Strawberry naevus
Peer reviewed by Dr Laurence KnottLast updated by Dr Colin Tidy, MRCGPLast updated 18 Feb 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonym: infantile haemangioma
Continue reading below
What is strawberry naevus?
Strawberry naevus is the name given to an haemangioma which occurs in infancy, usually on the face.
Natural history1
Back to contentsThe strawberry naevus may be present at birth, or may develop within the first weeks after birth.
They may begin as a small flat red area but usually develop into a raised dimpled (strawberry-like) lesion.
The strawberry naevus typically grow in size as the child grows, until the age of approximately 9 months, when they start to regress spontaneously.
Involution is usually comlete by 10-12 years of age.
Continue reading below
Epidemiology2 3
Back to contentsStrawberry naevi are the most common vascular tumours of infancy, usually appearing in early infancy.
Strawberry naevi are very common, occurring in about 5-10% of white babies.
Strawberry naevi are rather less common in children of Afro-Caribbean origin and even more uncommon in those of Asian extraction.
There is a 3:1 female preponderance.
They can be associated with a low birth weight, prematurity, multiple gestation and chorionic villus sampling.
Presentation4
Back to contentsOne third of strawberry naevi will be evident at birth, the remainder developing in the first 4-6 weeks after birth.
In the initial stages, the strawberry naevus may be bluish or red spots or patches and the superficial lesions may remain flat. Deeper lesions have a bluish appearance. Compound lesions may occur, having both superficial and deep areas.
The vast majority (around 60%) of strawberry naevi occur on the head and neck but, occasionally, these lesions may occur at other sites throughout the body.
Capillary haemangioma or strawberry birthmark
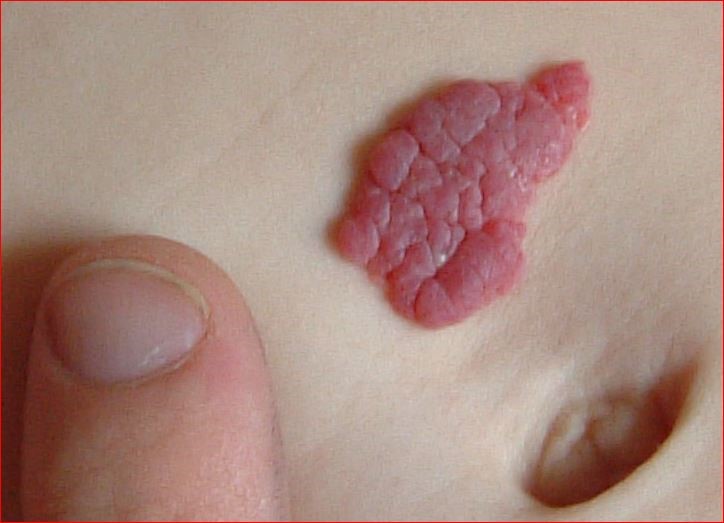
© User: Zeimusu, Public domain, via Wikimedia Commons
Around 20% are multiple. If more than five are present, this can indicate internal haemangiomatosis. The liver is the most common site.
They classically undergo a proliferative period lasting months during young infancy, followed by a longer period of gradual involution throughout childhood.
The vast majority of strawberry naevi cause no symptoms at all; however, visceral haemangiomas or large superficial haemangiomas may cause problems.
Continue reading below
Differential diagnosis
Back to contentsAngiosarcoma.
Arteriovenous (AV) malformation.
Congenital haemangioma (that does not involute).
Teratoma.
Venous malformation.
Diffuse neonatal haemangiomatosis.
Investigations1 5
Back to contentsUsually, no investigations will be required. The diagnosis is usually made clinically.
If there is uncertainty about the lesion, MRI and Doppler ultrasound may be used. Doppler may be useful to assess the persistence, increase or resolution of AV fistulae, as this can influence the decision to observe or to treat.
Imaging with ultrasound or MRI is recommended for those patients with complicated strawberry naevi.
Biopsy, if required, should be undertaken with caution, as these lesions are very vascular.
If more than five strawberry naevi are found then an ultrasound of the liver should be undertaken.
Associated diseases
Back to contentsIn approximately 10% of patients strawberry naevi can be complicated, particularly those involving the airway, the oral cavity or the eye6 .
Periorbital strawberry naevi particularly with involvement of the upper eyelid, require refraction with retinoscopy to check for visual disturbances, especially astigmatism, and to prevent visual deprivation amblyopia.
Rapidly growing strawberry naevi can impinge on vital structures of the head and neck, particularly the airway or auditory canals. Large strawberry naevi of the beard area have a higher incidence of upper airway haemangiomas. This may present as noisy breathing or stridor.
A strawberry naevus over the midline of the back may be a sign of an underlying occult spinal dysraphism, such as a tethered cord.
Very rarely, they can be associated with systemic conditions, such as Kassabach-Merritt syndrome (thrombocytopenia) and neurocutaneous PHACE syndrome (a disorder in which a child is born with posterior fossa malformation, cervico-facial haemangiomas, arterial anomalies, cardiac defects and various eye anomalies)7 .
