS.
Conservative treatment
Conservative treatment will usually be used first and up to 90% of athletes with spondylolisthesis returned to activities within 6 months of conservative management.5
Conservative treatment includes restricting activity, bracing ,and pain control using medication. If this has not been successful within 2 weeks, physiotherapy is normally advised and exercise such as cycling or swimming is recommended to maintain fitness levels without causing further damage. Treatment such as bracing and decreased activity have been shown to be most effective with patients who have early diagnosis and treatment. If this is not successful within 6 weeks, epidural steroid injections or selective nerve blocks may be considered.5
Surgical treatment
If there is evidence of progression or if conservative measures are ineffective then surgical therapy may be offered. This depends also on degree and aetiology.
Surgical intervention involves a prolonged rehabilitation period so it is generally not considered until conservative treatments have failed. An exception would be in the case of significant instability or neurological compromise and in high-grade slips.
Surgical therapy involves fusing the affected vertebra with a neighbouring normally aligned vertebra (both anteriorly and posteriorly). The intervertebral disc is usually also removed, as it is inevitably damaged. The slipped vertebra may be realigned.
There are relatively few studies looking at the benefits of surgical management although those that exist tend to show that patients report benefit from surgery.5
Complications of surgical repair
Back to contentsImplant failure.
Pseudoarthrosis (failure of bone healing leading to a 'false joint').
Poor alignment of the fusion.
Neurological damage: foot drop, spinal cord compression. Chronic nerve injury/inflammation: neuropathic pain can persist in the face of apparent surgical success, possibly due to permanent changes in the nerves or a deregulation of pain control mechanisms.
Prognosis1
Back to contentsThe prognosis for low grade spondylolisthesis is excellent with the majority of patients remaining asymptomatic or expressing very little progression over time. Children with spondylosis and low-grade spondylolisthesis usually remain stable and the x-ray findings may revert to normal without intervention. Adults usually have little progression although this can occur with age-related degenerative changes.
High-grade spondylolisthesis is more difficult to predict. Progression is more likely and adults often present with significant mechanical instability, sagittal malalignment, and neurological symptoms. They are more likely to need surgical intervention, although the risk of complications means this needs careful planning.
Dr Mary Lowth is an author or the original author of this leaflet.
Further reading and references
- Margetis K, Gillis CC; Spondylolisthesis.
- R Prasath et al.; Lumbar Spondylosis: Clinical Presentation And Treatment Approaches –A Systematic Review. Journal of Pharmaceutical Negative Results, Volume13, Special Issue9, 2022
- Spondylolysis: A Narrative Review of Etiology, Diagnosis, and Management; V Madden et al; International Journal of Environmental Research and Public Health
- Hyperlordosis.
- Li N, Scofield J, Mangham P, et al; Spondylolisthesis. Orthop Rev (Pavia). 2022 Jul 27;14(3):36917. doi: 10.52965/001c.36917. eCollection 2022.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Nov 2026
20 Nov 2021 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free