Localised scleroderma
Morphoea
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 17 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Localised scleroderma article more useful, or one of our other health articles.
In this article:
Continue reading below
What is localised scleroderma?
Localised scleroderma, also called morphoea or morphea, is a disorder of excessive collagen deposition leading to thickening of the dermis and sometimes the subcutaneous tissues. The word scleroderma means 'hard skin' and in localised scleroderma, fat, fascia, muscle and bone may also be affected but not internal organs as in systemic scleroderma. See the separate Systemic Sclerosis (Scleroderma) article.
The most widely used classification for localised scleroderma is the Mayo Clinic Classification, in which there are 5 groups:1
Plaque morphoea: the most frequent form in adults; well-circumscribed and typically confined to the dermis.
Generalised morphoea: defined as morphoea plaques involving more than 2 body sites. It is more common in women.
Bullous morphoea: a rare form of morphea characterised by the appearance of bullae or erosions on morphoea plaques.
Linear scleroderma: characterised by one or more linear streaks of cutaneous induration that may involve dermis, subcutaneous tissue, muscle and underlying bone. Linear scleroderma is often seen in children and adolescents, and is the most frequent form of scleroderma in childhood. Includes subtypes that involve the head and face, linear scleroderma ‘en coup de saber' (LScs) and progressive facial hemiatrophy (PFH),
Deep morphoea: usually manifests itself as a single lesion on the upper trunk, near the spine. The overlying skin may have a normal appearance, an atrophic appearance or be hardened, and will almost always be depressed or adhered to the deep plane. It is usually asymptomatic and is not associated with visceral involvement.
How common is localised scleroderma? (Epidemiology)
Back to contentsLocalised scleroderma is an uncommon condition where the affected person has areas of thickened skin. Studies of incidence and prevalence are inadequate; the actual numbers are likely to be far higher because many cases may not come to medical attention. However, a relatively recent study reports incidence in children (under the age of 16 years) in the UK and Ireland to be 3.4 per million per year.2
Up to half of all cases occur in children. Prevalence is similar in adults and children; however, children are 90% more likely to have localised scleroderma than the systemic disease.1 The most common age of disease onset in children is 5-10 years.2 3 Peak incidence in adults is in the 5th decade.1 Women are at least twice as likely as men to be affected.4 When acquired in childhood, the disease tends to take a more severe form.5
Continue reading below
What causes localised scleroderma? (Aetiology)
Back to contentsThe cause of localised scleroderma is unknown. It is thought that a genetic predisposition may lead to an immunologically mediated cytokine release, causing inflammation, dysfunction of the connective tissue metabolism and subsequent fibrosis.6 It appears to be debatable whether there is any risk of progression to systemic sclerosis; however, although the pathogenesis is similar, it is probably a completely separate disease.7 8
In some cases it has been thought to follow:4
Tick bites - it has been associated with Lyme disease.
Measles and other viral infections.
Localised injury.
Pregnancy.
Autoimmune diseases, including vitiligo, diabetes, lichen sclerosus and lichen planus.
Radiotherapy. It may be as common as 2 in every 1,000 patients treated with radiotherapy.9
A few familial cases have been reported. People with localised scleroderma tend to have a family history of autoimmune disease.8
Localised scleroderma symptoms (presentation)4
Back to contentsPlaque morphoea
This is the most common type of morphoea:
Plaques are thickened, usually oval patches of skin between 1-20 cm (or greater) in diameter.
They start as a mauve colour, then change to ivory white in the middle with a lilac edge over several months. Long-standing plaques may be brown.
Their surface is hairless, smooth and shiny. They tend not to sweat. Several asymmetrical plaques may be present on both sides of the trunk and limbs.
Sometimes the surface is hyperpigmented with very little to feel.
Morphea located on the back of a 16 year old Caucasian woman
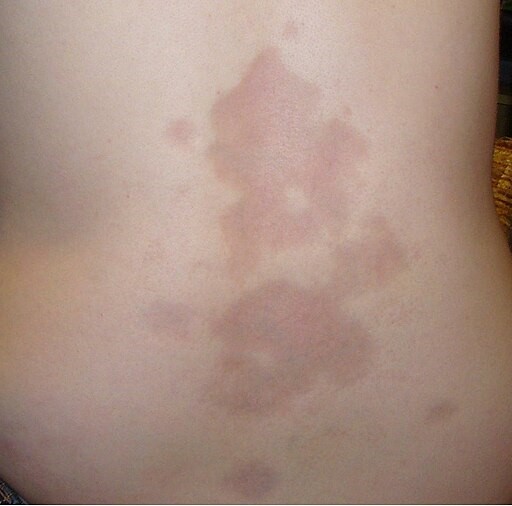
© Leith C Jones at English Wikipedia, CC BY 3.0, via Wikimedia Commons
Superficial morphoea
Middle-aged women usually present with symmetrical, mauve-coloured patches in the skin folds.
