Eczema in children
Peer reviewed by Dr Krishna Vakharia, MRCGPAuthored by Dr Colin Tidy, MRCGPOriginally published 5 Jul 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is childhood eczema?1
Most children with eczema have atopic eczema. However, contact dermatitis also occurs in children. Children with atopic eczema may also have contact dermatitis, including skin reactions occasionally caused by eczema treatments, particularly emollients. See the links for the separate articles to provide further information.
Atopic eczema (also known as atopic dermatitis) is a chronic inflammatory skin condition that affects people of all ages, although it most frequently presents in early childhood (mostly before 5 years of age).
The term 'atopic' is used to describe a group of conditions (eczema, asthma, hay-fever, and food allergy) that are linked by an increase in the allergy response activity of the immune system. A personal or familial history of other atopic conditions is common among those with atopic eczema.
Contact dermatitis is an inflammatory skin condition which occurs as a result of exposure to an external irritant or allergen.2
How common is childhood eczema? (Epidemiology)1
Back to contentsAtopic eczema is common. Estimates vary in different populations, but figures suggest that atopic eczema affects about 10–30% of children.
There is no difference in prevalence based on sex and ethnicity.
Around 70–90% of cases of atopic eczema first present before 5 years of age with about 45% of cases beginning in the first 6 months of life and about 60–65% of cases in the first year of life.
There is an increased prevalence of atopic eczema in children with an affected parent or sibling. About 70% of people with atopic eczema have a positive family history of atopic disease (atopic eczema, asthma, and/or hay fever).
The prevalence of contact dermatitis in children is unclear. One review found that patch testing was positive in 27–95% of referred children.2
Continue reading below
Symptoms of childhood eczema (presentation)1
Back to contentsAtopic eczema is characterised by dry, pruritic skin, and is typically an episodic disease of flares (exacerbations), which may occur occasionally or frequently, and remissions. In severe cases, disease activity may remain constantly severe.
Contact dermatitis can present as acute or chronic:2
Acute contact dermatitis typically presents with erythema and vesiculation. Dryness, scaling and bullae may also be present.
Chronic contact dermatitis typically presents with dryness, lichenification and fissuring.
Diagnose atopic eczema when a child has an itchy skin condition plus 3 or more of the following:3
Visible flexural dermatitis involving the skin creases, such as the bends of the elbows or behind the knees (or visible dermatitis on the cheeks and/or extensor areas in children aged 18 months or under).
Previous flexural dermatitis (or dermatitis on the cheeks and/or extensor areas in children aged 18 months or under).
Dry skin in the last 12 months.
Asthma or allergic rhinitis (or history of atopic disease in a first-degree relative of children aged under 4 years).
Onset of signs and symptoms under the age of 2 years (do not use this criterion in children aged under 4 years).
Dermatitis
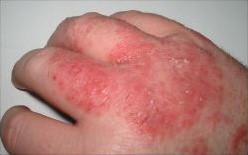
© Topbanana at English Wikipedia., CC BY-SA 3.0, via Wikimedia Commons
In Asian, Black Caribbean and Black African children, atopic eczema can affect the extensor surfaces rather than the flexures, and discoid (circular) or follicular (around hair follicles) patterns may be more common.
Atopic dermatitis child
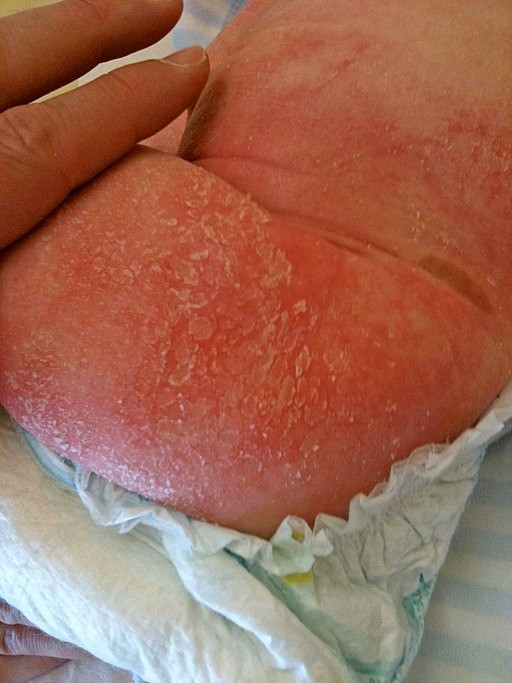
© Gzzz, CC BY-SA 4.0, via Wikimedia Commons
Assessment3
Back to contentsAssessment of severity
Take clinical and drug histories of children with atopic eczema, including questions about:
Time of onset, pattern and severity of the atopic eczema.
