Seborrhoeic wart
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 17 Feb 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Seborrhoeic warts article more useful, or one of our other health articles.
In this article:
Synonyms: seborrhoeic keratosis, basal cell papilloma
Continue reading below
What are seborrhoeic warts?
Seborrhoeic warts (also known as seborrhoeic keratoses) are common benign, hyperkeratotic skin lesions associated with ageing.
Causes of seborrhoeic warts (aetiology)1
Back to contentsThe cause is not fully understood. Ageing is closely linked to the development of seborrhoeic keratoses. Sunlight and UV light exposure appears to play a role in causation, given the typical distribution of seborrhoeic warts. They have been known to follow sunburn.
An infectious aetiology has been proposed, with human papillomavirus and Merkel cell polyomavirus detected in seborrhoeic warts in some studies. However, these were felt to either be surface contamination or non-causal co-infection.1
Some cases of multiple seborrhoeic warts are inherited in an autosomal dominant pattern.2 Oncogenic mutations are involved in pathogenesis and a broad spectrum of somatic mutations in the FGFR3, PIK3CA, RAS, AKT1 and EGFR genes has been noted.3
Continue reading below
How common are seborrhoeic warts? (Epidemiology)45
Back to contentsPresence and frequency increases with age: almost all elderly patients have some. It has been estimated that over 90% of adults aged 60 or more have at least one seborrhoeic wart.
They usually present from the fourth decade onwards.
No sex difference exists.
Seborrhoeic warts are less common in people with darker skin tones, but can occur in anyone.
The trunk and face are the sites most commonly affected.
It is common to have more than one lesion and there may be many lesions.
Symptoms of seborrhoeic warts (presentation)
Back to contentsTypical clinical appearance
Flat-topped or warty-looking lesions that appear to be 'stuck on' to the skin.
Usually pigmented, sometimes deeply and may even be black. Others can be paler in colour.
There is usually a well-circumscribed border.
Size ranges from 1 mm to several cm.
The surface is usually pitted and irregular with visible keratin dots giving a granular and rough appearance.
Initially, lesions are velvety and soft in texture, before developing a warty surface and becoming uneven, with multiple plugged follicles.
The surface may become covered by adherent greasy scale.
Multiple lesions may align along skin folds.
They are usually asymptomatic but may become irritated, itchy or inflamed spontaneously or after minor trauma.
Black pigmented verrucous lesion
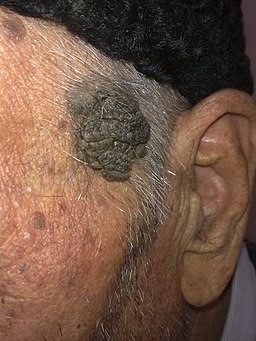
© Alborz Fallah, CC BY-SA 3.0, via Wikimedia Commons
Seborrhoeic keratosis
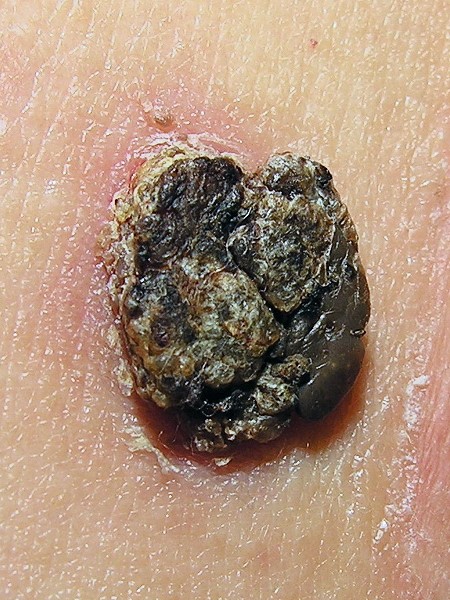
© Lmbuga, Public domain, via Wikimedia Commons
Dermoscopic features56
Thickened epidermis with multiple milia-like cysts and comedo-like openings.
Gyri and sulci (looking like the surface of the brain).
Fingerprint-like structures.
Bloods vessels are fine, regular and hairpin in shape and surrounded by a milky halo.
'Moth-eaten' borders in the thinner lesions.
Variants
Less common variants of seborrhoeic warts include:
Stucco keratoses - multiple skin-coloured or white, dry, scaly lesions often seen on the extremities (dorsa of hands, forearms, ankles and feet).7
Dermatosis papulosa nigra - multiple small, brown or black pedunculated lesions seen on the face of dark-skinned individuals. Often have an earlier onset than typical seborrhoeic warts.8
Solar lentigo - well-circumscribed, flat pigmented patches which occur in sun-exposed areas.9
Melanoacanthoma - very deeply pigmented seborrhoeic warts.10
Continue reading below
Differential diagnosis11
Back to contentsVerruca vulgaris.
