Breast lumps and breast examination
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 17 Jun 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Breast lumps article more useful, or one of our other health articles.
In this article:
The detection of a lump in the breast causes understandable fear of a cancer diagnosis.
Careful examination will increase the chance of correct diagnosis.
Examination alone leads to about half the number of breast cancer diagnoses compared with mammography and examination in screening.1 Where women present with a breast lump, clinical examination is found to have a high sensitivity and specificity when diagnosing a malignancy.2
Regardless of examination findings, women over 30 with breast lumps should always be referred to a breast clinic for further imaging.3
History
Organised screening, education programmes and improved consciousness of the female population mean that breast cancer tends to be found earlier than in the past. Occasionally, patients (usually elderly but not always) will still present with a fungating mass that has obviously been neglected for a long time.
Patients presenting with a lump in the breast will be aware of the possible diagnosis and may be anxious. This should be taken into account when taking the history and discussing management.
Direct questions should include the following:
When was the lump first noticed?
Has it changed in size or in any other way? This includes a nipple becoming inverted.
Is there any discharge from the nipple?
Menstrual history. If she is premenopausal, when was her last menstrual period?
Any changes noted through the menstrual cycle?
Family history (including breast cancer, other cancers and other conditions).
Questions relating to the risk factors listed above.
Examination
In line with good practice and GMC guidance, explain to the patient what you intend to do and why. 4 Obtain consent for the examination and document this. Offer a chaperone and document the discussion.5
In the past, advice has been to use the examination to teach the patient self-examination. There is no evidence it reduces mortality and it can increase anxiety when women present with benign lumps. However recent studies suggest that the majority of women with breast cancer present after a self-examination and therefore it may be beneficial.6It is likely that regular self-examination is not necessary.
Breast inspection
Inspect with the patient sitting and then with their hands raised above head.
A lump may be visible.
Look for:
Variations in breast size and contour.
Whether there is an inverted nipple (nipple retraction) and, if so, is it unilateral or bilateral?
Any oedema (may be slight).
Redness or retraction of the skin.
Dimpling of the skin (called peau d'orange and is like orange peel because of oedema of the skin. This has sinister significance as it is caused by lymphatic invasion, and therefore is due to an invasive underlying tumour, or an inflammatory breast cancer).
The next stage is palpation, and a systematic search pattern improves the rate of detection.
Technique for palpation of the breast
There is no proven "best method" to examine the breast. Different people have different techniques and the following description is not the only approach. Gloves are generally thought to make breast examinations less reliable.7
Ask the patient to lie supine with their hands above their head. Examine from the clavicle medially to the mid-sternum, laterally to the mid-axillary line and to the inferior portion of the breast. Remember the axillary tail of breast tissue. Examine the axilla for palpable lymphadenopathy.
Examine with the hand flat to avoid pinching up tissue. Use the pads or palmar surfaces of the second, third and fourth fingers held together and moved in small circles.
Some advise beginning with light pressure and then repeating in the same area using medium and deep pressure before moving to the next section.
Three search patterns are generally used:
Radial spoke method (wedges of tissue examined starting at the periphery and working in towards the nipple in a radial pattern).
Concentric circle method, examining in expanding or contracting concentric circles.
Vertical strip method, which examines the breast in overlapping vertical strips moving across the chest.
If you have difficulty finding a discrete lump, ask the patient to demonstrate it for you.
A discrete mass should be described in terms of location, size, mobility and texture. Mobility includes whether attached to skin or underlying tissue.
Examine both breasts.
Support the patient's arm to palpate axillary nodes and then feel for supraclavicular and cervical nodes. Note the presence or absence of palpable regional nodes.
If there is a history of discharge from the nipple it is often easier to get the patient to demonstrate the discharge (rather than the doctor attempting to do so). If there is no such history, it is inappropriate to attempt to demonstrate a discharge.
It is also worth noting:
Breast examination should be thorough.
It can be taught using silicone models.
