Pleural effusion aspiration
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 6 Aug 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Pleural effusion article more useful, or one of our other health articles.
In this article:
Synonym: thoracentesis, pleural tap
See also the separate Pleural effusion article.
Continue reading below
What is pleural effusion aspiration?
Pleural aspiration (thoracocentesis) is the aspiration of a pleural effusion from the pleural space. The indications for pleural aspiration include aiding the diagnosis of a unilateral, suspected exudative pleural effusion, or excluding empyema as this requires urgent intercostal drainage.
Why is pleural effusion aspiration needed? (Indications)
Back to contentsPercutaneous pleural effusion aspiration is carried out:
To investigate the cause of pleural effusion
The British Thoracic Society (BTS) guidelines suggest that pleural aspiration should be reserved for the investigation of unilateral exudative pleural effusions. It should not be carried out if a unilateral or bilateral transudative effusion is suspected, unless there are atypical features or there is failure of response to therapy.1
As symptom relief for breathlessness
Urgent decompression of the pleural space may be required to alleviate respiratory distress.2
Repeated 'tapping' of fluid may be useful in palliative care. However, there is a high recurrence rate if pleurodesis (intrapleural instillation of a sclerosant) is not carried out simultaneously.3
Continue reading below
Relative contra-indications to pleural effusion aspiration
Back to contentsVery small volume of fluid.
Bleeding diathesis.
Anticoagulant therapy.
Mechanical ventilation (increased likelihood of tension pneumothorax or bronchopleural fistula if the lung is punctured).
Cutaneous disease over the proposed skin puncture site.
What happens during pleural effusion aspiration? (Procedure)
Back to contentsLungs and airways - pleural effusion
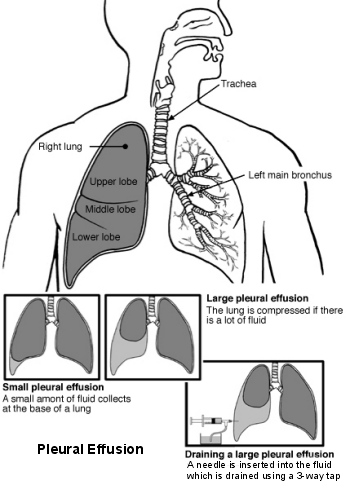
This can be performed in the clinic or by the bedside.1
Radiological guidance (particularly using ultrasound) is increasingly used and reduces the risk of complications.4
Sit the patient as upright as possible. A pillow can be used to support arms and head on an adjustable table or couch. If the patient leans forward too much it increases the risk of liver/spleen injury.
Use an aseptic technique throughout the procedure.
Use percussion to determine the upper level of fluid.
The conventional site for aspiration is posteriorly, approximately 10 cm lateral to the spine (mid-scapular line) and 1-2 intercostal spaces below the upper level of the fluid.
Mark the spot and clean the area using antiseptic.
Use local anaesthetic (5-10 ml of 1% lidocaine) to infiltrate the skin and underlying tissues. A 25G needle can be used for this.
Avoid the intercostal nerves and vessels that run immediately beneath the rib by inserting the needle just above the upper border of the rib, below your mark.
You can confirm the correct location for pleural aspiration by aspirating a small amount of fluid through this smaller needle.
Attach a 21G needle to a 50 ml syringe.
Again, avoid the intercostal nerves and vessels by inserting the needle just above the upper border of the rib below your mark. Aspirate while you are advancing the needle.
50-100 ml of fluid is usually adequate for diagnostic purposes.
Look at the fluid obtained and note any odour: purulent fluid suggests empyema; milky, opalescent fluid suggests chylothorax; grossly bloody fluid suggests haemothorax; anaerobic infection has a pungent odour.
Separate the pleural fluid into different sterile pots to be sent for biochemistry, microbiology, cytology ± immunology. Some fluid should also be added to blood culture bottles.
A post-procedure CXR to look for pneumothorax is not generally needed provided the patient is asymptomatic and the procedure was uncomplicated.
If the procedure is being carried out to relieve breathlessness, a greater volume of fluid usually needs to be drained:
Use a 14G intravenous cannula instead of the 21G needle.
Administer oxygen and use pulse oximetry throughout the procedure.
Follow the same steps as above.
When the cannula is inserted, remove the stylet and connect a closed pleural aspiration kit.
The fluid should still be sent for analysis.
It is best to remove fluid slowly.
Monitor for chest pressure or pain during fluid removal. This can be a sign of lung entrapment due to extensive pleural involvement or endobronchial obstruction which will prevent re-expansion of the lung when the fluid is removed. If this occurs, stop the procedure.
Rarely, if more than 1.5 litres of fluid are drained off, fluid shifts can cause haemodynamic instability or pulmonary oedema. The recommended fluid drainage limit is 1.5 litres.4
A chest drain can also be inserted for pleural fluid drainage.56
Continue reading below
Investigations to be requested on the pleural fluid
Back to contentsThe BTS suggests the following initial investigations:1
Microbiology
It is generally recommended that pleural fluid samples from pleural effusions of unknown cause be cultured for bacteria, mycobacteria and fungi. However, studies confirm that the positive yield of smears and cultures on pleural fluid specimens is low in the general population and in cancer patients.7
Send one pot for Gram stain, acid-alcohol fast bacilli (AAFB) stain, microscopy, culture and sensitivity.
