Venous leg ulcers
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 17 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Venous leg ulcers article more useful, or one of our other health articles.
In this article:
Continue reading below
Appearance of venous leg ulcers
Venous ulcers are usually large, shallow, painless and situated around the medial or lateral malleoli. They are associated with other signs of venous hypertension such as varicose veins, varicose eczema, haemosiderin pigmentation, atrophie blanche and venous flare. Oedema of the lower leg may be present and chronic venous stasis can lead to warty hyperplasia of the skin or thickening of the subcutaneous tissues.
Venous ulcers are caused by incompetent valves in the veins of the lower leg, especially in the perforators. These incompetent valves cause blood to be squeezed out into the superficial veins, when the calf muscles are contracted, instead of upwards towards the heart.
Dilation of superficial veins occurs (varicosities) and the subsequent raised venous pressure results in oedema, venous eczema and ulceration. Valves may also become damaged following the venous hypertension that occurs in pregnant women and there may be congenital absence of valves.
Pre-surgery venous leg ulcer
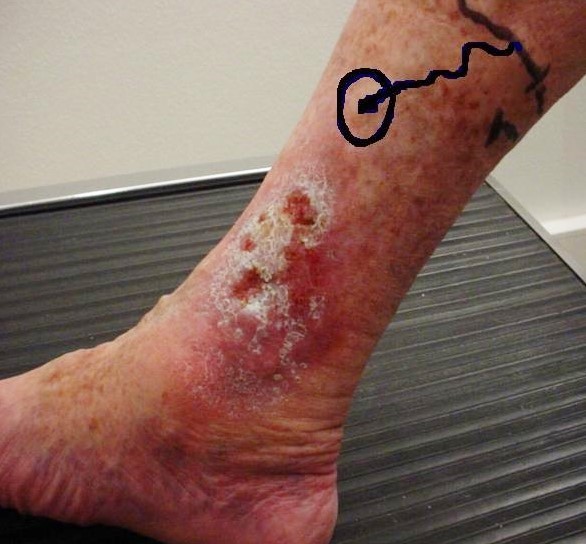
© Nini00, CC BY-SA 3.0, via Wikimedia Commons
How common are venous leg ulcers? (Epidemiology)
Back to contentsThe point prevalence of open venous leg ulcers in the UK is about 3 cases per 1,000 people, and many people experience recurrent episodes of prolonged ulceration.1
The prevalence increases with age and reaches 20 per 1,000 in the 80-plus age group. There is no socio-economic predilection but ulcers take longer to heal in lower socio-economic groups.2
This may be due to difficulties in accessing evidence-based management, such as Doppler assessment and compression therapy.3
Continue reading below
Diagnosis2 4
Back to contentsThe diagnosis is usually made clinically. A leg ulcer is defined as the loss of skin below the knee on the leg or foot, which takes more than two weeks to heal.
History
The following history may suggest venous ulceration:
Pre-existing varicose veins.
Deep vein thrombosis.
Phlebitis.
Previous fracture, trauma or surgery.
Family history of venous disease.
Symptoms of venous insufficiency - for example, pains or heaviness in the legs, aching, itching, swelling, breakdown of the skin surface, pigmentation, eczema.
Features in the history which suggest a non-venous cause include:
Family history of non-venous ulcers.
History of: heart disease, stroke, transient ischaemic attack.
Diabetes mellitus.
Peripheral arterial disease or intermittent claudication.
Cigarette smoking.
Rheumatoid arthritis.
Examination
80% of all leg ulcers are venous ulcers and a large shallow relatively painless ulcer with an irregular granulating base in the 'gaiter' region of the leg (between the knee and ankle) is likely to be venous in origin.5 There may be surrounding stasis dermatitis.
Examination can help to rule out a number of differential diagnoses, as follows:
Arterial ulcer - look for reduced pulses in the foot and ankle and possibly the femoral artery. These ulcers occur most commonly in areas of poor blood supply (eg, the tip of the toes or over the tibia) and are typically painful and deep. Other evidence of poor blood supply may include peripheral cyanosis and claudication.
Neuropathic ulcer - this is painless and deep, often with overlying hyperkeratosis. It occurs at sites of loss of nerve supply and recurrent trauma, ie the heel and the metatarsal heads.
Malignancy - malignant ulcers in this area are rare but the possibility should not be overlooked. Watch out for an ulcer with a rolled everted edge. If ulceration occurs in the area of scar tissue, Marjolin's ulcer should be considered.6 Chronic venous ulcers can develop into malignant ones, so any non-healing ulcer should be referred for biopsy.
