Dacryocystitis and canaliculitis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 6 Mar 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Watering eyes article more useful, or one of our other health articles.
In this article:
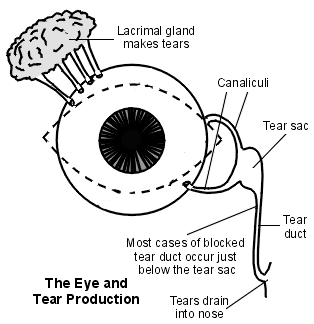
The lacrimal drainage system consists of the puncta - upper and lower within the eyelids and which are the opening to the upper and lower canaliculus. These meet at the common canaliculus and open into the lacrimal (tear) sac. This runs parallel to the nose and is separated from the middle meatus of the nasal cavity by two thin plates of bone. It continues down to become the nasolacrimal duct (tear duct) which opens out into the inferior nasal meatus.
Close-up view
Continue reading below
What is dacryocystitis?1
Dacryocystitis is an inflammation of the lacrimal sac, often as a result of infection. It may be acute or chronic. For anatomical reasons, it occurs more frequently on the left side. An ocular origin for inflammation of the lacrimal system is less common than a nasal origin.
Rarely, congenital dacryocystocele can occur as part of the picture of nasolacrimal duct obstruction. The incidence of congenital dacryocystocele varies from 1% to 12%.2 This is a serious condition because the orbital septum is poorly formed in infants and there is a significant risk of spread (orbital cellulitis and its complications).3
How common is dacryocystitis? (Epidemiology)4
Back to contentsIt is more common in females. It tends to occur either in infants (uncommon) or in adults (much more common) over the age of 40 years, peak age 60-70 years.
Continue reading below
Symptoms of dacryocystitis
Back to contentsAcute dacryocystitis5
Symptoms and signs are over the region of the lacrimal sac (but may spread to the nose and face with teeth pain being experienced by some). Therefore, look just lateral and below the bridge of the nose for:
Excess tears (epiphora) - almost invariably.
Pain.
Redness.
Swelling.
The patient may complain of decreased visual acuity owing to the excess tears and an abnormal tear composition.4
Examination will reveal a tender, tense, red swelling (± preseptal cellulitis in severe cases). Mucopurulent discharge can be expressed from the punctum. There may be a fever and an elevated leukocyte count too.
Chronic dacryocystitis6
This may present with a history of chronic or recurring epiphora and may have persistent redness of the medial canthus. There may be a painless or recurring swelling over the lacrimal sac, and pressure over this will result in reflux of mucopurulent material through the lower punctum.
Differential diagnosis
Orbital or facial cellulitis (discharge cannot be expressed from the punctum).
Acute ethmoid or frontal sinusitis.
Dacryocystocele (mild enlargement of a non-inflamed lacrimal sac in an infant).
Investigations7
In severe or atypical cases (for example, non-responsive to antibiotics), culture the expressed contents of the sac.
CT scan of the orbit and the paranasal sinuses can be useful.
A dacryocystography (DCG) may be performed where structural abnormalities are suspected.
Associated diseases
This is most commonly associated with nasolacrimal duct obstruction which results in stasis of the lacrimal sac contents. Less commonly, it is associated with anatomical abnormalities of the lacrimal sac or with nasal or sinus surgery. Nasal disease may be found in a number of these patients - for example, various forms of rhinitis, trauma or the presence of a foreign body. Some common systemic diseases associated with chronic dacryocystitis include granulomatosis with polyangiitis, sarcoidosis, and systemic lupus erythematosus. Rarely, there may be a lacrimal sac tumour.
Treatment for dacryocystitis
Back to contentsAcute dacryocystitis management5
Patients tend to be managed on an outpatient basis unless they are systemically unwell.
Initially, treatment of acute dacryocystitis is with oral antibiotics and analgesia. Empiric antibiotics should include Gram-positive and Gram-negative coverage.4
The regime is guided by clinical response but, typically, a 10- to 14-day course is required.
Incision and drainage may be considered if the infection extends outside the sac and a superficial skin abscess is formed. This carries the risk of forming a fistula, resulting in tears draining directly to the skin surface.8 However, a study found that early surgery produced faster resolution of the condition than surgery which was deferred until the infection had been treated conservatively.9
Chronic dacryocystitis management 710 11
Non-surgical treatment involves warm compresses, massage and probing of the nasolacrimal duct.
