Raynaud's disease
Peer reviewed by Dr Laurence KnottLast updated by Dr Colin Tidy, MRCGPLast updated 18 Feb 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Raynaud's phenomenon article more useful, or one of our other health articles.
In this article:
Synonyms: Raynaud's phenomenon
Continue reading below
Pathogenesis
Raynaud's disease was discovered by Maurice Raynaud (a Parisian physician) in the latter half of the nineteenth century. Raynaud's disease is characterised by a paroxysmal vasospastic and subsequent vasodilatory chain of events affecting peripheral arterioles, usually in the hands and feet. It commonly occurs as a response to cold exposure but may also be precipitated by emotional turmoil. The process may occur as a primary entity or secondary to other disease processes.
The pathogenesis of Raynaud's disease is complex but abnormalities of the blood vessel wall, of neural control mechanisms and of intravascular circulating factors are known to interact and contribute1 .
Raynaud also has a type of gangrene (symmetrical gangrene of the extremities) and a sign (symmetrical, mottled cyanosis of extremities with patches of erythema and excessive sweating) named after him2 .
Epidemiology3 4 5
Back to contentsThe most common trigger of Raynaud's disease is thought to be exposure to cold. Attacks may even occur after minor changes in temperature, such as moving into an air-conditioned building from a hot summer day. Other reported triggers include emotional stress, medications such as beta-blockers, injury due to vibrations or forcible trauma, extended use of digits, smoking and the presence of other arterial diseases, such as vasculitis.
Raynaud's phenomenon is common, occurring less frequently in warmer climates). Most cases (80-90%) of Raynaud's phenomenon are primary.
Primary Raynaud's is more common in women and typically develops at a younger age (second or third decade) than secondary Raynaud's.
A systematic review reported a pooled prevalence of primary Raynaud's phenomenon of 4.85% and a pooled annual incidence of 0.25%.
The main risk factors identified for primary Raynaud's phenomenon were female gender, positive family history, smoking and migraine. Smoking and hand-arm vibration syndrome are more commonly implicated in men.
Secondary Raynaud's is much less common (10-20% of cases) and is the initial manifestation of an associated underlying connective tissue disease, such as scleroderma, dermatomyositis, systemic lupus erythematosus, mixed connective tissue disease, Sjögren's syndrome or rheumatoid arthritis. Over 90% of people with systemic sclerosis have Raynaud's phenomenon.
One UK study among 720 schoolchildren found that 18% of girls and 12% of boys reported a change of colour in their fingers in cold climates at least once a month, or a 'numb or tingly' sensation in the fingers with cold exposure. The prevalence increased with age, especially among the girls6 .
Continue reading below
Presentation
Back to contentsRaynaud's disease symptoms
The patient may initially notice pallor of the distal portion of one or more digits. For reasons as yet unknown, the thumb is usually spared7 .
There is usually a clear demarcation line between affected and normal skin.
There then follows a feeling of numbness or pain in the digit(s) accompanied by cyanosis (blueing) of the digit.
Finally, there is a hyperaemic phase where the digit becomes red and feels warm.
Individual patients may show variation in the sequence of these three phases.
Hands in Raynaud's disease
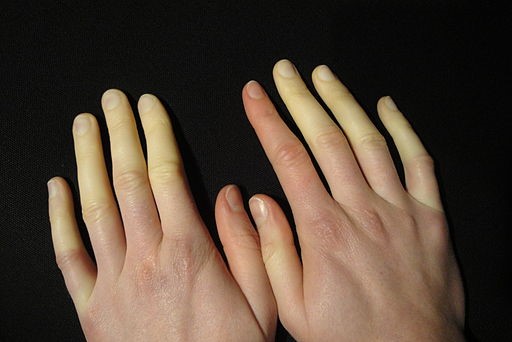
© Niklas D, CC BY-SA 3.0, via Wikimedia Commons
The patient's age and sex will influence the likelihood of this being primary or secondary Raynaud's disease. Enquire about any associated Raynaud's disease symptoms such as migrainous headache, recent joint or muscle pains, rashes, symptoms of infection, weight loss, etc, to detect possible underlying causes.
