Epididymo-orchitis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Pippa Vincent, MRCGPLast updated 14 Jul 2023
Meets Patient’s editorial guidelines
In this series:Scrotal lumps, pain and swellingTesticular torsionEpididymal cystVaricoceleHydrocele in adultsHydrocele in children
Epididymo-orchitis is an inflammation of the epididymis (the tube which stores and transports sperm) and/or testicle (testis). In adults, epididymo-orchitis is usually due to infection, most commonly from a urine infection or a sexually transmitted infection. A course of antibiotic medicine will usually clear the infection. Full recovery is usual. Epididymo-orchitis complications are uncommon.
In this article:
Continue reading below
What is epididymo-orchitis?
Epididymitis means inflammation of the epididymis (the structure next to the testicle (testis) that is involved in making, storing and transporting sperm).
Orchitis means inflammation of a testicle.
As the epididymis and testis lie next to each other, it is often difficult to tell if the inflammation is of the epididymis, the testis or both. Therefore, the term epididymo-orchitis is often used.
Testis - epididymitis and orchitis
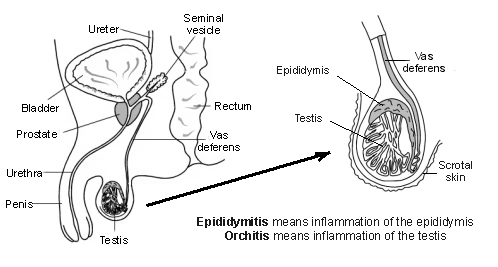
Causes of epididymo-orchitis
In boys who have not reached puberty, epididymo-orchitis is rare and symptoms are usually not due to an infection though they can occasionally occur as a result of a urine infection. The most common cause at this age is thought to be urine refluxing into the duct that sperm pass down (the ejaculatory duct, or vas deferens).
Rarely, epididymo-orchitis in children can be a complication of Henoch-Schönlein purpura, a condition caused by inflammation of the blood vessels.
In over-14s, most cases of epididymo-orchitis are due to an infection. Causes of infection include the following:
A complication from a urine infection
Germs (bacteria) such as E. coli that cause urine infections can sometimes track down the vas deferens (the tube that connects the epididymus to the urethra) to cause an epididymo-orchitis. This can happen at any age and is the most common cause of epididymo-orchitis in men aged over 35 years. This is because partial blockage of urine flow becomes more common with increasing age, either due to an enlarged prostate gland or narrowing of the urethra (urethral stricture). The urethra is the tube that urine flows out of from the bladder. Partial blockage of urine makes you more prone to develop urine infections.
Sexually transmitted infection
A sexually transmitted infection is the most common cause of epididymo-orchitis in young men (but can occur in any sexually active man). It most commonly occurs with chlamydial and gonorrhoeal infections. In men, these infections typically infect the urethra to cause a urethritis. However, sometimes the infection can track down the vas deferens to the epididymis and testicle (testis).
The mumps virus
The mumps virus used to be a common cause. Most people with mumps develop swelling of the parotid salivary glands. However, mumps in boys also causes epididymo-orchitis in about 1 in 5 cases. The virus gets to the testicles via the bloodstream. This cause is now less common since the measles, mumps and rubella (MMR) immunisation is now routinely given to children.
An operation to the prostate gland or urethra
This may allow germs (bacteria) into the urethra which may track down to the testicles. Epididymo-orchitis used to be a common complication after removal of the prostate gland (prostatectomy). This is now rare due to newer surgical techniques.
Medication
Epididymo-orchitis can occasionally be a side-effect of a medicine called amiodarone (a medication used for heart rhythm problems). It normally occurs at doses above 200 mg, especially when the dosage range reaches 400-800 mg.
Uncommon causes of epididymo-orchitis
Other viral infections are uncommon causes of epididymo-orchitis. Infection from other parts of the body can travel in the blood to the testicles, such as tuberculosis (TB) and brucellosis. When this happens it is usually in people who have a problem with their immune system (for example, people with AIDS).
Schistosomiasis is a tropical infectious disease that can cause epididymo-orchitis. Men with Behçet's disease may develop inflamed testicles to cause a non-infective epididymo-orchitis. Injury to the scrotum can cause inflammation of the epididymis and testicle.