Response to previous and current treatments.
Possible trigger factors (irritant and allergic).
The impact of the atopic eczema on the child and their parents or carers.
Dietary history, including any dietary manipulation.
Growth and development.
Personal and family history of atopic conditions.
Assessment of wellbeing and quality of life
Use a holistic approach when assessing a child's atopic eczema at each consultation, taking into account the severity of the atopic eczema and the child's quality of life, including everyday activities, sleep, and psychosocial wellbeing. There is not necessarily a direct relationship between the severity of the atopic eczema and the impact it has on quality of life.
Clear: normal skin, no evidence of active atopic eczema: no impact on quality of life.
Mild: areas of dry skin, infrequent itching (with or without small areas of redness): little impact on everyday activities, sleep and psychosocial wellbeing.
Moderate: areas of dry skin, frequent itching, redness (with or without excoriation and localised skin thickening): moderate impact on everyday activities and psychosocial wellbeing, frequently disturbed sleep.
Severe: widespread areas of dry skin, incessant itching, redness (with or without excoriation, extensive skin thickening, bleeding, oozing, cracking and alteration of pigmentation): severe limitation of everyday activities and psychosocial functioning, nightly loss of sleep.
Assess whether the child's atopic eczema is consistent in severity, or whether there are areas of differing severity. If there are areas of differing severity, treat each area independently.
Take into account the impact of atopic eczema on parents or carers as well as the child, and provide them with advice and support.
All categories of severity of atopic eczema can have a negative impact on psychological and psychosocial wellbeing and quality of life.
Assessment tools
Consider using the following additional tools to provide objective measures of the severity of atopic eczema, quality of life and response to treatment:
Visual analogue scales (0 to 10) capturing the child's and/or parents' or carers' assessment of severity, itch and sleep loss over the previous 3 days and nights.
Validated tools:
Patient-Oriented Eczema Measure (POEM) for severity.
Children's Dermatology Life Quality Index (CDLQI), Infants' Dermatitis Quality of Life Index (IDQoL) or Dermatitis Family Impact (DFI) questionnaire for quality of life.
Continue reading below
Differential diagnosis1
Back to contentsPsoriasis: less itchy, well-circumscribed, reddish, flat-topped plaques with silvery scales. Typically symmetrical.
Allergic contact dermatitis: eczematous rash, at any site related to a topical allergen, in a person of any age. Allergic contact dermatitis can be both an alternative diagnosis and a trigger factor of atopic eczema. Consider a diagnosis of allergic contact dermatitis in children with an exacerbation of previously controlled atopic eczema, or reactions to topical treatments.3
Seborrhoeic dermatitis: red, sharply marginated lesions with greasy scales; usually confined to areas with sebaceous gland activity (eg, beard area, eyebrows, scalp, and nasolabial folds).
Fungal infection: annular patch or plaque with slightly raised, sometimes scaly, border, and central clearing.
Scabies or other infestations: should be suspected when there is recent onset of an itchy rash in a family.
Food allergy: consider in children and young people who have not responded to conventional treatment for atopic eczema.
Diagnosing childhood eczema (Investigations) 3
Back to contentsInvestigations are not required to establish the diagnosis of atopic eczema. However, they may be useful in excluding differential diagnoses, especially in people whose symptoms do not respond to treatment.
Most children with mild atopic eczema do not need to have tests for allergies.
Advise parent not to use high street or internet allergy tests, because there is no evidence of their value in managing atopic eczema.
The gold standard investigation for diagnosis of contact dermatitis is patch testing. If patch testing is indicated, refer to dermatology.2
Identifying and managing trigger factors
When assessing children with atopic eczema, identify potential trigger factors, including:
Irritants, eg, soaps and detergents (including shampoos, bubble baths, shower gels and washing-up liquids).
Skin infections.
Contact allergens.
Food allergens.
Inhalant allergens.
Consider a diagnosis of food allergy in:
Children with atopic eczema who have had immediate symptoms from eating a particular food.
