Dermatitis herpetiformis
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 29 Mar 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Coeliac diseaseGastrointestinal malabsorption
Dermatitis herpetiformis is a skin condition where you develop a very itchy rash. It is caused by intolerance to a food ingredient called gluten. It can be effectively treated with medication plus a gluten-free diet. Dermatitis herpetiformis is linked to a condition called coeliac disease, which is also caused by gluten intolerance. Treatment for both conditions is often needed.
In this article:
Video picks for Food allergy and intolerance
Continue reading below
What is dermatitis herpetiformis?
Dermatitis herpetiformis (DH) is a skin condition causing a very itchy rash. It is due to intolerance to gluten, which is a natural substance (a protein) found in certain foods. Gluten is in wheat, rye and barley. Gluten intolerance also causes a gut condition called coeliac disease, which is closely linked to DH.
What causes dermatitis herpetiformis?
Back to contentsThe cause of dermatitis herpetiformis is gluten intolerance. In this condition, your body reacts to gluten in food. Gluten intolerance is also sometimes called gluten sensitivity.
People with gluten intolerance have a kind of allergy to gluten, but it is not the same as a typical food allergy. With gluten intolerance, the gluten somehow triggers your body's immune system to react against the body's own organs.
This is instead of doing what the immune system normally does, which is to be a defence against infections, etc. This may lead to various symptoms in different parts of your body. With dermatitis herpetiformis, it is your skin which is affected.
It is not known exactly what causes the gluten intolerance in the first place.
Does dermatitis herpetiformis always mean you have coeliac disease?
Gluten intolerance also usually causes inflammation in the gut (in the small intestine). When this happens it is called coeliac disease. Most people with dermatitis herpetiformis have some degree of coeliac disease. However, they may not have had any noticeable symptoms and their coeliac disease may not have been diagnosed. See the separate leaflet called Coeliac Disease for more details.
The rest of this leaflet deals with dermatitis herpetiformis.
Continue reading below
How common is dermatitis herpetiformis?
Back to contentsAround 1 in 10,000 people have dermatitis herpetiformis. About 1 in 8 people with coeliac disease will have DH.
Dermatitis herpetiformis is more common in men than in women and usually starts between ages 30-50 years, although it can occur at any age.
What are the symptoms of dermatitis herpetiformis?
Back to contentsThere is an extremely itchy rash. It can affect any part of your skin, but is usually on your elbows, knees, buttocks and scalp. The rash is usually on both sides of your body at the same time (symmetrical). The rash has blisters and/or raised spots (papules) - but the blisters usually get scratched off to leave scabs. There may be burning or stinging on the area before the blisters start.
The rash can vary from week to week but does not usually clear up without treatment.
Dermatitis herpetiformis rash
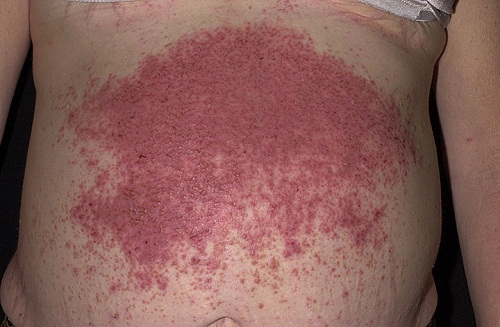
© Madhero88, CC BY-SA 3.0, via Wikimedia Commons
You may also have symptoms of coeliac disease, such as tummy (abdominal) symptoms or unexplained tiredness. However, some people with coeliac disease have little in the way of symptoms, and dermatitis herpetiformis may be the first sign of coeliac disease.
Continue reading below
How is dermatitis herpetiformis diagnosed?
Back to contentsThere are various skin conditions that cause itchy rashes with blisters, so a test is needed to diagnose dermatitis herpetiformis for certain. The test is a a skin biopsy. This involves taking a small sample of skin under local anaesthetic. The sample is examined under the microscope in a laboratory, using a special test to look for antibodies called IgA. This test can reliably diagnose DH.
If dermatitis herpetiformis is suspected, you will usually be offered tests for coeliac disease as well. Blood tests can help to show if coeliac disease is likely. If the blood tests are positive, you may be offered a test on the gut (a biopsy to sample the lining of your bowel), which can confirm if you have coeliac disease.
How is dermatitis herpetiformis treated?
Back to contentsThere are two treatments for dermatitis herpetiformis:
Diet.
Medication.
Diet
In the long term, a diet free of gluten will gradually reduce the dermatitis herpetiformis symptoms and may cure DH completely. (This diet also treats coeliac disease.) However, it can take months or years for the diet to improve DH. Therefore, medication is often needed to bring the skin symptoms under control. See the separate leaflet called Coeliac Disease Diet Sheet for more information about the gluten-free diet. In the UK more information is also available from Coeliac UK - see under 'Further Reading and References', below.
Medication
Medication helps control the rash quickly. The usual medication for dermatitis herpetiformis is dapsone. Dapsone often stops the itching within two days. Dapsone may have side-effects, including anaemia. Therefore, regular check-ups and blood tests are needed while you are taking it.
Dapsone is used to treat certain skin conditions, including DH. Exactly how it works is not known. However, it seems to have anti-inflammatory and antibacterial actions. In dermatitis herpetiformis, it is probably the anti-inflammatory action that is helpful.
If you cannot take dapsone or you have side-effects from it, other alternative medicines are available - for example, sulfasalazine or sulfapyridine.
Are there any possible complications?
Back to contentsDermatitis herpetiformis itself does not usually cause complications. However, the gluten intolerance and coeliac disease, if untreated, may make you ill and have possible complications. Most of these problems can be prevented or treated by following a gluten-free diet, which treats both dermatitis herpetiformis and coeliac disease.
What is the prognosis?
Back to contentsUntreated, dermatitis herpetiformis tends to go up and down in severity, but usually continues.
With treatment, the outlook (prognosis) is very good, as dermatitis herpetiformis clears up with medication and a gluten-free diet. Dapsone usually improves the rash quickly. The gluten-free diet takes longer to help - it may take a year or more to get the full benefit. About 8 in 10 people with dermatitis herpetiformis have good results from the diet so they can either stop taking dapsone, or can reduce the dose.
Patient picks for Food allergy and intolerance

Allergies, blood and immune system
Nut allergy
Nuts and peanuts can cause allergic reactions, which are sometimes severe. A severe reaction to nuts is called anaphylaxis and can be life-threatening. Symptoms often start quickly, within an hour of coming into contact with a nut, and sometimes within minutes. If you have a nut allergy, avoiding foods that contain nuts will prevent an allergic reaction. But, if you do come into contact with nuts, and a reaction starts then treating it quickly is important. If you have a severe allergic reaction, if available, give yourself an adrenaline (epinephrine) injection straightaway and call an ambulance. If you are well prepared and take action quickly the risk of having any serious problems is small.
by Dr Hayley Willacy, FRCGP

Allergies, blood and immune system
Oral allergy syndrome
Oral allergy syndrome causes symptoms around the mouth that are triggered by certain foods. It is associated with other conditions caused by plant allergies, such as hay fever and allergy to birch pollen. It's also called pollen-food syndrome, or pollen-food allergy.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Coeliac UK
- Reunala T, Hervonen K, Salmi T; Dermatitis Herpetiformis: An Update on Diagnosis and Management. Am J Clin Dermatol. 2021 May;22(3):329-338. doi: 10.1007/s40257-020-00584-2.
- Mirza HA, Gharbi A, Bhutta BS; Dermatitis Herpetiformis.
Continue reading below
About the authorView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 27 Mar 2028
29 Mar 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.