Prurigo nodularis
Peer reviewed by Dr Laurence KnottLast updated by Dr Colin Tidy, MRCGPLast updated 17 Jan 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: nodular prurigo, Hyde's disease, picker nodules, lichen corneus obtusus, nodular lichen simplex chronicus, nodular neurodermatitis circumscripta
Continue reading below
What is prurigo nodularis?
Prurigo nodularis is a chronic, recalcitrant inflammatory skin condition characterised by pruritic nodules. The exact cause of the condition is unknown, although immune and neural dysregulation are indicated in driving the itch-scratch cycle1 .
The constant scratching leads to the development of discrete, excoriated, nodular, hyperpigmented/purpuric lesions with crusted or scaly surfaces. The scaling, thickening and hyperkeratosis of the skin, induced by scratching, is known as lichen simplex chronicus which may also present in a plaque-like form.
Prurigo nodularis predominantly affects the extensor aspects of the lower limbs but also commonly affects the arms and sometimes other areas of the body. There are increased dermal levels of neuropeptides such as substance P, calcitonin gene-related peptide and nerve growth factor, as well as an excess of eosinophils and mast cells2 .
People with prurigo nodularis also have a reduced intraepidermal nerve fibre density. Whether this represents a causative aetiology or arises as a result of chronic scratching and skin irritation is not known. One study found hypoplasia of epidermal sensory nerves in the skin of those with prurigo nodularis, even in areas where pruritus was not a problem3 .
Prurigo nodularis epidemiology
Back to contentsPrurigo nodularis appears to be relatively common, particularly among patients who have some of the associated/precipitating conditions; however, there are no surveys of its prevalence in the general population.
It is more common in middle-aged women4 .
Prurigo nodularis was common in HIV-positive patients before the advent of antiretroviral therapy (ART) but is now.relatively uncommon in treated patients5 . However, it is still prevalent where access to ART is limited. One study found that the development of prurigo nodularis in HIV patients was a sign of severe immunosuppression6 .
Continue reading below
Presentation
Back to contentsPrurigo nodularis
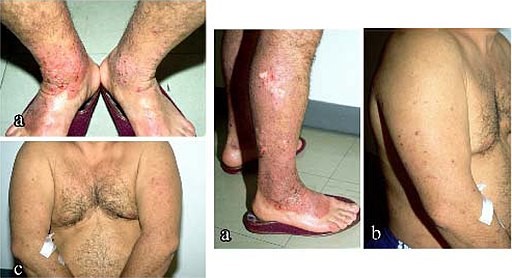
© Michael Katotomichelakis et al, CC BY 2.0, via Wikimedia Commons
Prurigo nodularis symptoms
It usually affects a middle-aged or older patient but may occur in children7 .
The patient complains of long-standing pruritus that is a constant problem in the affected areas.
There are specific sites that are identified as being itchy and on which pigmented nodular lesions later develop, usually symmetrically distributed.
Nodules are usually of constant size and they do not resolve spontaneously.
The number of nodules tends to increase over time.
There may be a history of one of the associated conditions (see 'Associated diseases', below).
Anxiety about the nature of the lesion and the itching is relatively common.
Up to 80% of patients have a personal/family history of atopic dermatitis, asthma or hay fever (compared to 25% of the general population)8 .
Signs
Nodules/papules:
≤2 cm in diameter.
Discrete.
Scaly.
Symmetrical distribution.
Firm.
Hyperpigmented or sometimes purpuric.
Usually on extensor surfaces of the legs/arms, and may occasionally affect the trunk.
There may be a few lesions or up to several hundred in some cases.
Patients may be observed to scratch repeatedly or rub the lesion during the consultation, often in preference to pointing them out when asked to indicate the problem.
Differential diagnosis9 10
Back to contentsThere is a wide-ranging differential:
Amyloidosis, nodular localised cutaneous.
Atypical fibroxanthoma.
Cutaneous horn.