Babies and young children with moderate or severe atopic eczema that has not been controlled by optimum management, particularly if associated with gut
dysmotility (colic, vomiting, altered bowel habit) or failure to thrive.
Consider a diagnosis of inhalant allergy in:
Children with seasonal flares of atopic eczema.
Children with atopic eczema associated with asthma or allergic rhinitis.
Children aged 3 years or over with atopic eczema on the face, particularly around the eyes.
For bottle-fed babies aged under 6 months with moderate or severe atopic eczema that has not been controlled by optimal treatment with emollients and mild topical corticosteroids, offer a 6- to 8-week trial of an extensively hydrolysed protein formula or amino acid formula in place of cow's milk formula. Refer children with atopic eczema for specialist dietary advice if they have followed a cow's milk-free diet for longer than 8 weeks.
Do not use diets based on unmodified proteins of other species' milk (eg, goat's milk or sheep's milk) or partially hydrolysed formulas to manage suspected cow's milk allergy in children with atopic eczema.
Offer diets that include soya protein along with specialist dietary advice for children aged 6 months or over.
For children who are being breast fed, explain that it is not known whether changing the mother's diet will reduce the severity of the atopic eczema. If food allergy is strongly suspected, consider a trial of an allergen-specific exclusion diet.
It is unclear what role factors such as stress, humidity or extremes of temperature have in causing flares of atopic eczema. However, these factors should be avoided or ameliorated when possible.
Treatment and management of childhood eczema3
Back to contentsFor contact dermatitis, avoidance of the stimulus is the most important element of treatment and prevention of recurrent episodes of contact dermatitis.2 Management will also include emollient and soap substitutes to maintain skin hydration and improve barrier repair, topical steroids to control symptoms, and treatment of any secondary infection. For further information, see the article on Contact and Occupational Dermatitis.
The rest of this section is directed towards the management of atopic eczema.
Use the stepped approach for managing atopic eczema in children. Emollients are the basis of management and should always be used, even when the skin is clear. Management can then be stepped up or down, according to the severity of symptoms:
Mild atopic eczema: emollients, mild-potency topical corticosteroids.
Moderate atopic eczema: emollients, moderate-potency topical corticosteroids, topical calcineurin inhibitors, bandages.
Severe atopic eczema: emollients, potent topical corticosteroids, topical calcineurin inhibitors, bandages, phototherapy, systemic therapy.
Provide information on how to recognise flares of atopic eczema (increased dryness, itching, redness, swelling and general irritability). Give clear instructions on how to manage flares according to the stepped-care plan, and prescribe treatments that allow children and their parents or carers to follow this plan.
Start treatment for flares of atopic eczema as soon as signs and symptoms appear, and continue treatment for approximately 48 hours after symptoms subside.
Emollients
Offer children with atopic eczema a choice of unperfumed emollients to use every day for moisturising. Prescribe large quantities of leave-on emollients (250 g to 500 g weekly) that are easily available to use at nursery, pre-school or school. Review repeat prescriptions at least once a year.
Emollients should be used in larger amounts and more often than other treatments, and on their whole body, both when the atopic eczema is clear and while using all other treatments.
provide advice on how to apply emollients, including how to smooth emollients onto the skin rather than rubbing them in.
If using emollients and other topical products at the same time of day, they should apply one product at a time, and wait several minutes before applying the next product, and they can choose which product to apply first. Advise that:
Leave-on emollients or emollient soap substitutes should be used instead of soaps and detergent-based wash products.
Leave-on emollients can be added to bath water.
Children aged under 12 months should use leave-on emollients or emollient soap substitutes instead of shampoos.
Older children using shampoo should use a brand that is unperfumed and ideally labelled as suitable for eczema, and they should avoid washing their hair in bath water.
Do not offer emollient bath additives to children with atopic eczema.
Topical corticosteroids
Tailor the potency of topical corticosteroids to the severity of the child's atopic eczema (which may vary according to body site):
Use mild potency for mild atopic eczema.
Use moderate potency for moderate atopic eczema.
Use potent for severe atopic eczema.
Use mild potency for the face and neck, except for short-term (3 to 5 days) use of moderate potency for severe flares.
Use moderate or potent preparations for short periods only (7 to 14 days) for flares in vulnerable sites such as axillae and groin.
Do not use very potent preparations in children without specialist dermatological advice.
