Pyogenic granuloma
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 24 Jan 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: lobular capillary haemangioma
Continue reading below
What is pyogenic granuloma?1
Pyogenic granulomata are common rapidly growing, benign vascular lesions of the skin and mucosa. They are not infective, purulent or granulomatous (as the name might suggest) - rather, a reactive inflammatory mass of blood vessels and a few fibroblasts within the dermis of the skin.
What causes pyogenic granuloma? (Aetiology)2
Back to contentsThis is not fully understood: rapid growth occurs in response to an unknown stimulus that triggers endothelial proliferation and angiogenesis.
Trauma and burns can provoke the sequence but frequently there is no identifiable cause.
Bacterial infection may be involved. Staphylococcus aureus is often isolated from the lesion.
Other suggested causes include viral oncogenes, hormonal influences (pregnancy, oral contraceptive pill) and cytogenetic abnormalities.
They have also been associated with certain medications:
Continue reading below
How common is pyogenic granuloma? (Epidemiology)
Back to contentsMean age for presentation is 6-7 years. Thereafter, there is a decrease in incidence with age.8 They represent 0.5% of skin nodules in children.9
They are more common in women, due to frequent formation on the gingiva during pregnancy (pregnancy tumour, or epulis gravidarum) - occurring in up to 5% of pregnancies.10
What does pyogenic granuloma look like?2
Back to contentsSolitary red, purple or yellow papule or nodule arising from normal skin.11
Size varies from a few millimetres in diameter to several centimetres.
Polypoid appearance - they often develop a stalk or 'collarette' of scale at the base.
Friable lesion - they are often seen to be bleeding, crusted or ulcerated.
Pyogenic granuloma on the elbow
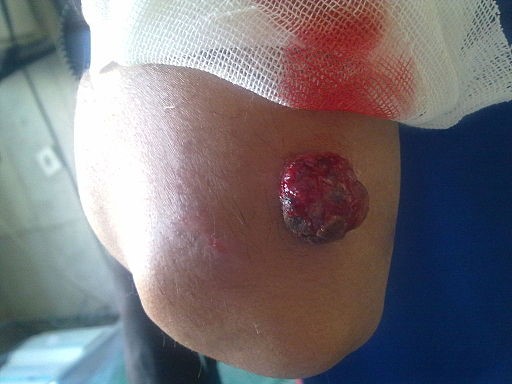
© Alborz Fallah, CC BY-SA 3.0, via Wikimedia Commons
By Alborz Fallah, CC BY-SA 3.0, via Wikimedia Commons
Continue reading below
Pyogenic granuloma symptoms2
Back to contentsRapid eruption and growth over a few weeks.
Most commonly, they occur on the head, neck and extremities (particularly the fingers).
They occasionally occur on the external genitalia.12
In pregnancy, they are most likely to occur on the maxillary intraoral mucosal surface during the second and third trimesters.
They have also been reported on the labial mucosa in men.13
Rarely, multiple satellite lesions may develop - especially in adolescents and young adults after prior attempts to remove the original lesion.
Differential diagnosis1 2 11
Back to contentsAlthough the diagnosis is often straightforward, the most important differential diagnosis is hypomelanotic melanoma, which tend to bleed less than pyogenic granuloma. Other features that may increase the level of suspicion of a hypomelanotic melanoma include:
No clear history of trauma.
Atypical site or age group.
Therefore lesions with any degree of uncertain diagnosis are best removed surgically (deep curettage and cautery, or excision) and sent for urgent histology. If this cannot be done in Primary Care within 4 weeks of presentation, or if there is a concern about the possible diagnosis of hypomelanotic melanoma, then refer urgently to secondary care (2-week wait for suspected cancer if any concern about melanoma).14
The differential diagnoses include:
Glomus tumour.
Congenital haemangioma.
Metastatic carcinoma of the skin.
Spitz naevus.
Investigation1
Back to contentsSome advocate sending all lesions for histological confirmation. This is because the vascular nature of the lesion makes dermoscopy unreliable.15 However, there may be occasions on which dermoscopy may be considered sufficient (eg, typical appearance in a very young child).16
Primary care management1
Back to contentsMost patients seek help because of the bleeding associated with the lesion.
Treatment options include imiquimod cream 5%, timolol gel 0.5% and other topical (or oral) beta-blockers, intralesional steroid injection, curettage and cautery, shave excision, excision with primary closure and laser therapy.
Cryotherapy may work but does not provide a histological specimen for diagnosis.
