Halo naevus
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 14 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: Sutton's naevus, leukoderma acquisita centrifugum
Continue reading below
What causes halo naevus?1 2
A halo naevus is a benign skin lesion that is a result of a common melanocytic naevus undergoing an inflammatory process, such that a zone of depigmentation surrounds the mole. There is an infiltration of T lymphocytes and macrophages and possibly some antibody-mediated autoimmunity. The aetiology and pathophysiology of the immune reaction to the presence of an aggregate of melanocytes is poorly understood.
The lesion can cause significant anxiety in those who have it, due to its characteristic and striking appearance. The central naevus may undergo involution leaving a grey or white halo that can resemble melanoma that has undergone regression, leaving the clinician with a diagnostic dilemma on occasions.
How common is halo naevus?
Back to contentsThey are common lesions and estimated to have a prevalence of about 1% in the general population.3 Turner syndrome patients have a higher prevalence of halo naevi than the general population.4 Some families may have a tendency to the lesions. Halo naevi most commonly affect younger people and the average age of onset is about 15 years.5
Continue reading below
Halo naevus symptoms2 6
Back to contentsHalo naevus
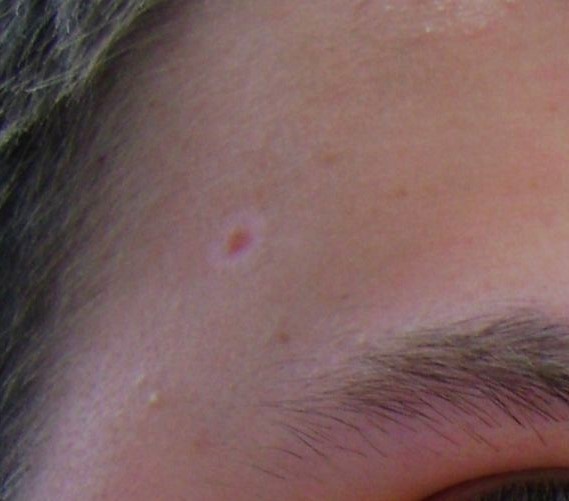
© JeffyP, Public domain, via Wikimedia Commons
They are usually asymptomatic lesions, apart from the cosmetic disturbance that they cause.
A solitary halo naevus or multiple halo naevi are most often found on the trunk. They are less common on the head and are rare on the limbs. Halo naevi may follow the Köbner phenomenon, arising within a mole that has been injured in some way.
The white halo is usually about 0.5-1.0 cm wide and is symmetrical (round or oval in shape). The halos develop at intervals round one or several moles, but not around all of them.
There are four stages of a halo naevus. It may take several years to complete the cycle. Multiple halo naevi can be at different stages:
Stage 1: A rim of pale skin surrounds a mole.
Stage 2: The mole may become pinker or less pigmented, and fades away.
Stage 3: A circular or oval area of depigmentation persists.
Stage 4: The affected skin gradually returns to its normal colour.
The central naevus may involute and then subsequently repigment, over a period of up to ten years.7
Differential diagnosis2 6
Back to contentsThe lesion has a characteristic appearance that usually means it is not confused with other diagnoses. The following problems can present with a similar appearance and should be considered as the cause of a depigmented lesion but should usually be able to be discriminated on the grounds of their history or appearance:
Lichen sclerosus et atrophicus.
Dysplastic naevus.
Hypopigmented skin lesion of sarcoidosis.
Continue reading below
Investigations2 6
Back to contentsNone is required if the lesion has a typical history and appearance.
A Wood's light may be used to distinguish diagnoses such as tinea/pityriasis versicolor.
Dermoscopy may be used to demonstrate characteristic patterns of pigmentation associated with benign melanocytic naevi.6
If there is any uncertainty as to the nature of the lesion, consider dermatological referral or excision biopsy to exclude melanoma.