Probing involves inserting a fine metal probe via the punctum and canalicular system and passing it into the nasolacrimal sac, past the obstruction. This can often be done without a general anaesthetic. If there is acute infection, the procedure is usually deferred for a few days, until antibiotics have taken effect.12
If this is not effective, surgical treatment is a DCR (see box below).
Balloon dacryoplasty, nasolacrimal intubation and nasolacrimal stenting have all been attempted with varying degrees of success.4
Congenital dacryocystocele management13
One study reported that conservative management, involving gentle massage over the lacrimal sac, warm compresses ± topical and systemic antibiotics, was effective in all cases.
Probing and irrigation may resolve the obstruction.
Be aware that serious infection can develop rapidly.
See also the separate Congenital nasolacrimal duct obstruction article.
Important information |
|---|
DCR |
Complications4
These lie mainly in the risk of spread which can be superficial (for example, cellulitis), deep (for example, orbital cellulitis, orbital abscess, meningitis) or generalised (for example, sepsis).15 These complications are rare and tend to be seen in the immunocompromised individuals and in cases of congenital dacryocystitis.
Intraocular surgery - such as cataract surgery - should be postponed until the dacrocystitis (whether acute or chronic) has been treated, as there is a significant risk of ensuing endophthalmitis. However, there are complications associated with DCR too:
Failed procedure.
Cutaneous scarring.
Epistaxis.
Cellulitis.
Cerebrospinal fluid rhinorrhoea (if the subarachnoid space is inadvertently entered).
Prognosis
This is good if managed promptly and surgery is not delayed once the acute phase has resolved. However, congenital dacryocystitis can be very serious and is associated with significant morbidity and mortality if not treated promptly and aggressively.
Continue reading below
What is chronic canaliculitis?16
Back to contentsThis is an uncommon condition where the canaliculi become chronically infected. Common pathogens reported are Staphylococcus spp., Streptococcus spp., Actinomyces spp. and Propionibacterium spp..17
Symptoms of chronic canaliculitis
Unilateral epiphora.
Chronic mucopurulent conjunctivitis (refractory to usual treatment).
Signs
Oedema of the canaliculus: look for a swelling at the medial end of the upper or the lower lid.
'Pouting' punctum: this is turned out and is prominent.
Gentle compression of the canaliculi results in expression of concretions: solid, pale-yellow fatty material.
Investigation
High-resolution ultrasound biomicroscopy may be helpful.18
Differential diagnosis
Dacryocystitis.
Nasolacrimal duct obstruction.
Treatment for chronic canaliculitis 19
Removal of the obstruction concretions (by expressing them through the punctum) and topical antibiotics (for example, ciprofloxacin qds for 10 days) may be effective in some cases.
Surgery (canaliculectomy or punctoplasty) is often performed, often with expression of concretions from the duct and irrigation with antibiotics or an iodine solution. Occasionally, more extensive surgery is needed.
One study suggested that intracanalicular antibiotics can be helpful as an alternative to surgery.
What is canalicular obstruction?20 21
Back to contentsObstruction of the lacrimal canaliculi may be congenital (see the separate Congenital nasolacrimal duct obstruction article) or acquired. Acquired causes include trauma, scarring, inflammatory conditions, local tumours, Bell's palsy, radiotherapy and certain drugs - for example, docetaxel.
Presenting features are excess tearing ± sticky discharge and irritation.
Investigations
Syringing and probing to identify the site of obstruction.
The Jones' fluorescein dye test.
Treatment of canalicular obstruction
Treat infection if present.
Syringing and probing may be used but they risk trauma to the duct and may aggravate the condition.
Surgical treatment - there are various treatment methods, including punctoplasty, insertion of a silicone tube, trephination, balloon canaliculoplasty, endocanalicular laser surgery, conjunctivodacryocystorhinostomy (CDCR) and canalicodacryocystorhinostomy (canaliculo-DCR).22 Laser or balloon canaliculoplasty may be well tolerated and a good alternative to CDCR23
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Lopez Montes T, Gurnani B, Stokkermans TJ; Assessment of the Watery Eye.
- Zaveri J, Cohen AJ; Lacrimal canaliculitis. Saudi J Ophthalmol. 2014 Jan;28(1):3-5. doi: 10.1016/j.sjopt.2013.11.003. Epub 2013 Nov 13.
- Dacryocystitis (acute) - clinical management guidelines; College of Optometrists, March 2024
- Pujari A; Congenital dacryocystocele. BMJ Case Rep. 2016 Dec 9;2016. pii: bcr-2016-218029. doi: 10.1136/bcr-2016-218029.