Management
Back to contentsThe majority of these strawberry naevus will involute spontaneously over time and will require no treatment2 . This is especially true of those in premature babies.
Some strawberry naevi of the head and neck cause disturbance of the visual axis or airway compromise due to mass effect and therefore require early intervention.
Currently, propranolol is the preferred treatment for problematic proliferating strawberry naevi. A Cochrane review found that oral propranolol and topical timolol maleate are more beneficial than placebo in terms of clearance or other measures of resolution, or both, without an increase in harms8
Beta-blockers, usually oral propranolol, can be very effective in treating these lesions9 .
Treatment with topical beta-blockers, such as topical timolol, have been shown to be an effective treatment10 .
The rapid action of propranolol has been shown to be especially dramatic in strawberry naevi involving dyspnoea, haemodynamic compromise, palpebral occlusion or ulceration11 .
The mechanism of effect of beta-blockers is not fully understood.
Intralesional corticosteroids slow proliferation but are less commonly used now12 .
Interferon alfa (IFN-α) is used in some cases13 .
Surgical excision of proliferating strawberry naevi needs care as they are very vascular.
Larger, visceral or life-threatening lesions may be treated with a combination of surgery and embolisation therapy.
Complications
Back to contentsLarge facial strawberry naevi may cause problems with sight, hearing, breathing, swallowing and speaking. They should be treated immediately to prevent further problems.
Bleeding or ulceration may occur.
Visceral haemangiomas may produce symptoms due to bleeding or mass effect. The symptoms will vary according to site.
Hepatic haemangiomas are associated with high-output cardiac failure that can be life threatening14 .
Occasionally, they may impinge on vital structures, ulcerate, bleed, and induce consumptive coagulopathy or significant structural abnormalities. Those on the face are of greatest concern.
Prognosis
Back to contentsStrawberry naevus are the most common tumours in infancy and usually resolve without any scarring.
Up to 90% resolve completely by the age of 9 years2 .
Further reading and references
- Infantile haemangiomas (including strawberry naevi); Primary Care Dermatology Society.
- Mahady K, Thust S, Berkeley R, et al; Vascular anomalies of the head and neck in children. Quant Imaging Med Surg. 2015 Dec;5(6):886-97. doi: 10.3978/j.issn.2223-4292.2015.04.06.
- Goelz R, Poets CF; Incidence and treatment of infantile haemangioma in preterm infants. Arch Dis Child Fetal Neonatal Ed. 2015 Jan;100(1):F85-91. doi: 10.1136/archdischild-2014-306197. Epub 2014 Oct 28.
- Smith CJF, Friedlander SF, Guma M, et al; Infantile Hemangiomas: An Updated Review on Risk Factors, Pathogenesis, and Treatment. Birth Defects Res. 2017 Jul 3;109(11):809-815. doi: 10.1002/bdr2.1023. Epub 2017 Apr 12.
- Infantile haemangioma; DermNet NZ
- Hernandez JA, Chia A, Quah BL, et al; Periocular capillary hemangioma: management practices in recent years. Clin Ophthalmol. 2013;7:1227-32. doi: 10.2147/OPTH.S39029. Epub 2013 Jun 21.
- Winter PR, Itinteang T, Leadbitter P, et al; PHACE syndrome - clinical features, aetiology and management. Acta Paediatr. 2016 Feb;105(2):145-53. doi: 10.1111/apa.13242. Epub 2015 Nov 27.
- Novoa M, Baselga E, Beltran S, et al; Interventions for infantile haemangiomas of the skin. Cochrane Database Syst Rev. 2018 Apr 18;4:CD006545. doi: 10.1002/14651858.CD006545.pub3.
- Kumar MG, Coughlin C, Bayliss SJ; Outpatient use of oral propranolol and topical timolol for infantile hemangiomas: survey results and comparison with propranolol consensus statement guidelines. Pediatr Dermatol. 2015 Mar-Apr;32(2):171-9. doi: 10.1111/pde.12435. Epub 2014 Dec 29.
- Ovadia SA, Landy DC, Cohen ER, et al; Local administration of beta-blockers for infantile hemangiomas: a systematic review and meta-analysis. Ann Plast Surg. 2015 Feb;74(2):256-62. doi: 10.1097/SAP.0000000000000390.
- Ji Y, Chen S, Xu C, et al; The use of propranolol in the treatment of infantile haemangiomas: an update on potential mechanisms of action. Br J Dermatol. 2015 Jan;172(1):24-32. doi: 10.1111/bjd.13388. Epub 2014 Dec 17.
- Izadpanah A, Izadpanah A, Kanevsky J, et al; Propranolol versus corticosteroids in the treatment of infantile hemangioma: a systematic review and meta-analysis. Plast Reconstr Surg. 2013 Mar;131(3):601-13. doi: 10.1097/PRS.0b013e31827c6fab.
- Mirbehbahani N, Rashidbaghan A; Treatment process for capillary hemangioma. Iran J Ped Hematol Oncol. 2014;4(3):127-30. Epub 2014 Jul 20.
- Bajenaru N, Balaban V, Savulescu F, et al; Hepatic hemangioma -review. J Med Life. 2015;8 Spec Issue:4-11.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Feb 2027
18 Feb 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free