Rheumatoid ulcer - these look a bit like arterial ulcers and are sharp, deep, well-demarcated ulcers with a punched-out appearance. They occur typically on the dorsum of the foot and calf and may be slow to heal. Venous ulcers also occur in rheumatoid patients, so the differentiation may be difficult. It is, however, worthwhile referring suspected rheumatoid ulcers to a rheumatologist, as such ulcers often respond well to a disease-modifying antirheumatic drug (DMARD).
Investigations2 4
Back to contentsBy the very nature of epidemiology, the patient may be elderly, frail and with reduced mobility, so that investigations in these circumstances may be limited. Primary care clinicians are advised to liaise with local community services to see what is available. Skilled nurses may well be able to carry out at least some of these investigations in the community.
Measurement of ankle brachial pressure index (ABPI) using Doppler - this is to exclude an arterial ulcer.7 A blood pressure cuff is applied to the lower calf muscle just above the ankle. A Doppler ultrasound probe is placed over the dorsalis pedis artery. The maximum cuff pressure at which a pulse can be heard is then recorded. The figure is then expressed as a ratio of the systolic pulse measured at the brachial artery. An index of 0.80 or less suggests significant peripheral arterial disease. In these cases, the Scottish Intercollegiate Guidelines Network (SIGN) recommends referral to a vascular specialist.
Measurement of the surface area - this gives an indication of rate of healing or failure to progress.
Swabs for microbiology - this is only necessary if there are clinical signs of infection such as cellulitis.
Patch testing - if there is associated dermatitis, chronic ulcer patients should be referred for patch testing using what is known as the 'leg ulcer series'. This is a group containing the kind of allergens to which a leg ulcer patient would be exposed - eg, chemicals contained in leg ulcer dressings.
Biopsy - if the ulcer has an atypical appearance or fails to heal after twelve weeks of active treatment.
Other tests - if an alternative or additional cause for the ulcer is suspected, consider other tests such as FBC, ESR, CRP, albumin, HbA1c, autoantibody screen and clotting and haemoglobinopathy screen.
Continue reading below
Venous leg ulcers primary care management2 4
Back to contentsFirst-line treatment for venous leg ulcers is compression therapy, but a wide range of dressings and topical treatments are also used.1
Graduated compression:
Before this treatment is tried, diabetes, neuropathy and peripheral arterial disease should be excluded and pre-existing swelling controlled by bed rest or elevation.
The treatment involves applying bandages to the leg, maximising the pressure at the ankle and gaiter area and reducing the pressure as one goes higher up the leg. This helps to control or reverse venous insufficiency.
There are many options available in terms of types of dressing, number of layers and whether to use elasticated or non-elasticated bandages. For uncomplicated venous ulcers, an elasticated multi-layer dressing (wool padding, dressing to keep padding in place, elasticated bandage and outer cover) can be used. This approach was confirmed by a Cochrane review. This review also found that four-layer dressing promoted faster healing than short stretch bandaging.8
A Cochrane review found evidence from one trial that compression hosiery reduces rates of reulceration of venous ulcers compared with no compression. Results from one trial suggested that recurrence is lower in high-compression hosiery than in medium-compression hosiery at three years whilst another trial found no difference at 5 years. Rates of patient intolerance of compression hosiery were high. There was insufficient evidence to aid selection of different types, brands, or lengths of compression hosiery.9
Debridement and cleaning - adherent slough should be debrided and any trapped pus released. A Cochrane review found only limited evidence to suggest that actively debriding a venous leg ulcer has a clinically significant impact on healing.10
Dressing - the treatment of choice for most vascular ulcers is an occlusive hydrocolloidal dressing which allows for epithelial cell migration and the influx of leukocytes and moisture. A Cochrane review found that alginate dressings were similarly effective.11 Topical growth factor has also been used to promote healing.
Antibiotics are not indicated for uninfected ulcers.12 For leg ulcer infection, NICE recommends (see guideline for further details):13
First choice oral antibiotic: flucloxacillin. Alternatives doxycycline, clarithromycin or erythromycin (in pregnancy).
Second choice (guided by microbiology when available) co-amoxiclav or co-trimoxazole.
If severely unwell, IV antibiotics in hospital.
Pentoxifylline - this is recommended at a dose of 400 mg tds for the treatment of chronic venous ulcers. An ulcer is deemed chronic if it fails to respond to first-line treatment after four weeks. It should be given for six months. It is thought to improve the microvascular circulation.
Topical steroids - a moderately potent steroid (eg, clobetasone) may be helpful in treating surrounding venous (stasis) dermatitis. Persistent dermatitis which fails to respond to treatment suggests an iatrogenically-induced allergy and is an indication for patch testing.
