Toe and finger clubbing
Peer reviewed by Dr Laurence KnottLast updated by Dr Colin Tidy, MRCGPLast updated 18 Feb 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: Hippocratic nails, Hippocratic fingers (first described by Hippocrates)
Continue reading below
What is toe and finger clubbing?
Toe and finger clubbing is described an increase in the soft tissue around the end of the fingers and toes. The swelling is painless and usually bilateral, unless a localised vascular abnormality exists. There is no change to the underlying bone. The nail base eventually becomes convex and extends halfway up the nail.
Clubbing is thought to result from changes to the volume of interstitial fluid and increased blood flow to the area but the exact pathophysiology remains unknown.
Primary toe and finger clubbing may be idiopathic or be a feature of an inherited condition. Secondary clubbing may be caused by a wide range of diseases.
Aetiology1
Back to contentsPrimary
Primary hypertrophic osteoarthropathy2 . Familial clubbing. | Pulmonary disease Interstitial lung disease. Idiopathic pulmonary fibrosis. Lipoid pneumonia. Empyema. Pulmonary artery sarcoma. Cryptogenic fibrosing alveolitis. Pulmonary metastases. | Cardiac disease Cyanotic congenital heart disease. Other causes of right-to-left shunting. |
Gastrointestinal disease Primary biliary cirrhosis. Leiomyoma of the oesophagus. Peptic ulceration of the oesophagus. | Skin disease
Bureau-Barrière-Thomas syndrome (digital clubbing associated with palmoplantar keratoderma). Fischer's syndrome (keratosis palmaris et plantaris, hair hypoplasia, onycholysis and onychogryphosis). Palmoplantar keratoderma (diffuse patches on the palms and soles). | Malignancies Thymus cancer. Disseminated chronic myeloid leukaemia (POEMS syndrome - polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy and skin changes). |
Miscellaneous conditions Thyroid acropachy (clubbing associated with Graves' disease and periosteal new bone formation). Pregnancy. |
Continue reading below
Epidemiology
Back to contentsThe epidemiology of secondary toe and finger clubbing depends on the cause. One review found3 :
In adults, the pooled prevalence of digital clubbing was 33.4% in people with intestinal diseases, 31.3% for interstitial lung diseases, 27% for infective endocarditis, and 22.8% for hepatic diseases.
In children and adolescents, the pooled prevalence of digital clubbing was 29.1% for HIV infection, 23% for haemoglobinopathies, 19.5% for cystic fibrosis and 17.1% for tuberculosis.
The pooled prevalence of hypertrophic osteoarthropathy was 10.1% in adults with cancers, and 5% in children and adolescents with cystic fibrosis.
Pachydermoperiostosis is rare and is characterised by skin thickening of the forehead, eyelids and hands, digital clubbing and periostosis4 .
Toe and finger clubbing symptoms
Back to contentsFinger clubbing
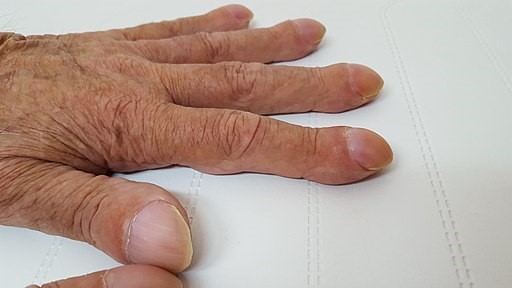
© Wesalius, CC BY-SA 4.0, via Wikimedia Commons
The patient may notice a swelling of the distal portion of the fingers or toes but the onset is usually so gradual as to make this a rare occurrence. Even more rarely, the patient may notice some discomfort, because most toe and finger clubbing is painless. The majority of clubbing is detected by doctors as part of a routine examination for other presenting symptoms.
Toe and finger clubbing has been described as a bulbous fusiform enlargement of the distal portion of a digit. It is commonly bilateral but may be unilateral and can affect a single digit. Both fingers and toes can be affected.