Continue reading below
How common is epididymo-orchitis?
Epididymo-orchitis occurs in about 1 in 1,000 males. It is common in men aged 15-30 years and in men aged over 60 years and is rare before puberty. About 3 in 10 boys who have mumps after puberty develop orchitis. The risk of developing epididymo-orchitis is increased if a catheter or other instruments are inserted into the urethra.
Symptoms of epididymo-orchitis
Symptoms usually develop quickly - over a day or so. The affected epididymis and testicle can swell rapidly and the scrotum often becomes enlarged, tender and red. It can be very painful. Sometimes there is pain without significant swelling or redness but it will be very tender when examined.
There may be other symptoms if the epididymo-orchitis is a complication from another infection. For example, there may be pain on passing urine if there is a urine infection or a discharge from the penis if there is a sexually transmitted infection. As with any infection, there may be a high temperature (fever) and general symptoms of feeling unwell.
Continue reading below
Diagnosing epididymo-orchitis
Tests to look for infecting germs (bacteria)
A urine test will usually be done if a urine infection appears to be the root cause. A urine sample might also be taken if a sexually transmitted infection is thought to be the root cause (swabs from the penis used to be taken but urine tests will often give the necessary results nowadays). Sexual partners of people with epididymo-orchitis caused by a sexually transmitted infection will also need testing.
Ideally, someone with epididymo-orchitis should be assessed in a sexual health clinic, particularly under the age of 40 where 50% of epididymo-orchitis infections will be due to a sexually transmitted infection.
See the separate leaflets called Genital Chlamydia, Urethritis and Urethral Discharge in Men and Gonorrhoea for more details.
Blood tests
Blood tests may occasionally be requested including a full blood count or aCRP to look for evidence of infection and inflammation. However, these would not usually be needed.
Tests of the urinary tract
Tests to look into the urethra and bladder may be needed if a urine infection is the cause and if this is thought to be due to other urinary tract abnormalities. Referral to a urology specialist may be considered depending on the results of some of the tests (eg if there is still urine left in the bladder after passing urine).
See the separate leaflets called Urine Infection in Men and Urine Infection in Children for more details.
Treatment for epididymo-orchitis
A course of antibiotic medicines is usually advised as soon as epididymo-orchitis is diagnosed; these are usually given for two weeks. These normally work well. Pain usually eases within a few days but swelling may take a week or so to go down, sometimes longer. The choice of the antibiotic depends on the most likely underlying cause of the infection.
Symptoms should start to improve within three days and further advice should be sought if there is no improvement or if the symptoms have not completely disappeared in two weeks.
If a sexually transmitted infection is the cause then sex should be avoided until treatment and follow-up have been completed. Sexual partners of men with epididymo-orchitis caused by a sexually transmitted infection may also need antibiotic treatment.
The vast majority of epididymo-orchitis infections are caused by bacteria which is why antibiotics are prescribed. Antibiotics do not kill viruses and they are not needed if a viral infection is the cause - for example, mumps.
Supportive underwear may help to ease the pain. Painkillers and ice packs (ice should never be applied directly to the skin) will also ease the pain.
Complications of epididymo-orchitis
Most people recover fully from epididymo-orchitis and complications are uncommon. Possible complications include:
Ongoing pain or swelling in the testicle - this settles within three months in more than four in five men with epididymo-orchitis.
A collection of pus due to infection (an abscess) occasionally develops in the scrotum. This may need a small operation to drain the pus.
Reduced fertility in the affected testicle (testis), especially in cases caused by the mumps virus.
An ongoing (chronic) inflammation occasionally develops.
Rarely, serious damage to the testicle may occur and result in dead tissue (gangrene) in the testicle that needs to be surgically removed.
Further reading and references
- Sexually Transmitted Infections in Primary Care; Royal College of General Practitioners and British Association for Sexual Health and HIV (Apr 2013)
- United Kingdom BASHH national guideline for the management of epididymo-orchitis; British Association for Sexual Health and HIV (2019)
- Epididymitis and Orchitis; Urology Care Foundation
- Rupp TJ, Leslie SW; Epididymitis.
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Jul 2028
14 Jul 2023 | Latest version

Feeling unwell?
Assess your symptoms online for free