When will I get my COVID-19 vaccine?
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Sarah JarvisLast updated 23 Feb 2021
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
With news that the COVID-19 vaccine has been offered to to government's top 4 priority groups in the UK, the prospect of vaccination available to all is becoming more real. Here we explore which groups have been offered vaccination, why they were prioritised and who comes next.
In this article:
Video picks for Vaccination, tests and treatment
Vaccinations are a crucial tool in preventing the spread of many diseases, and during the COVID-19 pandemic many of us have been waiting with bated breath for a vaccine to become available.
When the Government announced its plan for the largest vaccination programme in British history, they aimed to carry out 2 million vaccines a week at 2,700 vaccine sites around the UK. On 14th February, they reached their milestone of offering vaccination to the top 4 priority groups a day ahead of schedule.
Continue reading below
First vaccinations
The top 4 priority groups included all those at the highest risk of serious complications or death should they contract COVID-19, as well as those working in environments where they are at a high risk of contracting the virus and/or passing it on to vulnerable people.
This includes:
Residents and workers in care homes for older adults.
People over the age of 70 (70-79 year-olds will be invited after over-80s have all been invited).
Frontline social and healthcare workers.
Clinically extremely vulnerable people (who have received a letter asking them to shield).
The vaccinations were offered by a mixture of national vaccine centres and GP practices working together in 'hubs'. GP practices arranged the provision of vaccines to care homes and housebound patients.
Everyone in these groups has now been offered a vaccine and the vast majority, including at least 95% of care home residents, have had at least one dose. However, not everyone invited for vaccination has had one. For instance:
If you've had COVID-19, it's not possible to vaccinate until at least 28 days after your symptoms started or you had a positive test.
Some care homes have not been able to get vaccinations because of ongoing COVID-19 outbreaks at the home.
Some patients with multiple allergies aren't suitable for vaccination at GP hubs and have to wait for an appointment at a specialist centre with full resuscitation equipment on site.
In addition, some people have turned down the offer of vaccination, largely on the basis of unfounded vaccine scare stories. While over 1 million healthcare workers with patient-facing roles (about 90% of the total) have been vaccinated, only about 70% of care home workers have accepted vaccination, with even lower levels in areas such as London, where a higher proportion of care home workers are of BAME origin.
If you are in one of these 4 groups and haven't received an invitation, please contact your GP or the national coronavirus booking line if you live in England. You can find out more from the relevant national vaccine booking service if you live in Scotland, Wales or Northern Ireland. If you have recently moved, or changed your phone number, make sure that your GP practice has your up-to-date contact information.
What happens next?
Back to contentsAs it's impossible for everyone to get the vaccine at the same time, the Joint Committee on Vaccination and Immunisation (JCVI) has had to look at data and decide how they can best protect the vulnerable. The priority is to vaccinate those at highest risk of death from the disease in the first instance.
The JCVI has recommended the following priority order for the rollout of the vaccine now that everyone in groups 1-4 has been offered vaccination:
Group 5 - people aged 65-69.
Group 6 - anyone aged 16-64 who has an underlying health condition that makes them more at risk of suffering serious disease if infected with COVID-19.
Group 7 - people aged 60-64.
Group 8 - people aged 55-59.
Group 9 - people aged 50-54.
Practices, and the national booking service, will work their way through the priority groups, starting to invite people in the next group once the vast majority of people in previous groups have been invited.
During the vaccination process for groups 1-4, there was considerable confusion for some patients who were invited by both their practice and the NHS central booking service. As a result, invitations are now being separated out between the two providers.
If you are in group 5,you will receive a letter and can use the NHS central booking hub (in England) to book an appointment. You will need to be registered at a general practice to be eligible. You can choose to ask to be vaccinated at your practice instead, but this may entail a longer wait. If you're invited by the central hub, you can choose an appointment at one of the high street pharmacies which have also started providing a vaccination service.
If you are in group 6, you should be contacted by your practice over the next few weeks. The current aim is to offer everyone in groups 1-9 a vaccine by mid-April. However, it is worth bearing in mind that on 16th February, an extra 1.7 million people were added to the group asked to shield until at least 31st March.
These people have been identified as being at high risk on the basis of their age, underlying health conditions, deprivation, weight and ethnicity. While about 900,000 of them have already been offered vaccination on the basis of their age, the 800,000 remaining will be prioritised for invitation by practices above other people in group 6.