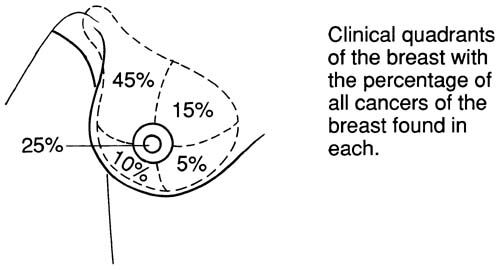
The diagram of frequency of malignancy by site in the breast:
Diagram of breast sections
If a lump is found, note size, consistency and whether it is attached to skin or underlying tissue.
Clinical features of palpable breast masses
Malignant breast masses | Benign breast masses |
Consistency: hard | Consistency: firm or rubbery |
Painless (90%) | Often painful (consistent with benign breast conditions) |
Irregular margins | Regular or smooth margins |
Fixation to skin or chest wall | Mobile and not fixed |
Skin dimpling may occur | Skin dimpling unlikely |
Discharge: bloody, unilateral | Discharge: no blood and bilateral discharge. Green or yellow colour |
Nipple retraction may be present | No nipple retraction |
Continue reading below
Appropriate referral3
The importance of minimising delay is consistently reported by patients in surveys to be very important and is recognised by professionals. GPs are advised by the National Institute for Health and Care Excellence (NICE) to convey optimism about the effectiveness of treatment and survival when referring people with suspected breast cancer.
The majority of palpable breast lumps are not breast cancer.
NICE guidance8
Refer people, using a suspected cancer pathway referral, for breast cancer, if they are:
Aged 30 and over and have a breast lump with or without pain.
Aged 50 and over with any of the following symptoms in one nipple only:
Discharge.
Retraction.
Other changes of concern.
Consider a suspected cancer pathway referral (for an appointment within two weeks) for breast cancer in people:
With skin changes that suggest breast cancer.
Aged 30 and over with an unexplained lump in the axilla.
Consider non-urgent referral in people aged under 30 with an unexplained breast lump with or without pain.
Investigations
Back to contentsIt is recommended that investigation prior to referral is not appropriate. Once seen in the breast clinic, investigation usually involves mammography and/or ultrasound, with biopsy if appropriate. For further details of investigation and diagnostic procedures, see the separate Breast cancer article.
Continue reading below
Breast cancer
Back to contentsEpidemiology
Breast cancer is the most common cancer in the UK, accounting for 15% of all new cancer cases (2021).9 In females in the UK, breast cancer is the most common cancer (30% of all new female cancer cases). 99% of breast cancer cases in the UK are in females, and 1% are in males.
Age-standardised rates for White females with breast cancer range from 122.4 to 125.7 per 100,000. Rates for Asian females are significantly lower, ranging from 59.7 to 92.3 per 100,000, and the rates for Black females are also significantly lower, ranging from 68.8 to 107.9 per 100,000.
In the UK, the lifetime risk for developing breast cancer is 14%. The incidence is strongly associated with age, with 24% of all new cases annually being in women over 75 years.9
Risk factors for malignancy10 11
Previous history of breast cancer.
Family history of breast cancer in a first-degree relative carries a 2-3 fold excess risk. A number of genetic mutations are implicated. The BRCA1, BRCA2 and TP53 mutations carry very high risk but only around 5-10% of women with breast cancer are shown to have a genetic cause. This increases to around 25% in women developing breast cancer under the age of 30.12
Age. In Europe, ≤5% of cases present before the age of 35, ≤25% before the age of 50. 24% occur in women over the age of 75.13 12
High lifetime exposure to oestrogen including: early menarche (under the age of 12), late menopause (over the age of 50), nulliparity or having a first child after the age of 30, not having breastfed.
Use of hormones - all hormonal contraceptives increase the risk of breast cancer, albeit by a relatively small percentage. This increase is higher in women over the age of 30 than those below the age of 30.14 HRT containing progesterone is known to increase breast cancer risks significantly over oestrogen-only HRT. However the use of Mirena or micronised progesterone has a much lower increased risk than oral synthetic progestagens.15
Radiation to chest (even quite small doses).