Dermatological manifestations of gastrointestinal disease.
Dermatological manifestations of haematological disease.
Dermatological manifestations of renal disease.
Hyperkeratosis lenticularis perstans (Flegel's disease).
Knuckle pads.
Lymphocytoma cutis.
Lymphomatoid papulosis.
Mastocytosis (urticaria pigmentosa).
Milker's nodules.
Multicentric reticulohistiocytosis.
Mycobacterium marinum infection of the skin (from cleaning out tropical fish tanks).
Papulonecrotic tuberculids.
Pilomatrixoma.
Pretibial myxoedema.
Xanthomas.
Continue reading below
Associated diseases
Back to contentsPrurigo nodularis has a wide range of purported systemic precipitants, including:
Infective:
Psychological/psychiatric conditions14 .
Acute kidney injury.
The role of these illnesses as precipitants or comorbidities is unclear. They may just be a range of conditions which induce a propensity to skin irritation and unmask a tendency to localised itchiness of the skin.
Investigations8
Back to contentsPruritus screening blood tests (such as FBC, CRP, iron studies, U&Es, LFTs, TFTs, serum calcium, glucose) may help to detect any underlying renal, hepatic, metabolic or infective associated illness.
Biopsy of the lesions is recommended to exclude unusual or atypical presentations of other disease such as squamous cell carcinoma, mycobacterial infections, fungal infections and cutaneous lymphoma.
Patch testing to look for evidence of a contact sensitivity precipitant may be carried out in a dermatology clinic.
Dermoscopy may be helpful in differentiating various nodular pruritic conditions18 .
Direct immunofluorescence looking for antibody deposition in the skin may be necessary to differentiate from bullous pemphigoid if blisters develop.
Prurigo nodularis treatment and management8 199
Back to contentsTreatment typically relies on the use of topical or intralesional steroids. More severe or treatment-resistant cases often require phototherapy or systemic immunosuppressives. Thalidomide and lenalidomide can both be used in severe cases, but toxicity makes them less favourable. Opioid receptor antagonists and neurokinin-1 receptor antagonists represent two potential therapeutic agents which may effectively treat prurigo nodularis with a lower toxicity profile than thalidomide or lenalidomide20 .
Local treatments
These include:
Emollients - use frequently to cool and soothe itchy skin; menthol may be added to supplement this effect.
Steroids are used to decrease inflammation and pruritus and to soften and smooth nodules, usually topically or under occlusive dressings but may be given intralesionally or orally. Response is often variable.
Intranodular steroid injections are sometimes used.
Phenol and local anaesthetic creams have also been found to be helpful.
Coal tar ointment is sometimes used as an alternative to steroids.
Calcipotriol ointment is sometimes more effective than topical steroids.
Capsaicin cream induces itching and burning and ultimately may stop itch. It requires repeated applications 4-6 times daily.
Cryotherapy with liquid nitrogen can shrink the nodules and reduce their itch.
Pulsed dye laser may reduce the vascularity of individual lesions.
One study reported that hypnosis and acupuncture were beneficial21 .
Systemic therapies22
These include:
Antihistamines may help to control itch in some cases.
The response to systemic corticosteroids is very unpredictable.
Ciclosporin, methotrexate and azathioprine have been found to be effective in some cases.
Thalidomide has been shown to be quite effective in severe cases but carries a teratogenic and peripheral neuropathic risk23 .
Opiate-receptor antagonists, such as naltrexone, have shown some efficacy in treating itch.
Systemic retinoids, such as acitretin, may shrink the nodules and reduce itching.
Psoralen combined with ultraviolet A (PUVA) treatment may help but carries the risks of prolonged UV exposure.
There is anecdotal evidence of good response, in severe, refractory cases, to the immunomodulatory macrolide, roxithromycin, either alone, or combined with the anti-fibroblast agent, tranilast24 .
The immunomodulators tacrolimus and pimecrolimus have been found to be beneficial in small studies of steroid-unresponsive patients and patients with thin skin.