- Cavazza S, Laffi GL, Lodi L, et al; Congenital dacryocystocele: diagnosis and treatment. Acta Otorhinolaryngol Ital. 2008 Dec;28(6):298-301.
- Taylor RS, Ashurst JV; Dacryocystitis
- Bakshi SS; Acute dacryocystitis. Cleve Clin J Med. 2020 Jul 31;87(8):477. doi: 10.3949/ccjm.87a.19121.
- Dacryocystitis (chronic) - clinical management guidelines; College of Optometrists, March 2024
- Huo Y, Li L, Mo Y, et al; A case report of chronic dacryocystitis caused by nasal stones. BMC Ophthalmol. 2023 Nov 6;23(1):445. doi: 10.1186/s12886-023-03185-9.
- Barrett RV, Meyer DR; Acquired lacrimal sac fistula after incision and drainage for dacryocystitis: a multicenter study. Ophthal Plast Reconstr Surg. 2009 Nov-Dec;25(6):455-7. doi: 10.1097/IOP.0b013e3181b80c59.
- Li EY, Wong ES, Wong AC, et al; Primary vs Secondary Endoscopic Dacryocystorhinostomy for Acute Dacryocystitis With Lacrimal Sac Abscess Formation: A Randomized Clinical Trial. JAMA Ophthalmol. 2017 Dec 1;135(12):1361-1366. doi: 10.1001/jamaophthalmol.2017.4798.
- Endoscopic dacryocystorhinostomy; NICE Interventional Procedures Guidance, February 2005
- Zengin MO, Eren E; The return of the jedi: comparison of the outcomes of endolaser dacryocystorhinostomy and endonasal dacryocystorhinostomy. Int Forum Allergy Rhinol. 2014 Jun;4(6):480-3. doi: 10.1002/alr.21302. Epub 2014 Feb 20.
- Wong RK, VanderVeen DK; Presentation and management of congenital dacryocystocele. Pediatrics. 2008 Nov;122(5):e1108-12. Epub 2008 Oct 27.
- Mimura M, Ueki M, Oku H, et al; Process of spontaneous resolution in the conservative management of congenital dacryocystocele. Clin Ophthalmol. 2014 Feb 26;8:465-9. doi: 10.2147/OPTH.S58342. eCollection 2014.
- Ullrich K, Malhotra R, Patel BC; Dacryocystorhinostomy.
- Lee S, Yen MT; Management of preseptal and orbital cellulitis. Saudi J Ophthalmol. 2011 Jan;25(1):21-9. doi: 10.1016/j.sjopt.2010.10.004. Epub 2010 Dec 10.
- Feroze KB, Patel BC; Canaliculitis.
- Zaldivar RA, Bradley EA; Primary canaliculitis. Ophthal Plast Reconstr Surg. 2009 Nov-Dec;25(6):481-4.
- Tao H, Xu LP, Han C, et al; Diagnosis of lacrimal canalicular diseases using ultrasound biomicroscopy: a preliminary study. Int J Ophthalmol. 2014 Aug 18;7(4):659-62. doi: 10.3980/j.issn.2222-3959.2014.04.15.13. eCollection 2014.
- Kaliki S, Ali MJ, Honavar SG, et al; Primary canaliculitis: clinical features, microbiological profile, and management outcome. Ophthal Plast Reconstr Surg. 2012 Sep-Oct;28(5):355-60. doi: 10.1097/IOP.0b013e31825fb0cd.
- Nasolacrimal duct obstruction (nasolacrimal drainage dysfunction); College of Optometrists, March 2016
- Liarakos VS, Boboridis KG, Mavrikakis E, et al; Management of canalicular obstructions. Curr Opin Ophthalmol. 2009 Sep;20(5):395-400.
- Athanasiov PA, Prabhakaran VC, Mannor G, et al; Transcanalicular approach to adult lacrimal duct obstruction: a review of instruments and methods. Ophthalmic Surg Lasers Imaging. 2009 Mar-Apr;40(2):149-59.
- Baek BJ, Hwang GR, Jung DH, et al; Surgical results of endoscopic dacryocystorhinostomy and lacrimal trephination in distal or common canalicular obstruction. Clin Exp Otorhinolaryngol. 2012 Jun;5(2):101-6. doi: 10.3342/ceo.2012.5.2.101. Epub 2012 Jun 12.
Continue reading below
About the authorView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Mar 2028
6 Mar 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free