They are particularly common in the groin, armpits and under the breasts.
Linear morphoea
This is the most common form in children:
It may present on the scalp/forehead and limbs. This is most often found on the limb of a child.
A long and narrow plaque may be associated with underlying contractures.
A deep form affecting the scalp is called 'en coup de sabre' - a sabre cut. The hair is lost permanently and the underlying skull bone may shrink.
Pansclerotic disabling morphoea
This is rare:
It affects children and results in extensive hardening of skin and underlying muscle.
The growth of bones may be affected.
It can lead to joint contractures, non-healing ulcers and squamous cell carcinoma.
Generalised morphoea
Four or more plaques affecting two or more body regions. There may be widespread skin thickening over the trunk.
Parry-Romberg syndrome
This is a rare neurocutaneous disorder:
Linear scleroderma is associated with progressive facial hemiatrophy, migraine, facial pain and epilepsy.10
Atrophoderma of Pierini and Pasini
Depression in the skin caused by significant loss of subcutaneous tissue.
It is possible for several types to be present in one patient.
Continue reading below
Investigations
Back to contentsBlood tests have little role in assessment of localised scleroderma, although confirmatory tests are sometimes done to assist in diagnosis. Polyclonal increases in immunoglobulin G and M may occur, especially in patients with linear and deep morphoea. Autoantibodies (eg, rheumatoid factor, antinuclear antibodies) are frequently positive. The autoantibody profile differs from systemic sclerosis (SSc) however. In SSc, the vast majority are positive for anti-nuclear antibody (ANA), whereas this varies from 20-80% in localised scleroderma.8 The SSc-specific autoantibodies are not usually found in people with localised scleroderma.
A presumptive diagnosis can frequently be made on clinical findings. Skin biopsy is recommended only in the case of diagnostic doubt with other scleroderma like disorders (scleromyxoedema, scleroedema, nephrogenic systemic fibrosis).11
Imaging may be helpful in cases of linear or deep morphoea where involvement of the underlying bone is suspected. It can also be used to monitor paediatric patients for potential growth defects. Ultrasound is increasingly useful to monitor underlying disease activity.12
Differential diagnosis
Back to contentsInfiltrating secondary neoplasia is a rare possibility.
A white atrophic surface can also be due to lichen sclerosus et atrophicus.
Brown pigmentation on the surface is most likely to be due to post-inflammatory hyperpigmentation rather than morphoea.
In very young infants, early skin changes may be misdiagnosed as port-wine stains.13
SSc. (Skin changes associated with Raynaud's phenomenon and other associated vascular and systemic features.)
Localised scleroderma treatment and management
Back to contentsAll suspected cases should be referred for diagnosis.
Unfortunately there is no available, effective treatment for most cases of localised scleroderma. As no truly effective treatment yet exists for localised scleroderma, management must be based on the extent and the severity of the disease, and focus primarily on the risk of deformities and movement limitation. Physiotherapy may be helpful to prevent joint contractures in severe disease.14
There is evidence for efficacy of the following treatment options:6 8
Ultraviolet B (UVB) phototherapy for superficial skin involvement.
UVA phototherapy for deeper skin involvement. Efficacy has been proven, although there is no certainty yet about the long-term safety and the risk of skin cancer.15
Immunosuppression. The best evidence is for methotrexate +/- systemic corticosteroids for involvement of underlying tissues and for rapidly progressive or severe disease. There has been some work to attempt to standardise treatment regimens.5 Mycophenolate mofetil is used as a second-line agent but the evidence base is less good.
Topical tacrolimus.16
Topical imiquimod.
Topical calcipotriol with or without betamethasone diproprionate.
Type of treatment is based on the type of localised scleroderma and its extent - for example:8
Limited superficial plaque morphoea may respond to topical treatment or local phototherapy.
Deep plaque morphoea may require phototherapy or systemic immunosuppression with methotrexate and steroids.
Linear morphoea is usually aggressively treated with immunosuppression.
Generalised morphoea is usually not suitable for topical therapy, due to the large surface area involved, so phototherapy or immunosuppression is usually required.
Prognosis
Back to contentsLocalised scleroderma is rarely life-threatening but may have a significant adverse effect on quality of life, as it can be disfiguring and disabling.
Generally the lesions gradually improve over a period of years and may even resolve spontaneously.
Plaque-type morphoea is usually active for several years then slowly softens, leaving brown staining and sometimes depressed areas of skin.
Linear morphoea tends to be more progressive and lasts longer but also eventually improves, although sometimes deposits of calcium arise within the lesions. It needs monitoring, as there may be reactivation after long dormant periods.17 There is a high likelihood of cosmetic sequelae.