Gabapentin has been used to good effect. It can, however, cause sedation.
Psychological distress and depression in predisposed subjects may play a key role in inducing a pruritic sensation, leading to the scratching that perpetuates the condition (the 'itch/scratch cycle'). As with lichen simplex chronicus, it is thought that psychological factors play a role in causing and maintaining both conditions. One study found that anxiety and depression were common in prurigo nodularis patients14 . Approaches to address the psychodermatology include:
Cognitive behavioural therapy (CBT). However, there is little evidence of efficacy and patients must be open to a psychological model of their problem to have a good chance of responding25 .
Habit reversal therapy, originally developed to treat tics, has been used to break the 'itch/scratch' cycle26 .
Anxiolytic drugs may be helpful but there is a danger of dependence. Similarly, antidepressants such as amitriptyline or doxepin may be useful.
One study reported control of pruritus with oral ketotifen and topical antibiotics27 .
Consider referring the patient to a relevant specialist if you think the condition may be a manifestation of underlying systemic disease, particularly if HIV, malignancy, renal or liver disease is suspected. Referral should also be considered if all therapeutic options available in primary care have been exhausted9 .
Complications
Back to contentsPrurigo nodularis is a benign condition. However, it can cause severe functional impairment and morbidity due to poor control of the itching/scratching and psychological symptoms. Some lesions may become permanently pigmented or show scarring.
Prognosis
Back to contentsIt is unusual for lesions to resolve spontaneously. They may lessen in severity with treatment but tend to persist over time. If the itch/scratch cycle can be completely broken then there is a chance of cure but this is not the norm.
Further reading and references
- Oh CC, Li H, Lee W, et al; Biopsychosocial Factors Associated with Prurigo Nodularis in Endogenous Eczema. Indian J Dermatol. 2015 Sep-Oct;60(5):525. doi: 10.4103/0019-5154.164451.
- Mullins TB, Sharma P, Riley CA, et al; Prurigo Nodularis. StatPearls, Sept 2021.
- Leis M, Fleming P, Lynde CW; Prurigo Nodularis: Review and Emerging Treatments. Skin Therapy Lett. 2021 May;26(3):5-8.
- Zeidler C, Stander S; The pathogenesis of Prurigo nodularis - 'Super-Itch' in exploration. Eur J Pain. 2016 Jan;20(1):37-40. doi: 10.1002/ejp.767. Epub 2015 Sep 28.
- Schuhknecht B, Marziniak M, Wissel A, et al; Reduced intraepidermal nerve fibre density in lesional and nonlesional prurigo nodularis skin as a potential sign of subclinical cutaneous neuropathy. Br J Dermatol. 2011 Jul;165(1):85-91. doi: 10.1111/j.1365-2133.2011.10306.x.
- Neild GH, Garcia-Agudo R, Manzano R, et al; Prurigo nodularis in a woman with Stage-4 chronic kidney disease. NDT Plus. 2011 Oct;4(5):354. doi: 10.1093/ndtplus/sfr069. Epub 2011 Jun 7.
- Cedeno-Laurent F, Gomez-Flores M, Mendez N, et al; New insights into HIV-1-primary skin disorders. J Int AIDS Soc. 2011 Jan 24;14:5. doi: 10.1186/1758-2652-14-5.
- Magand F, Nacher M, Cazorla C, et al; Predictive values of prurigo nodularis and herpes zoster for HIV infection and immunosuppression requiring HAART in French Guiana. Trans R Soc Trop Med Hyg. 2011 Jul;105(7):401-4. Epub 2011 May 28.
- Amer A, Fischer H; Prurigo nodularis in a 9-year-old girl. Clin Pediatr (Phila). 2009 Jan;48(1):93-5. Epub 2008 Jul 22.
- Prurigo nodularis; DermNet NZ
- Saco M et al; Prurigo nodularis: Picking the right treatment, 2015.