It is recommended that topical corticosteroids for atopic eczema should be prescribed for application only once or twice daily.
Topical corticosteroids should only be applied to areas of active atopic eczema (or eczema that has been active within the past 48 hours), which may include areas of broken skin.
If a mild or moderately potent topical corticosteroid has not controlled the atopic eczema within 7 to 14 days:
Exclude secondary bacterial or viral infection.
For children aged 12 months or over, use potent topical corticosteroids for as short a time as possible (no longer than 14 days, and not on the face or neck).
If the atopic eczema is still uncontrolled, review the diagnosis and refer the child for specialist dermatological advice.
Do not use potent topical corticosteroids in children aged under 12 months without specialist dermatological supervision.
Once the atopic eczema has been controlled, consider treating problem areas with topical corticosteroids for 2 consecutive days per week to prevent flares in children with frequent flares (2 or 3 per month). Review this strategy within 3 to 6 months.
Consider a different topical corticosteroid of the same potency as an alternative to stepping up treatment if tachyphylaxis to a topical corticosteroid is suspected in children with atopic eczema.
See also the article on Topical Steroids for the Skin.
Topical calcineurin inhibitors
Do not use topical tacrolimus or pimecrolimus for mild atopic eczema, or as first-line treatments for atopic eczema of any severity.
Topical tacrolimus is recommended as an option for the second-line treatment of moderate to severe atopic eczema in adults and children aged 2 years and older that has not been controlled by topical corticosteroids, where there is a serious risk of important adverse effects from further topical corticosteroid use, particularly irreversible skin atrophy.
Pimecrolimus is recommended as an option for the second-line treatment of moderate atopic eczema on the face and neck in children aged 2 years to 16 years that has not been controlled by topical corticosteroids, where there is a serious risk of important adverse effects from further topical corticosteroid use, particularly irreversible skin atrophy.
It is recommended that treatment with tacrolimus or pimecrolimus be initiated only by physicians (including general practitioners) with a special interest and experience in dermatology, and only after careful discussion with the patient about the potential risks and benefits of all appropriate second-line treatment options.
Topical calcineurin inhibitors should only be applied to areas of active atopic eczema, which may include areas of broken skin.
Topical calcineurin inhibitors should not be used under occlusion (bandages and dressings) for treating atopic eczema in children without specialist dermatological advice.
For facial atopic eczema in children that requires long-term or frequent use of mild topical corticosteroids, consider stepping up treatment to topical calcineurin inhibitors.
Dry bandages and medicated dressings (including wet wrap therapy)
Do not use occlusive medicated dressings and dry bandages to treat infected atopic eczema in children.
Localised medicated dressings or dry bandages with emollients may be considered as a treatment for areas of chronic lichenified (localised skin thickening) atopic eczema in children.
Localised medicated dressings or dry bandages with emollients and topical corticosteroids may be considered for short-term treatment of flares (7 to 14 days) or areas of chronic lichenified atopic eczema in children.
Do not use whole-body (limbs and trunk) occlusive dressings (including wet wrap therapy) or whole-body dry bandages (including tubular bandages and garments) as first-line treatment for atopic eczema in children. If using these treatments, they should be started by a healthcare professional trained in their use.
When combining whole-body (limbs and trunk) occlusive dressings (including wet wrap therapy) with topical corticosteroids for atopic eczema in children:
Use initially for 7 to 14 days.
Seek specialist dermatological advice before continuing this combination for longer.
Think about stopping the topical corticosteroids and continuing the dressings alongside emollients until the atopic eczema is controlled.
Antihistamines
See also the article on Antihistamines.
Do not routinely use oral antihistamines to manage atopic eczema in children.
For children with severe atopic eczema or children with mild or moderate atopic eczema who have severe itching or urticaria, offer a 1-month trial of a non-sedating antihistamine. If treatment is successful, think about continuing it while symptoms persist, and review every 3 months.
If sleep disturbance has a significant impact on the child or parents or carers, offer a 7- to 14-day trial of an age-appropriate sedating antihistamine to children aged 6 months or over during an acute flare of atopic eczema. Think about repeating this during subsequent flares.
Managing infections
Offer children with atopic eczema and their parents or carers information on how to recognise the symptoms and signs of bacterial infection with staphylococcus and/or streptococcus: weeping, pustules, crusts, eczema failing to respond to therapy, rapidly worsening eczema, fever and malaise.
