Lipoma
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 27 Feb 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Lumps article more useful, or one of our other health articles.
In this article:
Continue reading below
What is a lipoma?
Lipomas (lipomata) are slow-growing, benign, adipose tumours that are most often found in the subcutaneous tissues. They may also be found in deeper tissues such as the intermuscular septa, the abdominal organs, the oral cavity, the internal auditory canal, the cerebellopontine angle and the thorax. Most lipomas are asymptomatic, can be diagnosed with clinical examination and do not require treatment.
How common are lipomas? (Epidemiology)1
Back to contentsLipomas may be seen in all age groups, but usually first appear between 40 and 60 years of age.
Solitary lipomas are more common in women. Multiples - referred to as lipomatosis - are more common in men.
They have an estimated annual incidence of one per 1,000 of the population.
Congenital lipomas have been observed in children.2
Continue reading below
Variants
Back to contentsFamilial multiple lipomatosis
This is an autosomal dominant condition found most frequently in men. It is characterised by widespread symmetrical lipomas appearing most often over the extremities and trunk.3
Gardner's syndrome
Lipomatosis may also be associated with Gardner's syndrome, an autosomal dominant condition involving intestinal polyposis, cysts and osteomas.4
Dercum's disease
This is also known as adiposis dolorosa. It is rare and characterised by the presence of irregular painful lipomas, most often found on the trunk, shoulders, arms, forearms and legs. It is at least five times more common in women than it is in men and is often found in middle age. It also has asthenia and psychiatric disturbances as other prominent features.5
Madelung's disease
This is also known as benign symmetric lipomatosis. It is lipomatosis of the head, neck, shoulders and proximal upper extremities. Madelung's disease, often presents in men who drink excess alcohol, who may present with the characteristic 'horse collar' cervical appearance. Rarely, these patients experience swallowing difficulties, respiratory obstruction and even sudden death.6
Post-traumatic lipomas
Lipomas have been reported that have developed following blunt trauma. It is thought that at least some of these are due to herniation of fat through torn fascia. The resulting swelling is referred to as a 'pseudo-lipoma'.7
Liposarcoma
Back to contentsMalignancy is rare but can be found in a lesion with the clinical appearance of a lipoma. Liposarcoma presents in a fashion similar to that of a lipoma and appears to be more common in the retroperitoneum, on the shoulders and lower extremities.
Some recommend complete excision of a lipoma to exclude a possible liposarcoma, especially in fast-growing lesions. Pre-operative radiography may be a suitable alternative in some cases.8 Both ultrasound and magnetic resonance imaging (MRI) have been used with some success to differentiate lipomas and liposarcomas but are not entirely reliable.9 10 Other modalities such as computerised tomography (CT) scanning are occasionally required.11 Alternatively, fine-needle aspiration may be used to evaluate suspicious lesions.12 National Institute for Health and Care Excellence (NICE) guidelines advise urgent ultrasound for unexplained soft tissue lumps which are increasing in size, with two-week wait referral if ultrasound findings are suspicious or uncertain (within 48 hours for children).13 Local guidelines and protocols may differ.
Tumours that have characteristics consistent with a malignant liposarcoma include those that are:14
Greater than 5 cm in diameter.
Located in the extremities, retroperitoneally, in the groin, in the scrotum or in the abdominal wall.
Deep (beneath or fixed to superficial fascia).
Exhibiting malignant behaviour (rapid growth or invasion into nerve or bone).
Continue reading below
Lipoma symptoms (presentation)
Back to contentsA lipoma is usually a soft or firm nodule, size 0.5-10 cm, with a smooth normal surface and skin-coloured.
While about 80% of lipomas are less than 5 cm in diameter, some can reach more than 20 cm and weigh several kilograms.
Superficial subcutaneous lipoma
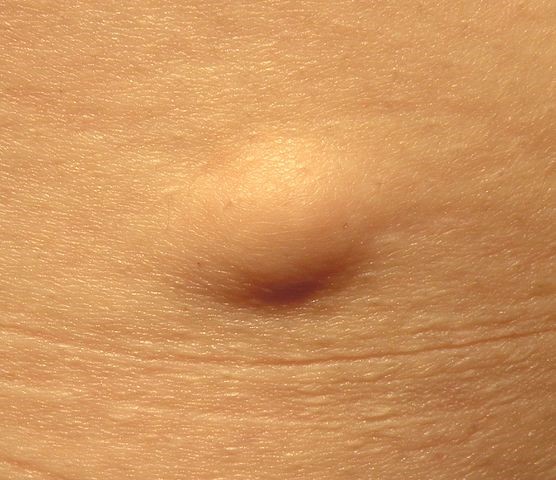
© By Jmarchn (Own work), via Wikimedia Commons
They are usually situated deep in the fatty layer with normal skin overlying them and should be mobile beneath the surface.
