Treating recurring yeast infections
Vaginal thrush
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 31 Jul 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Vaginal dischargeVaginal thrushBacterial vaginosisPreventing and treating bacterial vaginosis
A recurring yeast infection (vaginal thrush) is defined as an episode of thrush four or more times in a year. In some cases, there is a medical reason that you are more prone to thrush infection. Some hormone treatments may also affect your risk of repeated episodes.
In this article:
Video picks for Vaginal and vulval problems
A vaginal yeast infection (vaginal thrush) is an extremely common cause of vaginal discharge - up to 3 in 4 women will have at least one episode during their lives. In most cases, thrush in women settles with simple treatment, either topical (applied to the vagina in the form of pessaries or antifungal creams) or oral (a tablet or tablets). However, some women either have repeated new infections, or find that they still have symptoms because the initial thrush treatment has not been effective.
Continue reading below
What causes recurring yeast infections?
Speculum examination showing vaginal thrush
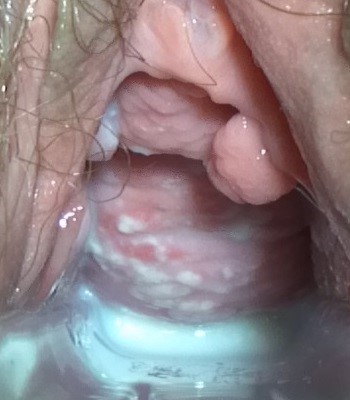
© Mikael Häggström, CC0, via Wikimedia Commons
Of women who develop a first bout of vaginal thrush, about 5 in 100 of them will get problems with recurring thrush. In most cases, the reason why this occurs is not known. Some women just seem more prone than usual to develop thrush. However women with high blood sugar (due to poorly controlled diabetes) and women with weakened immune systems may be more likely to develop recurrent thrush.
There is some debate as to whether women taking hormone replacement therapy (HRT) or birth control pills such as the combined oral contraceptive (COC) pill are more likely to develop a recurring yeast infection - the evidence is not yet clear.
How do I get rid of a recurring yeast infection?
Back to contentsIf you have repeated bouts of thrush then one option is simply to treat each bout as and when it occurs. See the separate leaflet Vaginal thrush (Yeast infection) for treatments for thrush.
Recurrent thrush is defined as 4 or more symptomatic episodes per year. If you have four or more episodes of vaginal thrush a year, with at least 2 episodes confirmed by a swab test, your doctor may suggest a different approach.
Before they do this, they may want to exclude another cause for your symptoms. This could include:
Taking a vaginal swab and sending it the laboratory to check for evidence of thrush or other infection.
Checking the pH (acidity level) in your vagina using a simple test strip. A lower pH (4.5 or below) makes it more likely that thrush is the cause. A higher pH (above 4.5) makes bacterial vaginosis (BV) or trichomonas infection (a sexually transmitted infection) more likely.
Other swabs or tests as appropriate.
Treatment for recurrent thrush
Using one of the usual treatments for vaginal thrush (topical treatments or tablets) - but for longer than usual. Your doctor will advise exactly how long to use the treatment for. Vaginal thrush can be treated with over the counter medicines, but as you need a longer course of treatment, your GP will give you a prescription for treatment if you need it.
How the recurring yeast infection is treated will also depend on your preferences and other factors such as whether you can tolerate the treatment, or have ever reacted badly to it, your age and whether you're pregnant (in which case vaginal pessaries will usually be advised). If you're 12-15 years old, or it's not clear whether your symptoms are due to recurrent vaginal thrush, your doctor may recommend a hospital specialist referral.
The first-line recommended 'induction treatment' is three doses of fluconazole 150 mg tablets (to be taken every 72 hours).
This is followed by regular 'maintenance treatment' to stop the thrush coming back, with once weekly tablets of fluconazole 150 mg for six months.
If you can't take fluconazole tablets for whatever reason, topical therapy (such as clotrimazole 500 mg vaginal pessary) can be used as induction treatment for 7-14 days, depending on how your symptoms respond. Maintenance treatment would then be a clotrimazole 500 mg vaginal pessary inserted once a week for six months or itraconazole tablets 50-100 mg once daily for six months.
Most women remain clear of thrush during maintenance treatment. If you and your doctor decide maintenance treatment is best for you, this will usually last for six months.
After treatment is stopped, many women remain free of thrush, or only develop the occasional bout again. However, some women return to developing recurring yeast infections. If this happens, the treatment plan can be repeated, and maintenance treatment continued for longer.
Regardless of the treatment you and your doctor agree, it's important to use lifestyle measures to reduce your risk of recurring yeast infections (you can find out more below). In addition, you should speak to your doctor if:
Your symptoms don't improve with treatment.
You develop thrush whilst on maintenance treatment. This may indicate that you have a resistant strain of Candida spp. which may require an alternative treatment.
You become pregnant or are breastfeeding.
You develop side-effects from the medication.
You develop new symptoms, such as smelly discharge, ulcers or blisters, abnormal vaginal bleeding or a bloodstained discharge.
You feel unwell in yourself.
Continue reading below
Can I prevent recurring yeast infections?
Back to contentsThe yeast that causes yeast infections, called Candida spp. such as Candida albicans, thrives in warm, moist, airless environments. General lifestyle changes that help prevent single episodes of vaginal thrush can also help reduce the risk of recurrent thrush.
If you have diabetes, your risk of recurring yeast infections is higher if your blood sugar is consistently high. Working with your diabetes team to bring your blood sugar under control can cut the risk of recurrent bouts of thrush.
If you experience recurring yeast infections, your doctor or nurse may also discuss your current method of contraception with you and suggest a change. There has been talk in the past about the combined oral contraceptive (COC) pill (the birth control pills that contain both oestrogen and progesterone hormones) possibly making recurrent vaginal thrush more likely. However, the evidence around this is a little unclear.
Patient picks for Vaginal and vulval problems

Women's health
Itchy vulva
Most women experience an itchy vulva and an itchy vagina from time to time. However, in pruritus vulvae, the itching is persistent and causes distress.
by Dr Rosalyn Adleman, MRCGP

Women's health
Vulvitis
Vulvitis is an inflammation of your vulva. It is not a disease or an actual condition. It is very common and can occur in women of all ages. It has many different causes, as listed below. It is sometimes difficult to determine the cause of the vulvitis.
by Dr Rachel Hudson, MRCGP
Further reading and references
- Candida - female genital: recurrent infection; NICE CKS, October 2023 (UK access only)
- Candida - female genital; NICE CKS, October 2023 (UK access only)
- Bacterial vaginosis; NICE CKS, July 2023 (UK access only)
- Vaginal discharge; NICE CKS, February 2024 (UK access only)
Continue reading below
About the author

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 30 Jul 2027
31 Jul 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.