General practices are working in groups of a few practices, of which one or two will usually be offering the vaccine. You may receive a letter, text or phone call inviting you for vaccination. Because many practices are sometimes only given a couple of days' notice of receipt of a supply of vaccine, the invitation may come at short notice.
Continue reading below
50-65 year-olds
Back to contentsMost people aged 60-64 (group 7) will not be invited for vaccination until everyone over 65 and all those with underlying health conditions have been vaccinated. Once this group is finished, invitations will go out to group 8 (55-59 year-olds), then group 9 (50-54 year-olds) once group 8 is finished.
The timeline for these isn't entirely set and is partly dependent on vaccine availability. However, there are about 4.7 million 50-54 year-olds, 4.4 million 55-59 year-olds, 3.8 million 60-64 year-olds and 3.4 million 65-69 year-olds in the UK. Add these to the 7.3 million in group 6 and each group should be invited (vaccine availability permitting), at a very rough estimate around the following dates:
Group 5/6 mid-February to mid-March.
Group 7 mid-second half March.
Groups 8 and 9 end of March-early April.
However, it's worth bearing in mind that some areas of the UK may vaccinate more quickly than other areas - that's why you may find people in a lower group than you being invited before you.
Why have these groups been chosen?
Back to contentsThe JCVI has prioritised the vaccine for those who are most at risk of serious complications or death from COVID-19. It estimates that groups 1-9 listed above represent about 99% of those at risk from dying of COVID-19.
Continue reading below
Under-50s
Back to contentsAs the vaccine is rolled out, scientists continue to study the data and the behaviour of the virus as more people gain immunity. The government is now talking about vaccinating all adults in the UK by July.
The efficacy and safety of the vaccines on those aged under 16 are not yet established, but tests are underway and the vaccine may be offered to children in the future. It is important to remember that children, even if they have serious underlying health problems, are at very much lower risk than older people of serious COVID-19 complications. However, studies of vaccine safety and efficacy are now going on in children, as vaccinating them may allow us to approach the 'community immunity' levels needed to prevent the virus circulating widely at all.
Vaccine FAQs
Back to contentsWhat if I am pregnant or breastfeeding?
Although the vaccine has been deemed safe, more data are required before it can be routinely recommended for all women who are pregnant. However, if you are pregnant and at higher than usual risk because of your occupation or an underlying health condition, you may be offered the vaccine.
If you become pregnant between your first and second doses, you should delay the second dose until you have had your baby (unless you are at high risk).
The vaccine has been deemed safe for women who are breastfeeding.
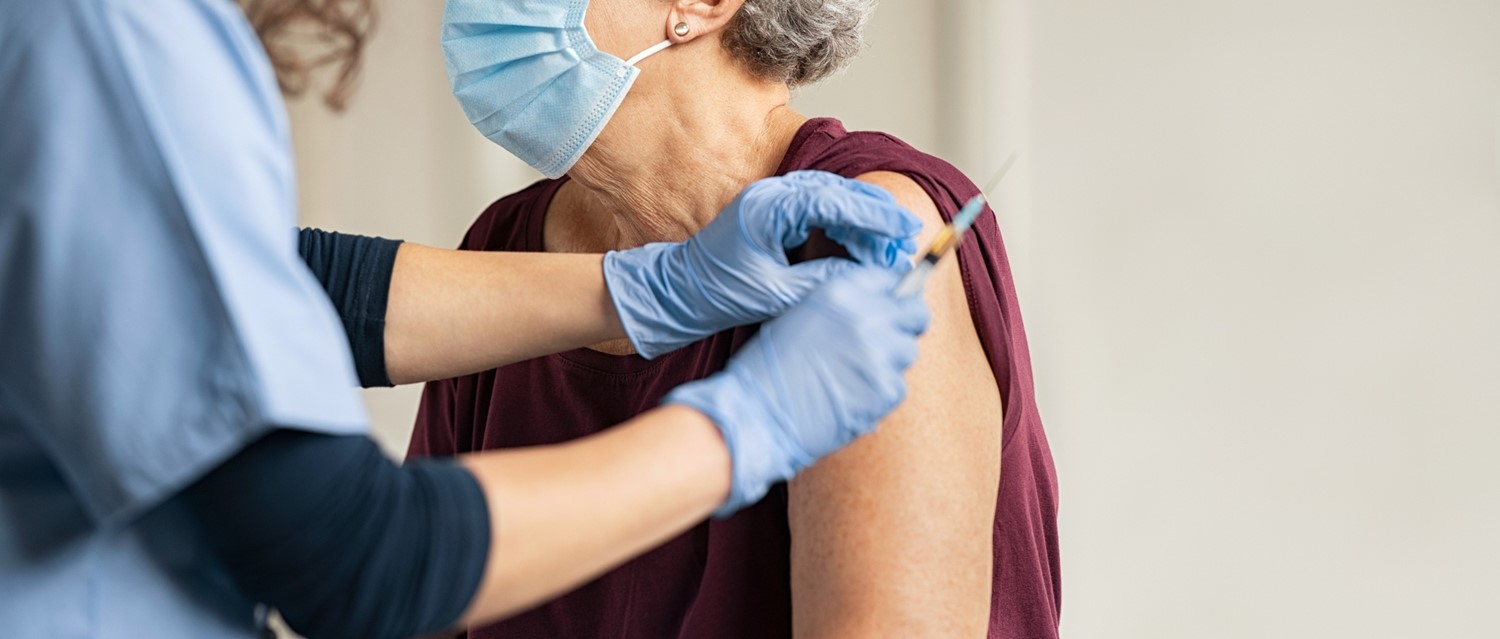
How is the vaccine administered?