Aspirin - a Cochrane review could not find sufficient evidence to come to a conclusion about the risks and benefits of aspirin as an adjunct to compression bandaging. Further research is required.14
Therapeutic ultrasound: it is uncertain whether therapeutic ultrasound (either high or low frequency) improves the healing of venous leg ulcers.15
When to refer2
Back to contentsReferral is indicated in the following situations:
After failure to respond to two weeks of primary care treatment.
Peripheral arterial disease (ABPI <0.8).
Rheumatoid ulcer.
Suspicion of malignancy.
Atypical distribution of ulcers.
Dermatitis resistant to topical steroids.
Patients who may benefit from venous surgery or skin grafting.
Failure to progress (especially in patients with significant comorbidity).16
Other treatments for venous leg ulcers
Back to contentsHyperbaric oxygen therapy
A systematic review found evidence suggesting that hyperbaric oxygen therapy does not significantly affect complete healing of venous leg ulcers. There was a statistically significant benefit in terms of reducing ulcer size, though in the absence of ulcer healing the clinical significance of this could not be established.17
Granulox®.18
RCT and observational study evidence has been presented to support the use of this spray, with further supporting evidence provided from case series data. Within both RCTs, the primary endpoint was met and no treatment related adverse events were reported. However, limitations surrounding the studies should be acknowledged, particularly potential methodological weaknesses in the observational studies. The economic evaluation presented provides evidence that Granulox® is likely to be effective and produce resource savings.
Venous surgery
This is indicated in the following situations:19
The patient is fit for surgery (local anaesthesia if necessary).
There is sufficient mobility to activate a calf muscle pump.
The patient is prepared to attend hospital for investigation and surgery.
Obesity is controlled (body mass index <30).
Superficial venous incompetence: no deep venous incompetence on duplex imaging, or predominantly superficial venous incompetence on ambulatory venous pressures with tourniquet occlusion of the superficial veins.
Skin grafting
Pinched skin grafting may be indicated in patients with extensive areas of ulceration. This has been done successfully by nurses in the community who have been trained in the technique.19 However, a Cochrane review has found that further evidence is required to support the use of skin grafting apart from bilayer artificial skin which was supported by evidence. Trials showed that bilayer skin grafts were effective when combined with compression bandaging.20
For complicated ulcers, artificial dermis combined with a thin skin graft has shown promising results.21
A minced skin graft has also been developed which is faster than the pinched skin method and may produce better cosmetic results.22
Prognosis2 23
Back to contentsThere is a wide variation in published healing and recurrence rates of venous leg ulcers:
Six-month healing rates have been reported as 45% for those treated in the community (about 80% of people with venous leg ulcers), and 70% for those treated in specialist clinics.
Twelve-month recurrence rates range between 26–69%.
In a retrospective cohort analysis of 505 people in a large UK primary care database of electronic medical records, 53% of all venous leg ulcers healed within 12 months, with an average healing time of 3 months.
Repeat cycles of ulceration, healing, and recurrence are common.
Poor prognostic factors include:
Wound duration of more than 1 year (recurrence rate in these ulcers is more than 70%).
Larger wounds.
History of surgical treatment of varicose veins.
Ankle brachial pressure index (ABPI) of less than 0.8.
Impaired calf muscle pump (reduces ulcer healing rates).
Fibrin in more than 50% of wound surface.
Lower socioeconomic group.
Poor compliance with treatment and lifestyle advice.
Prevention of venous leg ulcers2
Back to contentsPrimary prevention of venous insufficiency
Provide advice to:
Keep mobile with regular walking.
Elevate the legs when immobile.
Avoid trauma and wear appropriate (well-fitting) footwear.
Use an emollient frequently, and avoid products that may contain any identified sensitizing agents (such as lanolin and preservatives).
Adopt a healthy lifestyle, including losing weight if overweight or obese, eating a balanced diet (malnutrition impairs ulcer healing), drinking alcohol within recommended limits, and not smoking.
Use compression hosiery when there are early signs of venous insufficiency (eg, stasis dermatitis) to prevent the development of ulcers.
Secondary prevention of a recurrent ulcer
Correctly fitted compression hosiery should be worn for five years after an ulcer.
Underlying comorbidities - eg, diabetes, rheumatoid arthritis - should be managed appropriately.
Vascular surgery should be considered if the patient fits the criteria (see above).
Further reading and references
- Nelson EA, Adderley U; Venous leg ulcers. BMJ Clin Evid. 2016 Jan 15;2016:1902.
- Raffetto JD, Ligi D, Maniscalco R, et al; Why Venous Leg Ulcers Have Difficulty Healing: Overview on Pathophysiology, Clinical Consequences, and Treatment. J Clin Med. 2020 Dec 24;10(1):29. doi: 10.3390/jcm10010029.
