Keratoacanthoma
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 23 Nov 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What are keratoacanthomas?
Keratoacanthomas (KAs) are very rapidly growing squamo-proliferative lesions that look like well-differentiated squamous cell carcinomas (SCCs) pathologically. Keratoacanthomas are characterised by rapid growth over a few weeks to months, followed by spontaneous resolution over 4-6 months in most cases.
Keratoacanthomas are benign epidermal growths and not a malignant variant of SCC.1
How common are keratoacanthomas? (Epidemiology)
Back to contentsIncidence is estimated at 1 in 1,000.
Peak incidence occurs in those aged over 60 years. It is rare in young adults.
It is uncommon in darker-skinned patients.
Males are twice as often affected as females.
Epidemiological data are similar to SCC and Bowen's disease in terms of age, sex and the site of lesions.
Risk factors
Sunlight and chemical carcinogens have been implicated.
Trauma, genetic factors and immunocompromised status have also been associated.
Industrial workers exposed to pitch and tar have a higher incidence of both keratoacanthoma and SCC.
Continue reading below
Keratoacanthoma symptoms
Back to contentsTypically, rapid growth over a few weeks to months, followed by a slow spontaneous resolution over 4-6 months (but may take up to one year).
Most occur on sun-exposed areas - eg, the face, neck, and dorsum of hands and forearms.
They are usually solitary and begin as firm, round, skin-coloured or reddish papules that rapidly progress to dome-shaped nodules with a smooth shiny surface. A central crater of ulceration may develop, or a keratin plug that may project like a horn.
They leave a residual scar if not excised.
A recent large systematic review has shown that none of the cases of keratoacanthoma from 113 published articles resulted in death or distant metastases. This was compared with 429 cases of SCC of the skin, with 61 cases of metastases and 24 deaths as a direct result of SCC. The authors clearly state that the biological behaviour of the keratoacanthomas and SCCs is distinct and evident.1
Generalised eruptive keratoacanthoma (GEKA) of Grzybowski is a sporadically occurring, extremely rare variant of KA characterised clinically by severely pruritic, generalised eruption of numerous small follicular papules, often with a central keratotic plug, and histologically by typical features of solitary keratoacanthoma.2 .
Keratoacanthoma
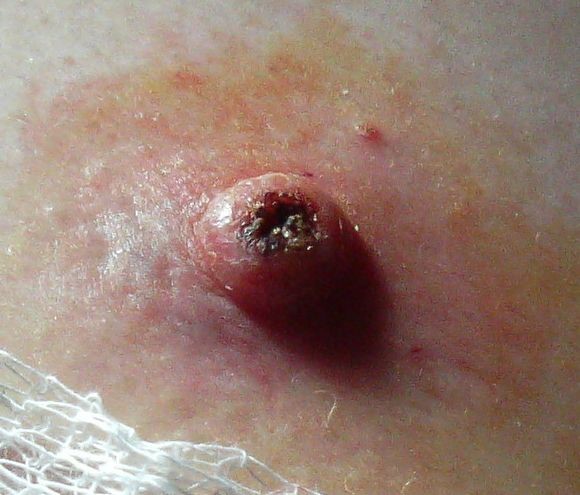
© Jmarchn, CC BY-SA 3.0, via Wikimedia Commons
Differential diagnosis3 4
Back to contentsContinue reading below
Investigations
Back to contentsShave biopsy of keratoacanthoma is indistinguishable from invasive SCC. Therefore, excisional or deep incisional biopsy is required.
A recent study has demonstrated that there is a large regional variation in the diagnosis of keratoacanthoma and SCCs in Great Britain and Ireland.5
This is because microscopic differentiation between these two entities is often problematic, and sometimes impossible.6
Keratoacanthoma treatment and management
Back to contentsAs they are hard to distinguish from SCCs, patients with suspected keratoacanthomas should be referred under the two-week waiting system. However, the patient can be reassured that they will not cause harm.
Complete excision is the treatment of choice for all skin lesions thought to be keratoacanthoma.
Medical treatment is reserved for when surgical intervention is not possible - eg, multiple lesions not amenable to surgery because of size or location.
Treatments that have produced some success include systemic retinoids (eg, isotretinoin), intralesional methotrexate, 5-fluorouracil, bleomycin and steroids, and topical imiquimod, and 5-fluorouracil.7 8
Prognosis
Back to contentsPrognosis is excellent following excisional surgery. Recurrence after surgical resection is rare.9
Without surgery, prognosis is usually good; however, there is a major controversy over the natural behaviour of KA. keratoacanthomas have been described as benign lesions, but also as variants of SCC.6
Prevention of keratoacanthomas
Back to contentsPatient education in sun-protection is important.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Keratoacanthoma; DermNet NZ
- Zito PM, Scharf R; Keratoacanthoma. StatPearls, Aug 2022.
- Keratoacanthoma; Primary Care Dermatology Society.
- Savage JA, Maize JC Sr; Keratoacanthoma clinical behavior: a systematic review. Am J Dermatopathol. 2014 May;36(5):422-9. doi: 10.1097/DAD.0000000000000031.
- Nofal A, Assaf M, Nofal E, et al; Generalized eruptive keratoacanthoma: proposed diagnostic criteria and therapeutic evaluation. J Eur Acad Dermatol Venereol. 2014 Apr;28(4):397-404. doi: 10.1111/jdv.12226. Epub 2013 Aug 6.
- Stefaniak AA, Chlebicka I, Krajewski P, et al; Do Not Judge a Book by its Cover: Masquerading as Keratoacanthoma. Acta Derm Venereol. 2020 Mar 12;100(6):adv00074. doi: 10.2340/00015555-3423.
- Riahi RR, Cohen PR; Malignancies with skin lesions mimicking keratoacanthoma. Dermatol Online J. 2013 Nov 15;19(11):20397.
- Carr RA, Houghton JP; Histopathologists' approach to keratoacanthoma: a multisite survey of regional variation in Great Britain and Ireland. J Clin Pathol. 2014 Apr 24. doi: 10.1136/jclinpath-2014-202255.
- Lammoglia-Ordiales L, Toussaint-Caire S, Contreras-Barrera M, et al; Assessment of syndecan-1 (CD138) and Ki-67 expression for differentiating keratoacanthoma and squamous cell carcinoma. J Drugs Dermatol. 2013 Mar;12(3):e53-8.
- Aubut N, Alain J, Claveau J; Intralesional methotrexate treatment for keratoacanthoma tumors: a retrospective case series. J Cutan Med Surg. 2012 May-Jun;16(3):212-7.
- Plachouri KM, Mulita F, Bousis D, et al; Successful treatment of a keratoacanthoma in a young patient with the application of topical 5% imiquimod cream. Clin Case Rep. 2021 Nov 6;9(11):e04920. doi: 10.1002/ccr3.4920. eCollection 2021 Nov.
- Liu XG, Liu XG, Wang CJ, et al; Lower lip recurrent keratoacanthoma: A case report. World J Clin Cases. 2022 Jul 16;10(20):6960-6965. doi: 10.12998/wjcc.v10.i20.6960.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 22 Nov 2027
23 Nov 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free