Provide clear information on how to access treatment for infected atopic eczema.
Advise to obtain new supplies of their topical atopic eczema medications after treatment for infected atopic eczema. This is because their medications can become contaminated and act as a source of infection.
Choice of antibiotics for children and young people aged from 1 month to under 18 years:4
For secondary bacterial infection of eczema in people who are not systemically unwell: do not routinely offer either a topical or oral antibiotic.
First-choice topical if a topical antibiotic is appropriate: fusidic acid 2%.
First-choice oral if an oral antibiotic is appropriate: flucloxacillin.
Alternative oral antibiotic for penicillin allergy or if flucloxacillin is unsuitable (other than pregnancy): clarithromycin.
Alternative oral antibiotic for penicillin allergy in pregnancy: erythromycin.
If meticillin-resistant staphylococcus aureus is suspected or confirmed: consult a microbiologist.
Consider herpes simplex (cold sore) infection if a child's infected atopic eczema fails to respond to treatment with antibiotics and an appropriate topical corticosteroid. If a child with atopic eczema has a lesion on the skin that is suspected to be herpes simplex, treat with oral aciclovir even if the infection is localised.
If eczema herpeticum (widespread herpes simplex) is suspected in a child with atopic eczema, immediately start treatment with systemic aciclovir and refer the child for same-day specialist dermatological advice. If secondary bacterial infection is also suspected, start treatment with systemic antibiotics.
Ezcema herpeticum
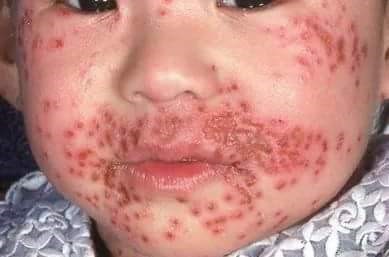
© Mohammad2018, CC BY-SA 4.0, via Wikimedia Commons
If eczema herpeticum involves the skin around the eyes, treat with systemic aciclovir and refer the child for same-day ophthalmological and dermatological advice.
Offer children with atopic eczema and their parents or carers information on how to recognise eczema herpeticum:
Areas of rapidly worsening, painful eczema.
Clustered blisters that look like early-stage cold sores.
Punched-out erosions (circular, depressed, ulcerated lesions), usually 1 mm to 3 mm, that are uniform in appearance (these may combine to form larger areas
of erosion with crusting).
Possible fever, lethargy or distress.
Phototherapy and systemic treatments
Consider phototherapy or systemic treatments for severe atopic eczema in children when other management options have failed or are inappropriate, and there is a significant negative impact on quality of life.
Only use phototherapy and systemic treatments under specialist dermatological supervision by staff who are experienced in working with children.
Only start phototherapy or systemic treatments in children with atopic eczema after assessment and documentation of severity of atopic eczema and quality of life.
Complementary therapies
The effectiveness and safety of the following therapies has not yet adequately been assessed in clinical trials: homeopathy, herbal medicine, massage, food supplements.
Topical corticosteroids are deliberately added to some herbal products intended for use in children with atopic eczema.
Liver toxicity has been associated with the use of some Chinese herbal medicines intended to treat atopic eczema.
Using regular massage along with emollients may improve atopic eczema.
Indications for referral3
Back to contentsImmediately (same day) refer children for specialist dermatological advice if eczema herpeticum is suspected.
Urgently (within 2 weeks) refer children for specialist dermatological advice if:
Their atopic eczema is severe and has not responded to optimal topical therapy after 1 week.
Treatment of bacterially infected atopic eczema has failed.
Refer children with atopic eczema for specialist dermatological advice if:
The diagnosis is, or has become, uncertain.
Management has not controlled the atopic eczema satisfactorily, based on a subjective assessment by the child, parent or carer (eg, the child is having 1 to 2 weeks of flares per month or is having adverse reactions to many emollients).
Atopic eczema on the face has not responded to treatment.
For advice on how to apply treatments (eg, bandaging techniques).
Contact allergic dermatitis is suspected (eg, persistent atopic eczema or facial, eyelid or hand atopic eczema).
The atopic eczema is causing significant social or psychological problems for the child or their parents or carers (eg, sleep disturbance or poor school attendance).
