Tear duct blockage in babies
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 11 Aug 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Tear duct blockage means that there is a blockage of the tiny channels (ducts) that drain tears from the inside corner of the eye into the side of nose. Many babies are born with blocked tear ducts. They usually open up without any treatment by the time they are one year old.
In this article:
Video picks for Baby and toddler
Continue reading below
What causes tear duct blockage in babies?
Many babies are born with a blocked tear duct. This happens when the tear ducts haven't fully developed and opened up yet. This can be due to:
A membrane (web of tissue) that hasn't yet broken down, and is blocking the tear duct.
A tear duct that is too narrow.
We don't know why this affects some babies and not others, although it's thought that some babies might inherit genetic variations that mean their tear ducts take a bit longer to fully develop.
It's also more likely to happen in babies who were born prematurely, and in babies with conditions that affect the shape of their face, such as Down's syndrome. But most babies with a blocked tear duct don't have any other health conditions.
Blocked tear ducts usually open after a bit more time for them to develop fully. For 9 out of 10 children, the tear duct opens up on its own by the time they are one year old.
Blocked tear ducts are common in babies and usually don't cause any serious problems. There are some rare complications to be aware of. See "When should you take your baby to see a doctor?" below for more.
In most babies, a blocked tear duct will simply get better with time, without causing any problems.
What are tear ducts for?
Back to contentsThe surface of the eye is kept moist by watery fluid (tears). This is really important to prevent any damage to the sensitive surface of the eye. The tears help to remove any dust or dirt from the surface of the eye. The tears are made in glands called the lacrimal glands, which are just above the outside corner of the eye, below the eyebrow.
Close-up view
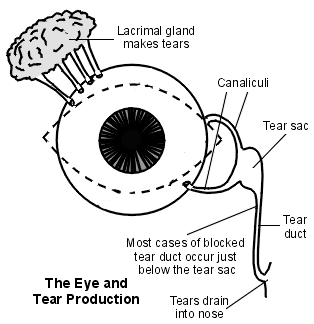
The lacrimal glands constantly make a small amount of tears which drains on to the eye.
When we blink, the eyelid spreads the tears all over the surface of the eye. Any excess tears drain out of the eye by passing through the small channels of the tear duct (nasolacrimal duct) and into the nose. (This is why your nose starts running if you are crying - the extra tears produced are going into your nose.)
There are also tiny glands (called meibomian glands) in the eyelids, which make a small amount of oily liquid. This oily liquid also helps to protect the surface of the eyes.
In babies with tear duct blockage, these tears don't drain into the nose properly. This means their tears back up in their eyes, and the can become more watery. The tears can also form a sticky discharge on, and around, the eyes.
Continue reading below
How common is tear duct blockage in babies?
Back to contentsBlockage of the tear duct is common in babies, occurring in up to 1 in 5 newborns. It is usually because the tear duct has not completely developed by the time of the birth. The blockage of the tear duct can affect just one eye or both eyes.
Abnormalities of the eye or the eyelids can also cause a blockage of the tears in babies but this is very rare.
What are the symptoms of a blocked tear duct?
Back to contentsTear duct blockage in babies can cause:
Watery eyes.
'Sticky eyes' - a white or yellowish discharge on the corner of the eyes, which might cause the eyelids to stick together.
Slight redness of the eyelids or eyes, if your child has been rubbing their eyes. (If the eye has become very red, it could be a sign of infection - see 'When should you take your baby to see a doctor?' below).
It may take until a week or two after birth before the tear glands (lacrimal glands) start to make tears. So, you may not notice your baby having watery eyes until they are a week or two old.
The symptoms are usually worse if your child has a cold, and can also be worse in cold weather.
You might notice that their eyes have a sticky discharge, particularly first thing in the morning. If their eye isn't red, this isn't due to an infection, but is just dried tear residue. It can be cleared away using clean water and cotton wool.
Continue reading below
Complications of a blocked tear duct in babies
Back to contentsMost babies with tear duct blockages don't get any other problems.
Rarely, it can cause other issues. These include:
The duct not opening up on its own. For most babies, the tear ducts simply open up as they grow, and should have opened in most babies by the time they are one year old. If they haven't opened by the time they are one, a small procedure to open up the tear ducts may be required.
