Aortic stenosis
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 15 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Heart valve diseaseMitral stenosisMitral regurgitationAortic regurgitationInfective endocarditis
The aortic valve is a heart valve that lies between the left ventricle and the aorta. In aortic stenosis, when the aortic valve opens to let blood pump through, it does not open as widely as it would normally. The opening between the left ventricle and the aorta is therefore narrowed (stenosed).
The amount of blood that can pass from the left ventricle to the aorta is therefore reduced. The more narrowed the valve, the smaller the amount of blood that can get through, and the more significant the symptoms.
In some cases, aortic stenosis occurs at the same time as aortic regurgitation.
In this article:
Video picks for Heart disease
Continue reading below
What is aortic stenosis?
Aortic stenosis is a narrowing of the aortic valve which is the valve between the left ventricle and the aorta. The aortic valve controls the flow of blood between the left ventricle and the aorta. If it is narrowed, the flow of blood is reduced. This can cause various complications which are listed below.
Aortic stenosis symptoms
Back to contentsMild aortic stenos often does not cause any symptoms.
The symptoms associated with more severe aortic stenosis may include:
Chest pain (angina) or tightness with activity.
Shortness of breath, especially with activity.
Heart failure symptoms, such as shortness of breath or swelling of the legs.
Continue reading below
Causes of aortic stenosis
Back to contentsThe most common cause of aortic stenosis is "atherosclerosis". This is a condition where there is a build up of calcium, fats and other deposits on the walls of the arteries. This becomes much more common with age and is also associated with high cholesterol or diabetes.
Some types of congenital heart disease (abnormalities of the heart present at birth), such as a bicuspid aortic valve, can also cause aortic stenosis later in life.
Rheumatic fever used to be a common cause of aortic stenosis - this was caused by a bacteria called streptococcus and often arose from a streptococcal throat infection. This is now very rare in the developed world but is still the commonest cause in some developing countries.
How quickly does aortic stenosis progress?
Back to contentsAortic stenosis progression is very difficult to predict.
The majority of people with mild aortic stenosis will never progress to developing clinically significant aortic stenosis. However, they may be offered a scan every three to five years to assess their valve.
Moderate and severe aortic stenosis usually does progress and cause symptoms. Again it is difficult to predict how quickly this can happen and the National Institute for Health and Care Excellence (NICE) guidelines now advise referral for consideration of surgery for everyone with moderate or severe aortic stenosis.
Continue reading below
Diagnosing aortic stenosis
Back to contentsAortic stenosis is often diagnosed before people have any symptoms. This may be because they are having an echocardiogram (an ultrasound scan of the heart) for another reason. Sometimes a heart murmur is heard whilst examining the heart and an echocardiogram is organised to determine the diagnosis. Sometimes, the symptoms of aortic stenosis lead to an echocardiogram being organised to assess the severity of the condition.
NICE recommends that all patients with a heart murmur, where aortic stenosis is suspected, should be considered for an echocardiogram, particularly if they are over 75 years old, if there is a family history of aortic stenosis or if there are other medical conditions, such as atrial fibrillation. An echocardiogram should always be offered if there is shortness of breath associated with a heart murmur.
A cardiology referral should be offered to anyone found to have moderate or severe aortic stenosis or anyone found to have a bicuspid aortic valve (usually due to congenital heart disease).
Aortic stenosis treatment
Back to contentsIf the narrowing (stenosis) is mild then usually no treatment is needed. There are no medications which slow down the progression of aortic stenosis or treat the aortic stenosis itself.
Surgery is usually advised when symptoms develop. Studies have shown that, once symptoms develop, the average survival is two to three years without surgical intervention. With surgery, the outlook is very good.
Medication
Medication may be used to help ease the symptoms of heart failure if heart failure develops as a result of aortic stenosis - for example, angiotensin-converting enzyme (ACE) inhibitors and/or 'water' tablets (diuretics). See separate leaflet called Heart Failure for more details on treatment methods.
Surgical treatments
An operation to fix aortic stenosis is a common procedure and has a very good chance of success. A surgeon will advise on which is the best option for each situation. The possible options include the following:
Open heart surgery to replace the valve. The replacement may be with a mechanical or a tissue valve.
Mechanical valves are made of materials which are not likely to react with the body, such as titanium. With this type of replacement, long term medication to reduce the risks of clots (usually warfarin) is required.
Tissue valves are made from treated animal tissue, such as valves from a pig.
Transcatheter aortic valve implantation (TAVI)
Plastic tubes (catheters) are inserted into the heart through various arteries. Using these tubes, an artificial valve is sited within the existing aortic valve. This procedure does not require open heart surgery. This has historically mainly been used for people who have a higher risk of complications during surgery but recent studies suggest that it has similar outcomes to aortic valve replacements in people over 70 years of age. Other studies have shown TAVI is probably better than open heart surgery in those patients who have intermediate or high risks of complications from surgery but that replacement surgery remains the better option for patients who are otherwise fit and well.
Stretching the stenosed valve (balloon valvuloplasty)
This is an option that is occasionally considered. This also does not require open heart surgery.
A catheter is passed through the blood vessels to the aortic valve and then the valve is stretched with a balloon.