Features that would prompt the need for excision biopsy include:
Irregularity of the margin of the pigmented or depigmented zones.
Non-uniformity of overall shape.
Papular component that is not centrally located.
Rapid growth of the lesion.
Rapid increase in pigmentation of the pigmented zone.
Irritation, bleeding or ulceration of the lesion.
Associated diseases
Back to contentsHalo naevi-associated leukoderma.9
Halo naevus treatment
Back to contentsHalo naevi are benign lesions that require no active management other than reassurance of the patient. Sometimes treatment for cosmetic reasons may be requested. The depigmentation can be particularly noticeable in darker-skinned individuals.
Other than excision, laser treatment has been used.10 If the area of depigmentation is large, this may lead to requests for cosmetic attention. Various techniques are reported, including tattooing and topical tacrolimus.11
Complications
Back to contentsThere are no complications as such, unless the lesion is misdiagnosed or there are problems associated with excision biopsy.
Prognosis
Back to contentsThe lesion is benign so the prognosis is excellent.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Improving outcomes for people with skin tumours including melanoma; NICE Guidance (May 2010 update)
- van Geel N, Vandenhaute S, Speeckaert R, et al; Prognostic value and clinical significance of halo naevi regarding vitiligo. Br J Dermatol. 2011 Apr;164(4):743-9. doi: 10.1111/j.1365-2133.2010.10154.x. Epub 2011 Mar 16.
- Cohen BE, Mu EW, Orlow SJ; Comparison of Childhood Vitiligo Presenting with or without Associated Halo Nevi. Pediatr Dermatol. 2016 Jan-Feb;33(1):44-8. doi: 10.1111/pde.12717. Epub 2015 Nov 17.
- Botella-Estrada R, Kutzner H; Study of the immunophenotype of the inflammatory cells in melanomas with regression and halo nevi. Am J Dermatopathol. 2015 May;37(5):376-80. doi: 10.1097/DAD.0000000000000205.
- Halo Naevus; Primary Care Dermatology Society (PCDS)
- Hoffman U et al; Simultaneous Onset of Segmental Vitiligo and a Halo Surrounding a Congenital Melanocytic Naevus, Acta Derm Venereol 2009; 89: 402–406.
- Bello-Quintero CE, Gonzalez ME, Alvarez-Connelly E; Halo nevi in Turner syndrome. Pediatr Dermatol. 2010 Jul-Aug;27(4):368-9. doi: 10.1111/j.1525-1470.2010.01171.x.
- Pustisek N, Sikanic-Dugic N, Hirsl-Hecej V, et al; "Halo nevi" and UV radiation. Coll Antropol. 2010 Apr;34 Suppl 2:295-7.
- Halo naevus; DermNet NZ.
- Aouthmany M, Weinstein M, Zirwas MJ, et al; The natural history of halo nevi: a retrospective case series. J Am Acad Dermatol. 2012 Oct;67(4):582-6. doi: 10.1016/j.jaad.2011.11.937. Epub 2012 Mar 2.
- Yaghoobi R, Omidian M, Bagherani N; Vitiligo: a review of the published work. J Dermatol. 2011 May;38(5):419-31.
- van Geel N, Speeckaert R, Lambert J, et al; Halo naevi with associated vitiligo-like depigmentations: pathogenetic hypothesis. J Eur Acad Dermatol Venereol. 2012 Jun;26(6):755-61. doi: 10.1111/j.1468-3083.2011.04160.x. Epub 2011 Jun 23.
- Mulekar SV, Issa AA, Eisa AA; Treatment of halo nevus with a 308-nm excimer laser: a pilot study. J Cosmet Laser Ther. 2007 Dec;9(4):245-8.
- Mahajan BB, Garg G; Tattooing with electrocauterization: a cosmetically acceptable therapeutic modality for a single halo naevus. Indian J Dermatol Venereol Leprol. 2002 Sep-Oct;68(5):288-9.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 13 Dec 2027
14 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free