As toe or finger clubbing progresses, the angle between the nail and the nail base (called the Lovibond angle) becomes obliterated. Normally, the angle is less than or equal to 160°. With increasing convexity of the nail, the angle becomes greater than 180°. In early clubbing, the nail may feel springy instead of firm when palpated and the skin at the base of the nail may become smooth and shiny.
In individuals without finger clubbing, if two opposing fingers are placed together, a diamond-shaped window will appear. In clubbing, this window is obliterated and the distal angle formed by the two nails becomes wider. This is known as Schamroth's window test.
Continue reading below
Differential diagnosis
Back to contentsPseudo-clubbing - this is overcurvature of the nails in both the longitudinal and transverse axes, with preservation of a normal Lovibond angle5 . The main features of pseudo-clubbing seen in one study were asymmetrical finger involvement and acro-osteolysis. Whilst these were present in the majority of cases they were also present in some cases of clubbing, so could not be said to be pathognomonic. Pseudo-clubbing may be seen in chronic kidney disease, hyperparathyroidism, sarcoidosis, scleroderma, subungual haematoma and chromosome deletion6 .
Investigations
Back to contentsLaboratory investigations
These will depend on the underlying conditions suggested by the overall clinical picture.
Imaging
This is not usually required to diagnose toe or finger clubbing but plain radiographs of the digits may help to elucidate the cause. Osteolysis is often seen in patients with congenital cyanotic heart disease, whilst bone hypertrophy suggests a pulmonary condition.
Other modalities sometimes employed in clinical and research settings include technetium-99m scanning to assess bone loss, thermography and positron emission tomography (PET) scanning.
CT and MRI scanning of other areas may be required to assist in diagnosing the underlying primary cause.
Toe and finger clubbing treatment and management
Back to contentsThis will be dictated by the underlying disease process.
Prognosis
Back to contentsToe and finger clubbing is potentially reversible if the underlying condition is treated early enough but the changes may be irreversible once collagen deposition has set in.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Seifert W, Kuhnisch J, Tuysuz B, et al; Mutations in the prostaglandin transporter encoding gene SLCO2A1 cause primary hypertrophic osteoarthropathy and isolated digital clubbing. Hum Mutat. 2012 Apr;33(4):660-4. doi: 10.1002/humu.22042. Epub 2012 Feb 24.
- Mukherjee A, Bhattacharyya P, Saha I, et al; Evaluation of a simple bedside tool developed to measure different parameters of clubbing. Lung India. 2011 Jul;28(3):228-9.
- Clubbing; DermNet NZ
- Spicknall KE, Zirwas MJ, English JC 3rd; Clubbing: an update on diagnosis, differential diagnosis, pathophysiology, and clinical relevance. J Am Acad Dermatol. 2005 Jun;52(6):1020-8.
- Shakya P, Pokhrel KN, Mlunde LB, et al; Effectiveness of non-steroidal anti-inflammatory drugs among patients with primary hypertrophic osteoarthropathy: A systematic review. J Dermatol Sci. 2018 Apr;90(1):21-26. doi: 10.1016/j.jdermsci.2017.12.012. Epub 2017 Dec 28.
- Essouma M, Nkeck JR, Agbor VN, et al; Epidemiology of Digital Clubbing and Hypertrophic Osteoarthropathy: A Systematic Review and Meta-analysis. J Clin Rheumatol. 2022 Jan 21. pii: 00124743-900000000-98290. doi: 10.1097/RHU.0000000000001830.
- Madruga Dias JA, Rosa RS, Perpetuo I, et al; Pachydermoperiostosis in an African patient caused by a Chinese/Japanese SLCO2A1 mutation-case report and review of literature. Semin Arthritis Rheum. 2014 Feb;43(4):566-9. doi: 10.1016/j.semarthrit.2013.07.015. Epub 2013 Sep 5.
- Farzaneh-Far A; Images in clinical medicine. Pseudoclubbing. N Engl J Med. 2006 Apr 13;354(15):e14.
- Santiago MB, Lima I, Feitosa AC, et al; Pseudoclubbing: Is It Different from Clubbing? Semin Arthritis Rheum. 2008 Mar 29.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Laurence Knott
General Practitioner, Medical Author
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Feb 2027
18 Feb 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free