Condyloma acuminatum.
Fibroepithelial polyp.
Melanocytic naevus.
Pigmented basal cell carcinoma.
Associated diseases
Back to contentsAlthough skin malignancy is thought to occur by chance in patients with seborrhoeic warts, studies report the occasional association with Bowen's disease and squamous epithelial dysplasia.12 This occurs more frequently in regions with high solar ultraviolet levels.13
Rarely, a sudden onset or increase in the number of seborrhoeic warts can herald an underlying malignancy (usually adenocarcinoma of the stomach but also colon, breast and lung).14 It can be associated with acanthosis nigricans. This sudden increase is known as the Leser-Trélat sign.5 The same phenomenon without internal malignancy is known as a pseudo-Leser-Trélat sign.15
Management of seborrhoeic warts5
Back to contentsReassurance: most often, no treatment is required.
Remove where there is cosmetic dislike, repeated irritation or chafing from clothes, or diagnostic uncertainty.
Removal by cryotherapy (this may require repeat treatments), curettage and cautery or shave excision are effective and produce a better result than excision and suture, although a pale white scar can be left.
Dermoscopy may be used by appropriately trained GPs to assist in diagnosis.16
When to refer
Usually, they can be managed in primary care. However, patients with lesions requiring removal from difficult areas should be referred. Lesions that are suspicious of melanoma (either with the naked eye or by dermoscopy) should be sent as a cancer network two-week referral to a dermatologist.16
Complications of seborrhoeic warts
Back to contentsRepeated irritation and inflammation where lesions catch on clothing.
Aesthetic dislike.
Concerns regarding malignancy:
It is harder to notice a malignant melanoma arise amongst multiple seborrhoeic warts.
Rarely, melanoma in situ can arise within a seborrhoeic wart, although this is rare.17
Prognosis
Back to contentsAlthough seborrhoeic warts are benign, they do not spontaneously resolve and they become larger and thicker with time.
Further reading and references
- Noiles K, Vender R; Are all seborrheic keratoses benign? Review of the typical lesion and its variants. J Cutan Med Surg. 2008 Sep-Oct;12(5):203-10.
- Gorai S, Ahmad S, Raza SSM, et al; Update of pathophysiology and treatment options of seborrheic keratosis. Dermatol Ther. 2022 Dec;35(12):e15934. doi: 10.1111/dth.15934. Epub 2022 Nov 1.
- Seborrheic Keratosis; Online Mendelian Inheritance in Man (OMIM)
- Hafner C, Hafner H, Groesser L; Genetic basis of seborrheic keratosis and epidermal nevi. Pathologe. 2014 Sep;35(5):413-23. doi: 10.1007/s00292-014-1928-9.
- Seborrhoeic Keratoses; DermNet NZ
- Seborrhoeic keratosis; Primary Care Dermatology Society
- Marghoob AA, Usatine RP, Jaimes N; Dermoscopy for the family physician. Am Fam Physician. 2013 Oct 1;88(7):441-50.
- Stucco keratosis. Primary Care Dermatology Society. Accessed 4th Jan 2025.
- Dermatosis Papulosa Nigra. StatPearls.
- Solar lentigo; DermNet NZ
- Vasani RJ, Khatu SS; Melanoacanthoma: Uncommon presentation of an uncommon condition. Indian Dermatol Online J. 2013 Apr;4(2):119-21. doi: 10.4103/2229-5178.110638.
- Seborrheic Keratosis; DermIS (Dermatology Information System)
- Rajabi P, Adibi N, Nematollahi P, et al; Bowenoid transformation in seborrheic keratosis: A retrospective analysis of 429 patients. J Res Med Sci. 2012 Mar;17(3):217-21.
- Gaffney DC, Muir JB, De'ambrosis B; Malignant change in seborrhoeic keratoses in a region with high solar ultraviolet levels. Australas J Dermatol. 2013 Apr 10. doi: 10.1111/ajd.12035.
- Ponti G, Luppi G, Losi L, et al; Leser-Trelat syndrome in patients affected by six multiple metachronous primitive cancers. J Hematol Oncol. 2010 Jan 11;3:2.
- Husain Z, Ho JK, Hantash BM; Sign and pseudo-sign of Leser-Trelat: case reports and a review of the literature. J Drugs Dermatol. 2013 May;12(5):e79-87.
- Dermoscopy - an overview; Primary Care Dermatology Society, 2013
- Repertinger S, Wang J, Adickes E, et al; Melanoma in-situ arising in seborrheic keratosis: a case report. Cases J. 2008 Oct 23;1(1):263.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Feb 2028
17 Feb 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free