Like most vaccines, the COVID-19 vaccine is delivered through injection into the arm. You may be vaccinated at a hospital, a dedicated vaccination site or a community vaccination site like your GP surgery or a pharmacy. Once the supply of vaccines is available, 24-hour vaccination sites may become available to ensure as many people as possible are being vaccinated every day.
Is it safe to extend the period between doses of the vaccine?
The initial dose should give 70-90% protection from COVID-19 within three weeks of the first dose. It's very important to remember that the vaccine takes time to take effect, so you should assume no protection for at least three weeks. Importantly, nobody who had one of the current vaccines in trials was ill enough to require hospital admission more than three weeks after their first dose.
While the initially studies for both the AstraZeneca and Pfizer vaccines involved two doses of vaccine three or four weeks apart, the JCVI, which regulates all vaccines in the UK, has reviewed the data in light of the huge number of COVID-19 cases, admissions and deaths the UK is experiencing.
They point to data for the AstraZeneca vaccine showing continued protection for study participants whose second vaccine was delayed; to data for the recently approved Moderna vaccine showing over 90% protection for up to three months; and to evidence from other vaccines showing a better immune response if the booster dose is given later.
In addition, giving the vaccines 12 rather than 3 weeks apart will allow twice as many people to be protected in the short term. As a result, all UK vaccines will now be offered up to 12 weeks apart. Following evidence of the immune response for the AstraZeneca vaccine being better with longer spacing, the World Health Organization has recommended that all AstraZeneca vaccines should be given 6-12 weeks apart.
New data from Public Health England on UK residents who have been vaccinated is extremely promising. It shows:
A single dose of Pfizer/BioNTech vaccine reduces hospitalisation and death by over 75%.
A single dose of Pfizer/BioNTech vaccine is 57% effective against catching symptomatic COVID-19 in over-80s, while two doses increases protection to more than 85%.
For the full protection offered by the vaccine you will still definitely need the second 'booster' dose no more than 12 weeks after your first dose. Your healthcare provider will inform you when your second dose will be administered.
I've been vaccinated, can I go out?
Like most vaccines, it is likely that those who have been vaccinated are less likely to pass on COVID-19 to others. However, as this is a new disease and vaccine, the data to back this up are limited at present (studies looking into this aspect are ongoing). Importantly, a study looking at people who have had COVID-19 infection has shown signs that they may still be able to carry and transmit the virus, even if they have antibodies.
To keep others safe and to prevent transmission of the virus, it is still essential to continue to follow measures set out by the Government.
What action should I take?
As GP surgeries and hospitals are now beginning to roll out the vaccine to the next most vulnerable groups, it is important that you don't contact them and overwhelm the service. You should be contacted when a vaccine becomes available for those in your risk category in your local area.
However, if you are not sure whether your GP has up-to-date contact details for you, it is worth checking and making sure you can be contacted when the time comes.
Continue reading below
About the authorView full bio

Dr Sarah Jarvis
SEO Executive
MA (Cantab), BM, BCh (Oxon), DRCOG, FRCGP, MBE
After training in medicine at Cambridge and Oxford, Dr Sarah Jarvis MBE became a GP.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is peer reviewed by qualified clinicians.
23 Feb 2021 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.