Infection of the outer part of the eye (infective conjunctivitis). This causes the eye to look inflamed and red, and may also cause a sticky discharge. This is not usually serious and can be easily treated.
Infection of the tear sac (dacryocystitis). This is rare. This causes redness and swelling between the inner corner of the eye and the nose. It is often treated with antibiotics.
Infection of the skin and soft tissues around the eye (preseptal cellulitis). This causes the skin around the eye to become swollen, red, and inflamed. It's rare, and usually a mild infection, but can occasionally lead to a more serious infection (orbital cellulitis), so usually needs antibiotic treatment.
A collection of fluid in the tear duct (a dacryocoele). This causes a swelling, usually blueish, between the nose and the corner of the eye. This can go away on its own, but often needs a small procedure to get rid of it.
When should you take your baby to see a doctor?
Back to contentsIf your baby has a watery or sticky eye, you can usually treat it at home without seeing a doctor.
You should take your baby to see a doctor if:
Your baby's eye is inflamed, angry or red.
Your baby does not seem to want to open his or her eye, or light seems to hurt your baby's eye.
Your baby has swelling or redness between the inner corner of their eye and their nose.
Your baby has red or swollen skin around their eyes.
Your baby still has symptoms of a blocked tear duct when they are one year old, or older.
You are concerned or worried about your baby.
What treatment is there for a tear duct blockage?
Back to contentsIn most babies, their tear duct opens up fully as they grow. It often happens in the first few months but can take up to a year.
So, for most babies, no treatment is needed, because the problem will go away on its own with time.
Simple massage of the tear duct of your baby can help drain the tears. Use gentle pressure with your finger on the outside of your baby's nose and then stroke downwards towards the point of the nose. This should be repeated regularly (5-10 times) each day. This can help to clear the excess tears that have become blocked. It may also help the tear duct to develop.
If your baby's eye seems sticky or crusty then this can be gently wiped away using a soft damp cloth or cotton pad. Moisten the cloth or pad with sterile water (use boiled water that has then cooled down).
If complications happen then other treatment may be required. This can include antibiotics and sometimes surgical procedures.
After 12 months of age
In most babies, the tear duct blockage clears by the time they are 12 months old.
If it hasn't cleared by this time, it is less likely to clear up on its own. So, if the problem is still there when they are 12 months old, your baby may be referred to an eye specialist.
The specialist may recommend a procedure (tear duct probing) to open up the tear ducts. This is a simple and safe operation that is very effective. It is done using a general anaesthetic and children can usually go home later in the day after the operation.
Your baby might also be referred to a specialist earlier if the blocked tear duct has caused a complication, or if it's thought that they might have a rare condition affecting the tear drainage that needs different treatment.
Patient picks for Baby and toddler

Children's health
Erythema toxicum neonatorum
Erythema toxicum neonatorum (ETN) is a common skin rash affecting healthy newborn babies. It is not serious, does not cause the baby any harm and clears up without any treatment. It is sometimes known as erythema toxicum, baby acne or toxic erythema of the newborn.
by Dr Hayley Willacy, FRCGP

Children's health
Oral thrush in babies
Oral thrush is an infection in the mouth caused by a yeast fungus called candida. Oral thrush in babies is not usually serious and can generally be cleared with treatment.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Takahashi Y, Kakizaki H, Chan WO, et al; Management of congenital nasolacrimal duct obstruction. Acta Ophthalmol. 2009 Jul 21.
- Resolution of congenital nasolacrimal duct obstruction with nonsurgical management; Arch Ophthalmol. 2012 Jun;130(6):730-4. doi: 10.1001/archophthalmol.2012.454.
- Petris C, Liu D; Probing for congenital nasolacrimal duct obstruction. Cochrane Database Syst Rev. 2017 Jul 12;7:CD011109. doi: 10.1002/14651858.CD011109.pub2.
- Vagge A, Ferro Desideri L, Nucci P, et al; Congenital Nasolacrimal Duct Obstruction (CNLDO): A Review. Diseases. 2018 Oct 22;6(4). pii: diseases6040096. doi: 10.3390/diseases6040096.
- Avram E; Insights in the treatment of congenital nasolacrimal duct obstruction. Rom J Ophthalmol. 2017 Apr-Jun;61(2):101-106. doi: 10.22336/rjo.2017.19.
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 10 Aug 2025
11 Aug 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.