Epididymal cysts
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 9 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Epididymal cyst article more useful, or one of our other health articles.
In this article:
Continue reading below
What are epididymal cysts?
Smooth, extratesticular, spherical cysts in the head of the epididymis are not uncommon in adult men. If the cyst contains spermatozoa (usually seen on histology only), it may be referred to as a spermatocele.
They are benign and do not usually require treatment. It is important to appreciate when they might be significant and when further investigation or treatment is recommended.
How common are epididymal cysts? (Epidemiology)
Back to contentsEpididymal cysts usually develop in middle-aged men.1 Epididymal cysts are rare in children and when they occur, usually present around puberty. The incidence in children is between 5-20%.2 The prevalence in the general population is difficult to estimate but a 2019 paper showed the incidence of men with either hydro or spermatocele diagnosis in specialised healthcare was around 100 per 100,000 men.3
Continue reading below
Symptoms of epididymal cysts
Back to contentsPatients usually present having noticed a lump. This often causes a great deal of anxiety and clinical examination can enable reassurance.
Often epididymal cysts are multiple and are frequently bilateral.1
Small cysts may remain undetected and asymptomatic. Small cysts are tolerated by patients. However, once epididymal cysts get large (with size equivalent to the size of a testicle) they are, unsurprisingly, more likely to present for removal.
As they are cystic and fluid-filled they are well defined, fluctuant and do not usually transilluminate.1
As they arise in the epididymis, the testis is palpable quite separately from the cyst (unlike a hydrocele where the testis is palpable within the fluid-filled swelling).
Extratesticular, fluctuant, and cystic swellings which are readily palpable separate from the body of the testis, are epididymal cysts and do not usually need further investigation.
These can readily be distinguished from testicular tumours which arise from the testis.
The image below represents a typical appearance during surgical procedure.
Epididymal cyst surgical exploration
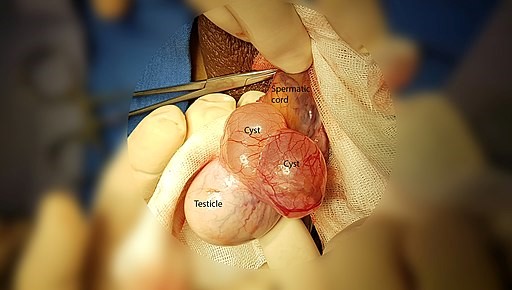
© E. dronism, CC BY-SA 4.0, via Wikimedia Commons
Differential diagnosis
Back to contentsInflammatory thickening, either acute or chronic of the epididymis.
Hydroceles. These are collections of fluid surrounding the entire testicle.
Varicoceles. These are dilated veins and have been described as feeling like 'a bag of worms'. They increase with increase in abdominal pressure (Valsalva manoeuvre).
Other scrotal masses, particularly extratesticular scrotal masses.4 These are predominantly benign and include adenomatoid tumour of the epididymis, paratesticular abscess and epididymal cystic lymphangioma.
Lipomas are the most common extratesticular tumours.
Continue reading below
Investigations
Back to contentsScrotal ultrasound will assist diagnosis if there is uncertainty. Aspiration of fluid is rarely useful or necessary from either a diagnostic or a treatment perspective.
Associated diseases
Back to contentsCystic fibrosis. Congenital absence of the vas deferens is the most common genital tract anomaly in cystic fibrosis (99% of patients).5 Epididymal cysts are common.
Von Hippel-Lindau disease. Along with other more significant manifestations of this syndrome, epididymal cysts are associated with the condition.6 It is a rare disease and important to recognise early.
Adult polycystic kidney disease (autosomal dominant).7
There is no evidence that epididymal cysts are associated with infertility.8
Treatment for epididymal cysts
Back to contentsTreatment is not usually necessary and explanation and advice are all that is usually required.1 Patients should be advised to seek medical advice if epididymal cysts become painful or suddenly start increasing in size.
Spontaneous resolution may take up to 50 months.9
Surgical excision is recommended in children with intractable scrotal pain or if the cyst size does not seem to involute. Excision may also be offered to symptomatic adults.
Percutaneous aspiration with instillation of sclerosant is another option. The success rate in one study (at a median of 31 months post-initial procedure, after at most two procedures) was 85% for spermatoceles/epididymal cysts.10
Complications
Back to contentsTorsion of the cyst can occur but is extremely rare with only a handful of cases reported.2 11 They do not become infected.
Further reading and references
- Zito PM, Scharf R; Epidermoid Cyst. StatPearls, Aug 2023.
- Scrotal pain and swelling; NICE CKS; August 2024 (UK access only)
- Bleve C, Conighi ML, Bucci V, et al; Torsion of huge epididymal cyst in a 16-year-old boy: case report and review of the literature. Pediatr Med Chir. 2018 May 29;40(1). doi: 10.4081/pmc.2018.162.
- Lundstrom KJ, Soderstrom L, Jernow H, et al; Epidemiology of hydrocele and spermatocele; incidence, treatment and complications. Scand J Urol. 2019 Apr - Jun;53(2-3):134-138. doi: 10.1080/21681805.2019.1600582. Epub 2019 Apr 16.
- O'Kelly F, McAlpine K, Abdeen N, et al; The futility of continued surveillance of epididymal cysts - A study of the prevalence and clinico-demographics in pre- vs. post-pubertal boys. Can Urol Assoc J. 2019 Apr 26:E398-E403. doi: 10.5489/cuaj.5667.
- Yoon JC, Casella JL, Litvin M, et al; Male reproductive health in cystic fibrosis. J Cyst Fibros. 2019 Oct;18 Suppl 2:S105-S110. doi: 10.1016/j.jcf.2019.08.007.
- Gomella PT, Shin P, Srinivasan R, et al; Obstructive azoospermia secondary to bilateral epididymal cystadenomas in a patient with von Hippel-Lindau. Urol Case Rep. 2019 May 29;27:100922. doi: 10.1016/j.eucr.2019.100922. eCollection 2019 Nov.
- Kim JA, Blumenfeld JD, Prince MR; Seminal Vesicles in Autosomal Dominant Polycystic Kidney Disease. Codon Publications, Nov 2015.
- Weatherly D, Wise PG, Mendoca S, et al; Epididymal Cysts: Are They Associated With Infertility? Am J Mens Health. 2018 May;12(3):612-616. doi: 10.1177/1557988316644976. Epub 2016 Apr 26.
- Mukendi AM; Bilateral epididymal cyst with spontaneous resolution. Clin Case Rep. 2020 Aug 22;8(12):2689-2691. doi: 10.1002/ccr3.3199. eCollection 2020 Dec.
- Low LS, Nair SM, Davies AJW, et al; Aspiration and sclerotherapy of hydroceles and spermatoceles/epididymal cysts with 100% alcohol. ANZ J Surg. 2020 Jan;90(1-2):57-61. doi: 10.1111/ans.15467. Epub 2019 Oct 18.
- Ozaal AMOM, Pragalathan B, Lavanya S, et al; Torsion of an Epididymal Cyst: A Rare Finding on Scrotal Exploration for Acute Scrotum. Case Rep Urol. 2020 Nov 22;2020:8858606. doi: 10.1155/2020/8858606. eCollection 2020.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Jan 2028
9 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free