Roundworms
Nematodes
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 13 Dec 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Roundworms article more useful, or one of our other health articles.
In this article:
Continue reading below
What are roundworms (nematodes)?
Roundworms (nematodes) have elongated, bilaterally long cylindrical bodies which contain an intestinal system and a large body cavity. Parasitic nematodes vary in length from several millimetres to approximately 2 metres and have larval stages and adult worms of both sexes. Approximately 60 species of roundworms are parasites of humans.1
Some roundworm infections can be transmitted directly from person to person but, in others, the nematode eggs must mature outside the host. The parasites may spend a part of their life cycle in the soil before becoming infective to humans. Nematodes commonly parasitic on humans include (click links below for separate articles which provide more detail):
Ascaris Lumbricoides.
Roundworm ascaris lumbricoides
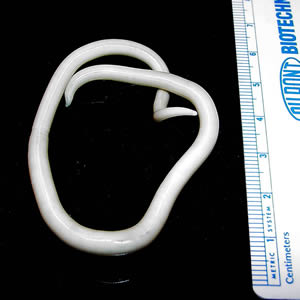
© CDC, Public Domain, via Wikimedia Commons
Filariasis, which is caused by thread-like filarial roundworms (nematodes) in the family Filarioidea (also known as 'filariae'). There are eight known filarial roundworms which use humans as the host. These are divided into three groups:
Lymphatic Filariasis - caused by the worms Wuchereria bancrofti, Brugia malayi, and Brugia timori.
Cutaneous Filariasis - caused by Loa loa (the African eye worm), Mansonella streptocerca and Onchocerca volvulus.
Body Cavity Filariasis - caused by the worms Mansonella perstans and Mansonella ozzardi.
Trichuriasis (Whipworm).
Trichinellosis.
Angiostrongyliasis.
Strongyloidiasis.
Gnathostomiasis.
Anisakiasis.
Cutaneous larva migrans is caused by skin penetration and subsequent migration of larvae of various roundworm parasites.
Helminth infections can affect the immune system in positive and negative ways. The host can benefit from suppression of collateral damage during parasite infection and from reduced allergic, autoimmune, and inflammatory reactions. However, helminth infection can also be detrimental in reducing vaccine responses, increasing susceptibility to co-infection and potentially reducing the body's protection against tumours.2
How common are roundworms (nematodes)?
Back to contentsThe bowel of a child living in poverty in a developing country is likely to be parasitised with at least one nematode and, in many cases, multiple infection (eg, whipworms, ascaris, and hookworms), with resultant impairments in physical, intellectual, and cognitive development.1 3
The prevalence of roundworm infections throughout the world is generally increasing but varies according to levels of poverty, natural disasters and human conflicts.4
The spread of infection is also increasing in line with increased travel and mobility (eg, angiostrongyliasis and anisakiasis). However, some eradication programmes (notably for guinea worm disease) have been effective in reducing the burden of infection.
Roundworm infections are rare in the UK. Infections diagnosed in the UK are likely to have been acquired abroad. Travellers and migrant populations are most often affected. It is estimated that up to 20% of migrants from endemic countries may have helminth infections at the time of their arrival in the UK.5
Continue reading below
Roundworm (nematode) treatment3
Back to contentsControl of roundworm (nematode) infections is based on drug treatment, improved sanitation and health education.
Antihelmintic drugs (eg, mebendazole, albendazole and tiabendazole) are often used for both symptomatic infections and for large-scale prevention of morbidity in children living in endemic areas. This has resulted in improvements in child health and education after deworming.
Concerns about the sustainability of periodic deworming with available drugs and the emergence of resistance mean that a great deal more needs to be done in terms of new drugs and developing effective vaccines, as well as education and alleviating poverty.
See the British National Formulary (BNF) treatment summary for helminth infections for further recommendations for treatment, and contact details for further advice on prophylaxis and treatment in the UK.6
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Parasites A-Z; Centers for Disease Control and Prevention
- Cox FEG; History of Human Parasitology
- Stepek G, Buttle DJ, Duce IR, et al; Human gastrointestinal nematode infections: are new control methods required? Int J Exp Pathol. 2006 Oct;87(5):325-41.
- Maizels RM, McSorley HJ; Regulation of the host immune system by helminth parasites. J Allergy Clin Immunol. 2016 Sep;138(3):666-675. doi: 10.1016/j.jaci.2016.07.007. Epub 2016 Jul 29.
- Bethony J, Brooker S, Albonico M, et al; Soil-transmitted helminth infections: ascariasis, trichuriasis, and hookworm. Lancet. 2006 May 6;367(9521):1521-32.
- Beyrer C, Villar JC, Suwanvanichkij V, et al; Neglected diseases, civil conflicts, and the right to health. Lancet. 2007 Aug 18;370(9587):619-27.
- Roundworm; NICE CKS, March 2018 (UK access only)
- Helminth infections; British National Formulary (BNF).
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 Dec 2027
13 Dec 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free