Balloon valvuloplasty has historically been used only in those who were unsuitable for valve replacement surgery because the improvement in the flow across the valve (following balloon valvuloplasty) often only lasts for a year or so. This option has largely been replaced by TAVI as this is also less invasive than open heart surgery but has much better long-term results.
An operation to widen the valve (valvotomy)
This requires open heart surgery and is very rarely offered any longer.
Complications of aortic stenosis
Back to contentsAortic stenosis can lead to a thickening of the muscle in the left ventricle because the left ventricle is working very hard to try and pump blood through the narrowed valve. This leads to heart failure which can cause fluid to build up in the lungs (causing shortness of breath) and the legs (causing swelling/oedema). This is the most common complication of aortic stenosis.
Other complications include: increased pressure in the blood vessels in the lungs (pulmonary hypertension), irregular heart rhythm due to the electrical conduction system in the heart muscle being affected, increased risk of infective endocarditis, and sudden death.
What is the outlook for people with aortic stenosis?
Back to contentsMany cases are mild and cause no symptoms. Symptoms tend to become worse over the years and, although medication may ease symptoms, they cannot reverse a narrowed (stenosed) valve.
Surgery is usually advised for anyone with symptoms but referral for consideration of surgery is now advised for anyone with moderate or severe aortic stenosis, even if they have no symptoms. Surgical treatment has greatly improved the outlook (prognosis) in most people. Surgery has a very good success rate.
The outlook is good if the valve is treated before the heart becomes damaged.
Patient picks for Heart disease

Heart health and blood vessels
Heart disease
The heart is a muscle pump located in the chest, which pumps blood around the body. It keeps pumping from a few weeks after conception until we die. There are a number of different conditions that can affect how the heart works.
by Dr Rachel Hudson, MRCGP
Heart health and blood vessels
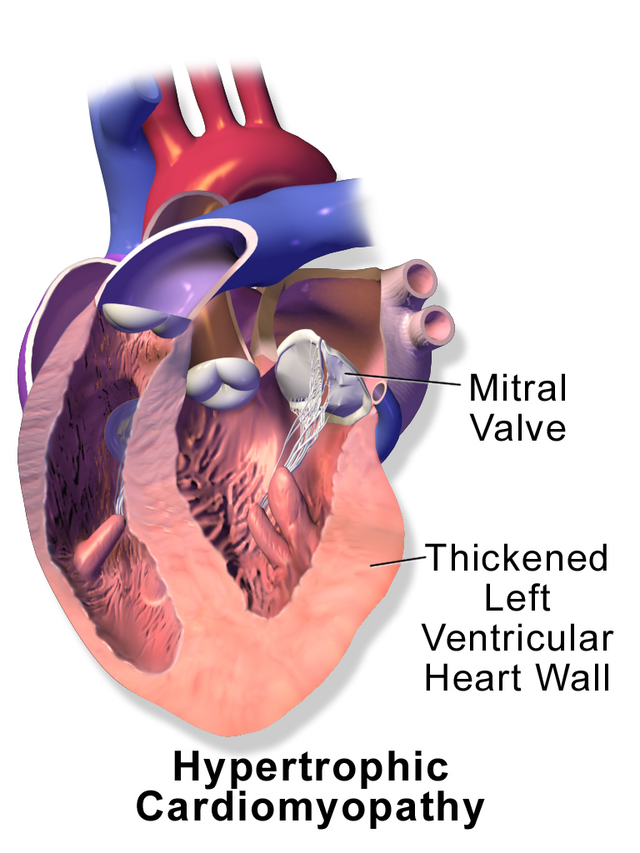
Hypertrophic cardiomyopathy
In hypertrophic cardiomyopathy the heart muscle becomes thickened (hypertrophies) in parts of the heart. In the normal heart, the muscle cells are regular and patterned. In hypertrophic cardiomyopathy the cells of the heart muscle become irregular and disordered.
by Dr Colin Tidy, MRCGP
Further reading and references
- Prophylaxis against infective endocarditis: Antimicrobial prophylaxis against infective endocarditis in adults and children undergoing interventional procedures; NICE Clinical Guideline (March 2008 - last updated July 2016)
- 2023 ESC Guidelines for the management of infective endocarditis; European Society of Cardiology (Aug 2023)
- Nishimura RA, Otto CM, Bonow RO, et al; 2017 AHA/ACC Focused Update of the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease. Circulation. 2017; CIR.0000000000000503. Originally published March 15, 2017.
- Ozkan M; What is new in ACC/AHA 2017 focused update of valvular heart disease guidelines. Anatol J Cardiol. 2017 Jun;17(6):421-422. doi: 10.14744/AnatolJCardiol.2017.7925.
- Heart valve disease presenting in adults: investigation and management; NICE guideline (November 2021)
- Aortic Valve Stenosis; Mayo Clinic
- Pujari SH, Agasthi P; Aortic Stenosis.
- Effect of Transcatheter Aortic Valve Implantation vs Surgical Aortic Valve Replacement on All-Cause Mortality in Patients With Aortic Stenosis; JAMA
- Transcatheter aortic valve implantation for aortic stenosis; NICE (July 2017)
Continue reading below
About the author

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 13 Nov 2028
15 Nov 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.