Atopic eczema is associated with severe and recurrent infections, especially deep abscesses or pneumonia.
If atopic eczema is responding to optimal management but the child's quality of life and psychosocial wellbeing has not improved, refer for psychological advice.
Refer children with moderate or severe atopic eczema and suspected food allergy for specialist investigation and management.
Refer children with atopic eczema for specialist advice relating to growth if they are not growing at the expected growth trajectory (as reflected by UK growth charts).
Complications of childhood eczema1
Back to contentsInfection:
Bacterial infection with Staphylococcus aureus may present as typical impetigo or as worsening of eczema.
Herpes simplex infection, including eczema herpeticum:
Eczema herpeticum is a medical emergency, especially in children under two years of age, and requires urgent referral for diagnosis and management. It can have serious sequelae, such as eye or meningeal involvement resulting in scarring.
Risk factors for eczema herpeticum include early-onset and severe atopic eczema, marked elevations in total IgE, elevated allergen-specific IgE levels, peripheral eosinophilia, and the presence of filaggrin mutations.
Superficial fungal infections are more common in people with atopic eczema.
Psychosocial problems:
Atopic eczema causes considerable distress, and depression has been reported in both teenagers and adults with atopic eczema.
Preschool children with atopic eczema have higher rates of behavioural problems, fearfulness, and dependency on their parents, than unaffected children.
School children with atopic eczema have problems including time away from school, impaired performance, social restrictions, teasing, and bullying.
Atopic eczema can be associated with poor self-image and self-confidence that can impair social development. Among children with moderate-to-severe eczema attending outpatient departments, psychological problems are double that of school children without eczema.
Sleep disturbance is a major problem for people with atopic eczema and their families.
Other atopic and non-atopic comorbidities:
Atopic eczema has been found to be associated with numerous atopic comorbidities, including asthma, allergic rhinitis (hay fever), food allergy, and eosinophilic oesophagitis.
Increased severity in infancy and persistent disease has been associated with greater risks of food allergy (particularly to egg and peanut).
Other non-atopic comorbidities associated with atopic eczema include allergic contact dermatitis, obesity and cardiovascular disease.
Prognosis1
Back to contentsAtopic eczema is typically an episodic disease of flares (exacerbations, which may occur as frequently as two or three times each month) and remissions. In severe cases (2–6% of cases), disease activity may be continuous.
Atopic eczema has a tendency to gradually improve with time, but not all children will grow out of atopic eczema and it may get worse in teenage or adult life.
The condition can be expected to clear in about 65% of children by the time they are 7 years of age and in about 74% of children by 16 years of age, although relapses may occur.
A systematic review and meta-analysis assessed the persistence rates of atopic eczema in 110,651 participants from 15 countries found that 80% of childhood atopic eczema did not persist by 8 years of age and less than 5% persisted by 20 years after diagnosis.
Children with already persistent disease, later onset, and/or more severe disease were more likely to experience further disease persistence.
Many children with atopic eczema will go on to develop asthma (30–50%) and/or hay fever (30–80%).
The prognosis of contact dermatitis is variable and depends on the causative agent and the feasibility of avoiding exposure.2
Further reading and references
- Eczema: Atopic Eczema; Primary Care Dermatology Society (PCDS)
- Leins L, Orchard D; Eczema management in school-aged children. Aust Fam Physician. 2017 Dec;46(12):896-899.
- Eczema: contact allergic dermatitis; Primary Care Dermatology Society.
- Atopic dermatitis; DermNet.
- Contact dermatitis; DermNet.
- Wollenberg A, Kinberger M, Arents B, et al; European guideline (EuroGuiDerm) on atopic eczema: part I - systemic therapy. J Eur Acad Dermatol Venereol. 2022 Sep;36(9):1409-1431. doi: 10.1111/jdv.18345.
- Eczema - atopic; NICE CKS, July 2024 (UK access only)
- Dermatitis - contact; NICE CKS, July 2018 (UK access only)
- Atopic eczema in under 12s: diagnosis and management; NICE Clinical Guideline (December 2007 - last updated June 2023)
- Secondary bacterial infection of eczema and other common skin conditions: antimicrobial prescribing; NICE Guideline (March 2021)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 3 Jul 2028
5 Jul 2023 | Originally published
Authored by:
Dr Colin Tidy, MRCGPPeer reviewed by
Dr Krishna Vakharia, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free