Hypospadias
Peer reviewed by Dr Rachel Hoad-RobsonLast updated by Dr Toni Hazell, MRCGPLast updated 15 Nov 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Hypospadias is a common abnormality of the urethra and penis that is present at birth; a type of birth defect. This can cause problems with passing urine and also with erections. It can range in severity. Surgical correction is usually very successful.
In this article:
Video picks for Penis problems
Continue reading below
What is hypospadias?
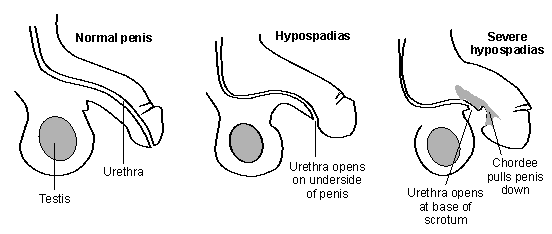
The main problem is that the urethra (which is the tube which drains urine from the bladder) forms in such a way that it opens on the underside of the shaft of the penis instead of at the tip of the penis (also called the head of the penis). There are different types of hypospadias - the location of the opening can be anywhere from just below the normal position (mild) to as far back as the base of the scrotum (severe). 7 out of 10 cases are usually the mild type.
Hypospadias may also include the following:
A hooded appearance of the foreskin. This is because the foreskin does not develop on the underside of the penis.
Tightening of the tissues on the underside of the penis (called 'chordee'). This pulls the penis down and it cannot fully straighten. The further back the urethral opening is, the more severe the chordee tends to be. Mild hypospadias may not have any chordee.
Hypospadias
Hypospadias occurs in about 1 in 250 boys. It seems to be getting more common. The reason why the penis does not develop properly is still not clear. The development of the penis whilst the baby is growing in the womb (uterus) is partly dependent on the male sex hormones such as testosterone. The effects of testosterone on the growing penis may be blocked in some way. Although it is not a genetic condition, hypospadias can run in some families.
What problems can hypospadias cause?
Back to contentsProblems are likely to occur if hypospadias is left untreated. The further back the opening of the urethra is, the more severe the problems are likely to be.
Passing urine is different to normal. Babies with hypospadias will have no symptoms of hypospadias, because they use a nappy. However, when older, the urine stream may not be able to be directed forward into a urinal. When going to the toilet the urine is likely to 'spray' backwards. Sitting on a toilet may be needed to pass urine without mess.
Chordee which causes bending of the penis. This is more noticeable when the penis is erect. Sexual intercourse may be difficult or impossible in severe cases.
Psychological problems about being 'different' to normal are common.
Mild erection difficulties and premature ejaculation have been reported in adulthood in patients who have had surgery for hypospadias in childhood.
Continue reading below
Are any tests needed?
Back to contentsThe diagnosis is usually obvious from examining the penis. No other tests are routine. However, a small number of people with severe hypospadias (when the urethral opening is at the base of the scrotum) may have other abnormalities of the genitals including undescended testicles. The appearance of severe hypospadias may be part of a rare 'intersex' syndrome. Therefore, tests of the chromosomes and scans of the genitals may be made to determine if it is part of a wider syndrome. Note: these syndromes are rare and most boys with hypospadias are of the male sex and have no other abnormalities.
How is hypospadias treated?
Back to contentsIf the hypospadias is mild, with the opening of the urethra just a little down from normal and with no bending of the penis, no treatment may be needed.
Hypospadias surgery
However, in most cases an operation is required to correct the hypospadias - a hypospadias repair. This can usually be done in one operation. However, if the hypospadias is more complicated, two operations may be necessary. The operation is usually done when the child is around 4-18 months old.
A full discussion with a surgeon is needed to decide what can be done. The goals of treatment are:
For urine to be passed in a forward way.
For the penis to be straight when erect.
For the penis to look as normal as possible.
The position of the opening of the urethra is altered. Also, if chordee is present then this is corrected to allow the penis to straighten. The foreskin is usually used during the operation to make the new urethra so it is very important that a circumcision is not done before the corrective surgery is performed. Parents who would usually circumcise their child for religious reasons may want to discuss the need to delay circumcision with their spiritual leader, who would usually be able to reassure them as to how this can be done in accordance with their faith.
Continue reading below
What is the outlook (prognosis) for hypospadias?
Back to contentsThe success of the operation and the 'normality' that can be achieved, depend on the severity of the hypospadias.
Patient picks for Penis problems

Men's health
Peyronie's disease
Peyronie's disease causes a curved or bent penis. It is caused by scar tissue forming along the shaft of the penis. This causes painful erections and a bend or curve, usually about halfway along the penis. The change in shape is usually only obvious when the penis is erect.
by Dr Doug McKechnie, MRCGP

Men's health
Phimosis and paraphimosis
Phimosis means that the foreskin of the penis is too tight and so cannot be pulled back off the rounded head of the penis (glans). In paraphimosis, the foreskin has been pulled back (retracted) but cannot be returned to the original position. Paraphimosis needs emergency medical treatment to prevent complications.
by Dr Doug McKechnie, MRCGP
Further reading and references
- van Rooij IA, van der Zanden LF, Brouwers MM, et al; Risk factors for different phenotypes of hypospadias: results from a Dutch case-control study. BJU Int. 2013 Jan 10. doi: 10.1111/j.1464-410X.2012.11745.x.
- EAU Paediatric Urology Guidelines. Edn. presented at the EAU Annual Congress Copenhagen; European Association of Urology, 2018 - updated 2023
- van der Horst HJ, de Wall LL; Hypospadias, all there is to know. Eur J Pediatr. 2017 Apr;176(4):435-441. doi: 10.1007/s00431-017-2864-5. Epub 2017 Feb 11.
- White JT, Kovar E, Chambers TM, et al; Hypospadias Risk from Maternal Residential Exposure to Heavy Metal Hazardous Air Pollutants. Int J Environ Res Public Health. 2019 Mar 15;16(6). pii: ijerph16060930. doi: 10.3390/ijerph16060930.
- Mole RJ, Nash S, MacKenzie DN; Hypospadias. BMJ. 2020 Jun 17;369:m2070. doi: 10.1136/bmj.m2070.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Nov 2027
15 Nov 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.