One study reported the use of sclerotherapy employing sodium tetradecyl sulfate as the sclerosant. As with cryotherapy, this technique does not provide a histological specimen.17 Moreover, sodium tetradecyl sulfate is only licensed for the treatment of varicose veins in the UK, so the usual considerations concerning the use of unlicensed medicines apply.
When to refer1
Back to contentsFor assistance with diagnosis and removal.
Following a recurrence.
Where a melanoma is suspected (see Differential diagnosis section above).
Persistently discharging umbilical granulomas in neonates may signify deeper involvement.
Complications
Back to contentsPain and bleeding are the most usual problems associated with this lesion.
Prognosis2
Back to contentsPyogenic granulomata are benign lesions.
Untreated lesions will atrophy eventually but only a minority will spontaneously involute within six months.
Recurrence rates following treatment can be common regardless of treatment modality.
Pregnancy tumours tend to regress spontaneously following childbirth so treatment should be postponed accordingly.
Further reading and references
- Kumar P, Das A, Mondal A, et al; Pyogenic granuloma-like basal cell carcinoma on the abdomen: A deceptive presentation. Indian Dermatol Online J. 2016 Sep-Oct;7(5):446-448.
- Sarwal P, Lapumnuaypol K; Pyogenic Granuloma. StatPearls, Jan 2022.
- Pyogenic granuloma; Primary Care Dermatology Society (PCDS)
- Pyogenic Granuloma; DermNet NZ
- Badri T, Hawilo AM, Benmously R, et al; Acitretin-induced pyogenic granuloma. Acta Dermatovenerol Alp Panonica Adriat. 2011;20(4):217-8.
- Tinoco MP, Tamler C, Maciel G, et al; Pyoderma gangrenosum following isotretinoin therapy for acne nodulocystic. Int J Dermatol. 2008 Sep;47(9):953-6. doi: 10.1111/j.1365-4632.2008.03662.x.
- Wollina U; Multiple eruptive periungual pyogenic granulomas during anti-CD20 monoclonal antibody therapy for rheumatoid arthritis. J Dermatol Case Rep. 2010 Dec 19;4(3):44-6. doi: 10.3315/jdcr.2010.1050.
- Curr N, Saunders H, Murugasu A, et al; Multiple periungual pyogenic granulomas following systemic 5-fluorouracil. Australas J Dermatol. 2006 May;47(2):130-3.
- Paul LJ, Cohen PR; Paclitaxel-associated subungual pyogenic granuloma: report in a patient with breast cancer receiving paclitaxel and review of drug-induced pyogenic granulomas adjacent to and beneath the nail. J Drugs Dermatol. 2012 Feb;11(2):262-8.
- Durgun M, Selcuk CT, Ozalp B, et al; Multiple disseminated pyogenic granuloma after second degree scald burn: a rare two case. Int J Burns Trauma. 2013 Apr 18;3(2):125-9. Print 2013.
- Kamal R, Dahiya P, Puri A; Oral pyogenic granuloma: Various concepts of etiopathogenesis. J Oral Maxillofac Pathol. 2012 Jan;16(1):79-82. doi: 10.4103/0973-029X.92978.
- Jafarzadeh H, Sanatkhani M, Mohtasham N; Oral pyogenic granuloma: a review. J Oral Sci. 2006 Dec;48(4):167-75.
- Marghoob A et al; An Atlas of Dermoscopy, Second Edition, 2012
- Arikan DC, Kiran G, Sayar H, et al; Vulvar pyogenic granuloma in a postmenopausal woman: case report and review of the literature. Case Rep Med. 2011;2011:201901. doi: 10.1155/2011/201901. Epub 2011 Sep 8.
- Ravi V, Jacob M, Sivakumar A, et al; Pyogenic granuloma of labial mucosa: A misnomer in an anomolous site. J Pharm Bioallied Sci. 2012 Aug;4(Suppl 2):S194-6. doi: 10.4103/0975-7406.100269.
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated January 2026)
- Zaballos P, Carulla M, Ozdemir F, et al; Dermoscopy of pyogenic granuloma: a morphological study. Br J Dermatol. 2010 Dec;163(6):1229-37. doi: 10.1111/j.1365-2133.2010.10040.x.
- Lacarrubba F, Caltabiano R, Micali G; Dermoscopic and histological correlation of an atypical case of pyogenic granuloma. Pediatr Dermatol. 2013 Jul;30(4):499-501. doi: 10.1111/pde.12123. Epub 2013 Mar 14.
- Sacchidanand S, Purohit V; Sclerotherapy for the treatment of pyogenic granuloma. Indian J Dermatol. 2013 Jan;58(1):77-8. doi: 10.4103/0019-5154.105317.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 23 Jan 2028
24 Jan 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free