Limbs affected by severe morphoea may be stiff and weak if there is muscle wasting. Growth may be affected and there may be limb length differences and joint contractures
Facial atrophy may develop.
There may be ocular and neurological sequelae where it presents on the head and neck of children. Neurological complications include seizures, headaches, peripheral neuropathy, vascular malformations, and behavioural changes.
Where the condition develops in childhood, it tends to have more of a relapsing and remitting course and to produce more severe lesions than that which arises for the first time in adulthood.18
Further reading and references
- Morphoea; Primary Care Dermatology Society. July 2023.
- Careta MF, Romiti R; Localized scleroderma: clinical spectrum and therapeutic update. An Bras Dermatol. 2015 Jan-Feb;90(1):62-73. doi: 10.1590/abd1806-4841.20152890.
- Herrick AL, Ennis H, Bhushan M, et al; Incidence of childhood linear scleroderma and systemic sclerosis in the UK and Ireland. Arthritis Care Res (Hoboken). 2010 Feb;62(2):213-8. doi: 10.1002/acr.20070.
- Weibel L, Laguda B, Atherton D, et al; Misdiagnosis and delay in referral of children with localized scleroderma. Br J Dermatol. 2011 Dec;165(6):1308-13. doi: 10.1111/j.1365-2133.2011.10600.x. Epub 2011 Nov 2.
- Morphoea; DermNet NZ
- Li SC, Torok KS, Pope E, et al; Development of consensus treatment plans for juvenile localized scleroderma: a roadmap toward comparative effectiveness studies in juvenile localized scleroderma. Arthritis Care Res (Hoboken). 2012 Aug;64(8):1175-85. doi: 10.1002/acr.21687.
- Kreuter A; Localized scleroderma. Dermatol Ther. 2012 Mar-Apr;25(2):135-47. doi: 10.1111/j.1529-8019.2012.01479.x.
- Fett NM; Morphea (localized scleroderma). JAMA Dermatol. 2013 Sep;149(9):1124. doi: 10.1001/jamadermatol.2013.5079.
- Fett N; Scleroderma: nomenclature, etiology, pathogenesis, prognosis, and treatments: facts and controversies. Clin Dermatol. 2013 Jul-Aug;31(4):432-7. doi: 10.1016/j.clindermatol.2013.01.010.
- Alhathlool A, Hein R, Andres C, et al; Post-Irradiation Morphea: Case report and review of the literature. J Dermatol Case Rep. 2012 Sep 28;6(3):73-7. doi: 10.3315/jdcr.2012.1106.
- Maletic J, Tsirka V, Ioannides P, et al; Parry-Romberg Syndrome Associated with Localized Scleroderma. Case Rep Neurol. 2010 Jun 1;2(2):57-62.
- Rongioletti F, Ferreli C, Atzori L, et al; Scleroderma with an update about clinico-pathological correlation. G Ital Dermatol Venereol. 2018 Apr;153(2):208-215. doi: 10.23736/S0392-0488.18.05922-9. Epub 2018 Jan 24.
- Zulian F, Cuffaro G, Sperotto F; Scleroderma in children: an update. Curr Opin Rheumatol. 2013 Sep;25(5):643-50. doi: 10.1097/BOR.0b013e3283641f61.
- Kanoh H, Shu E, Ichiki Y, et al; Localized scleroderma presenting as port-wine stains: report of two cases and a literature review. Acta Derm Venereol. 2015 Nov;95(8):1003-4. doi: 10.2340/00015555-2100.
- Bielsa Marsol I; Update on the classification and treatment of localized scleroderma. Actas Dermosifiliogr. 2013 Oct;104(8):654-66. doi: 10.1016/j.adengl.2012.10.012. Epub 2013 Aug 13.
- Kerr AC, Ferguson J, Attili SK, et al; Ultraviolet A1 phototherapy: a British Photodermatology Group workshop report. Clin Exp Dermatol. 2012 Apr;37(3):219-26. doi: 10.1111/j.1365-2230.2011.04256.x. Epub 2012 Jan 25.
- Cantisani C, Miraglia E, Richetta AG, et al; Generalized morphea successfully treated with tacrolimus 0.1% ointment. J Drugs Dermatol. 2013 Jan;12(1):14-5.
- Piram M, McCuaig C, Saint-Cyr C, et al; Short And Long Term Outcome Of Linear Morphea In Children. Br J Dermatol. 2013 Sep 6. doi: 10.1111/bjd.12606.
- Saxton-Daniels S, Jacobe HT; An evaluation of long-term outcomes in adults with pediatric-onset morphea. Arch Dermatol. 2010 Sep;146(9):1044-5.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 15 Aug 2028
17 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free