It is important to take an occupational history and specifically ask about the use of vibrating tools at work or at home. Take a medication history, including over-the-counter/complementary preparations, and ask if anyone in the family has the same problem. Ask if the patient has ever had frostbite, which is thought to increase the risk of subsequent vasomotor hyperactivity.
Signs
In primary Raynaud's disease there will usually be nothing to find, as patients rarely present during the event.
To detect evidence of an alternative cause for the symptoms, or an underlying disease associated with secondary Raynaud's disease, look for any abnormality in pulses of the affected hand/foot:
Note whether there is atrial fibrillation/other cardiac dysrhythmia or murmur, or any other evidence of a cause for embolic disease.
Look at the skin of the face for malar rash indicating systemic lupus erythematosus. Look for sclerodactyly, calcinosis or ulcer formation, and carefully seek evidence of vasculitic changes in the nail beds (magnification will help with this), suggesting progressive systemic sclerosis.
Examine any joints that are sore, palpate the abdomen to exclude hepato/splenomegaly and check the lymph fields to detect any evidence of malignancy. Examine any other relevant systems if other underlying causes are possible - eg, chest examination if pulmonary malignancy is suspected.
Differential diagnosis8
Back to contentsAssociated diseases causing secondary Raynaud's phenomenon
Dermatomyositis or polymyositis |
Arteriosclerosis |
Carcinoid syndrome |
Tobacco smoking Trauma Vibration (hand-arm vibration syndrome) Pressure from use of crutches Exposure to lead, arsenic, vinyl chloride |
Other neoplasms/paraneoplastic syndromes |
Mycoplasma pneumoniae |
Lymphoma Cryoglobulins Cryofibrinogenaemia |
Beta-blockers Ergot derivatives Combined oral contraceptive pill Cytotoxics: bleomycin, vinblastine, cisplatin Interferon (alfa and beta) Methysergide |
Many conditions may co-exist as above. The symptom complex is usually fairly distinctive, but other causes of vascular compromise may cause similar symptoms. If in doubt, consider vascular flow imaging/vascular surgical advice. Possible diagnoses that are not classically associated as causative diseases but which may cause symptoms that resemble Raynaud's phenomenon are:
Arterial thromboembolism.
Reflex sympathetic dystrophy (algodystrophy).
Continue reading below
Investigations
Back to contentsIn classically presenting primary Raynaud's disease, in a young woman who is well and has no evidence of other causes on examination, you are unlikely to detect anything on investigation:
It is probably worth checking FBC, antinuclear antibodies and CRP/ESR/plasma viscosity in this situation as basic screening for unrecognised associated disease.
If there is reason to suspect an underlying cause then investigations should be directed to confirming or refuting the association as below:
Consider U&E/liver function/thyroid function testing as the basic screening tests in appropriate patients. The presence of specific autoantibodies - eg, antinuclear antibodies - may suggest underlying inflammatory disease. Check plasma glucose for possible diabetes. Urine/serum protein electrophoresis, cold agglutinins and fibrinogen levels may identify hyperviscosity states. CXR (thoracic outlet views) may show a cervical rib.
Refer patients with suspected secondary Raynaud's disease for capillaroscopy if available. Other investigations performed in secondary care include infrared thermography, laser Doppler flowmetry, portable radiometry, and digital plethysmography10 .
Distinguishing between primary and secondary Raynaud's disease10
Back to contentsPrimary
Younger age (<30, but can be any age); female; genetic component (30% have an affected first-degree relative).
No symptoms/signs of underlying disease; no tissue necrosis or gangrene; normal nail fold capillaries.
Normal ESR; negative antineutrophil antibodies.