- Norman G, Westby MJ, Rithalia AD, et al; Dressings and topical agents for treating venous leg ulcers. Cochrane Database Syst Rev. 2018 Jun 15;6(6):CD012583. doi: 10.1002/14651858.CD012583.pub2.
- Leg ulcer - venous; NICE CKS, August 2021 (UK access only)
- Petherick ES, Cullum NA, Pickett KE; Investigation of the effect of deprivation on the burden and management of venous leg ulcers: a cohort study using the THIN database. PLoS One. 2013;8(3):e58948. doi: 10.1371/journal.pone.0058948. Epub 2013 Mar 19.
- Bonkemeyer Millan S, Gan R, Townsend PE; Venous Ulcers: Diagnosis and Treatment. Am Fam Physician. 2019 Sep 1;100(5):298-305.
- Collins L, Seraj S; Diagnosis and treatment of venous ulcers. Am Fam Physician. 2010 Apr 15;81(8):989-96.
- Chong AJ, Klein MB; Images in clinical medicine. Marjolin's ulcer. N Engl J Med. 2005 Mar 10;352(10):e9.
- Sihlangu D, Bliss J; Resting Doppler ankle brachial pressure index measurement: a literature review. Br J Community Nurs. 2012 Jul;17(7):318-20, 322-4.
- O'Meara S, Cullum N, Nelson EA, et al; Compression for venous leg ulcers. Cochrane Database Syst Rev. 2012 Nov 14;11:CD000265. doi: 10.1002/14651858.CD000265.pub3.
- Nelson EA, Bell-Syer SE; Compression for preventing recurrence of venous ulcers. Cochrane Database Syst Rev. 2014 Sep 9;2014(9):CD002303. doi: 10.1002/14651858.CD002303.pub3.
- Gethin G, Cowman S, Kolbach DN; Debridement for venous leg ulcers. Cochrane Database Syst Rev. 2015 Sep 14;2015(9):CD008599. doi: 10.1002/14651858.CD008599.pub2.
- O'Meara S, Martyn-St James M; Alginate dressings for venous leg ulcers. Cochrane Database Syst Rev. 2013 Apr 30;4:CD010182. doi: 10.1002/14651858.CD010182.pub2.
- O'Meara S, Al-Kurdi D, Ologun Y, et al; Antibiotics and antiseptics for venous leg ulcers. Cochrane Database Syst Rev. 2014 Jan 10;(1):CD003557. doi: 10.1002/14651858.CD003557.pub5.
- Leg ulcer infection: antimicrobial prescribing; NICE Guidance (February 2020)
- de Oliveira Carvalho PE, Magolbo NG, De Aquino RF, et al; Oral aspirin for treating venous leg ulcers. Cochrane Database Syst Rev. 2016 Feb 18;2:CD009432. doi: 10.1002/14651858.CD009432.pub2.
- Cullum N, Liu Z; Therapeutic ultrasound for venous leg ulcers. Cochrane Database Syst Rev. 2017 May 15;5(5):CD001180. doi: 10.1002/14651858.CD001180.pub4.
- Anderson I; Mixed aetiology: complexity and comorbidity in leg ulceration. Br J Nurs. 2008 Aug 14-Sep 10;17(15):S17-8, S20-3.
- Keohane C, Westby D, Nolan FC, et al; Hyperbaric Oxygen as an Adjunct in the Treatment of Venous Ulcers: A Systematic Review. Vasc Endovascular Surg. 2023 Mar 8:15385744231162924. doi: 10.1177/15385744231162924.
- Granulox® haemoglobin spray - Innovative Medical Technology Overview: Number 006/2016; Healthcare Improvement Scotland
- Simon DA, Dix FP, McCollum CN; Management of venous leg ulcers. BMJ. 2004 Jun 5;328(7452):1358-62.
- Jones JE, Nelson EA, Al-Hity A; Skin grafting for venous leg ulcers. Cochrane Database Syst Rev. 2013 Jan 31;1:CD001737. doi: 10.1002/14651858.CD001737.pub4.
- Canonico S, Campitiello F, Della Corte A, et al; The use of a dermal substitute and thin skin grafts in the cure of "complex" leg ulcers. Dermatol Surg. 2009 Feb;35(2):195-200.
- Hamnerius N, Wallin E, Svensson A, et al; Fast and Standardized Skin Grafting of Leg Wounds With a New Technique: Report of 2 Cases and Review of Previous Methods. Eplasty. 2016 Mar 10;16:e14. eCollection 2016.
- Guest JF, Fuller GW, Vowden P; Venous leg ulcer management in clinical practice in the UK: costs and outcomes. Int Wound J. 2018 Feb;15(1):29-37. doi: 10.1111/iwj.12814. Epub 2017 Dec 15.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 10 May 2028
17 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free