Send some fluid in blood culture bottles (increases yield, especially for anaerobic organisms).
Biochemistry
Send one pot for protein, lactate dehydrogenase (LDH) and pH.
Cytology
Send a 20 ml sample in a sterile pot for cytological examination. Some cytologists prefer samples to be sent in a citrate bottle to prevent clots (discuss with your laboratory).
The sample needs to be fresh.
Malignant effusions can be diagnosed by pleural fluid cytology alone in 60% of cases.8 A second sample can increase diagnostic yield.
Additional investigations should be requested under specific circumstances:
If empyema is suspected send some fluid for centrifuge to differentiate from chylothorax.
If chylothorax is suspected send some fluid for centrifuge, cholesterol and triglyceride levels and investigation for the presence of cholesterol crystals and chylomicrons.
If haemothorax is suspected, or the pleural fluid is grossly bloody, send some fluid for haematocrit level.
If rheumatoid disease is suspected send some fluid for glucose and complement levels.
If pancreatitis is suspected send some fluid for amylase level.
Interpretation of pleural fluid results
Back to contentsSee the separate Pleural effusion article.
Complications of pleural effusion aspiration4910
Back to contentsPain during and after the procedure at the puncture site.
Pneumothorax complicates 12-30% of pleural aspirations but chest drain treatment is required in <5% of these.
Persistent air leak.
Bleeding (may be cutaneous or intrapleural).
Empyema.
Inadvertent liver/spleen puncture.
Re-expansion pulmonary oedema.
Malignant metastatic seeding (rare).
Further reading and references
- Breathlessness; NICE CKS, July 2024 (UK access only)
- Jany B, Welte T; Pleural Effusion in Adults-Etiology, Diagnosis, and Treatment. Dtsch Arztebl Int. 2019 May 24;116(21):377-386. doi: 10.3238/arztebl.2019.0377.
- Ferreiro L, Porcel JM, Valdes L; Diagnosis and Management of Pleural Transudates. Arch Bronconeumol. 2017 Nov;53(11):629-636. doi: 10.1016/j.arbres.2017.04.018. Epub 2017 Jun 19.
- Manoharan A, Argaez C; Pleuroscopy for the Diagnosis of Cancer in Patients with Pleural Effusion: A Review of the Diagnostic Accuracy, Safety, Cost-Effectiveness and Guidelines. Canadian Agency for Drugs and Technologies in Health. Apr 2020.
- British Thoracic Society Guideline for pleural disease; British Thoracic Society - BMJ (2023).
- Maslove DM, Chen BT, Wang H, et al; The diagnosis and management of pleural effusions in the ICU. J Intensive Care Med. 2013 Jan-Feb;28(1):24-36. doi: 10.1177/0885066611403264. Epub 2011 Nov 11.
- Mierzejewski M, Korczynski P, Krenke R, et al; Chemical pleurodesis - a review of mechanisms involved in pleural space obliteration. Respir Res. 2019 Nov 7;20(1):247. doi: 10.1186/s12931-019-1204-x.
- Corcoran JP, Psallidas I, Wrightson JM, et al; Pleural procedural complications: prevention and management. J Thorac Dis. 2015 Jun;7(6):1058-67. doi: 10.3978/j.issn.2072-1439.2015.04.42.
- Zisis C, Tsirgogianni K, Lazaridis G, et al; Chest drainage systems in use. Ann Transl Med. 2015 Mar;3(3):43. doi: 10.3978/j.issn.2305-5839.2015.02.09.
- George RS, Papagiannopoulos K; Advances in chest drain management in thoracic disease. J Thorac Dis. 2016 Feb;8(Suppl 1):S55-64. doi: 10.3978/j.issn.2072-1439.2015.11.19.
- Bailey M, Eapen G, Ost D, et al; Routine Microbiologic Studies of Pleural Fluid Specimens in Cancer Patients. Am J Med. 2020 Feb;133(2):240-244. doi: 10.1016/j.amjmed.2019.07.022. Epub 2019 Aug 8.
- Karkhanis VS, Joshi JM; Pleural effusion: diagnosis, treatment, and management. Open Access Emerg Med. 2012 Jun 22;4:31-52. doi: 10.2147/OAEM.S29942. eCollection 2012.
- Daniels CE, Ryu JH; Improving the safety of thoracentesis. Curr Opin Pulm Med. 2011 Jul;17(4):232-6. doi: 10.1097/MCP.0b013e328345160b.
- Duncan DR, Morgenthaler TI, Ryu JH, et al; Reducing iatrogenic risk in thoracentesis: establishing best practice via experiential training in a zero-risk environment. Chest. 2009 May;135(5):1315-20. doi: 10.1378/chest.08-1227. Epub 2008 Nov 18.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Aug 2027
6 Aug 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free