They are round or irregular in shape and may be single or multiple.
Lipomas usually present as non-painful, round, mobile masses with a characteristic soft, doughy feel.
Most lipomas are asymptomatic but they can cause pain when they compress nerves.
Diagnosis of lipomas
Back to contentsThis is usually made on clinical appearance alone. Any doubt should prompt referral for imaging or specialist opinion. Ultrasound, MRI and CT scans are all used, depending on availability and index of suspicion. MRI is the imaging method of choice.15 Biopsy is not usually required if MRI is available.
Differential diagnosis
Back to contentsEpidermoid cyst - these may be differentiated by the punctum in their surface and also by their site in the dermis, attached to the surface.
Subcutaneous tumours.
Nodular fasciitis.
Liposarcoma.
Metastatic disease.
Nodular subcutaneous fat necrosis.
Weber-Christian panniculitis (recurring inflammation in the fat layer of the skin).
Vasculitic nodules.
Rheumatic nodules.
Infections - eg, onchocerciasis.
Haematoma.
Management of lipomas
Back to contentsThey can be left alone. The size usually plateaus after initial growth.
They may need to be removed for cosmetic reasons, because of compression of surrounding structures or if the diagnosis is uncertain.
Because lipomas generally do not infiltrate into surrounding tissue, they can usually be shelled out easily during excision.
Minimal scarring can be achieved with a technique called segmental extraction - a small stab incision followed by blind dissection of the lipoma and extraction in a segmental fashion.10
Non-excisional treatment of lipomas includes steroid injections and liposuction.10
Further reading and references
- Soft tissue tumors: Lipoma/benign lipomatous tumors; Atlas of Genetics and Cytogenetics in Oncology and Haematology, 2013
- Pachani AB, Shojai AR, Gautam R, et al; A giant congenital lipoma over the back. Indian J Surg. 2010 Jul;72(Suppl 1):361-2. doi: 10.1007/s12262-010-0111-7. Epub 2010 Oct 20.
- Lee CH, Spence RA, Upadhyaya M, et al; Familial multiple lipomatosis with clear autosomal dominant inheritance and onset in early adolescence. BMJ Case Rep. 2011 Feb 17;2011. pii: bcr1020103395. doi: 10.1136/bcr.10.2010.3395.
- Chatziralli IP, Papazisis L, Sergentanis TN; Incomplete Gardner's syndrome with blepharoptosis as the first symptom. Int Ophthalmol. 2013 Apr 12.
- Hansson E, Svensson H, Brorson H; Review of Dercum's disease and proposal of diagnostic criteria, diagnostic methods, classification and management. Orphanet J Rare Dis. 2012 Apr 30;7:23. doi: 10.1186/1750-1172-7-23.
- Suresh Chandran CJ, Godge YR, Oak PJ, et al; Madelung's disease with myopathy. Ann Indian Acad Neurol. 2009 Apr;12(2):131-2. doi: 10.4103/0972-2327.53086.
- Rathi NV, Dahake PT, Thakre K, et al; Traumatic pseudo-lipoma in 3-year-old child. Contemp Clin Dent. 2012 Oct;3(4):487-90. doi: 10.4103/0976-237X.107451.
- Jones AP, Lewis CJ, Dildey P, et al; Lipoma or liposarcoma? A cautionary case report. J Plast Reconstr Aesthet Surg. 2012 Jan;65(1):e11-4. doi: 10.1016/j.bjps.2011.08.004. Epub 2011 Aug 23.
- Brisson M, Kashima T, Delaney D, et al; MRI characteristics of lipoma and atypical lipomatous tumor/well-differentiated liposarcoma: retrospective comparison with histology and MDM2 gene amplification. Skeletal Radiol. 2013 May;42(5):635-47. doi: 10.1007/s00256-012-1517-z. Epub 2012 Sep 18.
- Nguyen T, Zuniga R; Skin conditions: benign nodular skin lesions. FP Essent. 2013 Apr;407:24-30.
- Weerakkody Y et al; Liposarcoma, Radiopaedia.org
- Jagtap SV, Nikumbh DB, Jagtap SS, et al; Huge dedifferentiated liposarcoma of the left thigh with a high grade fibrosarcomatous differentiation and a local recurrence. J Clin Diagn Res. 2013 Mar;7(3):553-6. doi: 10.7860/JCDR/2013/4610.2823. Epub 2013 Mar 1.
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated April 2026)
- Costea R, Vasiliu E, Zarnescu NO, et al; Large thigh liposarcoma--diagnostic and therapeutic features. J Med Life. 2011 May 15;4(2):184-8. Epub 2011 May 25.
- Abd Rabou A et al; Lipoma; Radiopaedia.org
Continue reading below
About the author

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 26 Feb 2028
27 Feb 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free