Obesity.
High alcohol intake - may increase risk in a dose-related manner.16
Breastfeeding and physical activity may reduce risk.
Breast augmentation is not generally associated with increased risk. There are also concerns that implants may slow detection and therefore adversely affect survival.17There are some specific cancers which can occur as a result of breast implants - these breast implant associated (BIA) malignancies include anaplastic large cell lymphoma and squamous cell carcinoma. Although very rare, BIA-SCC is a serious condition with a high mortality rate.18
Presentation
Presenting symptoms of breast cancer:
Breast lump. Most patients present having felt a lump - usually painless but may be painful in some.
Nipple change - for example, inversion, change in shape or a scaling rash.
Nipple discharge.
Bloodstained discharge from nipple - intraduct carcinoma may present in this way.
Skin contour changes.
Axillary lumps - lymph nodes.
Symptoms of metastatic disease - bone pains/fractures, symptoms of lung, liver or brain metastases. (Unusual at presentation.)
Asymptomatic but picked up at routine mammography screen.
Further reading and references
- Suspected cancer; NICE Quality standard, June 2016 - last updated December 2017)
- Veitch D, Goossens R, Owen H, et al; Evaluation of conventional training in Clinical Breast Examination (CBE). Work. 2019;62(4):647-656. doi: 10.3233/WOR-192899.
- Effectiveness of clinical breast examination as a ‘stand-alone’ screening modality: an overview of systematic reviews; T TNgan et al
- Ravi C, Rodrigues G; Accuracy of clinical examination of breast lumps in detecting malignancy: a retrospective study. Indian J Surg Oncol. 2012 Jun;3(2):154-7. doi: 10.1007/s13193-012-0151-5. Epub 2012 May 22.
- Breast cancer - recognition and referral; NICE CKS April 2025 (UK access only)
- Good medical practice; General Medical Council (GMC). 2024.
- Intimate examinations and chaperones; GMC
- Huang N, Chen L, He J, et al; The Efficacy of Clinical Breast Exams and Breast Self-Exams in Detecting Malignancy or Positive Ultrasound Findings. Cureus. 2022 Feb 21;14(2):e22464. doi: 10.7759/cureus.22464. eCollection 2022 Feb.
- The Breast Exam
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated April 2026)
- Breast cancer - managing FH; NICE CKS, December 2018 (UK access only).
- Familial breast cancer: classification, care and managing breast cancer and related risks in people with a family history of breast cancer; NICE Clinical Guideline (June 2013 - last updated November 2023).
- Breast cancer - managing FH: Summary; NICE CKS, March 2024 (UK access only)
- Menon G, Alkabban FM, Ferguson T; Breast Cancer.
- Primary breast cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up; ESMO (2015)
- Combined and progestagen-only hormonal contraceptives and breast cancer risk: A UK nested case–control study and meta-analysis; D Fitzpatrick et al
- Risk of breast cancer with HRT depends on therapy type and duration; BMJ
- Miller ER, Wilson C, Chapman J, et al; Connecting the dots between breast cancer, obesity and alcohol consumption in middle-aged women: ecological and case control studies. BMC Public Health. 2018 Apr 6;18(1):460. doi: 10.1186/s12889-018-5357-1.
- Sonden ECB, Sebuodegard S, Korvald C, et al; Cosmetic breast implants and breast cancer. Tidsskr Nor Laegeforen. 2020 Feb 24;140(3). pii: 19-0266. doi: 10.4045/tidsskr.19.0266. Print 2020 Feb 25.
- Niraula S, Katel A, Barua A, et al; A Systematic Review of Breast Implant-Associated Squamous Cell Carcinoma. Cancers (Basel). 2023 Sep 12;15(18):4516. doi: 10.3390/cancers15184516.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Jun 2028
17 Jun 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free