- Jackson S et al; Differential Diagnosis for the Dermatologist, 2012.
- Saporito L, Florena AM, Colomba C, et al; Prurigo nodularis due to Mycobacterium tuberculosis. J Med Microbiol. 2009 Dec;58(Pt 12):1649-51. Epub 2009 Aug 6.
- Hernando-Harder AC, Booken N, Goerdt S, Singer MV, et al; Helicobacter pylori infection and dermatologic diseases. Eur J Dermatol. 2009 Sep-Oct;19(5):431-44. Epub 2009 Jun 15.
- Weisshaar E, Stander S; Prurigo nodularis in hepatitis C infection: result of an occupational disease? Acta Derm Venereol. 2012 Sep;92(5):532-3. doi: 10.2340/00015555-1209.
- Dazzi C, Erma D, Piccinno R, et al; Psychological factors involved in prurigo nodularis: A pilot study. J Dermatolog Treat. 2011 Aug;22(4):211-4. Epub 2010 Jul 28.
- Wu TP, Miller K, Cohen DE, et al; Keratoacanthomas arising in association with prurigo nodules in pruritic, actinically damaged skin. J Am Acad Dermatol. 2013 Sep;69(3):426-30. doi: 10.1016/j.jaad.2013.03.035. Epub 2013 May 10.
- Seradj MH, Naderi N, Peiman S, et al; Metastatic transitional cell carcinoma of the skin presenting as painful zosteriform eruptions. Oxf Med Case Reports. 2015 May 1;2015(5):281-3. doi: 10.1093/omcr/omv036. eCollection 2015 May.
- Shiotani A, Sakurane M, Furukawa F; Helicobacter pylori-positive patients with pruritic skin diseases are at increased risk for gastric cancer. Aliment Pharmacol Ther. 2004 Jul;20 Suppl 1:80-4.
- Errichetti E, Stinco G; The practical usefulness of dermoscopy in general dermatology. G Ital Dermatol Venereol. 2015 Oct;150(5):533-46. Epub 2015 Jun 18.
- Lee MR, Shumack S; Prurigo nodularis: a review. Australas J Dermatol. 2005 Nov;46(4):211-18; quiz 219-20.
- Kowalski EH, Kneiber D, Valdebran M, et al; Treatment-resistant prurigo nodularis: challenges and solutions. Clin Cosmet Investig Dermatol. 2019 Feb 28;12:163-172. doi: 10.2147/CCID.S188070. eCollection 2019.
- Samuels N, Sagi E, Singer SR, et al; Hypnosis and acupuncture (hypnopuncture) for prurigo nodularis: a case report. Am J Clin Hypn. 2011 Apr;53(4):283-92.
- Prurigo; Primary Care Dermatology Society, Last updated Nov 2021
- Sharma D, Kwatra SG; Thalidomide for the treatment of chronic refractory pruritus. J Am Acad Dermatol. 2015 Nov 11. pii: S0190-9622(15)02237-9. doi: 10.1016/j.jaad.2015.09.039.
- Horiuchi Y, Bae S, Katayama I; Uncontrollable prurigo nodularis effectively treated by roxithromycin and tranilast. J Drugs Dermatol. 2006 Apr;5(4):363-5.
- Shenefelt PD; Psychological interventions in the management of common skin conditions. Psychol Res Behav Manag. 2010;3:51-63. Epub 2010 Mar 26.
- Tey HL, Wallengren J, Yosipovitch G; Psychosomatic factors in pruritus. Clin Dermatol. 2013 Jan-Feb;31(1):31-40. doi: 10.1016/j.clindermatol.2011.11.004.
- Sharma AD; Oral ketotifen and topical antibiotic therapy in the management of pruritus in prurigo nodularis: a randomized, controlled, single-blind, parallel study. Indian J Dermatol. 2013 Sep;58(5):355-9. doi: 10.4103/0019-5154.117300.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Jan 2027
17 Jan 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free