Secondary
Older age (>30, but can be any age); less common (10-20%).
Symptoms and signs of underlying disease; tightness of finger skin; more severe pain; digital ischaemia (digital pitting scars, ulceration, or gangrene); abnormal nail fold capillaries.
Raised ESR; positive antineutrophil antibodies or anti-extractable nuclear antigen antibodies.
Management of primary Raynaud's disease11
Back to contentsGeneral/preventative
Self-help measures
Smoking cessation - this is the most important self-help measure.
Avoid exposure to cold and take precautionary measures before exposure to cold; use gloves or electrically heated mittens in the winter (available from patient support groups via specialist outfitters - see 'Further reading & references' section, below).
Change occupation/DIY habits if vibration is a likely underlying cause.
Topical agents
Evidence on topical nitrates is limited but studies have shown that10 :
Topical glyceryl trinitrate applied to the dorsum of the finger results in digital vasodilatation with fewer systemic side-effects than with oral nitrates.
Nitroglycerin applied to the affected finger reduces the severity of Raynaud's phenomenon but not the duration or frequency of attacks.
Systemic agents
Calcium-channel blockers: these are most widely used in the treatment of Raynaud's phenomenon. Nifedipine promotes relaxation of vascular smooth muscle cells and leads to vasodilatation10 .
A Cochrane review found low to moderate quality evidence that calcium-channel blockers (especially the dihydropyridine class) may be useful in reducing the frequency, duration, and severity of attacks, and also pain and disability associated with primary and secondary Raynaud's phenomenon12 .
Apart from calcium-channel blockers, which are considered to be the drugs of choice, evidence of the effects of alternative pharmacological treatments is limited. A Cochrane review found that evidence is insufficient to support the use of vasodilators and suggests that vasodilator use may even worsen disease13 .
Intravenous prostaglandins: intravenous iloprost has been shown to reduce the frequency and severity of attacks10 .
Surgery10
Surgical intervention may be considered for severe and disabling symptoms.
Surgical interventions include arterial reconstruction, peripheral sympathectomy, embolectomy and ulcer debridement, or a combination of techniques.
Cervical sympathectomy is no longer recommended..
Management of secondary Raynaud's disease
Back to contentsOptimal management of the underlying cause can alleviate the symptoms but, unfortunately, many cases do not seem to respond well and persist despite best treatment of the precipitating illness. General/preventative measures are the same as for primary Raynaud's disease as above. Those cases associated with progressive systemic sclerosis are often most troublesome and may lead to severe digital ischaemia and gangrene. See also the separate Systemic Sclerosis (Scleroderma) article.
When to refer
Back to contentsMost patients can be managed in primary care14 . However, referral should be considered in the following circumstances3 :
Admit immediately if the person has severe ischaemia of one or more digits.
Refer:
Suspected secondary Raynaud's phenomenon.
Children aged 12 years or younger with Raynaud's phenomenon.
Symptoms worsening, severe or unresponsive to standard treatment.
Most causes will be due to connective tissue disorders and referral to a rheumatologist would be appropriate. If an occupational cause is suspected, refer to an occupational medicine specialist or vascular clinician with expertise in this area (depending on local protocol)..
Prognosis3
Back to contentsPrimary Raynaud's is typically benign and does not progress or lead to tissue damage. Studies have found rates of remission (no attacks for two cold seasons, or 12 months without symptoms) between 3% and 33% after 7-14 years. The frequency and severity of symptoms fluctuate with changes in daily temperature and may lessen with increasing age.
An underlying disorder develops in 13% of cases of the primary form. Primary Raynaud's disease may go into remission. Most patients have a stable course and over half improve over time15 . Secondary cases are more prone to be problematic - ulceration, scarring, or gangrene occur in 17% of people with Raynaud's disease secondary to systemic sclerosis16 .
Complications
Back to contentsSevere cases may lead to digital infarction and gangrene with loss of the tissue of the finger pulp or distal phalanx. The skin may become chronically ischaemic and ulcerate. The digit(s) may lose viability and require amputation in the very worst cases.
Prevention of attacks
Back to contentsAvoid smoking14 .
Avoid beta-blocker treatment.
Wear gloves or have them to hand at all times.
Use specialist heated gloves if necessary.
Anticipate exposure to cold and take appropriate ameliorative steps.
Advise considering moving to warmer climes (particularly during the coldest months) if the condition is troublesome enough and the patient has the resources to do so.
Avoid use of vibrating hand tools.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Herrick AL; The pathogenesis, diagnosis and treatment of Raynaud phenomenon. Nat Rev Rheumatol. 2012 Aug;8(8):469-79. doi: 10.1038/nrrheum.2012.96. Epub 2012 Jul 10.
- A. G. Maurice Raynaud; Whonamedit.com
- Raynaud's phenomenon; NICE CKS, February 2020 (UK access only)
- Garner R, Kumari R, Lanyon P, et al; Prevalence, risk factors and associations of primary Raynaud's phenomenon: systematic review and meta-analysis of observational studies. BMJ Open. 2015 Mar 16;5(3):e006389. doi: 10.1136/bmjopen-2014-006389.
- Maverakis E, Patel F, Kronenberg DG, et al; International consensus criteria for the diagnosis of Raynaud's phenomenon. J Autoimmun. 2014 Feb-Mar;48-49:60-5. doi: 10.1016/j.jaut.2014.01.020. Epub 2014 Feb 1.
- Goldman RD; Raynaud phenomenon in children. Can Fam Physician. 2019 Apr;65(4):264-265.
- Chikura B, Moore TL, Manning JB, et al; Sparing of the thumb in Raynaud's phenomenon. Rheumatology (Oxford). 2008 Feb;47(2):219-21.
- Herrick AL; Evidence-based management of Raynaud's phenomenon. Ther Adv Musculoskelet Dis. 2017 Dec;9(12):317-329. doi: 10.1177/1759720X17740074. Epub 2017 Nov 20.
- Khouri C, Blaise S, Carpentier P, et al; Drug-induced Raynaud's phenomenon: beyond beta-blockers. Br J Clin Pharmacol. 2016 Mar 7. doi: 10.1111/bcp.12912.
- Goundry B, Bell L, Langtree M, et al; Diagnosis and management of Raynaud's phenomenon. BMJ. 2012 Feb 7;344:e289. doi: 10.1136/bmj.e289.
- Landry GJ; Current medical and surgical management of Raynaud's syndrome. J Vasc Surg. 2013 Jun;57(6):1710-6. doi: 10.1016/j.jvs.2013.03.012. Epub 2013 Apr 23.
- Rirash F, Tingey PC, Harding SE, et al; Calcium channel blockers for primary and secondary Raynaud's phenomenon. Cochrane Database Syst Rev. 2017 Dec 13;12:CD000467. doi: 10.1002/14651858.CD000467.pub2.
- Su KY, Sharma M, Kim HJ, et al; Vasodilators for primary Raynaud's phenomenon. Cochrane Database Syst Rev. 2021 May 17;5:CD006687. doi: 10.1002/14651858.CD006687.pub4.
- Smith J; Focused assessment with sonography in trauma (FAST): should its role be reconsidered? Postgrad Med J. 2010 May;86(1015):285-91. doi: 10.1136/pgmj.2008.076711. Epub 2010 Apr 3.
- Jackson CM; The patient with cold hands: understanding Raynaud's disease. JAAPA. 2006 Nov;19(11):34-8.
- Herrick A; Raynaud's Phenomenon. Curr Treat Options Cardiovasc Med. 2008 Apr;10(2):146-55.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Laurence Knott
General Practitioner, Medical Author
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Feb 2027
18 Feb 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free